Zinc-responsive acral hyperkeratotic dermatosis
Ritu Rani1, Reena K Sharma 1, Mudita Gupta2
1, Mudita Gupta2
1Department of Dermatology, Civil Hospital Kangra, H.P., India, 2Department of Dermatology, IGMC Shimla, H.P., India
Corresponding author: Reena K Sharma, MD
Submission: 05.05.2021; Acceptance: 02.11.2021
DOI: 10.7241/ourd.20223.17
Cite this article: Rani R, Sharma RK, Gupta M. Zinc-responsive acral hyperkeratotic dermatosis. Our Dermatol Online. 2022;13(3):308-310
Citation tools:
Copyright information
© Our Dermatology Online 2022. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
Zinc-responsive acral dermatitis is a rare entity characterized by chronic, persistent, well-defined, hyperpigmented, and hyperkeratotic plaques on the acral regions of the body. One needs to differentiate this disease from its close differentials such as necrolytic migratory erythema and pellagra. Herein, we report a case of zinc-responsive acral hyperkeratotic dermatosis in a 35-year-old female previously treated with multiple topical drugs without any significant improvement. The diagnosis of zinc-responsive dermatosis should be kept in mind in the case of treatment-refractory, hyperpigmented plaques on the hands and feet.
Key words: Acral hyperkeratosis; Necrolytic migratory erythema; Zinc
INTRODUCTION
Zinc-responsive acral dermatitis is a rare clinical disorder with distinctive clinical features showing a significant response to oral zinc therapy. Clinically, it is characterized by well-defined, hyperpigmented, hyperkeratotic plaques distributed symmetrically on the acral regions of the body [1]. Herein, we describe the case of a 35-year-old female presenting with hyperpigmented plaques on the dorsa of the hands and feet responsive to oral zinc therapy.
CASE REPORT
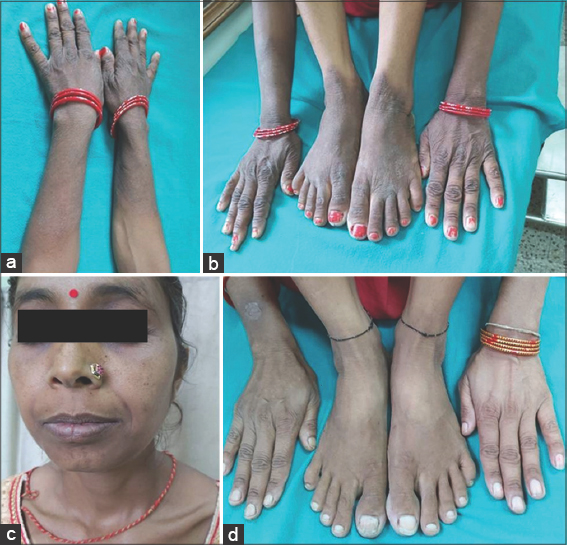
A 35-year-old female presented with persistent darkening and thickening of the hands and feet for the last two years and a history of multiple consultations and being treated with topical steroids, tacrolimus, vitamin D analogs, and antihistamines but without improvement. On clinical examination, the lesions were well-defined, hyperpigmented, hyperkeratotic plaques on the dorsa of both hands and feet (Figs. 1a and 1b). No other skin lesions were found. The hair, nail, and oral mucosas were normal. We kept the possibility of necrolytic acral erythema, zinc-responsive dermatosis, and pellagra. We investigated the patient against the possible cause, including a complete hemogram, a urine routine test, liver and renal function tests, serology for hepatitis B, C, and HIV, and serum zinc levels. Routine investigations were normal except for mild anemia. The alkaline phosphatase levels were 32 IU/L, slightly lower than the normal range (40–120 IU/L). Serum zinc levels were 60 mg/dL, slightly less than the normal range (70–120 mg/dL). The viral serological markers were found to be negative. Other systemic gastrointestinal and neurological symptoms, the Casal necklace around the neck, were not seen as in the case of pellagra (Fig. 1c). The hepatitis C viral marker associated with necrolytic acral erythema was also negative. As the patient was unresponsive to topical steroids and other immunomodulators previously along with lower levels of zinc and alkaline phosphatase found on investigations, we made the final diagnosis of zinc-responsive dermatosis and decided to put the patient on oral zinc therapy at the dose of 200 mg three times a day for at least six weeks along with emollients. A follow-up at six weeks was done and a remarkable response to treatment was noted (Fig. 1d).
DISCUSSION
Zinc-responsive acral hyperkeratotic dermatosis is a rare entity characterized by well-defined, hyperpigmented plaques on the acral parts of the body [1]. The diagnosis requires a strong suspicion along with ruling out close differential diagnoses such as necrolytic acral erythema and pellagra. A rapid response to zinc therapy helps to establish the diagnosis of zinc-responsive dermatosis.
Necrolytic acral erythema (NAE) manifests itself similarly as well-circumscribed, violaceous plaques with or without scales, symmetrically distributed on the acral areas. However, it may be present on the Achilles tendons, malleoli, legs, and knees. Less frequent sites of involvement include the elbows, hands, buttocks, and genitalia [2]. It may be associated with metabolic alterations such as hypoalbuminemia, hypoaminoacidemia, increased glucagon levels, hyperglycemia, and deranged liver function [3]. NAE has been considered to be a cutaneous marker of hepatitis C infection [4,5]. However, cases of NAE have been reported all over the world in those who are seronegative to the hepatitis C virus (HCV) [6,7].
Cases of pellagra have significantly decreased after the late 90s and only certain high-risk groups are affected, in which the staple diet is corn or maize. It mainly occurs due to a deficiency of niacin and affects the skin and the gastrointestinal and nervous systems. The four classic Ds of the disease are dermatitis, dementia, diarrhea, and death [8]. The typical rash in pellagra involves the photo-exposed parts of the hands and feet and the Casal necklace around the neck [9,10]. Low serum niacin levels and a remarkable improvement after nicotinamide therapy may aid in the diagnosis.
Herein, we report a unique presentation of treatment-refractory hyperkeratotic acral plaques and their significant response to oral zinc therapy, urging dermatologists to adopt a wider approach to their diagnosis. Knowledge of the condition and close differentials taken into account will help in early diagnosis and treatment without an unnecessary investigation burden.
CONCLUSION
The diagnosis of zinc-responsive acral hyperkeratotic dermatosis should be considered in the case of chronic and treatment-refractory hyperpigmented plaques on the acral parts of the body.
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients gave their consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Ghosh A, Aggarwal I, De A, Samanta A, Chatterjee G, Bala S, et al. Zinc-responsive acral hyperkeratotic dermatosis-A novel entity or a subset of some well-known dermatosis?Indian J Dermatol. 2015;60:136-41.
2. Inamadar AC, Shivanna R, Ankad BS. Necrolytic acral erythema:Current insights. Clin Cosmet Investig Dermatol. 2020;13:275-81.
3. Ilyas S, Cheema SM, Rashid T. Necrolytic acral erythema:A rare entity. J Pak Assoc Dermatol. 2016;26395-8.
4. Das A, Kumar P, Gharami RC. Necrolytic acral erythema in the absence of hepatitis C virus infection. Indian J Dermatol. 2016;61:96-9.
5. Botelho LF, Enokihara MM, Enokihara MY. Necrolytic acral erythema:A rare skin disease associated with hepatitis C virus infection. An Bras Dermatol. 2016;91:649-51.
6. Srisuwanwattana P, Vachiramon V. Necrolytic acral erythema in seronegative hepatitis C. Case Rep Dermatol. 2017;9:69-73.
7. Pandit VS, Inamadar AC, Palit A. Seronegative necrolytic acral erythema:A report of two cases and literature review. Indian Dermatol Online J. 2016;7:304-7.
8. Brahmaiah U, Parveda AR, Hemalatha R, Laxmaiah A. Pellagra:A forgotten entity. Clin Dermatol Rev. 2019;3:126-9.
9. Gupta SK, Arora AK, Sood N, Kaur S. Pellgra revisited. Indian Dermatol Online J. 2014;5:525-6.
10. Harsha N S, Suraj B M, Kanakavidu SS, Kodali R. Pellagra:A forgotten ailment in current clinical practice. Med J DY Patil Vidyapeeth. 2019;12:78-80.
Notes
Source of Support: Nil,
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
|



Comments are closed.