Hidradenitis suppurativa and bilateral interstitial keratitis: A case report
India Robinson , Gabriella Santa Lucia, Alex Ritter, John Plante, Manuel Valdebran
, Gabriella Santa Lucia, Alex Ritter, John Plante, Manuel Valdebran
Department of Dermatology and Dermatologic Surgery, Medical University of South Carolina, Charleston, SC, USA
Corresponding author: India Robinson, BA
How to cite this article: Robinson I, Santa Lucia G, Ritter A, Plante J, Valdebran M. Hidradenitis suppurativa and bilateral interstitial keratitis: A case report. Our Dermatol Online. 2022;13(2):172-174.
Submission: 27.07.2021; Acceptance: 23.11.2021
DOI: 10.7241/ourd.20222.13
Citation tools:
Copyright information
© Our Dermatology Online 2022. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
Hidradenitis Suppurativa (HS) is a chronic inflammatory disease that cause painful abscess and nodules in skin that contain apocrine glands. While HS has known associations with several inflammatory disorders, a rare association is interstitial keratitis. We present a case of bilateral interstitial keratitis attributed to a severe flare of HS disease resulting in systemic inflammation. Other case reports have established that bilateral interstitial keratitis can be attributed to HS, as well as other eye symptoms and diseases. Despite the rarity of keratitis in patients with HS, clinicians should be aware that this association does exist when their HS patient presents with severe or atypical eye symptoms.
Key words: Keratitis; Hidradenitis Suppurativa; Inflammatory Disease; Autoimmunity
INTRODUCTION
Hidradenitis Suppurativa (HS) is a chronic, inflammatory disease resulting in panful abscesses in skin bearing apocrine glands. This disease more often affects women beginning in their second or third decade of life [1, 2]. Interstitial Keratitis (IK) is characterized by nonulcerative and nonsuppurative inflammation of the corneal stroma [3]. While inflammatory disorders such as inflammatory bowel disease, spondyloarthropathy, and other autoimmune disease are commonly associated with HS, IK is described as an association that is uncommon in daily clinical practice [1,4]. Here we describe a patient with a history of Hidradenitis Suppurativa presenting with bilateral interstitial keratitis.
CASE REPORT
A 34-year-old female with a 15-year history of Hurley Stage 3 Hidradenitis suppurativa (HS) with draining sinuses on her left buttock and right axilla (Fig. 1) presented to the clinic with bilateral eye pain, decreased vision, and redness (Fig. 2). Her disease is severe with poor response to typical HS treatments. She began Adalimumab in November 2019 with relief but was discontinued. Nine months later, the patient presented to an acute care center with a white spot on her right eye with erythema, pain and pruritis that progressed over 10 days to include her left eye. She was prescribed prednisolone drops and showed improvement within a day.
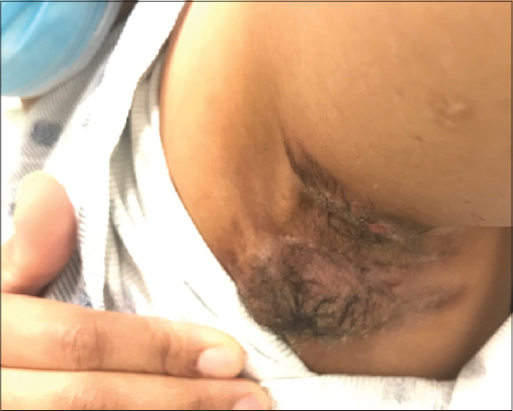 |
Figure 1: Axillary HS with nodules forming sinus tracts. |
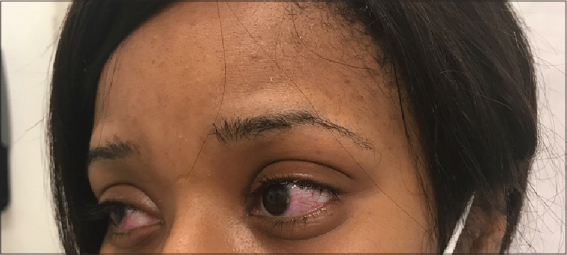 |
Figure 2: Bilateral eye erythema. |
Ophthalmology diagnosed her with bilateral peripheral interstitial keratitis and continued prednisolone eye drops with oral steroids and cyclosporine on reserve. They gathered ANA titers, ANCA, RF, CCP, CMP, CBC, CRP/ESR and syphilis titers. She had an ANA titer of 1:160 with a negative reflex, positive c-ANCA, and slightly elevated CRP/ESR. Suspicion for Granulomatosis Polyangiitis was low due to a negative MPO/PR3, low ANA titers without negative reflex, and lack of other autoimmune symptoms. Coogan’s Syndrome was considered but ruled out due to no hearing loss. Her keratitis and elevated inflammatory markers were ultimately attributed to severe HS disease resulting in systemic inflammation. They recommended restarting Adalimumab, but she did not due to insurance reasons. Currently, her HS disease is stable without recent flares and her keratitis has resolved.
DISCUSSION
Although bilateral interstitial keratitis is a rather rare complication of HS, it may be important to screen these patients for this complication along with other immune dysregulation phenomena such as acne conglobata, spondyloarthropathies, pyoderma gangrenosum, synovitis-acne-pustulosis-hyperostosis-osteitis syndrome, Dowling-Degos disease, fox den disease, florid steatocystoma multiplex, pyoderma vegetans, and pityriasis rubra pilaris.3 Prevalence and incidence data is limited for the association of HS and keratitis, but there are at least 10 cases in which the two entities were linked to one another [4].
One of these case reports is a similar presentation of another young Black female with severe HS that presented with bilateral interstitial keratitis that initially responded well to topical steroids, as our patient did [5]. One month following discontinuation of topical steroids, she had a flare of her HS disease that coincided with another flare of keratitis. Both conditions responded to Adalimumab and remained in remission for 7 months. Although we cannot associate a response of our patient’s keratitis to Adalimumab, we also saw that there was a temporal association with the activity of our patient’s HS disease and her keratitis. Her keratitis initially presented when her HS disease was flaring and remained stable when her HS symptoms were minimal.
Another study investigated the associated of HS with any type of inflammatory eye disease (IED). They found 20 patients with concomitant HS and IED, though the association between the two could not be determined as causal [3]. The majority were, similar to our patient, African American and female with 35% of patients without another autoimmune/inflammatory disease to explain the IED. Despite topical steroids being considered first line therapy, most patients with HS required systemic immunosuppression to alleviate symptoms [3].
CONCLUSION
Despite this being a rare phenomenon, it is valuable to be watchful of any HS patients with any eye discomfort, pain, change in vision, or change in appearance of the eyes, and consider urgent referral to ophthalmology. Alongside referral, prompt escalation of therapy to systemic immunosuppressive agents is necessary in over 70% of HS cases complicated by inflammatory eye disease and results in significant improvement [1,3]. Although our patient did not require any systemic therapy, coordination between ophthalmology, rheumatology, and dermatology resulted in the appropriate ruling out of any other autoimmune conditions, and attribution of her keratitis symptoms to her HS disease.
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients gave their consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Alikhan A, Lynch PJ, Eisen DB. Hidradenitis suppurativa:A comprehensive review. J Am Acad Dermatol. 2009;60:539-63.
2. Jemec GB. Clinical practice. Hidradenitis suppurativa. N Engl J Med. 2012;366:158-64.
3. Alzaga Fernandez AG, Demirci H, Darnley-Fisch DA, Steen DW. Interstitial keratitis secondary to severe hidradenitis suppurativa:a case report and literature review. Cornea. 2010;29:1189-91.
4. Sayg?n D, Syed AU, Lowder CY, Srivastava S, Maya JJ, Hajj-Ali RA. Characteristics of inflammatory eye disease associated with hidradenitis suppurativa. Eur J Rheumatol. 2018;5:165-8.
5. Knox CM, Holsclaw DS. Interstitial keratitis. Int Ophthalmol Clin. 1998;38:183-95.
Notes
Source of Support: Nil,
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0002-6043-4279 http://orcid.org/0000-0002-6043-4279 |



Comments are closed.