The most common childhood skin diseases
1Student of Semmelweis University PhD School, Budapest, Hungary, 2Faculty of Health Sciences, Semmelweis University, Budapest, Hungary
ABSTRACT
The most common childhood skin disorders are usually diagnosed by district nurses, health visitors, panel pediatricians or school doctors. Dermatological or specifically pediatric dermatological examinations are seldom necessary. This article reviews the most common childhood skin disorders and the directives of their treatments.
Key words:Childhood skin disease; Bacterial skin disease; Fungal skin disease; Viral skin disease
HISTORICAL OVERVIEW
It was at the beginning of the 19th century that dermatology separated from internal medicine. The pioneers of dermatology used clinical and histological images to describe symptoms. Later, in the etiological era, the pathogens of certain diseases were demonstrated. This was followed by the exploration of the diseases of the skin and the internal organs.
As it is understood today, several external and internal factors are required for the development of skin disease. The human body should be considered not only as a unit, controlled and coordinated by the hormones of the cerebral cortex, but it is also in close connection with the environment. That is to say, the fact that whether a person is healthy or ill, results from the dynamic relationship between the external and the internal environment.
In the last decades, the discoveries of molecular biology have had a great influence on the development of medicine. Modern dermatology studies abnormal functions behind abnormal morphological lesions, but it also takes into consideration environmental influences as well as changes in the inner organs [1].
A common field for dermatology and paediatry is child dermatology. The knowledge of both professional fields is an essential criterion for successful therapy and prevention.
BACTERIAL SKIN DISEASES
Micro-organisms get onto the infant’s skin while traversing the birth canal. The characteristic bacterial flora develops in the first two weeks after birth, the majority being Gram-positive bacteria. Due to their need for a high degree of moisture, Gram-negative bacteria are mostly found in the folds [2].
Impetigo Contagiosa
Impetigo contagiosa is an extremely contagious, superficial skin infection. It appears mostly on young children. According to the statistical data of the Dermatology Department of Heim Pál Children’s Hospital Budapest, more than 70% of the cases are caused by aureus, in 20-25% of the cases we can talk about a blended infection (Staphylo- and Streptococcus), and only 5-10% of the cases have Streptococcus as the pathogen [1].
Clinical symptoms: Small, red maculae appear mainly on the face or on the limbs, with vesicles and blisters, which break almost immediately. The serous discharge, drying on the oozing blister base and on the surrounding skin, will generate characteristic honey-yellow slough [3]. Sloughing spreads quickly, not only on the edges, but also to further areas of the body, by autoinoculation, or it may be transmitted by tableware or clothing. The type with an epidemic-like occurrence on young babies is the bullous form, starting mainly from around the body orifices [4]. In the case of older children, the appearing symptoms are mostly accompanied by thick sloughing, in most cases on the lower limbs, where there is an injury or bites that have been scratched open.
Treatment: generally topical. Systemic antibiotics are required only in case the infection is extended or reoccurring. The topical treatment is applied in three phases:
- The removal of sloughs: By means of a neomagnol compress, or antiseptic cream (ung. Antisepticum Fo.No.)
- We should apply antiseptic paint which does not sting (sol. Merbromini 2%)
- Cream or ointment again (ung. Prednisolon J., ung. Antisepticum)
Nephritis may develop as a complication of impetigo caused by extended Streptococcus, therefore control (urine test) is recommended for 6 weeks.
Folliculitis
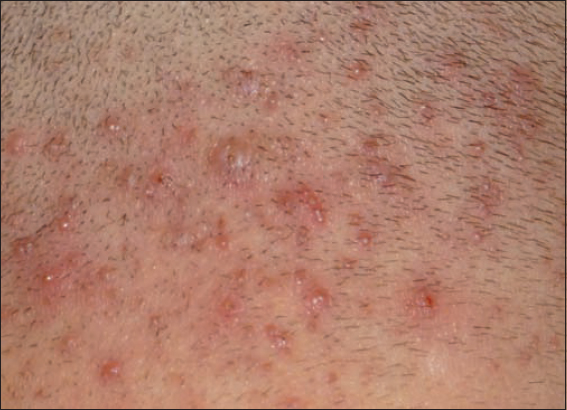
Folliculitis is a pustule, 1-2 millimetres in diameter, surrounded by a red halo of a few millimetres, and with a hair in the centre. In childhood, it appears mostly on the head, the gluteus, or on the limbs. Its larger and deeper type is the boil, developing mostly on adolescents (Fig. 1). It is generally caused by Staphylococcus [5].
Treatment: having removed the hair, apply antiseptic paint, and poultice in the case of a boil. Sometimes surgical intervention or systemic antibiotic treatment is needed.
Ecthyma
Ecthyma is a painful ulcer, 0.5-1 centimetre in diameter, and covered with deep, thick slough, which develops mainly on the legs and gluteus after a trauma or when insect bites have been scratched open. It is caused by Streptococcus heamolyticus [6].
Treatment: systemic antibiotics, topically the same as with the above mentioned [7].
Paronychia
Paronychia is an acute and painful inflammation of the nail-bed and the nail fold. Pressing the nail-bed will drain pus. It is caused by Streptococcus aureus; it develops in areas of thumb-sucking, injury, or ingrown nails on the feet [8].
Treatment: antiseptic soaking, topical or if needed, systemic antibiotics, or possibly surgical opening [9].
Erysipelas
Appearing mainly on the head of infants and babies, erysipelas is superficial dermatitis. The skin is shiny, red, warm to the touch and painful. The erythema has an irregular shape, but it has sharp edges and spreads like tongues of flame. Its pathogen is generally ß-Streptococcus, less frequently Staphylococcus. It gets into the skin through epithelial injuries, and spreads through the lymphatic vessels. It is accompanied by general symptoms, shivering, fever, and malaise.
Treatment: systemic Penicillin or Erythromycin [10]. Topically it is treated with cold packs (preceded by protection with ointment. eg. with Ung. Burow).
Erythrasma
The occurrence of erythrasma is less frequent with young children, and more common with adolescents. Slightly scaly russet colour maculae with sharp edges and a few centimetres in size develop in the axilla or in the folds of the groin. It does not cause subjective symptoms. Pathogen: Corynebacterium minutissimum [11].
Treatment: Erythromycin in full dose [10].
FUNGAL SKIN DISEASES
Fungi are less pathogenic than bacteria or viruses but due to antibiotic and steroid treatments they increasingly come to the fore. Childhood fungal infections are mostly caused by dermatophytons and proliferous fungi [12]. They can sicken the skin, the hair, the nails as well as the mycoderm.
Tinea Capitis
Tinea capitis is caused by threadlike fungi. The two most frequent types are trichophytia and microsporia, affecting mostly children between 2-5 years of age. One or more plaques with alopecia (bald patches) of a few centimetres are formed. The phenomena may be inflamed or inflammation-free. Raised from the surface of the skin and localized on the hair follicles, confluent and purulent nodes and sloughs are formed. Microsporia causes mildly scaling plaques. The hair shafts break at 2-3 millimetres [13]. The hair stubs are surrounded by a white, powdery capsule and the skin of the scalp looks as if it has been dusted with flour.
Pathogens: dermatophytons [13], which live in the earth, on animals, or on human skin. In recent times, the most frequently occurring infection has been microsporum canis, spreading from animals to children. The pathogen may be carried by symptom-free animals (dogs, cats, guinea pigs and hamsters) as well [14].
Treatment: systemic antimycoticum (Lamisil, Orungal) [15].
Tinea Corporis et Faciei
One or several round lesions, 1-2 centimetres in diameter, appear on the face, neck, chest or arms. The scaly lesions have sharp margins and are surrounded on the edges by vesicles or papules, occasionally forming unbroken lobate areas. They itch, which results in excoriations and sloughs on the skin. The lesions on the face are less characteristic, and are difficult to diagnose [16].
Tinea Inguinalis
Tinea inguinalis affects mainly boys, especially in hot weather. Increased sudation, wearing tight clothing, underwear rubbing the skin, are all predisposing factors. The characteristic fungal symptoms manifest in the folds of the groin.
Tinea Pedis
- Erosion interdigital: the skin between the toes is macerated, it cracks and itches
- Hyperkeratotic type: the skin of the sole thickens, scales, and it is slightly erythemic
- Pustular type: scaling, inflamed plaques, bordered by small pustules, develop on the sole
- Dyshidrotic type: small, deep-set vesicles develop in the instep, accompanied by oozing and scaling. If it is symmetrical, detected on both soles, it is a secondary symptom, a so-called id reaction. In this case, it is not a case of infection, but a lesion, attached to a primary centre and developing because of an allergy [1].
Tineas are generally treated with disinfectant paint and antifungal ointments (sol. Merbromini 2%, ung. Nizoral). In the case of tinea on the hairy scalp, systematic treatment is necessary [16].
Pityriasis Versicolor
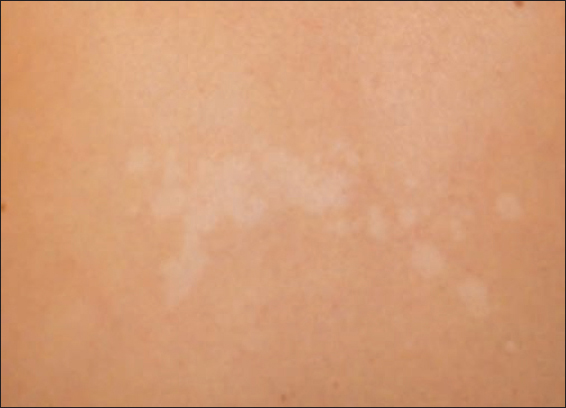
Young children are rarely affected, it appears quite often in puberty. The pathogen lives on the hairy scalp, and there it does not cause any symptoms. After getting on the skin of the trunk, it induces light brown maculae, 0.5-1 centimetre in size, mainly on the shoulders [17]. The maculae occasionally blend together, forming a map-like image, and turning white after sunbathing (Fig. 2).
Treatment: Nizoral shampoo [18], antifungal paint, and cream.
Candidiasis
Candidiasis is caused by candida albicans [19], a facultative parasite of the gastrointestinal tract. Infancy, old age, a tumour, leukaemia, and metabolic diseases are predisposing factors. Candidiasis of the oral mucosa of infants (soor oris) is a frequent phenomenon, since normal bacterial flora has not developed yet. White accretions develop on the oral mucosa, a few millimetres in size and occasionally confluent, which are indelible [1].
Treatment: sol. Canesten, Borax-glicerin solution Fo.No., Nystatin [19].
Angulus Infectiosus
Angulus infectiosus is caused by candida albicans [20]. Inflammation, scaling, or cracks emerge in one or both labial commissures [21].
Treatment: ung. Borosalicylatum Fo.No., Nizoral.
Diaper Dermatitis
Diaper dermatitis is a frequent, polietiological skin disease. It is manifested as tiny pustules and plaques with scaly edges, on the areas of infants’ skin, covered with the diaper. Erosions and oozing can be detected in the folds. Apart from the pathogen, candida albicans, getting onto the skin from faeces, a role is played by the occlusive effect of urine and the diapers [22, 23], or if textile diapers are used, the residues of the detergent and the fabric conditioner.
Treatment: see candidiasis. Prevention is of utmost importance, as well as the application of the right skin cleansing oils, emulsions, and adherent protective baby bottom ointment [23].
VIRAL SKIN DISEASES
Herpes Simplex
The primary infection mostly runs its course symptom free. The viruses remain in the spinal ganglia and get onto the skin from there [24].
Herpes Simplex recidivans
As a result of fever, trauma, stomach or bowel diseases, herpes simplex recidivans develops around the mouth of children, who are already infected by the virus. Following an itchy, stinging sensation, groups of vesicles [25] are formed on an erythemic basis, which will open and slough in a few days and heal without leaving a trace. There are no accompanying general symptoms, however, painful regional lymph-node swelling may develop even before the appearance of the skin symptoms.
Treatment: having opened the vesicles, apply antiseptic epithelizing paint, or possibly paste (zink-sulfate solution, zink paste) Hevizos cream [1].
Aphthosis
Aphtosis is one or several painful erosions on the oral mucosa, a few millimetres in size, encircled by a red ‘halo’, and covered with yellow fur. It heals without scars in 7-10 days [26]. It is probably caused by a virus, but an autoimmune origin might be a possibility as well.
Treatment: antiseptic and epithelizing paint.
Diseases Caused by the Verruca Virus
One of the most common skin lesions. A genetic predisposition and reduced cellular immunity result in susceptibility for infection. It is not a severe condition, however, in case of a multiplex occurrence, it is extremely uncomfortable. The incubation period may last as long as six months.
Verruca vulgaris (common wart)
A brownish-grey epitheliolid papula, a few millimetres-1 centimetre in diameter, and with a hyperkeratotic surface [27]. It appears most frequently on the hands, less frequently on the knees, while in the case of nail-biting children, under the nails or around the nail-bed. Filiform increments on the face and neck, flat, corn-like lesions on the soles, which may blend in a larger area like a mosaic (Fig. 3). There is a high rate of reoccurrence, and occasionally there is spontaneous healing. It is extremely infectious.
Treatment: the wart may be removed through peeling by layers with keratolytic paint (Verrumal), or through electrocoagulation under local anaesthesia, or possibly cryotherapy [27,28].
Verruca plana juvenilis (flat warts, plantar warts)
Flat, cuticolour, generally multiplex epitheliolid papules on the face or on the back of the hand [29], 1-2 millimetres in diameter. Their localization is linear, appearing along a wound or scratching.
Treatment: keratolytic paint with a milder effect (Egaverr).
Condyloma accuminatum
Small increments, developing on the genitalia or around the anus [30], effected by moisture and rubbing. It occurs on verruca-infected children and infants.
Treatment: paint with 10% Podophyllin [31].
Molluscum contagiosum (‘swimming-pool’ warts)
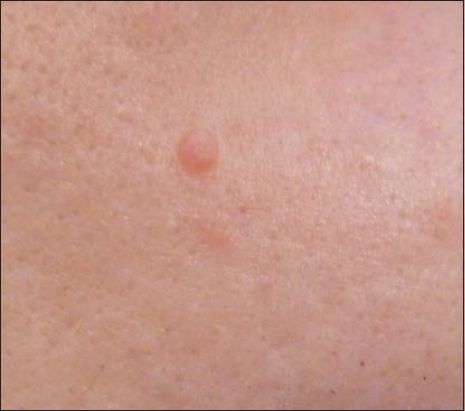
The incubation period may last several months. The semispherical warts are generally small, 1-3 millimetres in diameter [32] and have a flat surface, with a navel-like retraction in the middle and a narrow opening (Fig. 4). When pressed, gritty matter passes. It is extremely infectious. Pearl-like small nodules appear along scratching lines. Warts sometimes heal spontaneously.
Treatment: the warts can be removed with a Volkmann spoon or tweezers, or they may be exfoliated with iodized paint.
CONCLUSION
The majority of childhood skin disorders are of infectious origin. They are caused mainly by bacteria, fungus and viruses. The authors of this article summarized the characteristics of these diseases trusting that reviewing them will lead to early diagnosis, which coupled by adequate treatments speeds up the remission of the affected children.
REFERENCES
1. Zitás É, Prevention possibilities of the childhood diseases. Unpublished degree thesis 2004; Budapest: Semmelweis University;
2. Mempel M, Schnopp C, Selected bacterial infections of the skin in childhoodHautarzt 2015; 66: 252-7.
3. Iovino SM, Krantz KD, Blanco DM, Fernández JA, Ocampo N, Najafi A, NVC-422 topical gel for the treatment of impetigoInt J Clin Exp Pathol 2011; 4: 587-95.
4. Someshwar S, Jerajani HR, Bullous impetigoIndian Pediatr 2014; 51: 243.
5. Laureano AC, Schwartz RA, Cohen PJ, Facial bacterial infections: folliculitisClin Dermatol 2014; 32: 711-4.
6. Sonthalia S, Singal A, Khurana R, EcthymaIndian Pediatr 2014; 51: 510-1.
7. Kárpáti S, Bőrgyógyászat és venerológia 2013; Budapest: Medicina; 89.
8. Duhard É, ParonychiaPresse Med 2014; 43: 1216-22.
9. Langer MF, Lötters E, Wieskötter B, Surke C, Treatment of paronychiaOper Orthop Traumatol 2011; 23: 204-12.
10. Empinotti JC, Uyeda H, Ruaro RT, Galhardo AP, Bonatto DC, PyodermitisAn Bras Dermatol 2012; 87: 277-84.
11. Penton PK, Tyagi E, Humrighouse BW, McQuiston JR, Complete Genome Sequence of Corynebacterium minutissimum, an Opportunistic Pathogen and the Causative Agent of ErythrasmaGenome Announc 2015; 3: e00139-15.
12. Jain A, Jain S, Rawat S, Emerging fungal infections among children. A review on its clinical manifestations, diagnosis, and preventionJ Pharm Bioallied Sci 2010; 2: 314-20.
13. El-Taweel AE, El-Esawy F, Abdel-Salam O, Different Trichoscopic Features of Tinea Capitis and Alopecia Areata in Pediatric PatientsDermatol Res Pract 2014; 848763.
14. Atzori L, Aste N, Aste N, Pau M, Tinea faciei due to microsporum canis in children: a survey of 46 cases in the District of Cagliari (Italy)Pediatr Dermatol 2012; 29: 409-13.
15. Fellner MJ, Trichotillomania in a young male complicated by tinea capitis associated with Cryptococcus laurentii and Candida parapsilosisClin Cosmet Investig Dermatol 2013; 71-3.
16. Ely JW, Rosenfeld S, Seabury Stone M, Diagnosis and management of tinea infectionsAm Fam Physician 2014; 90: 702-10.
17. Archana BR, Beena PM, Kumar S, Study of the Distribution of Malassezia Species in Patients with Pityriasis Versicolor in Kolar Region, KarnatakaIndian J Dermatol 2015; 60: 321.
18. Framil VM, Melhem MS, Szeszs MW, Zaitz C, New aspects in the clinical course of pityriasis versicolorAn Bras Dermatol 2011; 86: 1135-40.
19. Leibovitz E, Strategies for the prevention of neonatal candidiasisPediatr Neonatol 2012; 53: 83-9.
20. Stoopler ET, Nadeau C, Sollecito TP, How do I manage a patient with angular cheilitis?J Can Dent Assoc 2013; 79: d68.
21. Park KK, Brodell RT, Helms SE, Angular cheilitis, part 1: local etiologiesCutis 2011; 87: 289-95.
22. Balasubramanian P, Jagadeesan S, Thomas J, Panicker VV, Anjanayen G, Diaper dermatitis with psoriasiform id eruptionsIndian J Dermatol Venereol Leprol 2015; 81: 435.
23. Merrill L, Prevention: Treatment and Parent Education for Diaper DermatitisNurs Womens Health 2015; 9: 324-36.
24. Ball MJ, Lukiw WJ, Kammerman EM, Hill MJ, Intracerebral propagation of Alzheimer’s disease: strengthening evidence of a herpes simplex virus etiologyAlzheimers Dement 2013; 9: 169-75.
25. Stoopler ET, Kuperstein AS, Sollecito TP, How do I manage a patient with recurrent herpes simplex?J Can Dent Assoc 2012; 78: c154.
26. Liang MW, Neoh CY, Oral aphthosis: management gaps and recent advancesAnn Acad Med Singapore 2012; 41: 463-70.
27. Leung L, Treating common warts – options and evidenceAust Fam Physician 2010; 39: 933-7.
28. Sultana R, Alam M, Khondker L, Ahamed RS, Safety in use of cryotherapy and topical salicylic acid with lactic acid combination in treating verruca vulgarisMymensingh Med J 2012; 21: 715-22.
29. Pavithra S, Mallya H, Pai GS, Extensive presentation of verruca plana in a healthy individualIndian J Dermatol 2011; 56: 324-5.
30. Varma S, Lathrop E, Haddad LB, Pediatric condyloma acuminataJ Pediatr Adolesc Gynecol 2013; 26: e121-2.
31. Simmons PD, Podophyllin 10% and 25% in the treatment of ano-genital warts. A comparative double-blind studyBr J Vener Dis 1981; 57: 208-9.
32. Nguyen HP, Tyring SK, An update on the clinical management of cutaneous molluscum contagiosumSkin Therapy Lett 2014; 19: 5-8.
Notes
Source of Support: Nil,
Conflict of Interest: None declared.

Comments are closed.