Efficacy of propranolol in severe segmental infantile hemangioma of the face
Boh Fanta Diané 1, Thierno Mamadou Tounkara1, M’Mah Aminata Bangoura2, Mohamed Maciré Soumah1, Fatimata Keita1, Mamadou Diouldé Kanté1, Moussa Keita1, Moussa Savané1, Mariame Touré1, Houleymatou Baldé1, Mohamed Cissé1
1, Thierno Mamadou Tounkara1, M’Mah Aminata Bangoura2, Mohamed Maciré Soumah1, Fatimata Keita1, Mamadou Diouldé Kanté1, Moussa Keita1, Moussa Savané1, Mariame Touré1, Houleymatou Baldé1, Mohamed Cissé1
1Dermatology-Venereology Department, CHU Donka, Conakry, Guinea, 2Department of Pediatrics, CHU Donka, Conakry, Guinea
Citation tools:
Copyright information
© Our Dermatology Online 2022. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
Infantile hemangioma (IH) is the most common benign vascular tumor of childhood. Most of IHs regress spontaneously, yet some require a more rapid intervention. Herein, we report the case of a two-month-old female who was brought in for consultation by the mother with a voluminous segmental IH of the face in respiratory distress. The infant was hospitalized, after taking advice from other specialists and performing a pre-treatment check-up, the patient was administered oral propranolol. Respiration returned to normal after several hours. The evolution was marked by the regression of the hemangioma and positive drug tolerance. Our observation shows the value of early diagnosis and the need for the rapid management of severe segmental IH of the face treated with oral propranolol. Apart from the efficacy of propranolol in the treatment of IH, we report the difficulties due to the unavailability of the adapted syrup form for infants in Guinea.
Key words: Segmental hemangioma; Infants; Propranolol
INTRODUCTION
Infantile hemangioma (IH) is the most common benign vascular tumor of childhood [1,2]. The growth of hemangiomas is characteristic: invisible at birth, then proliferation from 2-6 weeks with rapid growth for 3-9 months, followed by a plateau phase and finally spontaneous regression from about the second year for several years [3–5]. Depending on its volume and/or topography, hemangiomas may lead to complications that warrant specific therapeutic management [3]. If there is a vital, functional, and/or esthetic risk, first-line treatment is based on propranolol, which is rapidly effective and well-tolerated in children [4,6]. Herein, we report the case of a two-month-old female brought by her mother for a large segmental hemangioma of the face, which we treated with propranolol tablets.
CASE REPORT
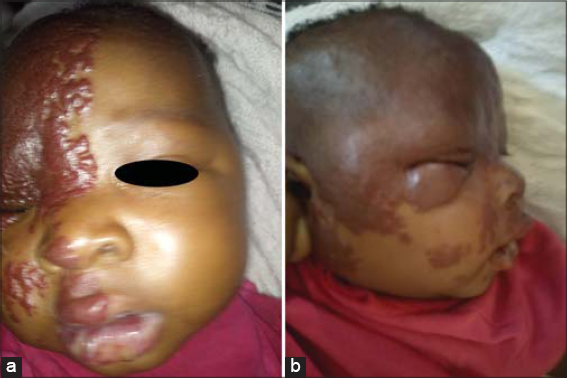
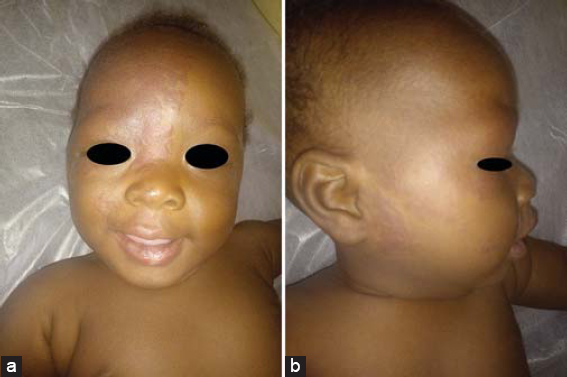
The patient was a two-month-old female who had been seen in consultation for tumor-like lesions on the face, which had been progressing since birth and with dyspnea. The history revealed that she was the fourth of four siblings, born to a 27-year-old mother from a full-term pregnancy and eutocic delivery. A physical examination revealed a dark red tumor cupboard with sharp edges, of geographical contour and firm and elastic consistency, sitting on the right hemiface with palpebral edema, preventing the opening of the right eye, overflowing on the right side of the neck with spaces of healthy skin. The half-mucous membranes and labial mucous membranes were the sites of the same lesions. In view of these localizations, we requested a multidisciplinary consultation. The ophthalmologic consultation concluded that there was sub-palpebral injury with an amblyogenic risk. The otolaryngology consultation revealed a localization of the hemangioma lesions in the right nasal fossa causing the respiratory difficulty. The rest of the otolaryngology examination was without particularity. On pediatric consultation, the anthropometric parameters were normal, yet noted the presence of dyspnea with a respiratory frequency of 67 cycles per minute. In view of this clinical presentation, we retained the diagnosis of severe segmental infantile hemangioma of the face in the proliferative phase (Figs. 1a and 1b), and the infant was hospitalized. The assessment, including cardiac ultrasound, blood glucose, and blood count, was normal. Treatment with propranolol tablets crushed in a small amount of water was immediately initiated at a dose of 1 mg/kg/day two times a day (May 2019). The hours following the administration of propranolol were marked by the disappearance of dyspnea. We increased the dose to 2 mg/kg/day two times a day at the second week of treatment. The infant was discharged after two weeks of hospitalization. The dose of propranolol was increased and maintained at 3 mg/kg/day starting from the third week of treatment. The infant returned for blood pressure and glycemic control once weekly for the next month and then once every two weeks. We noted a rapid regression of the palpebral hemangioma with a decrease in palpebral edema in the early months (Figs. 2a and 2b). At the fourth month of treatment, the hemangioma almost regressed and a discreetly hyperpigmented macular cupboard remained in place (Figs. 3a and 3b) with no adverse effects.
DISCUSSION
Our observation illustrates the value of early diagnosis and the need for making early therapeutic decisions in the case of severe segmental infantile hemangioma of the face in the proliferative phase with a vital, functional, and esthetic risk, which has progressed favorably under oral propranolol. Infantile hemangioma (IH) is the most common tumor in children in all locations [1,7,8]. Despite its benign and spontaneously favorable evolution, its prognosis may sometimes be severe in terms of function (palpebral or labial localizations), aesthetics (thoracic localization in young females), but also vital (bleeding, damage to the respiratory axis) [7]. The growth of IH is rapid, usually during the first three months, yet may last until the sixth or eighth month in superffcial forms, and until the ninth or twelfth month in deep involvement forms. In rare cases, particularly in segmental IH, it may extend to the twenty-fourth month [4]. IH eventually stabilizes spontaneously, then a regression over several months or years is observed. The involution is slow and progressive and results in the appearance of central bleaching of the superficial lesions and sagging of the subcutaneous components [2,4,9]. There is little known about the regulators of hemangioma proliferation and involution. During the growth phase, angiogenesis is stimulated by the basic fibroblast growth factor (bFGF) and the vascular endothelial growth factor (VEGF). In this proliferation phase, histology reveals active endothelial and interstitial cell division; in the involutional phase, however, apoptosis of these groups of cells is observed [4,10–13]. There are four main indications for the treatment of childhood hemangiomas. Those with a topography and/or volume that may be life-threatening, those that may entail a functional risk (periorbital region), those that may be painful in the case of ulcerated hemangiomas, and those that have an especially high risk of mutilating sequelae with major long-term aesthetic repercussions, particularly in periorificial localizations [10]. Our case concerned the palpebral region with a limitation of the opening of the right eye, which may lead to amblyopia, damage to the mucous membrane and the labial half-mucous membrane hindering sucking (functional risk), damage to the right nasal fossa leading to respiratory difficulty (vital risk), and facial localization and the size and appearance of the lesions (aesthetic risk). All infants with this type of hemangioma must be treated imperatively with oral propranolol, which is the first-line treatment, rapidly effective and well-tolerated in children, as several authors indicate [4,5,13–15]. Since the publication in the New England Journal of Medicine in 2008 [16], reporting the efficacy of propranolol on eleven complicated cases of IH, this fortuitous discovery prompted physicians in different countries to test this treatment on complicated IH. Thus, a multitude of retrospective [17], prospective [14], and multicentric [18] studies have been published after this original article confirming the treatment’s efficacy on complicated IH. Noukeu et al. [3] described a case of favorably evolving sub-palpebral hemangioma under oral propranolol. Yilmaz et al. [1] reported, in their study on 25 cases of complicated hemangiomas, 18 parents (21, 86%) with a highly favorable perception and 3 parents (21, 14%) with a favorable perception of the efficacy of treatment and the evolution of IH. Our observation is related to the data in the literature [4,5,9,13,15,19], which reports that the initiation of treatment should be early and progressive (with a starting dose of 1 mg/kg/day increased in steps to reach an effective dose of 2-3 mg/kg/day). As the oral solution of propranolol is unavailable in our country, we used the tablet form to be dissolved in water in a fraction equivalent to the infant’s dosage. The compliance of the parents allowed us to obtain a satisfactory result.
CONCLUSION
Propranolol transformed the prognosis and management of severe segmental facial IH. Therapeutic success is nevertheless based on early treatment. Although the oral solution of propranolol is not yet available in our country, the tablet remains a therapeutic alternative with satisfactory results. The HEMANGIOL 3.75 mg/mL oral solution (propranolol) specialty received a positive opinion from the Committee for Medicinal Products for Human Use (CHMP) on February 20, 2014, and a marketing authorization (MA) on April 23, 2014, accompanied by a risk management plan (RMP) and risk minimization measures in Europe. A study on a larger sample would be necessary to assess the efficacy and tolerance of this presentation of propranolol.
Statement of Human and Animal Rights
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2008.
Statement of Informed Consent
Informed consent was obtained from both parents to be included in the study
REFERENCES
1. Yilmaz L, Dangoisse C, Semaille P. [Infantile hemangioma:A new indication for propranolol? Retrospective study:A case-series of 25 infants]. Rev Med Brux. 2015;36:3-9.
2. Chang LC, Haggstrom AN, Drolet BA, Baselga E, Chamlin SL, Garzon MC, et al. Growth characteristics of infantile hemangiomas:Implications for management. Pediatrics. 2008;122:360-7.
3. Noukeu ND, Ebana SR, Enyama D, Meguieze CA, Koum DK. Efficacitédu propanolol dans l’hemangiome sous palpebral chez un nourrisson de 4 mois. Health Sci Dis. 2017;18(2 Suppl):1-2.
4. Léauté-Labréze C. [Infantile hemangioma:Update and treatment]. Arch Pédiatrie. 2013;20:517-22.
5. Léauté-Labréze C, Harper JI, Hoeger PH. Infantile haemangioma. Lancet. 2017;390:85-94.
6. Léauté-Labréze C. [Propranolol in infantile hemangiomas]. Arch Pediatr. 2015;22:452-5.
7. Leboulanger N, Cox A, Garabedian E-N, Denoyelle F. Hémangiomes infantiles et b-bloquants en ORL. Tribol Int-TRIBOL INT. 2011;128:279-83.
8. Fernandez-Pineda I, Williams R, Ortega-Laureano L, Jones R. Cardiovascular drugs in the treatment of infantile hemangioma. World J Cardiol. 2016;8:74-80.
9. Yilmaz L, Dangoisse C, Semaille P. [Infantile hemangioma and propranolol:A therapeutic „revolution”. Literature review]. Rev Med Brux. 2013;34:479-84.
10. Itinteang T, Withers AHJ, Davis PF, Tan ST. Biology of infantile hemangioma. Front Surg. 2014;1:38.
11. Greenberger S, Bischoff J. Infantile hemangioma:Mechanism(s) of drug action on a vascular tumor. Cold Spring Harb Perspect Med. 2011;1:a006460.
12. Bota M, Popa G, Blag C, Tataru A. Infantile hemangioma:A brief review. Clujul Med. 2015;88:23-7.
13. Delmotte N, Curti C, Montana M, Crozet M, Vanelle P, Gensollen S. News on infantile hemangioma therapy by beta-blocker. Thérapie. 2012;67:257-65.
14. Laranjo S, Costa G, Paramés F, Freitas I, Martins JD, Trigo C, et al. The role of propranolol in the treatment of infantile hemangioma. Rev Port Cardiol Engl Ed. 2014;33:289-95.
15. Hoeger PH, Harper JI, Baselga E, Bonnet D, Boon LM, Atti MCD, et al. Treatment of infantile haemangiomas:Recommendations of a European expert group. Eur J Pediatr. 2015;174:855-65.
16. Léauté-Labreze C, Dumas de la Roque E, Hubiche T, Boralevi F, Thambo J-B, Taeeb A. Propranolol for severe hemangiomas of infancy. N Engl J Med. 2008;358:2649-51.
17. Saka B, Téclessou J, Akakpo S, Mahamadou G, Mouhari-Toure A, Soga Gottara W, et al. [Treatment of infantile hemangioma in Togo]. Ann Dermatol Vénéréol. 2018;145:790-2.
18. Uthurriague C, Boccara O, Catteau B, Léauté-Labreze C, Chiaverini C, Maruani A, et al. Hémangiome cutanédes voies aériennes: pattern cutanéassocié. Ann Dermatol Vénéréol. 2015;142:S539.
19. Broeks IJ, Hermans DJJ, Dassel ACM, van der Vleuten CJM, van Beynum IM. Propranolol treatment in life-threatening airway hemangiomas:A case series and review of literature. Int J Pediatr Otorhinolaryngol. 2013;77:1791-800.
Notes
Source of Support: Nil,
Conflict of Interest: The authors have no conflict of interest to declare.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0003-1371-5198 http://orcid.org/0000-0003-1371-5198 |




Comments are closed.