Takayasu’s arteritis: The case report of a sixty-year-old male with digital gangrene
Nada Bennouna , Fatimazahra Elfetouaki, Fouzia Hali, Soumiya Chiheb
, Fatimazahra Elfetouaki, Fouzia Hali, Soumiya Chiheb
Department of Dermatology and Venerology, Ibn Rochd University Hospital, Casablanca, Morocco
Citation tools:
Copyright information
© Our Dermatology Online 2024. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
Sir,
Takayasu arteritis (TA) is a chronic vasculitis of medium and large arteries, mainly affecting the aorta and its major branches, with a preponderance for young females during the second or third decades of life. It is an idiopathic granulomatous vasculitis of the aorta and its predominant branches and is one of the most widespread vasculitides [1]. Although it may take a variety of clinical presentations, digital ischemia has rarely been reported in large vessel vasculitis [2]. This case study aims to highlight the importance of screening for TA in male patients so that the diagnosis is not overlooked and adds more data to the limited literature on male patients.
A sixty-year-old male patient presented with brutal pain in the fingers associated with cyanosis. He had a history of high blood pressure, erythema nodosum three months previously, and no history of Raynaud’s phenomenon.
A clinical examination revealed a well-limited, necrotic lesion of the right middle finger, pulpal petechiae, and periungueal infarction with a prolonged capillary refill time (Fig. 1a).
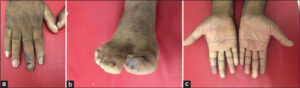 |
Figure 1: (a) Necrotic lesion on the middle finger. (b) Cyanosis of the big toe. (c) Pallor of the palmar side of the hands. |
Cyanosis, pallor, and coldness also was found on vascular examination with an abolition of the right and left ulnar pulses and asymmetric arterial blood pressure: 110/70 mmHg in the right arm and 130/85 mmHg in the left arm (Figs. 1b and 1c).
His full blood count and renal, liver, and thyroid functions were normal. Coagulation tests and total blood calcium and magnesium showed no abnormalities. ESR: 39 mm/h; CRP: 41 mg/L.
IgM anticardiolipin antibody, lupus anticoagulant, and antiBeta-2 glycoprotein IgG and IgM antibodies were negative. Antinuclear antibody, anti-dsDNA, cytoplasmic anti-neutrophil cytoplasmic antibodies, and perinuclear ANCA were negative as well.
Doppler ultrasound of the upper limbs revealed total thrombosis of the collateral of the right radial artery and of both ulnar arteries of the forearms. CT angiography showed total occlusion of both ulnar arteries.
Diagnosis of TA was retained according to ACR criteria, and a treatment of 1 g/day IV pulse of methylprednisolone was instore, then switched to oral prednisone combined with cyclophosphamide and the amputation of the distal phalanx of the third finger.
The evolution was a significant clinical recovery with the normalization of ESR and CRP and a follow-up appointment every month.
Our case presents the rare findings of a Moroccan male whose initial symptoms appeared at the age of six years. According to the American College of Rheumatology, the diagnosis may be reached if three of the six criteria are met, with our patient meeting four of them, They consist of claudication of the extremities; a decreased pulsation of one or both brachial arteries; a systolic blood pressure differential between the arms of at least 10 mmHg; arteriographic narrowing or occlusion of the whole aorta, its primary branches, or large arteries in the upper or lower limbs excluding arteriosclerosis, fibromuscular dysplasia, or other causes [3].
Due to the non-specific clinical presentations, the diagnosis of Takayasu’s arteritis is delayed or missed. In the case of our patient, the initial clue to the diagnosis was the unilateral necrotic lesion on the finger, and there have been only three similar cases reported in the literature [4].
Research conducted so far has reported that the occurrence of digital gangrene in AT is localized only in the lower limbs. Furthermore, the incidence of symptomatic digital gangrene in the upper limb is infrequent, owing to the high abundance of collaterals and the limited extent of atherosclerosis in the upper limb. Thus, the development of digital gangrene in the upper extremity in association with TA, as occurred in our patient, is a remarkably rare finding. For appropriate diagnosis and treatment of patients presenting with digital gangrene, one should always take Takayasu arteritis into consideration.
ACKNOWLEDGMENT
We would like to thank Nada Bennouna, Department of Dermatology and Venerology, Ibn Rochd University Hospital, Casablanca, Morocco.
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients gave their consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Russo RAG, Katsicas MM. Takayasu arteritis. Front Pediatr. 2018;6:265.
2. Lau RA, Bains R, Suraweera D, Ma J, Heinze ER, Wong AL, et al. A rare case of digital ischemia and gangrene in ANCA-associated vasculitis with review of the literature. Case Rep Rheumatol. 2017;2017:2421760.
3. Maffei S, Di Renzo M, Bova G, Auteri A, Pasqui AL. Takayasu’s arteritis:A review of the literature. Intern Emerg Med. 2006;1:105-12.
4. Kaditis AG, Nelson AM, Driscoll DJ. Takayasu’s arteritis presenting with unilateral digital clubbing. J Rheumatol. 1995;22:2346-8.
Notes
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
|




Comments are closed.