Acne fuminans in the course of oral isotretinoin treatment. Presentation of cases
Magdalena Kręgiel, Anna Żuchowska, Katarzyna Tomaszewska, Agnieszka Wojciechowska, Anna Jędrowiak, Katarzyna Tabara, Wojciech Bienias, Joanna Krzysiek, Andrzej Kaszuba, Ewa Trznadel-Grodzka
Department of Dermatology, Pediatric Dermatology and Oncology, Medical University of Lodz, ul. Kniaziewicza 1/5, 91-347 Lodz, Poland
ABSTRACT
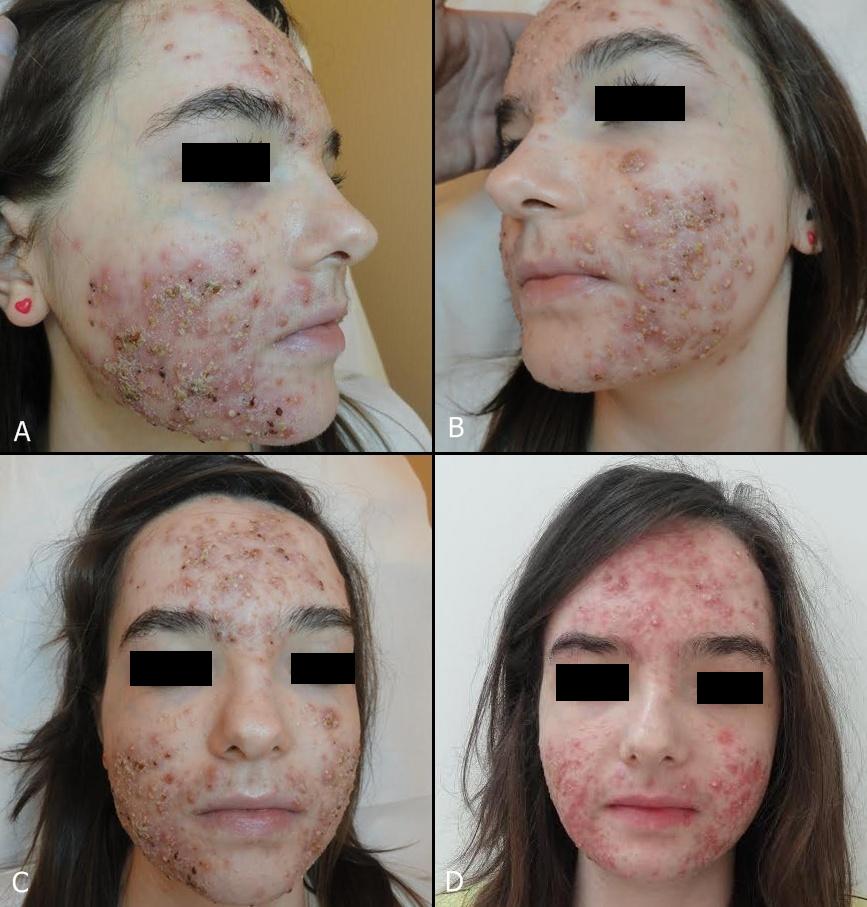
Isotretinoin is considered a gold standard in treating severe cases of acne. It brings lots of benefits but on the other hand can cause series of undesirable side-effects. I present 2 cases of patients suffering from acne fulminans in the course of treatment with oral isotretinoin. Acne fulminans is a very severe systemic disease and its course is difficult to foresee. The most important is rapid diagnosis and implementation of treatment. Systemic corticosteroids combined with isotretinoin or high does of antibiotics are the most effective. The alternative methods are: dapsone, infliximab.
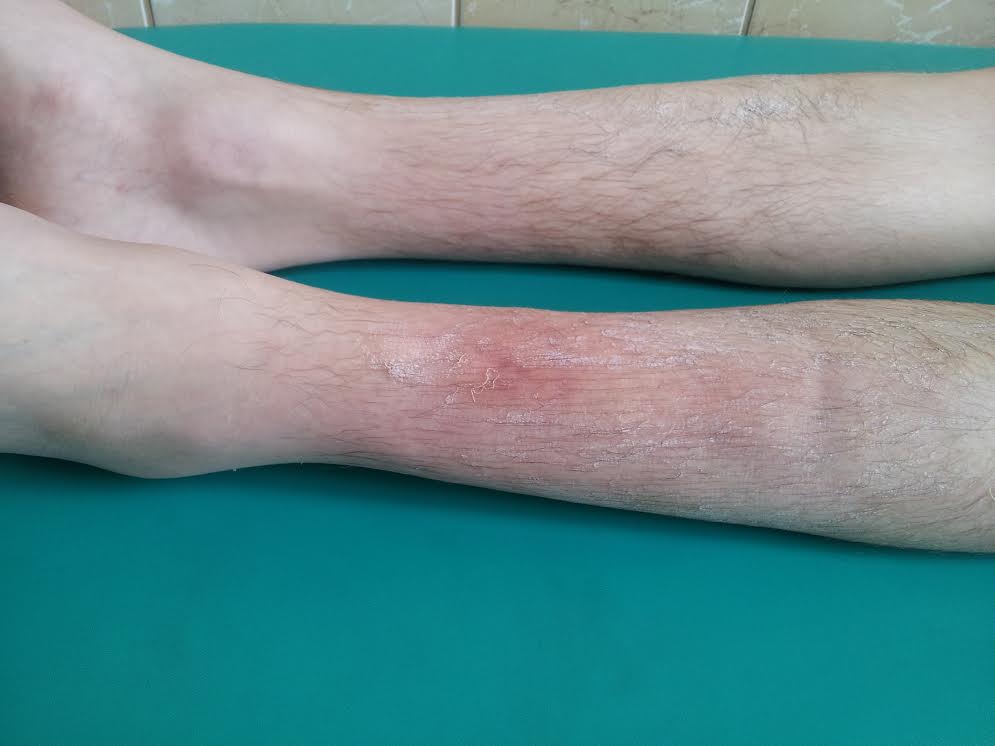
Key words: Acne fulminans, pseudo-acne fulminans, isotretinoin, erythema nodosum
INTRODUCTION
CASE REPORT


DISCUSSION
Consent
The examination of the patient was conducted according to the Declaration of Helsinki principles.
REFERENCES
1. Bergler-Czop B, Brzezińska-Wcisło L. Skórno-śluzówkowe objawy uboczne retinoidów doustnych w terapii trądziku pospolitego. Post Nauk Med. 2012;10:777-86.
2. Żaba R. Special paper safety of the treatment with retinoids. Post Dermatol Alergol. 2006;4:161–74 .
3. Eksioglu E, Oztekin F, Unlu E, Cakci A, Keyik B, Karadavut IK. Sacroilitis and polyneuropathy during isotretinoin treatment. Clin Exp Dermatol. 2008;33:122-4.
4. Aydogan K, Karli N. Effects of oral izotretinoin therapy on peripheral nerve functions; a preliminary study. Clin Exp Dermatol. 2007;32:81-4.
5. Plewig G, Kligman AM. Acne: morphogenesis and treatment. Springer. Berlin. 1975;196.
6. Pastuszka M, Kaszuba A, Kurowska-Poznańska K. Trądzik piorunujący (acne fulminans). Dermatol Prakt. 2010;2:52-8.
7. Geller AS, Alagia RF. Sacroiliitis after use of oral isotretinoin-association with acne fulminans or adverse effect? An Bras Dermatol. 2013;88:193-6 .
8. Sarifakioglu E, Onur O, Kart H, Yilmaz AE. Acute myopathy and acne fulminans triggered by isotertioin therapy. Eur J Dermatol. 2011;2:794-5.
9. Thomson KF. Cunliffe WJ. Acne fulminans „sine fulminans”. Clin Exp Dermatol. 2000;25:299-301.
10. Grando LR, Leite OG, Cestari TF. Pseudo-acne fulminans associated with oral isotetinoin. An Bras Dermatol. 2014;89:657-9.
11. Demircay Z, Kus S, Sur H. Predictive factors for acne flare during isotretinoin treatment. Eur J Dermatol. 2008;18:452-6.
12. Dreno B, Bettoli V, Ochsendorf F et al.An expert view on the tratment of acne with systemic antibiotics and/or oral isottetinoin in the light view of new European recommendations. Eur J Dermatol. 2006;212:168-76.
13. Tan BB, Lear JT, Smith AG.Acne fulminans and erythema nodosum during isotretinoin therapy responding to dapsone.Clin Exp Dermatol. 1997;22:26-7.
14. Joly P, Prost C, Gaudemar M, Revuz J. Acne fulminans triggered by isotretinoin therapy, Ann Dermatol Venerol. 1991;118:369-72.
15. Żaba R, Schwartz RA, Jarmuda S, Czarnecka-Operacz M, Silny W. Acne fulminans: explosive systemic form of acne. JEADV 2011;25:501-7.
16. Szepietowski J, Kapińska-Mrowiecka M, Kaszuba A, Langner A, Placek W, Wolska H, Matusiak Ł. Trądzik zwyczajny: patogeneza i leczenie.Konsensus Polskiego Towarzystwa Dermatologicznego. Przeg Dermatol. 2012;99:649–73.
17. Schwartz RA, Nervi SJ.Erythema nodosum: a sign of systemic disease. AM Fam Physician. 2007;75:695-700 .
18. Wong SS, Pritchard MH, Holt PJ. Familial acne fulminans. Clin Exp Dermatol. 1992;17:351-3.
19. Iqbal M, Kolodney MS. Acne fulminans with synovitis-acne-pustulosis-hyperostosis-osteitis (SAPHO) syndrome treated with infliximab. J Am Acad Dermatology. 2005;52:118-20.
20. Charakida A, Mouser PE, Chu AC. Safety and side effects of the acne drug, oral isotretinoin. Expert Opin Drug Saf. 2004;3:119-29.
Notes
Source of Support: Nil,
Conflict of Interest: None declared.



Comments are closed.