Epidemiological, clinical, and etiological aspects and management of chronic ulcers at the University Hospital Center of Dermatology in Bamako, Mali
Yamoussa Karabinta 1,2, Tenin Karambé3, Ibrahim Traoré1, Mariam Konaté4, Adama Dicko1,2, Mamadou Gassama1,2, Chata Traoré1, Ousmane Sylla1, Sanata Coulibaly1, Chata Koné1, Labassou Dissa1, Ousmane Faye1,2, Somita Kéita1,2
1,2, Tenin Karambé3, Ibrahim Traoré1, Mariam Konaté4, Adama Dicko1,2, Mamadou Gassama1,2, Chata Traoré1, Ousmane Sylla1, Sanata Coulibaly1, Chata Koné1, Labassou Dissa1, Ousmane Faye1,2, Somita Kéita1,2
1Dermatology Teaching Hospital of Bamako, Bamako, Mali, 2Medical and Dentistry, Faculty of Bamako, Bamako, Mali, 3Teaching Hospital of Gabriel TOURE, Bamako, Mali, 4Teaching Hospital of Kati, Koulikoro, Mali
Citation tools:
Copyright information
© Our Dermatology Online 2024. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
Background: Chronic ulcers of the lower limb (CULL) are characterized by non-healing skin loss, often associated with vascular, neurological, infectious, traumatic, or tumoral factors. These ulcers are prevalent, recurrent, severe, and have significant socio-economic implications. While Western data show a higher prevalence among women and the elderly, with varying rates (0.10% to 0.80%), developing countries, especially in sub-Saharan Africa, report a higher prevalence among young men due to infectious causes. Despite their impact, CULL often lacks attention from health authorities, resulting in delays in medical consultation. This study aims to share experiences in understanding the epidemioclinical aspects and management of CULL.
Objective: The objective was to offer a comprehensive overview of the epidemiological and clinical characteristics and treatment strategies for chronic lower limb ulcers observed at the University Hospital Center of Dermatology in Bamako.
Patients and Methods: Conducted at the Dermatology and Venereology Department of the University Hospital Center of Dermatology in Bamako, this cross-sectional study spanned a period from January to December 2021. It included 520 patients, with 22.1% having chronic ulcers of the lower limbs. Males (52.2%) were predominant, with an average age of 42.4 years. Trauma triggered 73.0% of the cases, and more than half waited over a year before seeking medical help. Bacteriological examinations revealed microbial infections in 67.8% of the cases.
Results: There was a 22.1% prevalence of chronic lower limb ulcers among the 520 patients. Males represented 52.2%, with a median age of 42.4 years. Trauma was the primary trigger in 73.0% of the cases. Bacteriological examinations identified various infections, with 67.8% being infectious in origin. There were diverse characteristics in size, shape, and edge conditions of the ulcers. Trauma was the leading factor in 73.0% of the cases. Bacteriological examinations identified Gram-negative bacilli, Staphylococcus aureus, Streptococcus, with 67.8% of the ulcers being infectious in origin. There was outpatient treatment in 64.3% of the cases. Therapies included postural drainage, venotonics, vasculoprotectors, analgesics, compression stockings, and surgical interventions. Antibiotic therapy based on antibiograms for infectious ulcers. There was maintenance treatment with delayed penicillin in recurrent cases; successful skin grafting in 80.9% of cases, with 40.8% achieving complete healing in less than three months.
Key words: Chronic ulcers, Epidemiological, Clinical, Etiological, Management
INTRODUCTION
The chronic ulcer of the lower limb (CULL) is defined as a loss of skin substance without a spontaneous tendency to heal. It is generally located in the dependent part of the lower limbs (LL), associated with a pathological process of various etiologies: vascular, neurological, infectious, traumatic, or tumoral [1]. Chronic ulcers of the lower limbs are common, recurrent, severe, and have a negative socio-economic impact [2]. Reading epidemiological data from Western series clearly shows that the patients are mostly women and elderly individuals (40–80 years) [3–5]. The analysis conducted by Begaud [2] based on thirteen epidemiological studies published between 1983 and 1997 showed a high prevalence within the general European population. According to this study, the rate fluctuated between 0.10% and 0.80%. In France, this represented at least 60,000 to 180,000 individuals among a population of 60 million. In the U.S., 500,000 to 600,000 individuals are treated for CULL each year [6]. In contrast, in developing countries, especially in sub-Saharan Africa, chronic ulcers of the lower limbs affect young men (25 to 35 years old), with a male-to-female ratio ranging between 1:5. In Africa, the predominant etiology is infectious and is exacerbated by malnutrition and precarious living conditions [7–10]. The studies conducted in Africa do not allow for the determination of a continental prevalence of the chronic ulcer of the lower limb [7–11]. A study conducted in Mali in 2004 reported that, out of 105 cases of chronic ulcers of the lower limbs, 53.3% were of infectious origin, and men represented 60% of the cases [12]. Despite these initial compelling results and the devastating nature of these ulcers, often leading to dramatic complications such as the risk of tetanus, septicemia, hemorrhages, and malignant degeneration, as well as their major socio-economic impact, chronic ulcers of the lower limbs do not receive sufficient attention from health authorities. Added to this is the delay in seeking medical consultation and resorting to traditional practitioners, resulting in serious complications. The aim of this work was to share our experience in understanding the epidemioclinical aspects and management of chronic ulcers of the lower limbs.
Objective
The objective was to present in detail the epidemiological and clinical aspects and therapeutic approaches adopted for chronic ulcers of the lower limbs identified at the University Hospital Center of Dermatology in Bamako.
PATIENTS AND METHODS
Our study was conducted at the Dermatology and Venereology Department of the University Hospital Center of Dermatology in Bamako. The University Hospital Center of Dermatology in Bamako is a specialized center for research on leprosy and endemic-epidemic diseases. It is located in the IV district of the Bamako District, specifically, in the Djicoroni-Para neighborhood. In addition to leprosy, its scope of activities includes dermatology, STIs/HIV-AIDS, and vaccine research. Several units are distinguished within the center: Leprology, Dermatology, Biology, Surgery-Rehabilitation, and the Vaccine Development Center (CVD).
We conducted a cross-sectional, descriptive study with prospective data collection on patients hospitalized and receiving outpatient care for chronic ulcers of the lower limbs at the Dermatology and Venereology Department of the University Hospital Center of Dermatology in Bamako for one year (from January to December 2021). It included all patients diagnosed with ulcers persisting for more than three months and followed at the Dermatology Department of the University Hospital Center of Dermatology in Bamako during the study period. Patients lost to follow-up or those who refused to participate in the study were excluded. A survey form allowed us to gather the following data.
Sociodemographic and epidemiological data (age, sex, ethnicity, occupation, marital status, and place of origin), medical history (HIV, diabetes, sickle cell anemia, etc.), surgical history, and lifestyle factors (tobacco, alcohol, substance abuse, herbal remedies).
Clinical and etiological data based on circumstances of occurrence; characteristics of the ulcer (location, size, shape, edges, base, periwound skin); general examination.
Paraclinical data: complete blood count (CBC)/erythrocyte sedimentation rate (ESR), fasting blood glucose, HIV serology, pus and/or serosity sampling for bacteriological examination and antibiogram, hemoglobin electrophoresis/Emmel test, V.D.R.L./T.P.H.A, X-ray of the affected lower limb, and lesion biopsy for anatomopathological examination. Additional tests may be requested depending on the clinical orientation; therapeutic data (management according to etiology); treatment outcomes. The epidemiological, clinical, and paraclinical data collected through a questionnaire was entered and analyzed using SPSS 16.0 software and document writing was performed using MS Office Word 2016. The free and informed consent of all patients was obtained before their inclusion.
RESULTS
Epidemiological Aspects
From January to December 2021, 520 patients were hospitalized and followed at the Dermatology and Venereology Department of the University Hospital Center of Dermatology in Bamako, including 115 cases of chronic ulcers of the lower limbs (Fig. 1), representing a hospital prevalence of 22.1%.
The male sex represented 52.2% (60 cases). The average age was 42.4 years, with extremes ranging from 10 to 75 years. The most represented age group was between 30 and 39 years, accounting for 26.1%. Among the identified professions, artisans and workers were the majority, accounting for 33.9%. Professions involving prolonged standing were present in 49.6% of the cases, mainly composed of traders and workers. The patients came from all regions of Mali, with a significant representation from Bamako (34.8%). A history of chronic smoking was reported in 23.5%, and a combination of antibiotics + NSAIDs + traditional therapy was found in 66.1% of our patients.
Clinical Aspects
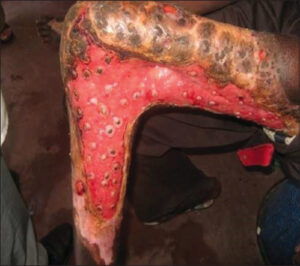
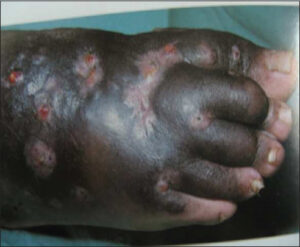
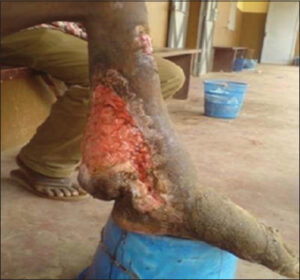
Trauma was the most common triggering factor, accounting for 73.0% of the cases. More than half of the patients waited over a year before their first consultation (61 cases), representing 53.0%. The size, shape, and condition of the edges varied (rounded, polycyclic, geographic contour) (Fig. 2).
Bacteriological examinations conducted on our patients found Gram-negative bacilli in four cases, accounting for 21.1% (Pseudomonas aeruginosa, Escherichia coli), Staphylococcus aureus in six cases, accounting for 31.6%, Streptococcus (Streptococcus spp., Enterococcus spp.) in seven cases, accounting for 36.8%, and plurimicrobial infections in two cases (Fig. 3), accounting for 10.5%. Infectious origin ulcers comprised 67.8% of our series, including 60.9% of bacterial origin, 5.2% of fungal origin (Fig. 4), and 1.7% of parasitic origin (cutaneous leishmaniasis).
Therapeutic Aspects
Patients were treated on an outpatient basis in 64.3% of the cases.
Several therapies were used for venous ulcers, including postural drainage by elevating the limbs associated with strict rest, venotonics (Veinosmine*, Cyclo 3 fort*), vasculoprotectors (Ginkor fort*), analgesics (Paracetamol 500 mg), elastic compression stockings and bands, and drainage kinesiotherapy for lymphedema. For arterial ulcers, the patients were given vasculoprotectors (Ginkor fort*), analgesics (Paracetamol 500 mg), and antiplatelet agents (low-dose aspirin, heparin). Then, the patients were referred to surgery for further management. Regarding infectious ulcers, depending on the etiology, patients received antibiotic therapy based on the antibiogram or, alternatively, broad-spectrum antibiotic therapy (Amoxi + Clavulanic Acid: 50–100 mg/kg/day, 1 to 3 doses). Analgesics (Paracetamol: 40 mg/kg/day in 2 to 3 doses/day), intramuscular or peri-lesional Glucantime, thermotherapy on lesions, antifungal treatment (Fluconazole: 200 mg per day) were also administered. In the case of malignant degeneration confirmed by histology, surgical intervention with lymph node dissection or leg amputation was performed in orthopedic surgery. Potassium permanganate bath followed by dermal Betadine was the most commonly used, representing 83.5% of the cases, followed by mechanical and/or chemical debridement (Cutimed Gel*), performed in almost all cases (90.4%) as local care. Iron supplementation and multivitamin therapy were administered in all cases of clinical and/or biological anemia, with tetanus vaccination performed in all cases.
Therapeutic Evolution
Maintenance treatment with delayed penicillin for 3 to 4 months after healing was given in recurrent ulcer cases and in cases of lymphedema. Skin grafting was successfully performed in 80.9% (93 cases). In our study, 47 patients (40.8%) achieved complete healing in less than three months of treatment.
COMMENTS AND DISCUSSION
Methodology
Out of a total of 520 patients hospitalized and followed in the service for one year, we included 115 cases of chronic ulcers of the lower limbs. The reduced sample size of 115 was due to the lack of means for some patients to undergo additional examinations and to fulfill prescriptions, as well as the loss of follow-up for certain patients.
Epidemiology
In our sample, men were the most affected, with a sex ratio of 1.1. The age group of 30–40 years was the most represented and particularly active (26.1%). This epidemiological data was comparable to those by Cissé [11] in Mali, who found a sex ratio of 3.1 in favor of men, with an average age of 38.45 years +/- 12.3. A study by Alzouma [12] in 2004 found a predominance of young men with an average age of 41.59 years +/- 18.4 and a sex ratio of 1.5. In general, our studies were not comparable to those conducted in Western countries, in which the maximum incidence was observed in the elderly, preferably in females, with a peak around 70–80 years [1]. This difference is explained by the frequency of trauma, the main triggering factor for chronic ulcers of the lower limbs in young individuals, constituting the most active layer of our population. We found 57 cases of professions with prolonged standing, representing 49.57%, which explains the frequency of varicose ulcers in our sample. The problem is that we cannot withdraw them from their activities or change their profession. There is also the issue of insufficient infrastructure or rather qualified healthcare personnel in certain regions, given that many of our patients resided in rural areas.
Clinical Aspects
Trauma to the lower limb (MI) was the most commonly reported triggering factor, accounting for 73% of the cases. This frequency is higher than that found by Cissé [11] in Mali, which was 54%, and by Alzouma [12] in Mali, which was 65.7%. Once again, our study confirmed the damage caused by neglected traumas to the lower limbs in our region. The characteristics of the ulcer, such as the number, location, size, shape, condition of the edges, base, and peri-ulcer skin, varied widely and often assisted us in determining the etiology. These elements allowed us to assess the severity and chronicity of the ulcerations. Thus, 61.7% of our cases had lesions on the right leg, and 16.5% had bilateral involvement. Bilateral involvement is an indicative factor for certain etiologies (vascular, hematological). Necrotic, purulent, and fibrinous lesions accounted for 88.7% of the cases, indicating the severity of infection. The condition of the edges and the base of the ulceration helped evaluate chronicity, direct toward a specific etiology (tumoral, mycobacteria), and predict prognosis or healing duration. In our study, the edges were elevated in 54.8% and jagged in 1.7% of the cases. The base was necrotic in 88.7% of the cases, with granulation observed in 15.7% of the cases. Varicose lesions suggested a vascular etiology of the ulceration; in our series, varices were observed in 4.3% of the patients. Clinical anemia was found in 33.9% of the cases, and a general state alteration was present in 2.6% of our patients. This may be explained by malnutrition and wound exudates. The presence of pain was reported in 67% of the cases. This presence of pain allowed us to consider malignant transformation, especially when associated with an ulceration that budded and bled at the slightest touch, and to think of an inflammatory process of infectious origin. Meanwhile, in the literature [1], the presence of pain was mainly assessed initially to classify vascular UCMI into two etiologies: venous or arterial.
Paraclinical Aspects
Paraclinical examinations were conducted on our patients. HIV serology was positive in 3.5% (4 out of 43 performed), hemoglobin abnormalities in 6.1% of the cases (7 out of 19 performed, including 4 SS trait cases and 3 AS trait cases), hyperglycemia in 5.2% of the cases (6 out of 74 performed), and biological anemia found in 3.5% of the cases (4 out of 63 performed). In our series, there was nothing to suggest that anemia was caused by the ulcer, and vice versa, yet it may be affirmed that it contributes to delayed healing. Most patients showed clinical improvement early in the anti-anemia treatment. SS sickle cell patients seem to be more affected by leg ulcers than those with AS traits, which is easily understandable: tissue damage is more significant in the former. Pus samples from the ulcer were obtained in 30 cases out of 115 patients. Bacteriological examinations revealed Gram-negative bacilli (Pseudomonas aeruginosa, Escherichia coli) in 4 cases, Staphylococcus aureus in 6 cases, Streptococcus (Streptococcus spp., Enterococcus spp.) in 5 cases, and cases of polymicrobial infections in 4 cases. Taking into account the number of cases where the base of the ulcer is purulent (102 cases), the number of bacteriological examinations performed was insufficient; 85 cases, or 73.9%, should have undergone pus sampling for bacteriological examination. In our series, only 41 patients underwent a leg X-ray: normal in 31 cases, bone involvement in 10 cases. This complication is formidable because germs lodged in bone structures are less accessible to antibiotic therapy. Management often requires surgical intervention; 2 cases were amputated in our series, representing 1.7%. Histological examinations were conducted in 32 out of 115 cases: no signs of malignancy were observed in 26 cases, or 22.6%, while signs of malignancy were present in 6 cases, or 5.2% (verrucous squamous cell carcinoma in 2 cases, differentiated keratinizing and infiltrating squamous cell carcinoma in 4 cases). Ulcers resistant to treatment, evolving over many years, have a risk of cancerization. However, they remain a rare yet not exceptional complication. Regarding vascular ulcers, Doppler ultrasound of the lower limbs was performed in 17 cases. Unlike in developed countries, Doppler ultrasound of the lower limb veins is not routinely performed in our regions due to its cost, which is not always accessible to all patients.
Therapeutic Aspects
All patients in our study received various types of local care. A potassium permanganate (KMnO4) bath of the affected limb before dressing was administered to disinfect the wound and facilitate healing. Skin grafting with success was performed in 80.9% of the cases to accelerate healing, strengthen the scar, and alleviate pain. We referred two cases to orthopedic surgery for amputation due to total necrosis of the affected limb. For treating infections, a combination of amoxicillin and clavulanic acid was used in 85% of the cases at the beginning of treatment, later replaced by another antibiotic sensitive according to the results of the antibiogram. In cases of clinical and/or biological anemia, iron supplementation was systematic. Tetanus vaccination was administered to all patients upon admission. Analgesics, multivitamins, antiparasitics, and anxiolytics were used as needed. The healing of leg ulcers often requires strict rest, which may only be achieved in a hospital setting. 32.5% of our patients were treated for a period equal to or longer than three months. However, any treatment exceeding three months further increases the already high cost of ulcer treatment.
Evolution
In our series, we observed 104 cases of favorable evolution (Figs. 5a – 5c), including 78 cases of complete healing, 11 cases of unfavorable evolution, including 2 cases of recurrence, 7 cases of complications, and 2 cases of stationary evolution. Thus, the therapeutic success was evaluated at 67.8% (complete healing). However, more than 1/4 of the patients (34 cases, 29.57%) were not reviewed after discharge.
CONCLUSION
At the end of our case study, it was clear that patient neglect or ignorance and the inadequacy of healthcare services were factors that had led the initial lesions to evolve into chronicity. Any ulceration of the lower limbs should be taken seriously by patients, healthcare professionals, and health authorities. Furthermore, chronic leg ulcers should receive early intervention to prevent dramatic complications.
ACKNOWLEDGMENTS
We would like to express our gratitude to the Director of the Dermatology Teaching Hospital of Bamako, Mali, as well as their staff, for their kind permission and assistance. We also extend our thanks to all clinical practitioners and patients for their collaboration.
Statement of Human and Animal Rights
All the procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the 2008 revision of the Declaration of Helsinki of 1975.
Statement of Informed Consent
Informed consent for participation in this study was obtained from all patients.
REFERENCES
1. Amblard P, Leccia MT. Leg ulcer. Encycl Méd Chir. 2001:16.
2. Begaud B. Epidemiology of leg ulcers. Ann Dermatol Venereol. 2002;129:1225-6.
3. Morrell CJ, Walters SJ, Dixon S, Collins KA, Brereton LM, Peters J, et al. Cost effectiveness of community leg ulcer clinics:Randomised controlled trial. BMJ. 1998;316:1487-91.
4. Franks PJ, Bosanquet N, Connolly M, Oldroyd MI, Moffatt CJ, Greenhalgh RM, et al. Venous ulcer healing:Effect of socioeconomic factors in London. J Epidemiol Community Health. 1995;49:385-8.
5. Nelzen O, Bergqvist D, Lindhagen A. Venous and non-venous leg ulcers:Clinical history and appearance in population study. Br J Surg. 1994;81:82-7.
6. Tanla JP. Leg ulcers. J Am Acad Dermatol. 1991:965-87.
7. Pierard GE, Franchimont C, Vardar M, Zaghloul A. Tropical ulcers. In:Pierard GE, Caumus E, Franchimont C, Arrese Estrada J. Tropical Dermatology. Brussels:Editions de L’Universite de Bruxelles/AUPELF. 1993:579-83.
8. Gheerert P, Song M. Clinical aspects of lower limb ulcers. Rev Med Brux. 1997;8:238-40.
9. Mazer A, Sankale M. Chronic ulcers of the lower limbs. Guide de Med. In Africa and the Indian Ocean, 1988;156:148-52.
10. Mahe A. Dermatology on dark skin. Pract Dermatol. 2001;159.
11. CisséF. Chronic ulcers of the lower limbs:Diagnostic and therapeutic possibilities. Med Thesis Bamako. 1990;74.
12. Kadri A. Chronic ulcers of the lower limbs:Epidemiological, clinical, etiological, and therapeutic aspects. Med Thesis Bamako. 2004;46-57.
Notes
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0001-7872-7937 http://orcid.org/0000-0001-7872-7937 http://orcid.org/0009-0003-3481-0968 http://orcid.org/0009-0003-3481-0968 |





Comments are closed.