One train hiding another: Antiphospholipid syndrome as a risk factor for Nicolau syndrome?
Stijn Maes 1, Joris Schollaert1, Glenn Broeckx2, Olivier Aerts3, Niels Horst3
1, Joris Schollaert1, Glenn Broeckx2, Olivier Aerts3, Niels Horst3
1Faculty of Medicine, University of Antwerp, Belgium, 2Department of Pathology, Antwerp University Hospital (UZA), Belgium, 3Department of Dermatology, Antwerp University Hospital (UZA), Belgium
Corresponding author: Stijn Maes, MD
How to cite this article: Maes S, Schollaert J, Broeckx G, Aerts O, Horst N. One train hiding another: antiphospholipid syndrome as a risk factor for Nicolau syndrome? Our Dermatol Online. 2021;12(3):331-332.
Submission: 12.03.2021; Acceptance: 08.05.2021
DOI: 10.7241/ourd.20213.25
Citation tools:
Copyright information
© Our Dermatology Online 2021. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
Sir,
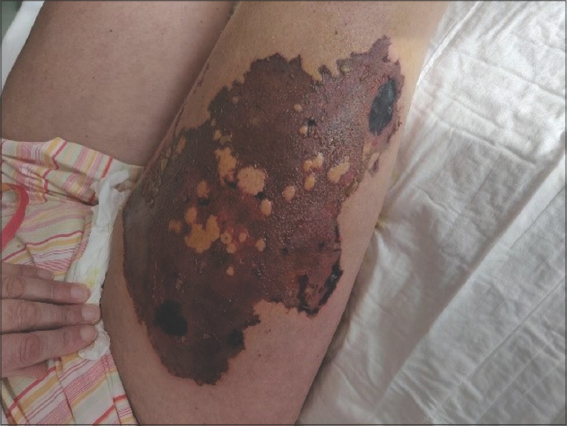
A 42-year-old female, known to have antiphospholipid syndrome (APS) and cutaneous lupus erythematosus, was hospitalized for type 2 non-ST segment elevation myocardial (NSTEMI) and bilateral adrenal infarction. She received 4.000 IE enoxaparin (low molecular weight heparin, LMWH) as secondary prophylaxis injected subcutaneously (sc.) at the anterior side of both upper legs. The day after, the LMWH dose was raised to 6.000 IE sc., after which the patient immediately developed an extremely painful and rapidly enlarging purpurous–necrotic skin lesion, albeit only in the upper right leg (Fig. 1). Duplex echography excluded deep vein thrombosis (DVT), and heparin-induced thrombocytopenia (HIT) was considered unlikely as no anti-PF4-heparin antibodies were present. Antigen tests equally excluded heparin-induced skin necrosis (HISN), a rare subtype of HIT with symptoms similar to Nicolau syndrome (NS). Moreover, the continued use of enoxaparin, without further worsening of the symptoms or the development of new lesions, equally argued against a diagnosis of HIT or HISN. A histopathological examination of a skin biopsy revealed acute, ulcerative, and pustular dermatitis with accompanying edema of the papillary dermis and steatonecrosis of the hypoderm. There was no clear vasculitis. Despite the absence of clearly visible emboli, easily missed in a small biopsy specimen, these characteristics were highly suggestive of NS (Figs. 2a – 2c). Despite the development of NS to enoxaparin sc., the latter was continued as the thromboembolic risks of APS were considered more important. Oral corticosteroids were administered to prevent further progression of the affected area, and antibiotics (piperacillin/tazobactam, later switched to meropenem) to treat the bacterial superinfection. Also, because both legs became diffusely edematous, with extension toward the abdomen, an additional treatment with furosemide had to be initiated. Surgical debridement of the necrotic tissue was performed until vascular tissue was seen. Following the debridement, two months of vacuum-assisted closure (VAC) therapy was initiated and, eventually, the created skin defect was restored with a skin graft.
NS is a rare, acute, and iatrogenic dermatologic complication, predominantly following an intramuscular (im.) injection of certain medications and, more rarely, as in the present case, occurring after a sc. injection. This condition typically begins with immediate and extreme pain in the injection site, followed by a localized livedoid-like or violaceous plaque. After the acute phase—usually after three days—the skin begins to necrotize, often necessitating surgical debridement [1,2]. The diagnosis of NS is made clinically, sometimes supported by histology, and therapy should initially focus on pain reduction and the prevention of infection. Importantly, the application of ice should be avoided as cold temperatures cause vasoconstriction and may thus further aggravate necrosis. Besides, systemic corticosteroids and revascularization therapies—that is, anticoagulants, pentoxifylline, etc.—are often employed as well [3]. Depending on the evolution and the degree of necrosis, surgical debridement may become necessary. Although the exact pathogenesis of NS remains poorly understood, thromboembolic vascular lesions in the skin are believed to play a major role. The present case suggests that, in the setting of APS (a hypercoagulable state), the development of NS might be facilitated, as such becoming likely even after sc. injections and even if the latter concerns a (therapeutic) anticoagulant. Nevertheless, in view of the severe consequences potentially associated with untreated and symptomatic APS, continued treatment with the same sc. agent may then still be possible.
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients gave their consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Kim K-K. Nicolau syndrome:A literature review. World J Dermatology [Internet]. 2015;4:103.
2. Marcus F, Claude EV, Josephine M, Teyang A. An exceptional cause of acute limb ischemia:Nicolau syndrome—Single-center experience with 4 cases. Ann Vasc Surg. 2019;58:383.e7-383.e11.
3. Senel E. Nicolau syndrome as an avoidable complication. J Fam Community Med [Internet]. 2012;19:52.
Notes
Source of Support: Nil,
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
|




Comments are closed.