Cutaneous Dubreuilh melanoma with ocular invasion
Siham Boularbah , Meryem Soughi, Zakia Douhi, Sara Elloudi, Hanane BayBay, Fatima Zahra Mernissi
, Meryem Soughi, Zakia Douhi, Sara Elloudi, Hanane BayBay, Fatima Zahra Mernissi
Department of Dermatology, University Hospital Hassan II, Fes, Morocco
Citation tools:
Copyright information
© Our Dermatology Online 2024. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
Sir,
Intraocular metastases of cutaneous melanoma are rare, mainly found in the choroid, rarely in the conjunctiva [1]. Herein, we study the case of a patient hospitalized for a cutaneous melanoma of Dubreuilh presenting with a conjunctival progression homolateral to the lesion.
An 82-year-old patient of clear phototype, reporting chronic sun exposure, consulted for a pigmented lesion on the left cheek, 5 cm in length, which had been evolving slowly for around seven years, with a central area more infiltrated and blackish (Fig. 1a). A biopsy established the diagnosis of Dubreuilh’s melanoma with a nodular component. A dermoscopic examination revealed a granular pattern, target appearance, and obliteration of the follicles (Fig. 1b). Ocular examination revealed a blackish pigmentation in the conjunctiva under the lower eyelid of the left eye (Fig. 1a). Ophthalmological examination and investigations confirmed the diagnosis of conjunctival progression of the cutaneous melanoma. An extension work-up revealed peri-umbilical permeation nodules. The patient was treated with chemotherapy.
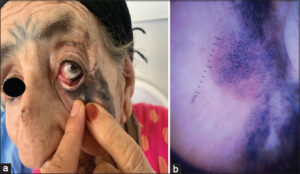 |
Figure 1: (a) Primary cutaneous Dubreuilh melanoma invading the lower eyelid and the ipsilateral ocular conjunctiva. (b) Dermoscopic image of Dubreuilh’s melanoma. |
Melanomas are malignant neoplasms that develop from dendritic melanocytes. Although the skin is the most common site of melanoma development, these neoplasms may occur in any tissue containing melanocytes. Ocular progression of a cutaneous melanoma is rare. Some studies suggest that the clear phototype, familial atypical mole syndrome, xeroderma pigmentosum, dysplastic nevi, and a family history of ocular melanoma may increase the risk of developing both cutaneous and ocular melanomas [2]. Our patient had conjunctival involvement, which may probably be explained by the surface progression of Dubreuilh’s melanoma, with the risk factors identified in our case being the light phototype and early and intensive exposure to the sun.
The fine and asymmetrical pigmentation of the follicular orifices in the lower part of the lesion is explained by the progression along the hair infundibulum of isolated or grouped melanocytic cells composed of dots, globules, then these structures fusing and becoming more homogeneous, sometimes bluish, progressively darkening the entire surface, even making the pilosebaceous orifices disappear in the upper part of the lesion. This dermoscopic aspect may explain the progression of the skin lesion toward the homolateral ocular conjunctiva [3–5].
Griech et al. reported that, in some cases, it was impossible to distinguish whether a tumor was of cutaneous or ocular origin, especially at the stage of metastasis [4,6]. Herein, the question may arise whether the tumors were related or had developed independently of each other, hence the interest in identifying the oncogenic mutation responsible for a tumor for diagnostic and therapeutic purposes when targeted therapies are available. In the case of our patient, ocular melanoma secondary to the progression of the cutaneous melanoma was easily diagnosed based on the following clinical criteria: the long-standing nature of her melanoma, the recent onset of visual disturbances, and the failure of the patient and her family to notice the pigmented ocular lesion.
In summary, dermatologists should also consider screening for ocular involvement in patients with the risk factors listed above with particular attention to the examination of the medial cantus region, eyelid folds, and conjunctiva by requesting a specialized ophthalmological examination to obtain an early diagnosis.
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients gave their consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Kaliki S, Shields CL. Uveal melanoma:Relatively rare but deadly cancer. Eye. 2017;31:241-57.
2. McDonald KA, Krema H, Chan A-W. Cutaneous signs and risk factors for ocular melanoma. J Am Acad Dermatol. 2021;84:1732-4.
3. Alexander DM, Kachiu CL, Kaveri K, Susan MS, Robert PD, Suephy C. Development of a pigmented facial lesion scale based on darkness and extent of lesions in older veterans. J Invest Dermatol. 2019;139:1185-7.
4. Valikodath NG, Rageh A, Materin MA. Pigmented corneal mass in a 59-year-old man with cutaneous melanoma. JAMA Ophthalmol. 2022 Sep 1;140:904-5.
5. El Hadj OE, Bouhajja L, Goucha A, Rekik W, El May A, Gamoudi A. Dubreuilh’s melanosis or malignant lentigo. Our Dermatol Online. 2017;8:231-2.
6. Saàdani CH, Gallouj S, Zinoune S, Senhaji G, Baybay H, Mernissi FZ, et al. Diffuse melanosis cutis secondary to metastatic malignant melanoma:Case report. Our Dermatol Online. 2019;10:79-81.
Notes
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0002-3975-8316 http://orcid.org/0000-0002-3975-8316 http://orcid.org/0000-0002-5942-441X http://orcid.org/0000-0002-5942-441X http://orcid.org/0000-0003-3455-3810 http://orcid.org/0000-0003-3455-3810 |




Comments are closed.