Penile annular lichen planus
Anissa Zaouak , Leila Bouhajja, Houda Hammami, Samy Fenniche
, Leila Bouhajja, Houda Hammami, Samy Fenniche
Department of Dermatology, Habib Thameur Hospital, Tunis, Tunisia
Corresponding author: Dr. Anissa Zaouak, E-mail: anissa_zaouak@yahoo.fr
Submission: 14.06.2019; Acceptance: 20.08.2019
DOI: 10.7241/ourd.20202.35
Cite this article: Zaouak A, Bouhajja L, Hammami H, Fenniche S. Penile annular lichen planus. Our Dermatol Online. 2020;11(2):218-219.
Citation tools:
Copyright information
© Our Dermatology Online 2020. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
Sir,
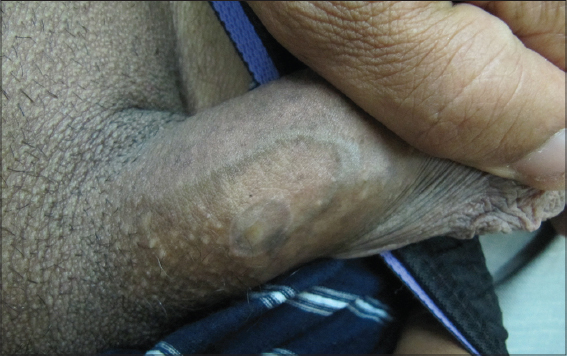
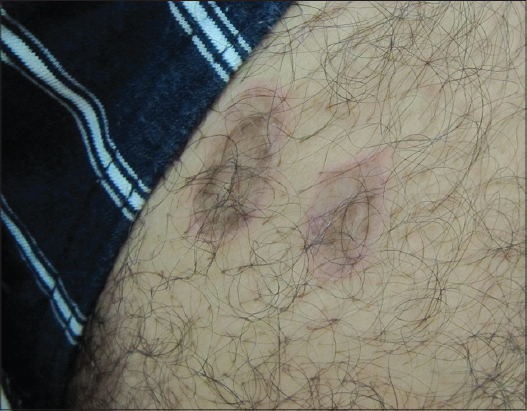
We report a 47-year-old circumcised man who presented to our department for annular lesions of the penis and the left thigh since one year. The lesions were slightly pruritic. The patient was a fairly healthy-looking man with no medical history. He had never had syphilis, was married and had 2 healthy children. Cutaneous examination revealed annular brown plaques with central hypopigmentation of the penile shaft (Fig. 1) in addition to purple annular scaly plaques on the left thigh (Fig. 2). The lesions were superficial but had a definite and firm consistence. They appeared first as small, flat papules which increased peripherally and involuted in the centre and so produced a ringed lesion. The lesions were slightly pruritic and no lesions occurred on the mucous membranes. Skin biopsy was performed on the edge of the plaque. Histopathological examination revealed a band-like infiltrate of T-cells at the epidermal-dermal junction. The epidermis was mildly acanthotic with compact hyperkeratosis and hypergranulosis. The basal layer showed vacuolar changes (Fig. 3).
Clinical and histopathological findings allowed us to assess the diagnosis of annular lichen planus. Serologies for hepatitis B and C were negative. A short course of mild topical corticosteroids was prescribed with an improvement of his skin condition. Lichen planus is a unique, non-infectious, pruritic, chronic inflammatory cutaneous and mucous membrane reaction pattern of immunological etiology which is relatively common. In 25% of the cases with lichen planus, male genitalia are involved especially the glans penis. Annular lichen planus is a well-defined variant of lichen planus and represents one of the approximately 20 distinct clinical variants of lichen planus and one of the rarest forms [1,2]. It is characterized by annular violaceous plaques which could be in rare cases atrophic [2,3]. It frequently presents on the penis and the scrotum. It has also a predilection for intertriginous sites such as the axilla, the groin folds or both [1]. Annular lichen planus is usually asymptomatic or slightly pruritic as in our patient. Two mechanisms were mainly proposed to explain how these annular shapes form. The first mechanism is that multiple lichenoid papules may converge in a circinate arrangement to form an annular shape. This configuration has been termed “papule-formed rings”. The second mechanism is that annular lesions may arise from central involution of a flat papule or plaque which at the same time expands peripherally with an advancing raised border. This configuration is also known as ring-formed papules and appears to be the most frequent mechanism [4].
Genital annular lichen planus may be confused with granuloma annulare, porokeratosis or syphilides [5]. Thus skin biopsy is necessary to confirm the diagnosis and usually shows typical features of lichen planus. No particular pathological pattern has been associated with genital annular lichen planus [1].
Short courses of mild topical corticosteroids are the first line treatments in this form of genital lichen planus with a satisfactory outcome in most patients. A brown post-inflammatory hyperpigmentation may persist after the disease has resolved [6].
In summary, annular lichen planus involves classically the male genitalia and should be considered among the differential diagnosis of annular genital lesions. It could also affect the proximal extremities such as the thigh and the buttocks.
Consent
The examination of the patient was conducted according to the Declaration of Helsinki principles.
REFERENCES
1. Reich HL, Nguyen JT, James WD. Annular lichen planus:a case series of 20 patients. J Am Acad Dermatol. 2004;50:595-9.
2. Friedman DB, Hashimoto K. Annular atrophic lichen planus. J Am Acad Dermatol. 1991;25:392-4.
3. Kim JS, Kang MS, Sagong C, Yu HJ. Annular atrophic lichen planus associated with hypertrophic lichen planus. Clin Exp Dermatol. 2008;33:195-7.
4. Sutton RL.The symptomatology and treatment of some variant forms of lichen planus. JAMA. 1914;62:175-83.
5. Barnette DJ Jr, Curtin TJ, Yeager JK, Corbett DW. Asymptomatic penile lesions. Cutis. 1993;51:116-8.
6. Moyal-Barraco M, Edwards L. Diagnosis and therapy of anogenital lichen planus. Dermatol Ther. 2004;17:38-46.
Notes
Source of Support: Nil.
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0003-2062-2256 http://orcid.org/0000-0003-2062-2256 |




Comments are closed.