Zoster eruption in COVID-19 multiple-shot vaccinated patients: A report of two cases
Laurent Dupoirieux
Department of Plastic Surgery, 74 avenue Jean Jaures 47200 Marmande, France
Citation tools:
Copyright information
© Our Dermatology Online 2023. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
Herein, we present two cases of COVID-19 multi-shot vaccinated patients (four and five doses) who developed a zoster eruption after receiving the last injection. Fortunately, the outcome of these patients was favorable. However, the increasing incidence of these adverse reactions suggests a relationship with COVID-19 vaccines and raises serious concerns about the safety of repeated COVID-19 vaccine injections. If possible, heterologous vaccination should also be avoided and careful observation by health agencies should be undertaken. Several patients have also reported unusual skin reactions, such as rash or itching, that they had not observed before COVID-19 vaccinations.
Key words: COVID-19 vaccination, Zoster eruption, Multiple doses
INTRODUCTION
After the introduction of the first COVID-19 vaccines, only limited information on adverse reactions was available from laboratories. However, with the introduction of open sources for the declarations of these adverse effects, we have now a more accurate scope of these complications. Among these complications dermatologic reactions are frequent, and most are mild or moderate [1]. Although it was not the most frequent dermatologic complication, we had already reported one case of zoster eruption after the AstraZeneca vaccine at the beginning of the pandemic after the first injection [2], yet we now observed two other cases in a different context as they had received multiple COVID-19 vaccine shots; these are presented in this paper.
CASE REPORTS
Case 1
A sixty-year-old French female living in Switzerland visited our office for a painful left thoracic eruption that appeared several days before following approximately the D7-D8 dermatome. The multiple crusty vesicles were typical of a zoster infection (Fig. 1). She had received a four-dose heterologous COVID-19 vaccine scheme with three Moderna doses in Switzerland and one Comirnaty dose in France. The time between the last injection and the eruption was six weeks. In her medical history, she had breast cancer treated in 2018 by hormonotherapy. She tested positive for COVID-19 after the second vaccine dose, and she mentioned no history of an allergy or previous zoster infection. A biological investigation revealed no perturbation in the hemogram (leucocytes at 6.14 G/L with 36.2% of lymphocytes). The D-dimer level was at 486 mg/L. Treatment with aciclovir at 200 mg (five tablets per day) for seven days was prescribed, and she healed normally without residual neuralgia. The French health authority was informed about the incident.
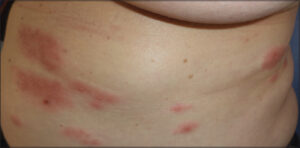 |
Figure 1: Lateral left thoracic eruption with multiple vesicles and marked erythema. |
Case 2
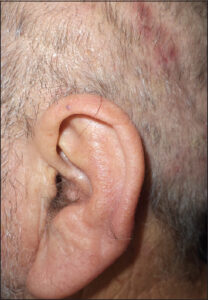
An 81-year-old male patient visited our office for a painful left ear for the previous ten days. During the clinical examination, a parietal eruption above the ear following the direction of the Arnold’s occipital nerve was noticed (Fig. 2). The left ear was swollen and extremely sensitive. The patient mentioned only cardiac arrhythmia in his medical history yet no allergy or previous zoster infection. A biological investigation revealed no inflammatory reaction with the D-dimer level at 316 mg/L. Treatment with aciclovir 200 mg (five tablets per day) was undertaken for seven days. The lesions healed rapidly after the treatment, yet he developed basal cell carcinoma on the left temporal skin several weeks later, which is currently under treatment. The French health authority was informed about the incident.
DISCUSSION
Adverse cutaneous reactions after COVID-19 vaccines are now well documented [3]. Most of the cutaneous reactions are immediate and limited to the point of injection, usual after any type of vaccine, yet delayed reactions such as multiple COVID-18 arms or V-REPP (vaccine-related eruption of papules and plaques) may be impressive, as described by a French survey on 192 patients [4].
In the OpenVAERS database, shingles is the most frequently declared dermatologic complication (15,721 cases as of May 19, 2023). Relative to the number of COVID-19 vaccines administered around the world, this is a low incidence, yet it is likely that the number of cases is underestimated. Furthermore, there are increasing reports of herpes zoster reactivation with COVID-19 vaccines in the medical literature [5]. Other epidemiologic data extracted from OpenVAERS reveal a double incidence in Comirnaty vaccinated patients. However, this is to be expected as the vaccine has been the most frequently injected in the world. Another relevant epidemiological data is that there is now a worldwide report of post-vaccinal zoster eruptions on all populations with all types of vaccines. Furthermore, an additional problem raised by the first case is the difficulty to attribute the origin of the complication with patients receiving a heterologous vaccination, and this problem is recurrent in other complications with COVID-19 vaccines. Thus, we recommend using the same type of vaccine for a booster injection. Our two cases raise two other questions.
The first is whether there is a relationship between COVID-19 vaccines and zoster eruption. To address this question, the onset time of the eruption must be carefully studied. As most appear between five and ten days of the last injection [5], the likelihood of a relationship was debatable in our first case as it appeared six weeks after the injection yet cannot be rejected. She had received an atypic vaccination scheme and there was no reference for this case in the medical literature.
The second question is whether there is an increasing incidence of zoster in the case of COVID-19 vaccines. It is extremely difficult to demonstrate this even with meta-analysis as there is no register of zoster cases in the general population and, thus, no control group [6–8]. However, a recent well-designed study with two matched cohorts has demonstrated a statistical increase in zoster eruptions in COVID-19 vaccinated patients [9]. Our real-life practice also questioned us as we had already observed four cases in an area of 100,000 residents since the beginning of the pandemic, yet none three years before.
In conclusion, we have observed in our daily practice an unusual occurrence of zoster eruption. These clinical observations suggested a possible link between COVID-19 vaccines and zoster eruption or its reactivation. Fortunately, these zoster eruptions had a favorable outcome with a standard treatment, yet general practitioners and dermatologists should be aware of this adverse effect to avoid a misleading diagnosis and introduce the appropriate treatment rapidly.
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients gave their consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Qaderi Q, Golezar MH, Mardani A, Mallah MA, Moradi B, Kavoussi H, et al. Cutaneous adverse reactions of COVID-19 vaccines:A systematic review. Dermatol Ther. 2022;35:e15391.
2. Dupoirieux L. Zoster infection after vaccination with the AstraZeneca COVID-19 vaccine:A case report. Our Dermatol Online. 2022;13:45-6.
3. Burlando M, Herzum A, Micalizzi C, Cozzani E, Parodi A. Cutaneous reactions to COVID-19 vaccine at the dermatology primary care. Immun Inflamm Dis. 2022;10:265-71.
4. Darrigade AS, Oules B, Sohier P, Jullie ML, Moguelet P, Barbaud A, et al. Sweet-like syndrome and multiple COVID arm syndrome following COVID-19 vaccines:’Specific’patterns in a series of 192 patients. Br J Dermatol. 2022;2:10.1111/bjd.21692.
5. Katsikas Triantafyllidis K, Giannos P, Mian IT, Kyrtsonis G, Kechagias KS. Varicella zoster virus reactivation following COVID-19 vaccination:A systematic review of case reports. Vaccines. 2021;9:1013.
6. Desai HD, Sharma K, Shah A, Patoliya J, Patil A, Hooshanginezhad Z, et al. Can SARS-CoV-2 vaccine increase the risk of reactivation of Varicella zoster?A systematic review. J Cosmet Dermatol. 2021;20:3350-61.
7. Akpandak I, Miller C, Sun Y, Arnold BF, Daniel Kelly J, Acharya NR. Assessment of herpes zoster risk among recipients of COVID-19 vaccine. JAMA Network Open. 2022;5:e2242240.
8. Préta LH, Contejean A, Salvo F, Treluyer JM, Charlier C, Chouchana L. Association study between herpes zoster reporting and mRNA COVID-19 vaccines (BNT162b2 and mRNA-1273). Br J Clin Pharmacol. 2022;88:3529-34.
9. Hertel M, Heiland M, Nahles S, von Laffert M, Mura C, Bourne PE, et al. Real-world evidence from over one million COVID-19 vaccinations is consistent with reactivation of the varicella-zoster virus. J Eur Acad Dermatol Venereol. 2022;36:1342-8.
Notes
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0001-8472-3262 http://orcid.org/0000-0001-8472-3262 |




Comments are closed.