Our Dermatol Online. 2011; 5(1): 62-64
DOI:. 10.7241/ourd.20141.16
Date of submission: 02.10.2013 / acceptance: 02.11.2013
Conflicts of interest: None
SUBUNGUAL GLOMUS TUMOR: AN UNCOMMON CAUSE OF MEDIAN CANALIFORM NAIL-DYSTROPHY OF HELLER
Mrinal Gupta, Vikas Sharma, Vikram K. Mahajan, Ravinder Singh
Department of Dermatology, Venereology and Leprosy, Dr. R. P. Govt. Medical College, Kangra (Tanda)-176001 (Himachal Pradesh), India
Corresponding author: Prof. Vikram K. Mahajan e-mail: vkm1@rediffmail.com
How to cite an article: Gupta M, Sharma V, Mahajan VK, Singh R. Subungual glomus tumor: an uncommon cause of median canaliform nail-dystrophy of Heller. Our Dermatol Online. 2014; 5(1): 62-64.
Abstract
Glomus tumor is an uncommon vascular tumor involving mostly subunguum of the thumb or the index finger. It commonly presents as a pink or purplish circumscribed nodule underneath the nail plate. Pain is paroxysmal in nature and precipitated often from exposure to cold or pressure/blunt trauma. Dystrophy of the nail plate occurs rarely. The described case, a 40-year-old woman, had dystrophic thumbnail ascribed to subungual glomus tumor that resembled median canaliform nail-dystrophy of Heller. .
Key words: Glomus tumor; Heller’s nail dystrophy; Median canaliform dystrophy; Nail dystrophy; Subungual tumor
Introduction
Glomus tumor (syn – glomangioma, glomangiomyoma) is an uncommon neuromyoarterial tumor of glomus bodies that affects both the genders usually in third or fourth decade and seen rarely in children. It notably involves the subunguum of thumb or the index finger, and occasionally the skin lesions over extremities, head, neck and penis have been described. Extracutaneous involvement of gastrointestinal tract, bones, lungs, liver and cervix may occur sometimes [1]. Pain is paroxysmal in nature and precipitated often from exposure to cold or pressure/blunt trauma. Dystrophy of overlying nail or erosion of underlying phalanx may occur rarely [2]. Median canaliform nail dystrophy of Heller, an uncommon form of nail dystrophy of one or both the thumbnails, is characterized by a midline or paramedian split or canal formation in the midline of nail plate in a characteristic inverted fir tree-like pattern. Most cases remain idiopathic and resolve spontaneously. An intentional trauma from pushing back the cuticle and proximal nail fold as a habitual tic is implicated in most instances. Familial cases of median canaliform nail dystrophy are on record and systemic retinoid therapy too has been a suggested causative factor [3]. However, its pathogenesis mostly remains obscure. The described case, a 40-year-old woman, had dystrophic thumbnail resembling median canaliform nail-dystrophy due to subungual glomus tumor.
Case Report
A 40-year-old woman presented with pain over proximal nail fold of right thumb for 3years. The pain often radiated to forearm and was severe even on mild touch and after exposure to cold. There was no history of prior trauma or drug intake. The nail plate showed a median split that had appeared over proximal nail plate and progressed longitudinally involving the whole nail plate within a year. A localized bluish discoloration over subunguum underneath the nail split was apparent that showed no inflammation (Fig. 1A, B). Direct pressure from pencil tip elicited severe pain (Love test) and tying tourniquet proximally to the arm provided no relief (negative Hildreth’s sign). Other finger and toenails, and systemic examination were normal. She was investigated further with a clinical possibility of onychmatricoma and median canaliform dystrophy of Heller. Routine laboratory investigations including hand x-rays were normal. A magnetic resonance imaging (MRI) of right thumb showed a 4mm hyper-intense mass in proximal nail bed suggestive of glomus tumour. A round bluish pink tumor (Fig. 1 inset) was excised after surgical nail avulsion under ring block and it showed histopathologic features of glomus tumor (Fig. 1C, D).
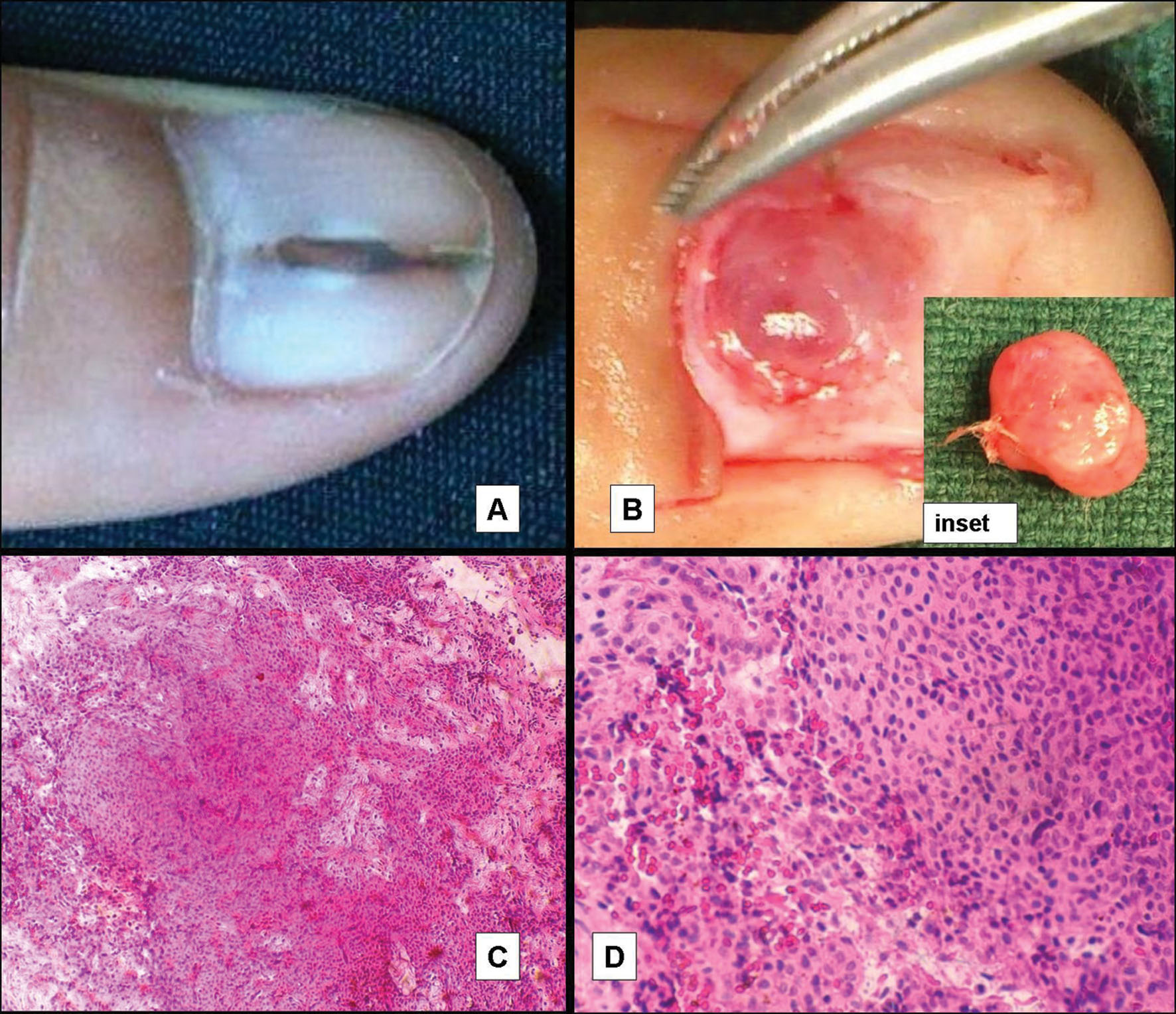 Figure 1. A. Longitudinal splitting of nail plate resembling median canaliform dystrophy. B. Bluish pink glomus tumor of nail bed as seen after surgical nail avulsion Inset shows excised glomus tumor. C. Histopathology of the excised tumor shows numerous dilated vascular spaces, surrounded by clusters of glomus cells (H&E, x 10). D. Single layer of endothelial cells lining the vascular lumina and surrounding tumor cells with scant cytoplasm and pale nucleus (H&E, x 40).
|
Discussion
Median canaliform dystrophy of Heller is a rare entity of obscure etiology; habitual tic is the most implicated factor in a sizeable majority. Subungual tumors (myxoid cyst, papilloma) have caused a median longitudinal split in a few cases by pushing up the nail plate from beneath or by pressure effects on the underlying nail matrix [4]. Some of the cases have been ascribed to glomus tumors involving the nail matrix or the nail bed [5,6]. Glomus tumor, a rare tumor of the glomus bodies, comprises only about 1-5% of all soft tissue tumors of hands [2]. Glomus bodies are present in reticular dermis at all body sites; most notably the subunguum has them in very high numbers. Nearly 90% patients present with solitary lesion and 25-75% cases have involvement of fingers (subunguum). An autosomal dominant inheritance may occur but most cases occur sporadically. A mutation of a specific gene, glomulin, has been mapped to chromosome 1p21-22 in cases of inherited glomangiomas [7]. Although the tumor may produce visible changes like erythronychia, distal onycholysis, nail dystrophy, discoloration of nail plate and even features of Raynaud’s phenomenon, the clinical diagnosis is often delayed for several (0-20) years as no clinically obvious lesion is seen in 1/3rd cases [8,9,2]. Glomus tumor requires differentiation from other painful cutaneous tumors (eccrine spiradnoma, leiomyoma, traumatic neuroma, neuromatoid hyperplasia), schwannoma, mucoid cyst, hemangioma, melanoma, or blue rubber bleb nevus when lesions are multiple. The glomus tumor can be visualized on radio-imaging studies like ultrasonography or MRI while x-ray examination may help in 25-60% cases who develop erosion of the underlying phalanx [10]. Thus, the clinical triad of severe pain, localized tenderness and temperature sensitivity is pathognomic. Surgically excised glomus tumor appears as a 1-20 mm bluish-red nodule. The histopathology of the tumor is characteristic with the presence of vascular lumina surrounded by proliferating glomus cells (identified from scanty eosinophilic cytoplasm and pale nucleus) arising from the arterial end of glomus body. Three distinct histological patterns can be identified:
1) ”solid glomus tumor” has sheets of cells resembling glomus cells,
2) ”glomangiomas” show dilated vascular channels surrounded by glomus cells, and
3) ”glomangiomyomas” have spindle shaped smooth muscle cells mixed with glomus cells.
Laser ablation, sclerotherapy, and surgical excision are available treatment options but recurrence in nearly 50% cases may occur following incomplete excision [5]. This patient had glomus tumor of the nail bed causing unusual form of nail dystrophy due to pressure effect on the growing nail by pushing it up. Surgical excision provided complete relief, and it has not recurred during 1-year follow up.
REFERENCES
1. Nigam JS, Misra V, Singh A, Karuna V, Chauhan S. A glomus tumour arising from the flexor aspect of the forearm: a case report with review of the literature. J Clin Diag Res. 2012;6:1559-61.
2. Moojen TM, Houpt P. Glomus tumors of the hand in the Netherlands: analysis of 107 patients. Eur J Plast Surg. 2000;23:224-6.
3. Sweeney SA, Cohen PR, Schulze KE, Nelson BR. Familial median canaliform nail dystrophy. Cutis. 2005;75:161-5.
4. Madke B, Gadkari R, Nayak C. Median canaliform dystrophy of Heller. Indian Dermatol Online J. 2012;3:224-5.
5. Lin Y-C, Hsiao P-F, Wu Y-H, Sun F-J, Scher RK. Recurrent digital glomus tumor: analysis of 75 cases. Dermatol Surg. 2010;36:1396-400.
6. Verma SB. Glomus tumor-induced longitudinal splitting of nail mimicking median canaliform dystrophy. Indian J Dermatol Venereol Leprol. 2008;74:257-9.
7. Brouillard P, Boon LM, Mulliken JB, Enjolras O, Ghassibé M, Warman ML, et al. Mutations in a novel factor, glomulin, are responsible for glomuvenous malformations (‘glomangiomas’). Am J Hum Genet. 2002;70:866-74.
8. Abdelrahman MH, Hammoudeh M. Glomus tumor presenting as Raynaud’s phenomenon. Case Rep Med. 2012;2012:380540.
9. Moon SE, Won JH, Kwon OS, Kim JE. Subungual glomus tumor: clinical manifestations and outcome of surgical treatment. J Dermatol. 2004;31:993-7.
10. Koç O, Kivrak AS, Paksoy Y. Subungual glomus tumor: magnetic resonance imaging findings. Australas Radiol. 2007;51:B107-9.
Comments are closed.