Our Dermatol Online. 2013; 4(2): 172-175
DOI:. 10.7241/ourd.20132.39
Date of submission: 18.01.2013 / acceptance: 20.02.2013
Conflicts of interest: None
ATROPHIC TYPE OF MORPHEA PROFUNDUS – AN INDIAN EXPERIENCE
Leena Raveendra, Belliappa Pemmanda Raju, Umashankar Nagaraju, Vivekananda, Priya Kootelu Sundar, Lokanatha Keshavalu
Department of Dermatology, Rajarajeswari Medical College and Hospital Kambipura, Kengeri Hobli, Mysore Road, Bangalore, India
Corresponding author: Dr Leena Raveendra e-mail: cbleena@gmail.com
How to cite an article: Raveendra L, Raju BP, Nagaraju U, Vivekananda, Sundar PK, Keshavalu L. Atrophic type of morphea profundus – an Indian experience. Our Dermatol Online. 2013; 4(2): 172-175.
Abstract
Localized scleroderma (also called morphea) is a term encompassing a spectrum of sclerotic autoimmune diseases that primarily affect the skin, but might also involve underlying structures such as the fat, fascia, muscle, and bones. Morphea profundus presenting with atrophic lesions has rarely been reported in the literature. Here we report two cases of morphea profundus presenting with noninflammatory depressed plaques, without any significant skin induration, pigmentation or textural change. Histopathology was confirmatory for morphea profundus.
Key words: morphea profundus; atrophic; multiple
Introduction
The term „morphea” includes a wide spectrum of clinical entities, varying from localized plaques of only cosmetic importance to deep lesions resulting in considerable morbidity for the patient. Four different types of deep morphea have been distinguished: Subcutaneous Morphea, Eosinophilic Fasciitis, Disabling pansclerotic morphea and Morphea Profundus [1]. Morphea profundus is a rare disease and it often has a progressive course with physical and psychological sequelae [2]. Morphea profundus usually presents with early induration followed by atrophy of subcutaneous tissue and on occasion that of muscle [3]. Here we report two cases of atrophic morphea profundus presenting without any significant skin induration, pigmentation or textural change, the published literature on this type of presentation is sparse.
Case Report
Two female patients presented to us with asymptomatic atrophy of skin on multiple sites of the body.
Case-1:
Our first patient was 24 years old and first noticed circumscribed swelling on left arm 2 years back. It was small to begin with and later gradually increased in size and further, after 4-5 months she noticed atrophy of the skin in the same region. She noticed similar lesions adjacent to the old lesion on left arm and also on right arm and on left side of face at inner margin of eye. On examination, there were atrophic areas on her left upper arm (Fig. 1) and right upper arm (Fig. 2) with ill-defined margins. The skin overlying the lesions showed no obvious induration or tenderness. Multiple nodules were present varying in size from 2cm × 1cm to 5cm ×3 cm, hard in consistency, mobile, with skin pinchable over them, distal to the atrophic areas. Swelling of the face involving left lower eyelid and maxillary region measuring about 6 cm × 8 cm was present (Fig. 3). Examination of the surrounding skin, hair, nails and other systems did not reveal any abnormality.
Case-2:
Our second patient was 16 years old and presented with asymptomatic atrophy of the skin of both upper arms and right side of face since seven months. It was first noticed on her right arm followed in a few months by similar lesions gradually appearing on her left arm and her face. On examination, atrophic areas on right side of face (Fig. 4), with ill-defined margins and patchy loss of hair was present in temporal, maxillary and mandibular region. Atrophic areas were also present on right upper arm (Fig. 5) and left upper arm (Fig. 6).The skin overlying the lesions showed no induration or tenderness. Both patients did not complain of pain, redness or itching on these areas. There was no history of trauma or any other skin lesions on these sites prior. There was no history of any systemic illness, and similar lesions in their families. They were not under any medication. Routine blood examination including hemogram, random blood sugar, urea, creatinine, sodium, potassium and liver function tests were normal. Anti-nuclear antibodies, Anti ds-DNA and serologies for Syphilis and HIV were nonreactive. Borrelia serology was not done due to unavailability of laboratory facilities. ESR was raised in both the patients and anti-histone antibody was positive in the first patient. Histopathological examination (Fig. 7, 8) of punch biopsies in both patients showed keratinized stratified squamous epithelium and increased bands of collagenous tissue in the papillary and reticular dermis. Subcutis revealed increased collagen bands. There was perivascular mononuclear infiltrate in the papillary and reticular dermis. A diagnosis of morphea profundus was made based on these typical histological features.
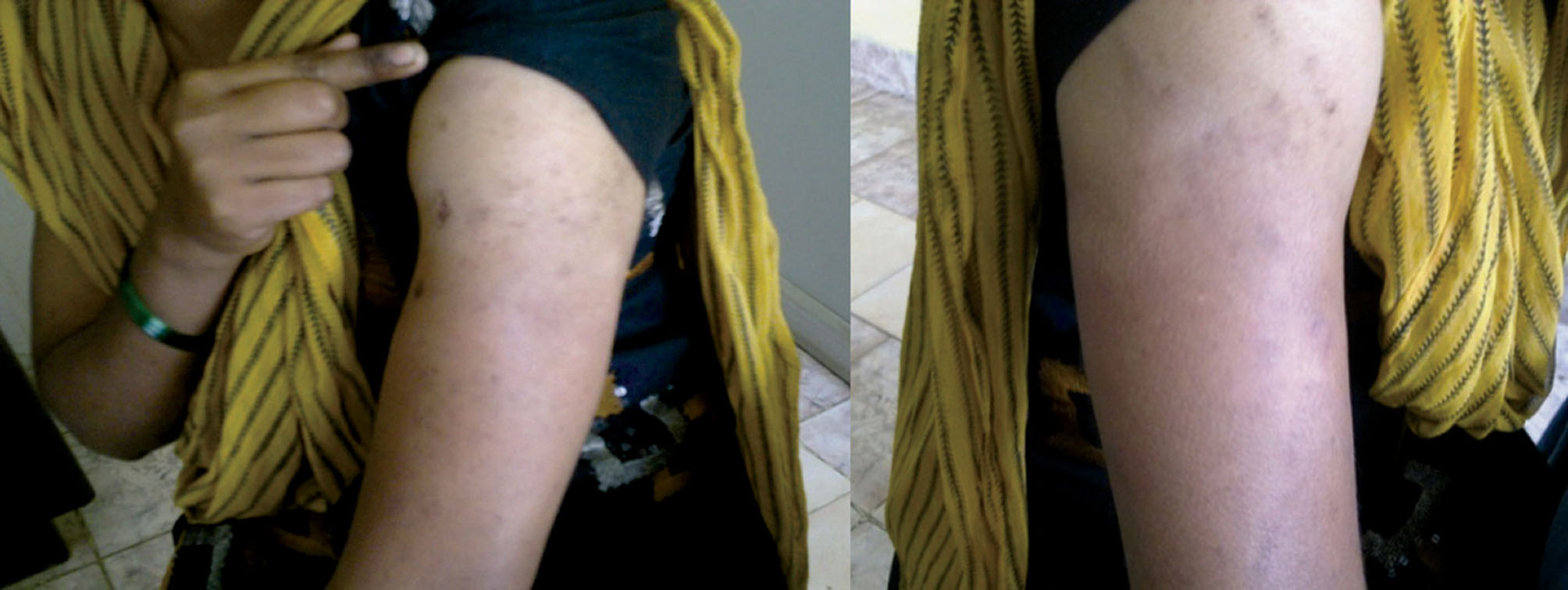 Figure 1. Atrophic areas on left upper arm in case 1; Figure 2. Atrophic areas on right upper arm in case 1
|
 Figure 3. Swelling of left side of face involving left lower eyelid and maxillary region; Figure 4. Atrophic areas on right upper arm in case 2
|
 Figure 5. Atrophic areas on left upper arm in case 2; Figure 6. Atrophic areas on right side of face in case 2
|
 Figure 7. Histopathology from atrophic area in case 1 showing keratinized stratified squamous epithelium and increased bands of collagenous tissue in the papillary and reticular dermis. Perivascular and periadenexal mononuclear infiltrate in the papillary and reticular dermis is seen
|
 Figure 8. Histopathology from atrophic area in case 2 showing normal epithelium and increased bands of collagenous tissue in the papillary and reticular dermis. Perivascular and periadenexal mononuclear infiltrate in the papillary and reticular dermis is seen
|
Discussion
Scleroderma is a chronic disease of unknown aetiology in which sclerosis of the skin develops with or without involvement of internal organs. Based on the presence or absence of systemic disease, scleroderma is divided into very distinct clinical categories: systemic scleroderma or systemic sclerosis, and localized scleroderma or morphea [4]. There are five principal forms of localized scleroderma: plaques, generalized morphea, bullous morphea, linear morphea and morphea profundus [5]. Morphea profundus is a rare variant of morphea and it was first described by Whittaker et al in 1989 as a solitary fibrotic plaque. Morphea profundus usually affects middle aged people and has approximately equal sex distribution. It commonly presents with a single fibrotic plaque and is usually located over the back, shoulder and neck or paraspinal area involving the skin and deeper tissue [8]. Other rare variants of morphea profundus include multiple deep atrophic lesions of the skin without preceding inflammatory changes [7] and noninflammatory cupuliform depressed plaques at sites of previous intramuscular vaccination without significant skin induration, pigmentation or texture change [8]. Bullae arising from plaques of morphea profundus have also been reported [9]. Both of our patients were young women and presented with depressed ill-defined plaques on various sites of the body without induration of skin. We considered a differential diagnosis of morphea profundus and lupus profundus in our first case. Skin biopsy showed features of morphea profundus. Lupus band test on direct immunofluorescence was negative. Lupus band is deposition of immunoglobulins and complement components in the skin of patients with lupus erythematosus as a linear band at the basement membrane zone [10]. Anti-nuclear and Anti ds-DNA antibodies were negative. Antihistone antibody was positive. Antihistone antibodies have been reported in 32% of patients with linear morphea and 25% with localized morphea [11] and it indicates disease activity [12]. High resolution ultrasonography and X-ray showed no involvement of muscle and bone respectively. Based on the investigative reports and typical histopathological findings a diagnosis of morphea profundus was made. In our second patient, differential diagnosis of morphea and localized involutional lipoatrophy was made. Involutional type of lipoatrophy usually presents with a solitary lesion that exhibits decrease in size of the individual adipocytes and is separated from each other by abundant eosinophilic hyaline material, or in some instances by mucoid material [13]. The histopathology in our patient was consistent for morphea. This is the first report on atrophic lesions in morphea profundus from India, to the best of our knowledge. Dermatologists should be aware of this rare variant of morphea profundus, and should consider this in the differential diagnosis of cases which present with atrophic skin lesions.
Acknowledgement
Dr Sushma MD – Assistant Professor, Department of Pathology, Rajarajeswari Medical college and Hospital Kambipura, Kengeri Hobli, Mysore road, Bangalore-560074
REFERENCES
1. Melani L, Cardinali C, Giomi B, Schincaglia E, Caproni M, Fabbri P: Periodic follow-up is necessary in morphea profunda to identify systemic evolution. Skinmed. 2005;4:188-90. 2. Stausbol-Gron B, Olesen AB, Deleuran B, Deleuran MS: Abatacept is a promising treatment for patients with disseminated morphea profunda: presentation of two cases. Acta Derm Venereol. 2011;91:686-8. 3. Amrinder J Kanwar, Dipankar De: Systemic collagen disorders. In: R.G.Valia, Ameet.R.Valia editor. IADVL Textbook of dermatology, 3rd ed. Mumbai: Bhalani Publishing house; 2010.p. 1236. 4. Angelo V, Marzano, Silvano Menni, Aurora Parodi, Alessandro Borghi, Alessandra Fuligni, et al: Localized scleroderma in adults and children. Clinical and laboratory investigations on 239 cases. Eur J of Dermatol. 2003;13:171-6. 5. Brocard A, Quereux G, Moyse D, Dreno B: Localized scleroderma and zinc: a pilot study.Eur J Dermatol. 2010;20:172-4. 6. Whittaker SJ, Smith NP, Jones RR: Solitary morphoea profunda. Br J Dermatol. 1989;120:431–40. 7. Giri S, Paudel U, Jha A, Gurung D, Parajuli S: Morphoea Profunda: Presenting with Atrophic Skin Lesions in a 26 Year Old Female: A Case Report. Clin Med Insights Case Rep. 2012;5:57–62. 8. Khelifa E, Masouye I, Chayaz P, Hauser H, Grillet JP, Borradori L: Primary Atrophic Solitary Morphoea Profunda. Dermatology. 2008;217:207–10. 9. Su WP, Greene SL: Bullous morphea profunda. Am J Dermatopathol. 1986;8:144-7. 10. Mehta V, Sarda A, Balachandran C: Lupus band test. Indian J Dermatol Venereol Leprol. 2010;76:298-300. 11. Sato S, Ihn H, Soma Y, Igarashi A, Tamaki T, Kikuchi K, et al: Antihistone antibodies in patients with localized scleroderma. Arthritis Rheum. 1993;36:1137–41. 12. El-Azhary RA, Aponte CC, Nelson AM: Do antihistone autoantibodies reflect disease activity in linear scleroderma? Arch Dermatol. 2004;140:759–60. 13. Scott N, Mcnutt Abelardo Moreno FÃ:¨lix Contreras: Inflammatory Diseases of the Subcutaneous Fat. In: Elder DE, Elenitsas R, Johnson BL, Murphy GF, editor. Lever’s histopathology of the skin, IX ed. Philadelphia: Lippincott Williams and Wilkins; 2005.p. 537.
Comments are closed.