Would you consider pilomatricoma as a differential diagnosis?
Yuka Inamura, Hiroo Hata, Keisuke Imafuku, Shinya Kitamura, Hiroshi Shimizu
Department of Dermatology, Hokkaido University Graduate School of Medicine, Sapporo, Japan
Sir,
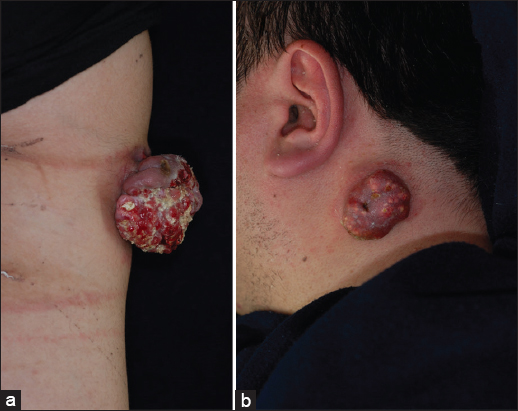
A 26-year-old man presented with a pedunculated, ulcerated, reddish and partially yellowish tumor of 6.5 cm in length by 6.0 cm in width by 3.0 cm in height on his left upper arm (Fig. 1a). The tumor had gradually developed during the half-year before the patient came to us on referral. There was no past history. We performed surgical removal of the entire tumor with a 1.0-cm margin, and the lesion was found to be a histopathologically poorly demarcated tumor without a capsule. There were darkly stained basophilic cells and so-called shadow cells with missing nuclei. There was no obvious nuclear atypia, and calcium deposits were found in the lesions. Based on these findings, we made the final diagnosis of pilomatricoma.
In a second case, a 42-year-old man presented with a pedunculated, non-ulcerated, reddish tumor of 5.0 cm in length by 2.5 cm in width by 0.8 cm in height on the left neck (Fig. 1b). We were able to see small yellowish dots on the surface. The tumor had gradually developed during the 3 months before the patient came to us on referral. The entire tumor was excisionally removed, and the surgical specimen showed the typical features of pilomatricoma.
Pilomatricoma is a common tumor derived from hair matrix cells; it is most often diagnosed in young children but may also affect adults. The clinical presentation is characterized by a subcutaneous nodule, usually up to 1 cm in diameter, with or without high mobility and calcification within the lesion that makes it feel hard and bony. For these reason it is easily diagnosed [1]. However, once the tumor is larger than 5 cm as the Case 1 and 2, they are called ‘giant pilomatricoma’, and it may become very difficult to make an accurate clinical diagnosis [2,3]. To date, several cases of giant pilomatricoma have been reported [4,5].
In Case 1, we initially suspected sebaceous carcinoma, squamous cell carcinoma or dermatofibrosarcoma protuberans, because of the unusual clinical manifestations. However, we considered pilomatricoma as an initial diagnosis when we encountered the Case 2, so we were able to avoid over-treatment on Case 2.
In conclusion, we should keep giant pilomatricoma in mind as a differential diagnosis when we see pedunculated, firm reddish tumor of >5.0 cm in size, with or without ulceration. This knowledge can avoid misdiagnosis and unnecessary examination and treatment.
Consent
The examination of the patient was conducted according to the Declaration of Helsinki principles.
REFERENCES
1. Julian CG, Bower PW, A clinical review of 209 pilomatricomasJ Am Acad Dermatol 1998; 39: 191-5.
2. Krausen AS, Ansel DG, Mays BR, JrPilomatrixoma masquerading as a parotid massLaryngoscope 1974; 84: 528-35.
3. Yamauchi M, Yotsuyanagi T, Saito T, Ikeda K, Urushidate S, Higuma Y, Three cases of giant pilomatrixoma-considerations for diagnosis and treatment of giant skin tumours with abundant inner calcification present on the upper bodyJ Plast Reconstr Aesthet Surg 2010; 63: e519-24.
4. Loader DE, Ortlechner K, Breier F, Wasilewicz-Stefani G, Steiner A, Feldmann R, Giant pilomatrixoma of the right armEur J Dermatol 2014; 24: 257.
5. Resende CI, Gomes J, Duarte Mda L, Brito C, Giant pilomatricoma in a patient with tuberous sclerosis, both diagnosed in the adult lifeBMJ Case Rep 2013; published online 29 August 2013
Notes
Source of Support: Nil,
Conflict of Interest: None declared.
Comments are closed.