Multiple squamous cell carcinomas complicating cocaine-induced morphea
Fatima Zahra Hashas , Hanane Baybay, Sokaina Chhiti, Zakia Douhi, Meryem Soughi, Sara Elloudi, Fatima-Zahra Mernissi
, Hanane Baybay, Sokaina Chhiti, Zakia Douhi, Meryem Soughi, Sara Elloudi, Fatima-Zahra Mernissi
Department of Dermatology, University Hospital Hassan II, Fes, Morocco.
Citation tools:
Copyright information
© Our Dermatology Online 2024. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
Localized cutaneous scleroderma, or morphea, is a highly heterogeneous group of autoimmune disorders that primarily affect the skin and adjacent tissues. Its pathogenesis remains unclear. Numerous factors, including genetics, drugs, infections, skin injuries, autoimmune diseases with abnormal cytokine production and/or such as vascular dysfunction, may play a role in the development of morphea. Fibrosis, inflammation, and chronic ulceration may ultimately contribute to skin neoplasia. Herein, we report a case of multiple metastatic squamous cell carcinomas complicating cocaine-induced morphea.
Key words: Squamous cell carcinoma, Induced scleroderma, Morphea, Drugs, Cocaine
INTRODUCTION
Morphea is a localized form of scleroderma that sometimes causes erosions and chronic ulcers on the skin. Herein, we report a case of multiple metastatic squamous cell carcinomas complicating cocaine-induced morphea.
CASE REPORT
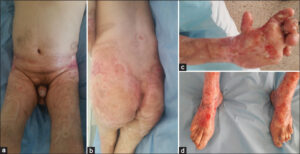
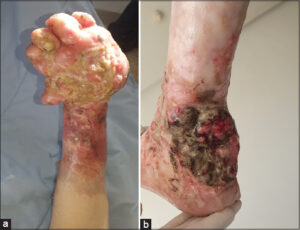
A 54-year-old patient had been a cocaine sniffer for 22 years. He had been suffering from rapidly extensive skin sclerosis for sixteen years without Raynaud’s phenomenon or other systemic signs. The initial clinical examination revealed scleroatrophic plaques on all four limbs and the trunk. The skin area was estimated at 50%. There were sclerodactyly and erosive plaques on the hands and feet, with synechiae and flessum of the limbs, resulting in functional impotence (Figs. 1a – 1d). Cocaine-induced generalized morphea was considered and immunosuppressive treatments were initiated. A combination of methotrexate and corticosteroids for six months did not yield an improvement, and the patient was put on imatinib. The evolution after two years was marked by the development of persistent erosions and ulcerations with hyper burgeoning, which led to taking a skin biopsy (Figs. 2a and 2b). A histological study confirmed the presence of a mature, well-differentiated squamous cell carcinoma with bone infiltration on the left hand and foot. An extension study revealed lymph node and lung metastases. The patient died before treatment was initiated.
DISCUSSION
Morphea, also known as llocalizeted scleroderma, is an inflammatory connective tissue disease with numerous clinical manifestations in adults and children. It is characterized by inflammation and fibrosis of the skin and underlying tissues, and sometimes even surrounding structures, such as the fasciae, muscles, bones, and the central nervous system [1].
Generalized morphea is characterized by at least four plaques measuring at least 3 cm that coalesce and affect two or more anatomical regions [2]. Although the etiology of the disease is unknown for certain, some stimuli (viruses, drugs, trauma) may cause vascular and immune dysfunction in genetically predisposed patients [1].
Cocaine is a potent vasoconstrictor agent that has been associated with the appearance of scleroderma syndromes characterized by diffuse cutaneous sclerosis and acral vasospasm with Raynaud’s phenomenon and a positive immunological assessment. Cocaine is known to produce vasoconstriction either by blocking the reuptake of norepinephrine and dopamine from the presynaptic space or by a direct vasoconstrictive effect independent of the vascular endothelium [3]. In our case, the diagnosis of cocaine-induced generalized morphea was retained given the negativity of the immunological and morphological workup and the chronological delay.
Malignant transformation of localized scleroderma is exceptionally rare and more associated with pansclerotic or generalized variants [4,5]. It occurs most often on the lower extremities of patients after a long evolution of the disease.
Immunosuppressive drugs used for the treatment of scleroderma may promote tumor formation [6]. Although carcinogenesis in scleroderma is a rare event, clinicians performing follow-up examinations should always be aware of the risk of tumor development on long-standing morphea lesions. In addition, common therapeutic strategies for morphea, such as immunosuppressive drugs and phototherapy, must be critically considered in light of their potential carcinogenic side effects.
CONCLUSION
Generalized morphea may be induced and maintained by cocaine as illustrated by our case. Although its malignant transformation is exceptionally rare, chronic ulcerations and hyper burgeoning should be examined with suspicion and benefit from histopathological evaluation at the slightest doubt.
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients gave their consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Papara C, De Luca DA, Bieber K, Vorobyev A, Ludwig RJ. Morphea:The 2023 update. Front Med (Lausanne). 2023;10:1108623.
2. Andreussi R, Silva LMB, da Silva HC, Luppino-Assad AP, Andrade DCO, Sampaio-Barros PD. Systemic sclerosis induced by the use of cocaine:Is there an association?Rheumatol Int. 2019;39:387-93.
3. Kilaru P, Kim W, Sequeira W. Cocaine and scleroderma:Is there an association?J Rheumatol. 1991;18:1753-5.
4. Saleh DB, Williams AM, Smith IM. Cutaneous squamous cell carcinoma arising within generalised morphea. J Plast Reconstr Aesthet Surg. 2011;64:149.
5. Boozalis E, Shah AA, Wigley F, Kang S, Kwatra SG. Morphea and systemic sclerosis are associated with an increased risk for melanoma and nonmelanoma skin cancer. J Am Acad Dermatol. 2019;80:1449-51.
6. Heck J, Olk J, Kneitz H, Hamm H, Goebeler M. Long-standing morphea and the risk of squamous cell carcinoma of the skin. J Dtsch Dermatol Ges. 2020;18:669-73.
Notes
Request permissions
If you wish to reuse any or all of this article please use the e-mail (contact@odermatol.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0002-5360-337X http://orcid.org/0000-0002-5360-337X http://orcid.org/0000-0003-3455-3810 http://orcid.org/0000-0003-3455-3810 http://orcid.org/0000-0002-5942-441X http://orcid.org/0000-0002-5942-441X |




Comments are closed.