Atypical localizations of the basal cell carcinoma: series of 12 cases
Ibtissam Assenhaji , Hanane Baybay, Kaoutar Achehboune, Zakia Douhi, Sara Elloudi, Fatima Zahra Mernissi
, Hanane Baybay, Kaoutar Achehboune, Zakia Douhi, Sara Elloudi, Fatima Zahra Mernissi
Department of Dermatology CHU Hassan II Fez, Morocco
Corresponding author: Dr. Ibtissam Assenhaji
Submission: 07.10.2019; Acceptance: 12.01.2020
DOI: 10.7241/ourd.2020e.86
Cite this article: Assenhaji I, Baybay H, Achehboune K, Douhi Z, Elloudi S, Mernissi FZ. Atypical localizations of the basal cell carcinoma: series of 12 cases. Our Dermatol Online. 2020;11(e):e86.1-e86.3.
Citation tools:
Copyright information
© Our Dermatology Online 2020. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
Sir,
Basal cell carcinoma (BCC) often affects the cephalic extremity, rarely the photoprotected areas 10 to 15% of cases [1].
We report a series of 12 BCC cases with unusual localization.
This is a retrospective study from 2015 to 2018 collecting all cases of BCC with unusual localization over 290 cases of BCC followed in the Dermatology Department CHU Hassan II of Fez, Morroco.
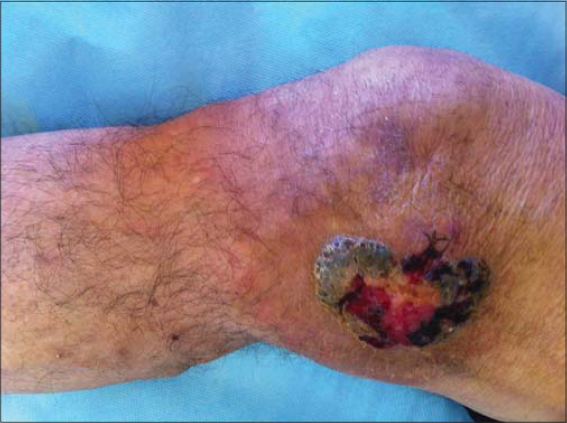
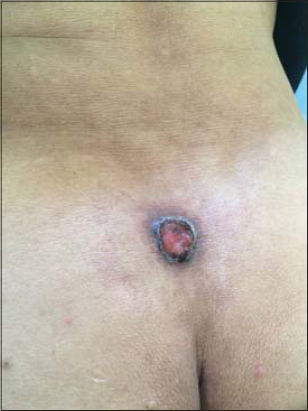
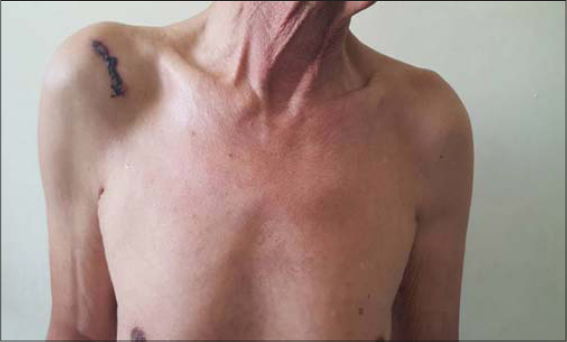
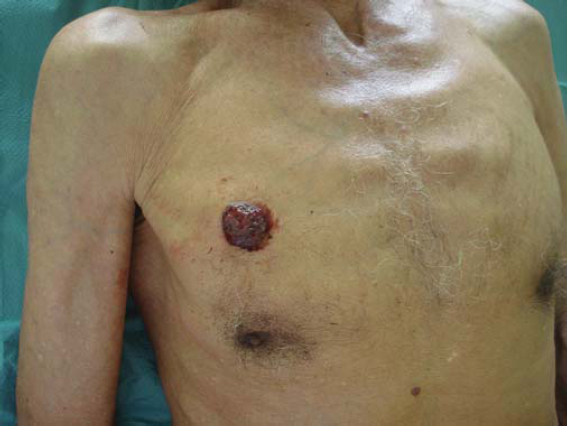
We collected twelve patients followed for BCC in unusual locations such as three in the back, three in the trunk (Figs. 1 and 2), and one the shoulder (Fig. 3), the sacral region (Fig. 4), the knee (Fig. 5), the leg, the elbow crease and one on a precursor lesion of hamartoma Jadassohn (Fig. 6).
The mean age at diagnosis was 59 years (35 to 82 years) with a male predominance; the phototype ranged from 3 to 4, the average consultation time was 4 years (1 to 12 years), no risk factors were found. The symptoms motivating the consultation were most often ulceration and increase in size.
Clinical examination found ulcero-budgeonnanneur tumors in 50% of cases, plaques ulcerated in 25.7%; nodules in 16%, and papules pigmented in 8.3%. The lesions averaged 20.5 mm (10 to 40 mm). The dermoscopic signs were in favor of CBC. The diagnosis of basal cell carcinoma was confirmed by histology.
The histological study concluded with a nodular CBC in 75%, superficial in 16.6%, nodular pigmented in 8.4%.
Surgical excision was required in all cases with healthy margins. The evolution was good in 12 of the cases with a free good evolution.
The prevalence of uncommon BCCs in our series is lower than that reported in the literature 10-15% [1]. The consultation period was late in our series, which can be explained by the occurrence of CBCs in hidden areas.
In non-photo-exposed areas, other undetermined etiological factors than UV exposure would also play an important role in their occurrence of CBCs, such as vesmodegib mutation abnormalities during Gorlin’s syndrome, radiotherapy, immunosuppression [2], not found in our series. Regarding the occurrence of BCC on a precursor lesion such as hamartoma Jadassohn, it is reported in less than 1% in the literature [3].
Dermoscopy allows the presumptive diagnosis of BCC in these unusual locations, but the confirmation is histological. Nodular BCC represents the histological subtype most commonly reported for these forms [1], consistent with our data. The evolution depends on the possibility of a complete excision with healthy margins [1,4], which varies according to the localizations. Indeed, it was favorable in all our patients with a satisfactory decline in most cases.
Our series illustrates the unusual locations of BCCs in non-photo-exposed areas, but not exceptional, justifying a complete clinico-dermoscopic cutaneous-mucosal examination.
Consent
The examination of the patient was conducted according to the Declaration of Helsinki principles.
The authors certify that they have obtained all appropriate patient consent forms. In the form the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
REFERENCES
1. Ouédraogo MS, Korsaga/SoméN, Ouédraogo AS, Ouédraogo NA, Tapsoba GP, Konsem T, et al. [Epidermoid carcinoma involving on chronic ulcer of the upper lip in a patient infected with HIV]. Our Dermatol Online. 2016;7:431-5.
2. BartošV, KullováM. Immunohistochemical evaluation of E-cadherin expression in basal cell carcinoma of the skin. Our Dermatol Online. 2015;6:257-64.
3. Tiwary AK, Mishra DK. Jadassohn Lewandowsky syndrome:Type 1 pachyonychia congenita. Our Dermatol Online. 2017;8:56-9.
4. BartošV, BulejčíkováT. Basal cell carcinoma of the skin with clear cell differentation:A report of two cases. Our Dermatol Online. 2016;7:422-6.
Notes
Source of Support: Nil,
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
|





 http://orcid.org/0000-0003-3455-3810
http://orcid.org/0000-0003-3455-3810
Comments are closed.