Pansclerotic morphea: A historical case in children
Zina Kaddioui , Fatima Ezzehra El Fetoiki, Fouzia Hali, Hayat Skalli Dehbi, Soumiya Chiheb
, Fatima Ezzehra El Fetoiki, Fouzia Hali, Hayat Skalli Dehbi, Soumiya Chiheb
Dermatology Department, UHC Ibn Rochd, Casablanca, Morroco
Corresponding author: Dr. Zina Kaddioui, E-mail: zina.kaddioui@gmail.com
Submission: 04.02.2020; Acceptance: 17.03.2020
DOI: 10.7241/ourd.2020e.25
Cite this article: Kaddioui Z, El Fetoiki FE, Hali F, Dehbi HS, Chiheb S. Pansclerotic morphea: A historical case in children. Our Dermatol Online. 2020;11(e):e25.1-e25.2.
Citation tools:
Copyright information
© Our Dermatology Online 2020. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
Morphea is a variant of localized scleroderma in which lesions are usually limited to the skin and subcutaneous tissue. Pansclerotic morphea is a rare atrophying and sclerosing type of morphea. It can follow a comparatively benign course with spontaneous resolution of symptoms, or sometimes can lead to a variety of complications resulting in progressive disability. We report a case of pansclerotic morphea in an 4-year-old female child involving the right upper limb, resistant to treatment and the cause of a major functional and esthetic damage.
Key words: Pansclerotic morphea; Corticosteroids; Methotrexate
INTRODUCTION
Morphea, or localized scleroderma, is characterized by sclerosis of the skin and subcutaneous tissues. Several variants have been described, which are distinguished by their clinical manifestations, their evolutionary profile and the cutaneous and subcutaneous anatomical structures affected by fibrosis.
We report a case of historical evolution, resistant to treatment and the cause of a major functional and esthetic damage.
OBSERVATION
4-year-old girl, presented in October 2016 with scleroatrophy of the right upper limb evolving for 1 year and 5 months having started with a single plate of shiny sclerous aspect at the posterior surface of the right wrist extending towards the entire limb. She had no history of fever, trauma, medication, or any exposure to chemicals or radiation. Clinical examination found an extensive sclerotic plaque of the whole upper limb, dyschromic in places, with stiffness and fixation of all joints of the right upper limb and atrophy of all muscles of the same limb (Figs. 1a and 1b). She had no muscle damage, no Raynaud’s phenomenon, no respiratory or gastrointestinal involvement. The clinical picture was suggestive of a pansclerotic morphea. We carried out an immunological assessment which showed anti-nuclear antibody positive at 400. Radiological examination of the affected limb showed soft tissue atrophy and thinning of the long bone diameter compared on the normal side. We put the patient on steroids 1.5 mg/kg/day with methotrexate 7.5 mg/ week with regular physical therapy sessions for 1 year with no improvement.
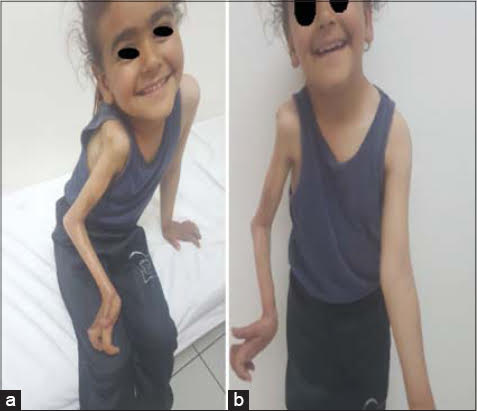 |
Figure 1: (a-b) Extensive plaque of the whole right upper limb with atrophy of all muscles. |
DISCUSSION
This observation illustrates a case of severe pansclerotic morphea characterized by its rapidly aggressive evolution and an attack of the skin and deep structures causing contractures and trophic disorders.
Pansclerotic morphea of childhood (PMC) is a rare subtype of juvenile localized scleroderma (JLS) characterized by the rapid progression of deep cutaneous fibrosis or pansclerosis that involves the subcutaneous adipose tissue and occasionally the fascia, muscles and bone [1]. Initially, the disease involves the extremities, spreading to the trunk, face and scalp, while distal areas are spared.
The exact cause is unknown; however, trauma, excessive physical activity, immobilization, radiation, infection by Borrelia burgdorferi, febrile illness, and vaccinations have been suggested as trigger factors.
Pansclerotic morphea usually starts before the age of 14 years with female predominance at a ratio of 3:1 [2]. Our patient was a female and presented with moprhea at the age of 2years and 7months.
Diagnosis is essentially clinical however skin biopsy can be useful. The disease is usually slowly progressive and spontaneous remission can occur. There is no effective treatment available.
Different therapeutic modalities with varying results have been tried: oral steroids, calcitriol, D-penicillamine, low dose methotrexate (MTX), tropical calcipotriene. However, none of these has shown any significant promise until now [3].MTX either in combination with corticosteroid or both with varied successes [4]. In recent years, other therapies that have been trialed to complement the initial treatments include mycophenolate mofetil, sirolimus, biologics, tyrosine kinase inhibitors (TKI), and JAKI. Given that IL-6 plays an integral role in PMC by regulating fibroblast differentiation and stimulating collagen synthesis, abatacept and tocilizumab are strong candidate drugs for managing PMC [4]. Our patient had received oral corticosteroids associated with MTX but without any improvement related to the severity of skin involvement and late presentation.
Complications include severe joint contractures, limb discrepancy, articular ankyloses [5], and cutaneous ulceration which often results in septicemia [6]. Apart from marked functional and psychological impacts, neoplasia, cardiomyopathy, and restrictive pulmonary disease have also been reported [7–10].
CONSENT
The examination of the patient was conducted according to the Declaration of Helsinki principles.
The authors certify that they have obtained all appropriate patient consent forms. In the form the patient(s) has/have given his/her/their consent for his/ her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
REFERENCES
1. Diaz Perez JL, Connolly SM, Winkelmann RK. Disabling pansclerotic morphea of children. Arch Dermatol. 1980;116:169–73.
2. Lewkonia RM, Lowry RB. Progressive hemifacial atrophy (Parry-Romberg syndrome) report with review of genetics and nosology. Am J Med Genet. 1983;14:385-90.
3. Dasgupta MK, Patra C, Sarkar S, Das S. Pansclerotic morphea:A male child with hemiatrophy of lower limb. Indian Dermatol Online J. 2014;5:170-2.
4. Soh HJ, Samuel C, Heaton V, Renton WD, Cox A, Munro J. Challenges in the diagnosis and treatment of disabling pansclerotic morphea of childhood:case-based review. Rheumatol Int. 2019;39:933–41.
5. Kura M, Jindal S. Disabling pansclerotic morphea of child- hood with extracutaneous manifestations. Indian J Dermatol. 2013;58:159.
6. Roldan R, Morote G, Castro MDC, Miranda MD, Moreno JC, Collantes E. Efficacy of bosentan in treatment of unre- sponsive cutaneous ulceration in disabling pansclerotic morphea in children. J Rheumatol.2006;33:2538–40.
7. Wollina U, Buslau M, Petrov I, Pramatarov K. Disa- bling pansclerotic morphea of childhood. Expert Rev Dermatol. 2007;2:775–84.
8. Forsea AM, Cretu AN, Ionescu R, Giurcaneanu C Disa- bling pansclerotic morphea of childhood—unusual case and man- agement challenges. J Med Life. 2008;1:348–54.
9. Wollina U, Looks A, Schneider R, Maak B. Disabling mor- phoea of childhood—beneficial effect of intravenous immuno- globulin therapy. Clin Exp Dermatol. 1998;23:292–3.
10. Petrov I, Gantcheva M, Miteva L, Vassileva S, Pramatarov K. Lower lip squamous cell carcinoma in disabling panscle- rotic morphea of childhood. Pediatr Dermatol. 2009;26:59–61.
Notes
Source of Support: Nil.
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
|



Comments are closed.