Erythroderma induced by dermatophytes
Takenobu Ohashi, Kinuko Irie, Toshiyuki Yamamoto
Department of Dermatology, Fukushima Medical University, Fukushima, Japan
Corresponding author: Prof. Toshiyuki Yamamoto
Submission: 04.03.2020; Acceptance: 01.06.2020
DOI: 10.7241/ourd.20203.24
Cite this article: Ohashi T, Irie K, Yamamoto T. Erythroderma induced by dermatophytes. Our Dermatol Online. 2020;11(3):319-320.
Citation tools:
Copyright information
© Our Dermatology Online 2020. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
Sir,
Erythroderma is a chronic condition presenting with generalized erythema occupying over 90% of the body surface. The causes of secondary erythroderma are various, such as eczema, contact dermatitis, psoriasis, pityriasis rubra pilaris, pemphigus foliaceus, cutaneous T-cell lymphoma, and drug eruption; however, erythroderma induced by tinea corporis is rare. We herein describe a rare case of erythroderma induced by dermatophytes.
A 66-year-old male visited out department, complaining of extensive erythema on the trunk. He was otherwise healthy and not on medication. He stated that itchy eruption appeared five years previously, and gradually spread in spite of being treated with topical ointment at a nearby clinic. He self-discontinued therapy and thereafter his skin rash gradually exacerbated. Physical examination showed diffuse, coalesced scaly erythemas on the trunk (Fig. 1). Potassium hydroxide (KOH) examination revealed a number of fungi (Fig. 2). Similar erythemas were observed on the genital areas, groins, buttocks, upper and lower extremities, and toe nails. Laboratory examination showed a white blood cell count of 8600/μl, with a differential count of 34% eosinophils. The IgE level exceeded 5,000 IU/ml, and thymus and activation-regulated chemokine (TARC) was also elevated (882 pg/ml; normal <450). Liver and renal function was normal, and human immunodeficiency virus antibody was negative. He was treated with oral terbinafine (100 mg/day), and skin lesions were improved seven weeks later with decreased eosinophil percentage (2%). Evaluation of pruritus with visual analogue scale score showed 89/100 before therapy, which decreased to 0/100 after successful therapy.
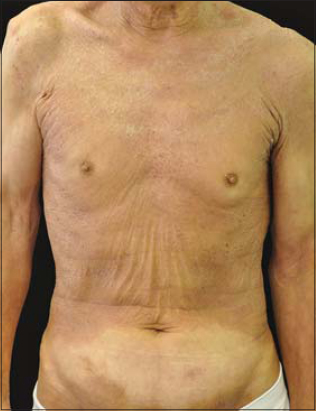 |
Figure 1: Diffuse erythema with scales on the trunk |
 |
Figure 2: KOH examination revealed a number of hyphae |
Secondary erythroderma is induced by various inflammatory skin diseases such as eczema and psoriasis. By contrast, cases of erythroderma due to dermatophyte are few [1]. In the present case, secondary fungal infection was excluded, because the patient recovered from generalized erythema only by anti-fungal therapy. KOH examination promptly made the correct diagnosis, and biopsy was avoided. Unfortunately, fungal culture was not carried out.
In a case series of erythroderma, cutaneous dermatophytosis was observed in 3 out of 103 cases (2.9%) [2]. In our department, over 70 patients were identified as having erythroderma in these 10 years, among whom only the present case was caused by fungal infection. Previous studies showed a significantly impaired permeability barrier function and reduced stratum corneum hydration in the lesional skin of tinea corporis [3]. In the present case, such profound changes in skin barrier structure and function i nduced by diffuse superficial dermatophytosis may have led to erythrodermic condition, via sweat dysfunction. We excluded the possibility that our patient had suffered from erythroderma for a long time, which secondarily developed superficial fungal infection, because his erythroderma was dramatically improved by oral terbinafine in a short period. In conclusion, it should be kept in mind that dermatophytosis is one of the causative factors of erythroderma.
Consent
The examination of the patient was conducted according to the Declaration of Helsinki principles.
The authors certify that they have obtained all appropriate patient consent forms. In the form the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
REFERENCES
1. Yousefian F, Crowley C, Skupsky H, Calame A, Cohen PR. Tinea corporis-associated erythroderma:case report and review of erythrodermic patients with chronic dermatophyte infection. Cureus. 2020;12:e7578.
2. Ndiaye M, Taleb M, Diatta BA, Diop A, Diallo M, Diadie S, et al. Etiology of intertrigo in adults:a prospective study of 103 cases. J Mycol Med. 2017;27:28-32.
3. Gauberg J, Wu N, Cramp RL, Kelly SP, Franklin CE. A lethal fungal pathogen directly alters tight junction proteins in the skin of a susceptible amphibian. J Exp Biol. 2019;222:pii:jeb 192245.
Notes
Source of Support: Nil,
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0002-8390-2573 http://orcid.org/0000-0002-8390-2573 |



Comments are closed.