Disseminated superficial actinic porokeratosis in a patient with generalized vitiligo: A case report
Department of Dermatology and Venereology, Al-Ramadi Teaching Hospital, Al-Anbar Health Directorate, Ministry of Health, Iraq
Corresponding author: Dr. Mancy Abdullah
Submission: 30.03.2020; Acceptance: 01.08.2020
DOI: 10.7241/ourd.20211.18
Cite this article: Abdullah M. Disseminated superfi cial actinic porokeratosis in a patient with generalized vitiligo: A case report. Our Dermatol Online. 2021;12(1):69-71.
Citation tools:
Copyright information
© Our Dermatology Online 2021. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
Disseminated superficial actinic porokeratosis (DSAP) is the most common type of porokeratosis, occurring mainly on sun-exposed skin. Chronic sun exposure is one of the main risk factors, in addition to genetic susceptibility. Most published data concerning the relationship between vitiligo and its predisposition to nonmelanoma skin cancer suggests that patients with vitiligo show the same or even a lower incidence than other populations. Herein, we report a case of disseminated superficial actinic porokeratosis occurring in vitiligo in which chronic sun exposure was the main risk factor.
Key words: Porokeratosis; Vitiligo; Sunlight; Ultraviolet radiation
INTRODUCTION
Porokeratosis is a keratinization skin disorder inherited as an autosomal dominant [1]. Disseminated superficial actinic porokeratosis (DSAP) is characterized by annular keratotic papules or plaques with a characteristic thread-like ridge and central atrophy that expand peripherally on sun-exposed skin [2]. A cornoid lamella is a distinctive histopathological feature of all its types [3]. Certain stimuli can hasten the appearance of porokeratosis, such as immunosuppression, radiation therapy, artificial ultraviolet radiation, and chronic sun exposure [4,5]. Herein, we present the case of a patient with generalized vitiligo in whom DSAP occurred mainly in a sun-exposed depigmented patch.
CASE REPORT
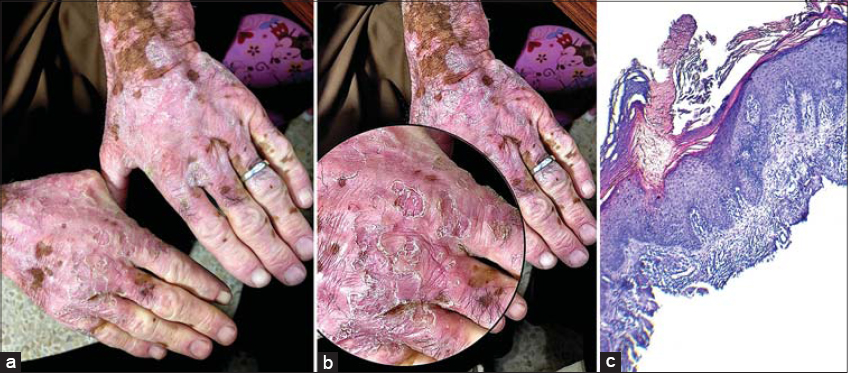
A 65-year-old male farmer presented to our dermatology clinic complaining of pruritic and hyperkeratotic skin on the back of the hands and fingers persistent for five years prior. He had had generalized vitiligo for the last twenty years with no special treatment and no history of treatment with phototherapy or immunosuppressive drugs. Upon examination, the patient looked healthy, apart from the vitiligo, which involved more than 70% of the body, including the face, extremities, and trunk. There were multiple annular plaques with sharply-defined thin edges and atrophic centers distributed bilaterally and symmetrically on the back of both hands, limited mostly to the depigmented skin (Figs. 1a and 1b). A punch biopsy was taken to show a cornoid lamella, the characteristic histopathological feature of porokeratosis (Fig. 1c). General laboratory investigations were within normal limits. The patient was advised to avoid sun exposure, apply sunscreen regularly in the daytime and topical retinoid at night, and attend regular follow-ups. Informed consent was taken from the patient and approval for the study was obtained from our institution.
DISCUSSION
Vitiligo is a common acquired pigmentary disorder that results from loss of melanin-producing cells. Melanin protects the skin from the harmful effects of the ultraviolet radiation (UVR) in sunlight [6]. UVR is the main factor in chronic sun exposure that induces nonmelanoma skin cancer (NMSC) by mutation of the TP53 gene [7]. Accordingly, vitiliginous skin is more vulnerable to these influences in comparison with normally pigmented skin. People with vitiligo show the same and even a lower incidence of cutaneous malignancies than other populations [1,8,9]. Some ascribe this to the increased expression of the tumor-suppressing gene TP53 in vitiligo [10,11]. Others point to the increase in certain cytokines and decrease in others acting as protective factors in vitiligo skin [10]. Photoadaptation, thickening of the stratum corneum, and the altered activity of the immune system are other explanations [11,12].
In contrast, there were several cases mentioned in the literature in which NMSC arose on depigmented skin, whether protected from the sun [2,11] or sun-exposed [13,14]. In our case, DSAP developed on sun-exposed vitiliginous skin, and this may be the first such case published in the literature so far. In our case, there were no specific risk factors apart from chronic sun exposure and a 30-year absence of photoprotection.
CONCLUSION
Although sun-exposed vitiliginous skin may have a lower chance to become affected by NMSC for different reasons, certain factors may increase this possibility, such as the age of the patient, the duration and extent of the vitiligo, the chronicity of sun exposure, the presence of immunosuppression, and a family history of other genetic diseases.
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients gave their consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Shin EJ, Gwak MJ, Jeong KH, Lee MH. Disseminated superficial actinic porokeratosis in a vitiligo patient undergoing treatment with long-term narrowband ultraviolet B. Ann Dermatol. 2018;30:249-51.
2. Bhaskar S, Jaiswal AK, Raj N, Reddy D. Porokeratosis – head to toe:an unusual presentation. Indian Dermatol Online J. 2015;6:101-4.
3. Souza PRM, Furtat TM, Reinisch N, Dario PHP. Scratching suspected porokeratosis lesion, simple and quick maneuver that facilitates its diagnosis. Our Dermatol Online. 2019;10:367-8.
4. Gupta M. Disseminated superficial actinic porokeratosis. Our Dermatol Online. 2017;8:241-2.
5. Sim CY, Shin JY, Lee SY, Park YL. Disseminated superficial actinic porokeratosis in a patient with psoriasis, after long-term narrowband ultraviolet B phototherapy. Ann Dermatol. 2018;30:211-3.
6. Brenner M, Hearing VJ. The protective role of melanin against UV damage in human skin. Photochem Photobiol. 2008;84:539-49.
7. Marcil I, Stern RS. Risk of developing a subsequent nonmelanoma skin cancer in patients with a history of nonmelanoma skin cancer:a critical review of the literature and meta-analysis. Arch Dermatol. 2000;136:1524-30.
8. Hexsel CL, Eide MJ, Johnson CC, Krajenta R, Jacobsen G, Hamzavi I, et al. Incidence of nonmelanoma skin cancer in a cohort of patients with vitiligo. J Am Acad Dermatol. 2009;60:929-33.
9. Paradisi A, Tabolli S, Didona B, Sobrino L, Russo N, Abeni D. Markedly reduced incidence of melanoma and nonmelanoma skin cancer in a nonconcurrent cohort of 10,040 patients with vitiligo. J Am Acad Dermatol. 2014;71:1110-6.
10. Vijay A, Jain SK, Kumar R. Squamous cell carcinoma on vitiligo patch:a rare association. Pigment Int. 2017;4:115-7.
11. Gangopadhyay A, Das JK, Agarwal AK. Squamous cell carcinoma in a patient with vitiligo of photo-covered skin. Indian J Dermatol. 2014;59:193-4.
12. Krüger C, Schallreuter KU. A review of the worldwide prevalence of vitiligo in children/adolescence and adults. Int J Dermatol. 2012;51:1206-12.
13. Dhawan AK, Verma P, Singal A, Sharma S. Squamous cell carcinoma complicating vitiligo in an Indian man. J Cutan Aesthet Surg. 2012;5:36-7.
14. Zhang XT, Ma XH, Jin WW, Chen SS, Xu HT. Concurrence of multiple cutaneous malignancies on sun-exposed vitiligo skin of a patient:a case report and review of the literature. Indian J Dermatol. 2018;63:346-8.
Notes
Source of Support: Nil.
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0002-3688-6953 http://orcid.org/0000-0002-3688-6953 |




Comments are closed.