Cutaneous leishmaniasis of the neckline mimicking squamous cell carcinoma
Siham Boularbah , Hanane Baybay, Sabrina Oujdi, Meryem Soughi, Sara Elloudi, Zakia Douhi, Fatima Zahra Mernissi
, Hanane Baybay, Sabrina Oujdi, Meryem Soughi, Sara Elloudi, Zakia Douhi, Fatima Zahra Mernissi
Department of Dermatology, University Hospital Hassan II, Fes, Morocco
Citation tools:
Copyright information
© Our Dermatology Online 2024. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
Sir,
Cutaneous leishmaniasis is a parasitic infection with cutaneous tropism linked to the inoculation of leishmaniasis transmitted by sandfly bites [1]. It is characterized by its ability to clinically simulate other pathological entities [2,3]. This highlights the need for a good dermoscopic analysis and extensive exploration to avoid diagnostic errors. Herein, we report the case of a patient presenting with an ulcerated, crusted lesion of the trunk revealing cutaneous leishmaniasis and mimicking squamous cell carcinoma [4,5].
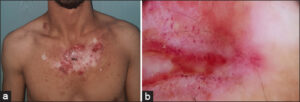
A 29-year-old female patient from an endemic region to Leishmania tropical, followed in our training for neurofibromatosis type 1, presented for two years before her admission with localized pruritus on the trunk with the self-medication of a topical corticosteroid. The evolution was marked by the later appearance of an ulceration of centrifugal evolution in the trunk with a notion of spontaneous healing then recurrence without other associated signs. A dermatological examination revealed a patch of scarring in places and erosive in others at the level of the slightly sclerotic trunk, poorly limited, irregular contours, infiltrated border with a budding bottom topped and an adherent crust (Fig. 1a). A dermoscopic examination found ulcerations, scabs, a yellow teardrop appearance, linear and point vessels, and an erythematous background. The rest of the somatic examination was normal (Fig. 1b).
The skin smear and the anatomopathological examination found some amastigote forms of Leishmania. PCR was positive. HIV serology was negative, the search for visceral leishmaniasis doesn’t find abnormality The diagnosis of cutaneous leishmaniasis was retained.
A pre-therapeutic assessment (NFS, renal, hepatic and cardiac assessment) was performed before putting the patient on systemic glucantime at a dose of 70 mg/kg/ day associated with sessions of dynamic phototherapy with methylene blue. A clear regression marked by the subsidence of the lesions was obtained after treatment for six weeks (Figs. 2a and 2b).
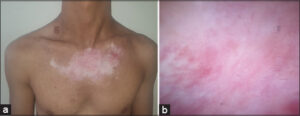 |
Figure 2: (a) Clinical image and (b) dermoscopy showing complete disappearance of the lesions after six weeks of treatment. |
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients gave their consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Mokni M. Cutaneous leishmaniasis. Ann Dermatol Venereol. 2019;146:232-46.
2. Mancy A, Awad KM, Abd-Al-Majeed T, Jameel NF. The epidemiology of cutaneous leishmaniasis in Al-Ramadi, Iraq. Our Dermatol Online. 2022;13:402-7.
3. Paudel V, Parajuli S, Chudal D. Cutaneous leishmaniasis in Nepal:An emerging public health concern. Our Dermatol Online. 2020;11:76-8.
4. Wollina U, Koch A, Bitel A. Deep chronic cutaneous New World leishmaniasis due to Leishmania guyanensis and trichinellosis in a German returnee from Ecuador. Our Dermatol Online. 2019;10:272-4.
5. Mehmet S Gl, Burak T, Soner U. Cutaneous leishmaniasis:A great imitator. Clin Dermatol. 2020;38:140-51.
Notes
Request permissions
If you wish to reuse any or all of this article please use the e-mail (contact@odermatol.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0002-3975-8316 http://orcid.org/0000-0002-3975-8316 http://orcid.org/0000-0003-3455-3810 http://orcid.org/0000-0003-3455-3810 http://orcid.org/0009-0002-5084-9152 http://orcid.org/0009-0002-5084-9152 http://orcid.org/0000-0002-5942-441X http://orcid.org/0000-0002-5942-441X |




Comments are closed.