Thromboembolic disease in a patient treated with bleomycin for endemic Kaposi’s disease at the Bamako Dermatology Hospital in Mali
Savané Moussa 1,2,5, Binta Guindo1, Alimata Keita1, Mamoudou Diakité1, Mamadou Gassama1,2, Youssouf Fofana3, Yamoussa Karabinta1,2, Labassou Dissa1, Nkesu Yannick Mukendi1, Adama A Dicko1,2, Mohamed Cissé4,5, Ousmane Faye1,2
1,2,5, Binta Guindo1, Alimata Keita1, Mamoudou Diakité1, Mamadou Gassama1,2, Youssouf Fofana3, Yamoussa Karabinta1,2, Labassou Dissa1, Nkesu Yannick Mukendi1, Adama A Dicko1,2, Mohamed Cissé4,5, Ousmane Faye1,2
1Department of Dermatology, Hospital of dermatology of Bamako, Bamako, Mali, 2Faculty of Medicine, University of Bamako, Bamako, Mali, 3Sominé Dolo Hospital of Mopti, Mopti, Mali, 4Faculty of Health Sciences and Technics, Conakry, Guinea, 5Donka National Hospital, Conakry, Guinea
Citation tools:
Copyright information
© Our Dermatology Online 2023. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
Herein, we report a case of thromboembolic disease occurring during endemic Kaposi’s disease treated with bleomycin. Kaposi’s disease is a vascular and fibroblastic disorder caused by human herpes virus type 8. The endemic form remains prevalent yet with a less severe prognosis. The first line of systemic treatment in our country is classically a monotherapy with bleomycin. This case of endemic Kaposi’s disease was treated with bleomycin monotherapy that reportedly caused thromboembolic disease on two occasions after administration. This was one of the rarely reported effects of bleomycin in monochemotherapy, especially in the case of the treatment of endemic Kaposi’s disease, considering the chronology of the appearance of this effect in your patient.
Key words: Bleomycin; Thromboembolic disease; Endemic Kaposi’s disease
INTRODUCTION
Kaposi’s disease is a vascular and fibroblastic disease caused by human herpes virus type 8 discovered in 1994 by Chang in the U.S. There are four clinical forms: the epidemic form, the endemic or African form, the classical or Mediterranean form, and the form related to iatrogenic immunosuppression. The endemic form remains prevalent yet with a less severe prognosis, and mainly affects the elderly with the elective involvement of the lower limbs [1].
The treatment of Kaposi’s disease, depending on the size and number of lesions, combines the restoration of immunity (antiretrovirals), local treatments (surgery, radiotherapy), and general treatments (chemotherapy) in the case of extensive lesions [2].
Antineoplastic therapies (hormones, chemotherapy, or radiotherapy) may also increase the risk of thrombosis [3]. The first line of systemic treatment is usually a monotherapy with bleomycin, which is a cytotoxic antibiotic. The most important adverse effect of bleomycin is pulmonary fibrosis, which may be fatal in 1% of cases [2]. Thromboembolic events with bleomycin are usually reported in combination with other anticancer drugs yet are rarely reported alone. Herein, we report a case of thromboembolic disease occurring during endemic Kaposi’s disease treated with bleomycin.
CASE REPORT
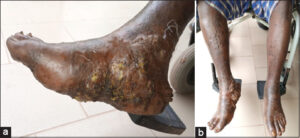
Endemic Kaposi’s disease, which began seven years previously, was diagnosed in a 58-year-old cattle breeder from Kayes (region of Mali, 600 km from Bamako) with an altered general condition, a Karnofsky index of 50%, and a BMI of 17.72. The skin involvement was diffuse with ulcerated angiomatous nodules on the right plantar area (Figs. 1a and 1b). An X-ray of the foot revealed chronic osteitis related to Kaposi’s disease. A pulmonary X-ray showed no particularity. We found no immunosuppression (no immunosuppressive treatments, negative HIV testing, normal blood sugar). CBC showed an anemia of 8 g/dL, normocytic hypochromic, with platelets at 197 G/l. A skin biopsy showed that the dermis was the site of a tumor proliferation taking a nodular aspect. It consisted of spindle cell patches alternating with a vascular proliferation. Vascular clefts with erythrodiapedesis were noted. The rest of the examination was normal. After correcting the anemia, which returned to 10.7 g/dL, treatment with bleomycin infusion of 15 mg every fifteen days was initiated on 09/06/2020. The evolution was marked 48 hours after the first administration by a painful, hot swelling of the right leg and a fever of 38.8°C. In front of this picture, erysipelas with ulcerated angiomatous nodules on the sole of the right foot and phlebitis were evoked. The patient received intravenous cefotaxime 3 g/d, and a workup was performed with the following particularities: D-dimer at 3343.63 ng/mL, PT at 60.60%, and Doppler echocardiography showing deep venous thrombosis in the affected limb involving the right femoro-tibio-peroneal trunk, and superficial thrombosis of the right leg. This clinical picture of thrombosis was treated with enoxaparin 8000 IU per day for six days and, then, relayed by warfarin 5 mg per day and elastic restraint with controls of the INR. Three weeks after clinical and biological improvement of the deep vein thrombosis, it was decided to continue with intramuscular bleomycin by the second dose of 15 mg (30/06/2020), which resulted in the same clinical picture within 48 hours as the first dose of bleomycin, this time accompanied by respiratory distress (pulmonary embolism), which rapidly led to the death of the patient (03/07/2020).
DISCUSSION
In view of the chronology of onset of thromboembolic disease in our patient and its occurrence on two occasions after the administration of 15 mg of bleomycin, we can say that this case was strongly suggestive of an adverse drug reaction. In a study by Yamamoto et al., the mean time between the administration of the treatment (bleomycin) and the appearance of the rash (flagellate erythema) varied from several hours to six months [4]. Although bleomycin has been cited to be a thrombogen in combination with other anticancer drugs, yet alone as monotherapy in the treatment of endemic Kaposi’s disease, it has never been reported in the literature to our knowledge. The annual incidence of symptomatic venous thrombosis in these patients is on average 11%, yet this is largely underestimated [5]. Cancer increases the risk of thrombosis by a factor of four when compared to the general population and by a factor of six in the case of associated chemotherapy treatment [6,11]. This was the case in our patient with endemic Kaposi’s disease treated with bleomycin. In addition, prolonged bed resting required prophylaxis of thromboembolic disease with low-dose acetylsalicylic acid (100 mg per day) during his hospitalization. Other risk factors, such as a platelet count greater than 350 G/L, a hemoglobin level below 10 g/dL, and the use of leukocyte growth factors or erythropoietin, were absent. Bleomycin, originally extracted from the fungus Streptomyces verticillus [7], is a molecule with both antibiotic and cytotoxic properties. Its oxidative power is indeed involved in the generation of DNA breaks, leading to cell death [8]. It is indicated in the treatment of various cancers: squamous cell carcinomas, malignant lymphomas, and germ cell tumors. More secondarily, it is employed as a topical treatment for keloid scars and plantar warts [9]. The mechanisms of thrombosis are multiple: an acquired deficiency in physiological inhibitors (antithrombin, proteins C and S), toxicity to normal cells (endothelium), and lysis of tumor cells. Its main side effects are the risk of pulmonary fibrosis, transient hyperthermic reactions shortly after injection, and skin manifestations, such as melanoderma, often predictive of pulmonary fibrosis [9]. In our case, we excluded prolonged bed resting as a possible cause of thromboembolic disease as the patient during hospitalization was on prophylaxis with acetylsalicylic acid 100 mg daily. Kaposi’s disease was also excluded because the patient had been living with his disease for seven years before coming to the clinic. Given the suggestive chronology, it seems reasonable to attribute this effect to bleomycin. The imputability score according to the French pharmacovigilance method was employed [10].
This original observation was, to our knowledge, the first published case of thromboembolic disease occurring during bleomycin monotherapy for endemic Kaposi’s disease.
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients gave their consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Maodo N, Assane D, Siritio B, Moussa D, Sara M, Ahy DB, et al. Endemic Kaposi disease in Dakar:Study of 29 cases. Mali Med. 2014;29:10-4.
2. Laschinski B, Arnault J.-P, Gras-Champel V. Tinnitus in a patient treated with bleomycin for Kaposi’s sarcoma. Therapy. 2015;70:539-40.
3. Elalamy I, Verdy E, Gerotziafas G, Hatmi M. Pathophysiology of venous thromboembolic disease during cancer. Pathol Biol. 2008;56:184-94.
4. Yamamoto T, Nishioka K. Flagellar erythema. Int J Dermatol. 2006;45:627-31.
5. Otten HM, Mathijssen J, ten Cate H, Soesan M, Inghels M, Richel DJ, et al. Symptomatic venous thromboembolism in cancer patients treated with chemotherapy:an underestimated phenomenon. Arch Intern Med. 2004;164:190-4.
6. Heit JA, Silverstein MD, Mohr DN, Petterson TM, O’Fallon WM, Melton 3rd LJ. Risk factors for deep vein thrombosis and pulmonary embolism:A population-based case-control study. Arch Intern Med. 2000;160:809-15.
7. Umezawa H, Maeda K, Takeuchi T, Okami Y. New antibiotics, bleomycin A and B. J Antibiot. 1966;19:200-9.
8. Burger RM, Peisach J, Horwitz SB. Activated bleomycin:A transient complex of drug, iron and oxygen that degrades DNA. J Biol Chem. 1981;256:11636-44.
9. Pasquet F, Pavic M, Estival JL, Karkowski L, Debourdeau P. Flagellar erythema:A rare complication of bleomycin. Med Interne. 2009;30:637-9.
10. Arimone Y, Bidault I, Dutertre JP, Gérardin M, Guy C, Haramburu F, et al. Update of the French method of imputability of adverse drug reactions. Therapy. 2011;66:517-25.
11. Descourt R, Jezequel P, Couturaud F, Leroyer C, Girard P. Thromboembolic venous disease and cancer. Rev Pneumol Clin. 2008;64:282-9.
Notes
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0003-3149-2987 http://orcid.org/0000-0003-3149-2987 |




Comments are closed.