Breast dermatoses: Dermatologists coming to the rescue of gynecologists
Hasna Kerrouch , Meryem Khalidi, Rachid Frikh, Naoufal Hjira, Mohammed Boui
, Meryem Khalidi, Rachid Frikh, Naoufal Hjira, Mohammed Boui
Dermatology Venerology Department, Military Hospital Instruction Mohammed V, University Mohammed V, Rabat, Morocco
Corresponding author: Hasna Kerrouch, MD
Submission: 02.11.2021; Acceptance: 15.02.2022
DOI: 10.7241/ourd.20223.11
Cite this article: Kerrouch H, Khalidi M, Frikh R, Hjira N, Boui M. Breast dermatoses: Dermatologists coming to the rescue of gynecologists. Our Dermatol Online. 2022;13(3):289-292.
Citation tools:
Copyright information
© Our Dermatology Online 2022. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
More than any other organ of the body, the breasts represent the symbol of femininity for a woman. As with any part of the skin, they may be the seat of inflammatory, infectious, and/or tumor-related dermatoses. The severity of these dermatoses is related to the existence of an underlying malignant neoplasia with a risk of mastectomy, creating a high psychological impact. Through five observations, we discuss different diagnoses to be evoked in front of a breast dermatosis apart from the tumor pathology.
Key words: Breast; Dermatoses; Etiology
INTRODUCTION
The breast is an extended area between the clavicle, the armpit, and the middle of the sternum as opposed to the pectoralis major muscle.
Although they are also present in men, the breasts are part of the female reproductive system as accessory organs. Women have more breast tissue and mammary glands, which produce breast milk.
The breasts may be the site of several dermatoses of mostly infectious, tumoral, and/or immunoallergic origin [1].
The severity of these dermatoses is related to the existence of an underlying malignant neoplasia with a risk of mastectomy, which puts at risk the vital and functional prognosis [2,3].
The objective of our article is to discuss, through five observations, the main diagnoses to be evoked in front of a breast dermatosis apart from the tumor pathology.
CASE REPORTS
Case 1
A 45-year-old female patient with no pathological history presented to our department with a six-month history of an ulceration of the right breast. A clinical examination revealed an erythematous ulceration with a raised, irregular border 1 cm in diameter (Fig. 1).
 |
Figure 1: An erythematous ulceration sitting at the lower internal quadrant of the right breast. |
The ulceration sat at the lower internal quadrant of the right breast and had a dry base. Pressure on the lesion caused a seropurulent discharge. There was no nipple discharge or palpable adenopathy. Paraclinical examinations—namely, mammography, breast ultrasound, and a chest X-ray—were unremarkable.
Pus culture on Löwenstein–Jensen medium showed colonies of Mycobacterium tuberculosis. A histological examination of a skin fragment revealed a tuberculoid granuloma without caseous necrosis. The diagnosis of tuberculous mastitis was retained. Antituberculosis treatment was initiated with good clinical evolution.
Case 2
A 38-year-old female patient with no pathological history presented with erosive, non-infiltrated, violet, and erythematous patches evolving for six months, covering the areolar region and the nipple, with no evidence of nipple discharge or oozing (Fig. 2).
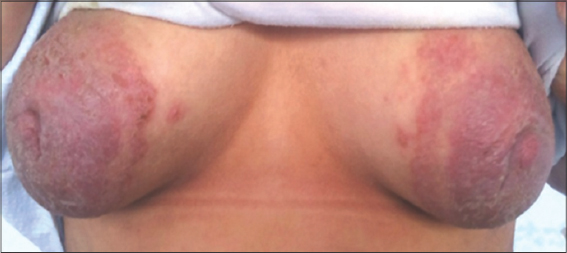 |
Figure 2: Erosive patches covering the areolar region and the nipple. |
Outpatient antibiotic and dermocorticoid treatment was without clinical improvement. Bacteriological and mycological samples were sterile. A histological examination revealed a non-specific inflammatory infiltrate without cyto-nuclear atypia. A careful interrogation revealed the notion of family conflicts. A hospitalization with psychological care and a local treatment were initiated with an evolution marked by a complete regression of the lesions. The diagnosis of pathomimia was then retained.
Case 3
An 82-year-old female patient without a notable pathological history was diagnosed with an erythematous placard of the left breast that occurred three days after a biopsy of the same site for the histological exploration of a nodule.
A clinical examination revealed a painful erythematous placard 6 cm in diameter with local mechanical bullae and exulcerations located in the lower external quadrant of the left breast with the presence of a sensitive unilateral adenopathy of around 1 cm in diameter (Fig. 3).
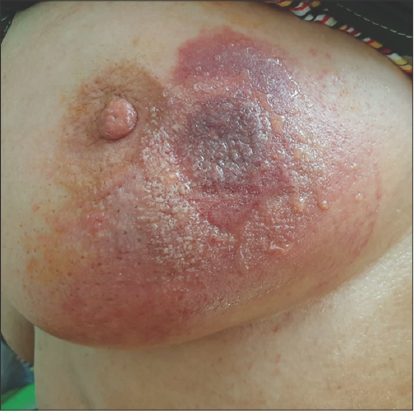 |
Figure 3: Erythematous placard and exulcerations located in the lower external quadrant of the left breast. |
On the biological level, an inflammatory syndrome was observed.
The diagnosis of infectious dermohypodermatitis with a common germ was retained and the patient was put under general antibiotic therapy and local care for fifteen days with good clinical and biological improvement.
Case 4
This patient was an eighteen-year-old female with no pathological history diagnosed with an erythematopruritic rash on both breasts that occurred 48 hours after the application of a cream containing sarsasapogenin (extracted from the roots of an Asian plant).
Upon clinical examination, an erythematous placard with crumbling edges surmounted by crusts in some places was noted on both breasts (Fig. 4).
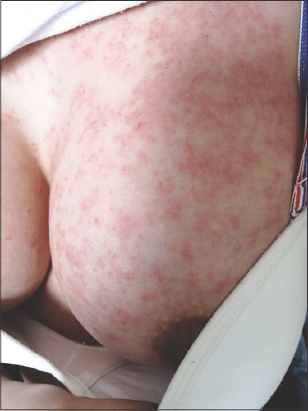 |
Figure 4: Erythematous placard with crumbling edges, surmounted by crusts in some places on both breasts. |
The clinical aspect, the time of appearance, and the localization evoked contact eczema.
The patient was put on class III dermocorticoids at a rate of one application per day for seven days, then one application every other day for seven days. The local skin signs regressed in a few days with a good clinical evolution.
Case 5
A 24-year-old female patient, who gave birth one year previously, presented with a non-regressive right breast engorgement. A clinical examination revealed ulcerative-bourgeous, infiltrated, erythematous, suppurative, and painless lesions of the right breast, which had been evolving for two months, with inflammatory arthralgias and erythema nodosum (Fig. 5).
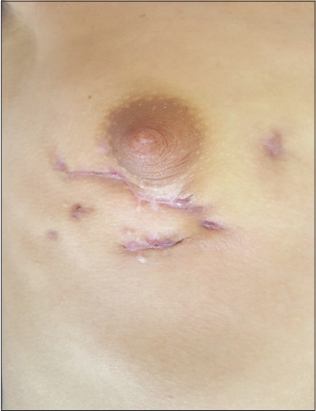 |
Figure 5: Ulcerative-bourgeous lesions of the right breast. |
On the biological level, a moderate inflammatory syndrome was observed.
Bacteriological and mycological examinations, as well as PCR tests for BK on pus and tissue samples, were negative.
A skin biopsy with a breast biopsy revealed epithelioid and giganto-cellular granuloma without caseous necrosis.
The diagnosis of idiopathic granulomatous mastitis was retained and the patient was put on oral corticosteroid therapy with a good clinical and biological evolution.
DISCUSSION
Breast dermatoses include all dermatological symptoms located in the mammary gland and/or its skin covering or secondary to a general disease.
The evaluation and management of these dermatoses rely on a good knowledge of the anatomy and the emotional, cultural, and sexual values of this region.
Mammary tuberculosis was first described by Sir Astley Cooper in 1829 in London as “scrofulous swelling of the mammary gland” or “cold tumor of the breast” in a young woman with a swollen breast [4].
Breast tuberculosis is a highly rare form of tuberculosis [5,6]. The rarity of this clinical form may be explained by the fact that breast tissue seems to be poorly suited to the survival and multiplication of the tubercle bacillus [7]. It mainly affects young women [8].
The diagnosis of breast tuberculosis is always difficult for it may mimic a large number of conditions, particularly malignant. This is also due to the lack of specificity in its clinical and radiological signs. Only histological evidence guarantees a definite diagnosis [6].
The treatment is mainly based on anti-tuberculosis drugs, yet surgical treatment is sometimes necessary.
Pathomimicry is defined as a self-induced disease in a clearly conscious state by the patient himself, at the level of the mucocutaneous membrane or the dander [9].
It is a relatively rare condition and one of the most complex problems for a dermatologist [10].
Medical intervention is complex, associating both psychological work and medical and surgical treatment.
Dermohypodermatitis with a breast infection is generally of staphylococcal origin. They are most often discovered at the stage of a breast abscess. The treatment is medical based on oral antibiotic therapy.
Contact dermatitis, also known as contact eczema, is a common inflammatory skin disease, occurring at the site of contact with non-protein chemical molecules.
In this area, the skin lesions are not different from other areas: They are erythematous and vesicular, sometimes discreetly scaly, and bullous in severe cases. They are associated with pruritus. The causative agent must be sought in order to avoid it, at best after performing patch tests.
Idiopathic granulomatous mastitis is a rare benign inflammatory mastopathy affecting women during their genital activity [11].
The definitive diagnosis is histological and its evolution remains capricious with a risk of recurrence. The treatment is medical, combining antibiotics and anti-inflammatory drugs. It is surgical in abscessed forms.
CONCLUSION
Dermatologic breast symptoms may be primary or secondary to an underlying disease. Directed paraclinical examinations are necessary to reach the diagnosis. They constitute a real challenge for both the dermatologist and the gynecologist.
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients gave their consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Levy-Bencheton A, Agostini A. Dermatoses de l’aréole et du mamelon. EMC Dermatology. 2013;98-871-A-10.
2. Lachapelle JM, Borradori L. Dermatoses des seins. Dermatologie et infections sexuellement transmissibles 6ème édition. 2017;958-61.
3. Ryerson AB, Miller J, Eheman CR. Reported breast symptoms in the National Breast and Cervical Cancer Early Detection Program. Cancer Cause Control. 2015;26:733-40.
4. Zouhal A, Outifa M, Filali A, El amrani N, Bensaid F, El fehri SH, et al. Les tumeurs pseudonéoplasiques du sein:Tuberculose Mammaire àpropos de 2 cas. Médecine du Maghreb. 2000;82:11–4.
5. Agoda-Koussema LK, Djibril AM, Adjenou KV, Gnakadja GN, Balaka A, Amegbor A, et al. Breast tuberculosis:A case report. J Afr Imag Méd. 2014;6:73-7.
6. Ben Hassouna J, Gamoudi A, Bouzaïene H, Dhiab T, Khomsi F, Chargui R, et al. [Mammary tuberculosis:A retrospective study of 65 cases]. Gynecol Obstet Fertil. 2005;33:870-6.
7. Marinopoulos S, Lourantou D, Gatzionis T, Dimitrakakis C, Papaspyrou I, Antsaklis A. Breast tuberculosis:Diagnosis, management and treatment. Int J Surg Case Rep. 2012;3:548-50.
8. Boukadoum N, Kaidi CH, Yassi F, Kheloufi F. Mastite tuberculeuse:un diagnostic àne pas méconnaître. Imag Femme. 2012;22:221-3.
9. Gieler U, Consolf SG, Tomas-Aragones L, Linder DM. Selfinflicted lesions in dermatology:Terminology and classification, a position paper from the European society for dermatology and psychiatry. Acta Derm Venereol. 2013;93:4-12.
10. Uçmak D, Harman M, Meltem Akkurt Z. Dermatitis artefacta:A retrospective analysis. Cutan Ocul Toxicol. 2014;33:22-7.
11. Carmalt HL, Ramsey-Stewart G. Granulomatous mastitis. Med J Aust. 1981;1:356-9.
Notes
Source of Support: Nil,
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0002-2127-3863 http://orcid.org/0000-0002-2127-3863 |



Comments are closed.