Generalized bullous fixed drug eruption masquerading as toxic epidermal necrolysis
Farhana Tahseen Taj , Anisha Bindagi
, Anisha Bindagi
Department of Dermatology, Jawaharlal Nehru Medical College, KLE, Academy of Higher Education, Belgaum,590010, Karnataka, India
Corresponding author: Dr. Farhana Tahseen Taj
Submission: 09.03.2020; Acceptance: 09.05.2020
DOI: 10.7241/ourd.2020S3.7
Cite this article: Taj FT, Bindagi A. Generalized bullous fixed drug eruption masquerading as toxic epidermal necrolysis. Our Dermatol Online. 2020;11(Supp. 3):21-23.
Citation tools:
Copyright information
© Our Dermatology Online 2020. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
Fixed drug eruption is an adverse cutaneous drug reaction by which a patient grows a skin lesion each time a drug is taken. Generalized fixed drug eruption is a severe form of fixed drug eruption by which the skin lesions clinically resemble toxic epidermal necrolysis. A female patient presenting herself with generalized bullous fixed drug eruption following the intake of an ofloxacin and ornidazole combination treatment given for diarrhea. We report this case to emphasize the difference between generalized bullous fixed drug eruption and toxic epidermal necrolysis.
Key words: Generalised bullous fixed drug eruption; Toxic epidermal necrolysis; Cyclosporine
INTRODUCTION
Fixed drug eruption (FDE) is a cutaneous adverse drug reaction characterized by dusky red patches or bullae occurring at the same site each time the offending drug is taken. FDE accounts for 10% of adverse cutaneous drug reactions. Generalized bullous FDE is an uncommon variant of FDE characterized by widespread bullae and erosions, which may mimic Stevens–Johnson syndrome (SJS) or toxic epidermal necrolysis (TEN) [1]. TEN, like FDE, is associated with a better prognosis than TEN. We report a case of generalized bullous fixed drug eruption (GBFDE) mimicking toxic epidermal necrolysis.
CASE REPORT
A 46-year-old female presented herself to the OPD with generalized itching and multiple erythematous patches and bullae present for the last three days. The patient developed these skin lesions after starting treatment for diarrhea. The patient was prescribed ofloxacin and ornidazole, then developed multiple painful fluid-filled lesions on the thighs, arms, and abdomen in a span of 24 hours (Figs. 1 and 2). The lesions progressed in size and number and ruptured to leave violaceous hyperpigmented patches all over the body. The patient had a similar episode in the past with the same medication.
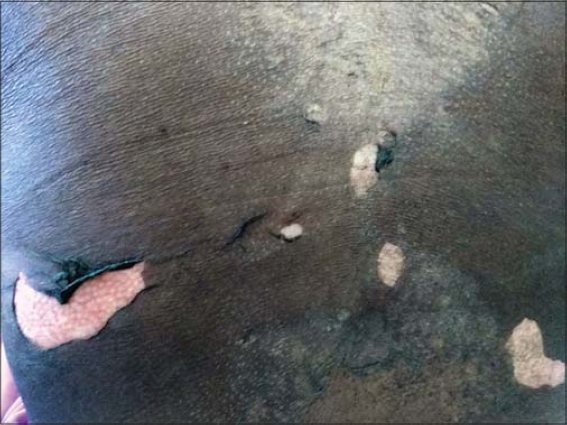 |
Figure 1: An eroded skin following the rupture of the bullae. |
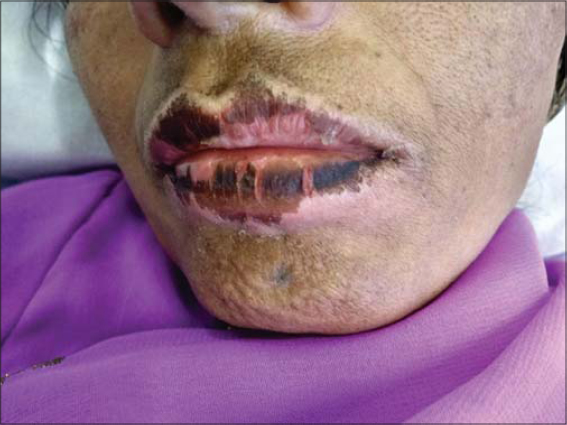 |
Figure 2: Crusting and pigmentation of the lips. |
On cutaneous examination, there were multiple erythematous patches with tense bullae distributed all over the body. Nikolsky’s sign was positive. There was no epidermal peeling or target lesions. A routine blood examination was within normal limits. Renal function tests, liver function tests, and a diabetic profile were within normal limits. An electrolyte panel showed no abnormality, and blood and urine cultures were negative. The patient was started on systemic corticosteroids and cyclosporine 3 mg/kg for five days. The intravenous antibiotic linezolid and a topical antibiotic cream were given. The patient showed an improvement of the skin lesions within 48 hours of initiating treatment. There were no new lesions, and the existing lesions were showing signs of healing. The patient was discharged after five days without complications.
DISCUSSION
An adverse drug reaction is a reaction that is noxious and unintended and that occurs at dosages normally used for prophylaxis, diagnosis, or treatment of a disease or for modification of a physiological function. It may range from common transient and benign erythema, occurring 6–9 days after the introduction of a new drug, to the most severe forms, which affect fewer than 1/10,000 patients.
Fixed drug eruption (FDE) characteristically recurs in the same site or sites each time the same drug is administered; with each exposure, however, the number of the sites involved may increase. Acute lesions usually develop 30 minutes to 8 hours after drug administration. Clinically, they appear as sharply marginated, round or oval itchy plaques of erythema and edema becoming dusky violaceous or brown, and sometimes vesicular or bullous. The eruption may initially be morbilliform or scarlatiniform or may resemble erythema multiforme. As healing occurs, crusting and scaling are followed by pigmentation, which may be especially persistent and occasionally extensive, especially in pigmented individuals. The lesions are distributed over the hands, feet, genitalia, and perianal areas.
The drugs most frequently associated with FDE are sulfonamides (in some series, up to 75% of cases), NSAIDs (in particular, phenazone derivatives), barbiturates, tetracyclines, and carbamazepine. Phenolphthalein-induced FDE is seen less commonly as it has been removed from a number of laxative preparations. A non-pigmenting variant of FDE, with large erythematous edematous plaques, has also been described, occurring primarily after the administration of pseudoephedrine [2].
GBFDE presents itself as severe bullous eruptions that may mimic TEN. GBFDE differs from SJS/ TEN clinically by a short latent period and a lesser mucosal involvement, and, histopathologically, by a more extensive eosinophilic infiltrate and more dermal melanophages. Immunohistopathology shows more dermal CD4+ cells and FOXP3 cells and fewer intraepidermal CD56+ cells and granulysin+ cells [3,4]. There is decreased serum granulysin in GBFDE. Granulysin is secreted by natural killer cell and cytotoxic T cells, which are responsible for the epidermal necrosis seen in SJS/TEN. Serum granulysin may be detected in SJS/TEN in the early phase of the disease even before skin detachment and mucosa erosions. FDE occurs due to antibody-dependent cellular cytotoxicity. Interleukin 20 is responsible for the site-specificity of the lesions [2].
The treatment of FDE includes antihistamines and topical corticosteroids. GBFDE requires treatment with immunosuppressive drugs. Cyclosporine has shown benefit in the treatment of GBFDE [5]. It inhibits interleukin 2, the Fas receptor, Fas ligand interactions, and CD8+ mediated cytotoxicity. Our patient had severe generalized bullous lesions, less mucosal involvement, without any systemic complications. The patient was started on cyclosporine, and the lesions started showing signs of healing within 48 hours, without any new lesions.
CONCLUSION
We report a case of GBFDE following the intake of an ofloxacin and ornidazole combination, treated successfully with cyclosporine. We emphasize the importance of differentiating GBFDE from TEN/SJD as managing severe TEN/SJS is more challenging than managing GBFDE. A systemic approach and careful observation are all that is required in the management of a severe drug rash.
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients gave their consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Daulatabadkar B, Pande S, Borkar M. Generalized bullous fixed drug reaction:A close similarity to stevens–johnson syndrome. Indian J Drugs Dermatol. 2017;3:28-31.
2. Podder I, Chandra S, Das A, Gharami RC. Doxycycline induced generalized bullous fixed drug eruption. Indian J Dermatol. 2016;61:128.
3. Tounkara TM, BaldéH, Soumah MM, Bangoura M, DianéBF, Keita M, et al. Severe cutaneous drug reactions in Guinean children:a monocentric retrospective study of 35 cases. Our Dermatol Online. 2018;9:118-22.
4. Cho YT, Lin JW, Chen YC, Chan CY, Hsiao CH, Chung WH, et al. Generalised bullous fixed drug eruption is distinct from Stevens-Johnson syndrome/toxic epidermal necrolysis by immunohistopathological features. J Am Acad Dermatol. 2014;70:539-48.
5. Beniwal R, Gupta LK, Khare AK, Mittal A, Mehta S, Balai M. Cyclosporine in generalised bullous fixed drug eruption. Indian J Dermatol. 2018;63:432–3.
Notes
Source of Support: Nil.
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
|



Comments are closed.