|
Get Citation
|
|
|
Mejri S, Attafi Sahli S, Bouchouicha S. Multiple piloleiomyomas. Our Dermatol Online. 2017;8(4):509-510 |
|
|
Download citation file:
|
Multiple piloleiomyomas
Salwa Mejri1, Salsabil Attafi Sahli2, Sana Bouchouicha1
1Department of Dermatology, Regional Hospital of Menzel Bourguiba, Menzel Bourguiba, Tunisia; 2Department of Pathology, Regional Hospital of Menzel Bourguiba, Menzel Bourguiba, Tunisia
Corresponding author: Dr. Salsabil Attafi Sahli, E-mail: sehlisalsabil@hotmail.com
Submission: 25.01.2016; Acceptance: 17.04.2017
DOI: 10.7241/ourd.20174.148
Sir,
Cutaneous leiomyomas (CL), also referred to as leiomyomas cutis, are an uncommon benign tumor of smooth muscle origin [1,2]. They may be sporadic or inherited occuring as a part of Reed’s syndrom or the hereditary leiomyomatosis and renal cell cancer syndrom [2,3]. The skin is the second commonest location for leiomyomas representing aproximatly 75% of extra-uterine leiomyomas [4,5]. According to the smooth muscle of origin and the clinicopathological characteristics, CL are classified as pilar or piloleiomyoma (PL), angioleiomyomas and genital leiomyomas [1–6]. PL derive from the arrector pili muscle. Theys represent the most common type of CL [5,7].
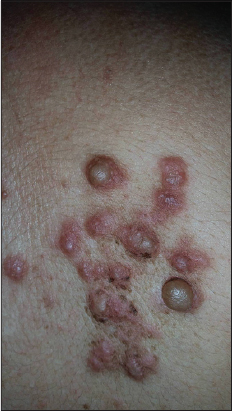
We report the case of multiple PL in a 61 year-old woman with no medical history. She presented with firm, pink-red and painful papulo-nodular lesions with a zosteriform disposition. The lesions were evolving for 10 years, measuring between 1mm and 5mm and sitting in the back and extremities (Fig. 1). The patient had a surgical excision of one nodule. The histological examination showed a non-encapsulated tumor arranged in interlacing bundles of smooth muscle fibers admixed with collagen in the upper dermis. There were neither vascular component nor myxoid or cystic changes. The tumor cells stained positively against smooth muscle actin. The S100 protein was negative. The diagnosis of multiple piloleiomyomas was retained. The patient was treated medically with nifedipine associated to cold prevention. The clinical course showed amelioration of the symptoms and especially a pain relief.
CL are rare representing almost 5% of all leiomyomas [4]. Literature concerning the pilar subtype of CL is scant and generally limited to case reports or non-standardized studies of limited number [1,5].
PL may be solitar or multiple. Theys appear preferentially in adulthood but they may occur in any age [4]. The sex distribution is not clear [2,4,5] but according to some studies [2], multiple PL occur preferentially in young male patients aged between 10 and 30 years. Contrary, solitary PL appear usually later than their multiple counterparts, especially in women [2]. Unlike, our patient is an elderly women. The lesions had appeared at the sixth decade and the diagnosis of multiple cutaneous piloleiomyomas was retained ten years later.
The distribution of multiple lesions is variable. They are often situated around Blaschko’s lines, linear, segmental, and zosteriform variants have been also described [5].
PL are typically firm, red-brown to flesh-colored papulonodules, measuring between 3 mm and 20 mm, located on the trunk or extremities [5].
The most important clinical symptom of CL is pain, present in almost 90% of cases. It can be provoked by cold, contact, pressure or emotion [5].
The presence of multiple CL can be associated whith hereditary leiomyomatosis and renal cell cancer (HLRCC) [3,5].
The differential diagnosis includes other painful skin tumors such as neurilemmoma, angiolipoma, glomus tumor, neuroma and granular cell tumor. Histologically, it may be confused with other CL (angioleiomyoma and genital leiomyoma), cutaneous neurofibromas which are not painful and stains positively with S100 protein [2,4,5].
Surgical excision is the treatment of choice for isolated PL or those in limited number [4–6]. For multiple lesions, several treatment modalities have been employed such as ablative, topical, or systemic treatments with no evidence on their efficacy [5–7].
REFERENCES
1. Fisher WC, Helwig EB. Leiomyomas of the skin. Arch Dermatol. 1963;88:510.
2. Morariu SH, Suciu M, Badea MA, Vartolomei MD, Buicu CF, Cotoi OS. Multiple asymptomatic cutaneous pilar leiomyoma versus spontaneous eruptive keloids – a case report. Rom J Morphol Embryol. 2016;57:283-7.
3. Lehtonen JH. Hereditary leiomyomatosis and renal cell cancer: Update on clinical and molecular characteristics. Fam Cancer. 2011;10:397–411.
4. Malhotra P, Walia H, Singh A, Ramesh V. Leiomyoma cutis: A clinicopathological series of 37 cases. Indian J Dermatol. 2010;55:337-41.
5. Malik K, Patel P, Chen J, Khachemoune A. Leiomyoma cutis: A focused review on presentation, management and association with malignancy. Am J Clin Dermatol. 2015;16:35-46.
6. Basendwh MA, Fatani M, Baltow B. Reed’s Syndrome: A Case of Multiple Cutaneous Leiomyomas Treated with Liquid Nitrogen Cryotherapy. Case Rep Dermatol. 2016;8:65-70.
7. Dilek N, Saral Y, Kotan ÖS, Bedir R. A case of late diagnosed multiple Pilar leiomyoma located on the cheek and neck. Pain Stud Treat. 2014;2:27.
Notes
Source of Support: Nil
Conflict of Interest: None declared.
Comments are closed.