N Dermatol Online. 2011; 2(2): 68-69
Conflicts of interest: None
MANUBRIOSTERNAL JOINT INVOLVEMENT IN PSORIATIC ARTHRITIS
Hassan Iffat, Yaseen Ummar, Ahmad Mashkoor, Masood Qazi
Postgraduate Department of Dermatology, STD, Leprosy Govt. Medical College, Associated SMHS Hospital, Srinagar-Kashmir, India
Corresponding author: Dr. Iffat Hassan e-mail: hassaniffat@gmail.com
How to cite an article: Hassan I, Yaseen U, Ahmad M, Masood Q. Manubriosternal joint involvement in psoriatic arthritis. Our Dermatol Online 2011; 2(2): 68-69.
Abstract
Psoriatic arthritis (PsA) is a type of seronegative arthiritis associated with psoriasis of skin and nails. It affects axial and eripheral joints with variable severity. The course and prognosis of the disease suggest that early diagnosis and aggressive treatment are important. The most common clinical type of PsA is oligoarthiritis in which four or fewer joints are involved often in an asymmetrical pattern, and arthritis mutilans which is the destructive form and is the least common. We report a case of PsA in which the manubriosternal joint alone was involved as initial manifestation in association with psoriatic erythroderma.
Key words: Psoriasis; Psoriatic arthritis; manubriosternal joint
Introduction
Psoriatic arthiritis (PsA) is a specific form of inflammatory arthritis associated with psoriasis of skin and nails and is usually seronegative for rheumatoid factor. Clinically, five different patterns of the diseases have been described: distal interphalangial arthritis ,oligoarthritis,polyarthritis,arthritis mutilans and spondyloarthropathy [1]. These clinical patterns can change with time and may develop into more destructive forms of the disease.It is therefore suggested that early diagnosis may prevent these adverse outcomes of PsA [2,3]. We hereby report a case of PsA in the form of monoarticular involvement of manubriosternal joint associated with psoriatic erythroderma.
Case Report
A 50 year old male patient who was a known case of psoriasis presented with a two weeks history of acute exacerbation of the disease. Patient was a diagnosed case of psoriasis vulgaris for twenty years and his disease used to get controlled by topical medications but two weeks back the disease got flared up after intake of some ayurvedic drugs. It was associated with fever and malaise. There was no history suggestive of joint pains or any other systemic disease, however, the patient complained of persistent pain over the anterior chest which started three days after the aggravation of disease. On examination, the patient was in erythroderma (Fig. 1) and typical psoriatic plaques were present on scalp and dorsum of hands and feets. Nail examination showed pitting and onycholysis in some of the finger nails. Tenderness and swelling was noted over manubriosternal joint (Fig. 2) and arthritis of the joint was suspected. Rest of the joint examination was insignificant. General physical and systemic examination was normal. Routine investigations like complete blood counts, urine examination, liver function tests and kidney function tests were normal. Serum uric acid was normal (5.6mg/dl). The synovial fluid aspirated from the inflamed joint was negative for crystal deposits. Rheumatoid factor and ANA were normal. Chest x-ray and ECG were normal. An MRI scan of the sternum revealed narrowing of the joint space and articular erosions confirming arthritis of the manubriosternal joint (Fig. 3). In view of the constellation of clinical, laboratory and radiological findings, a diagnosis of PsA of manubriosternal joint was made. The patient was given weekly methotrxate (25mg/wk) and the skin lesions and arthritis showed good response after two weeks and almost resolved completely after 8 weeks of treatment.
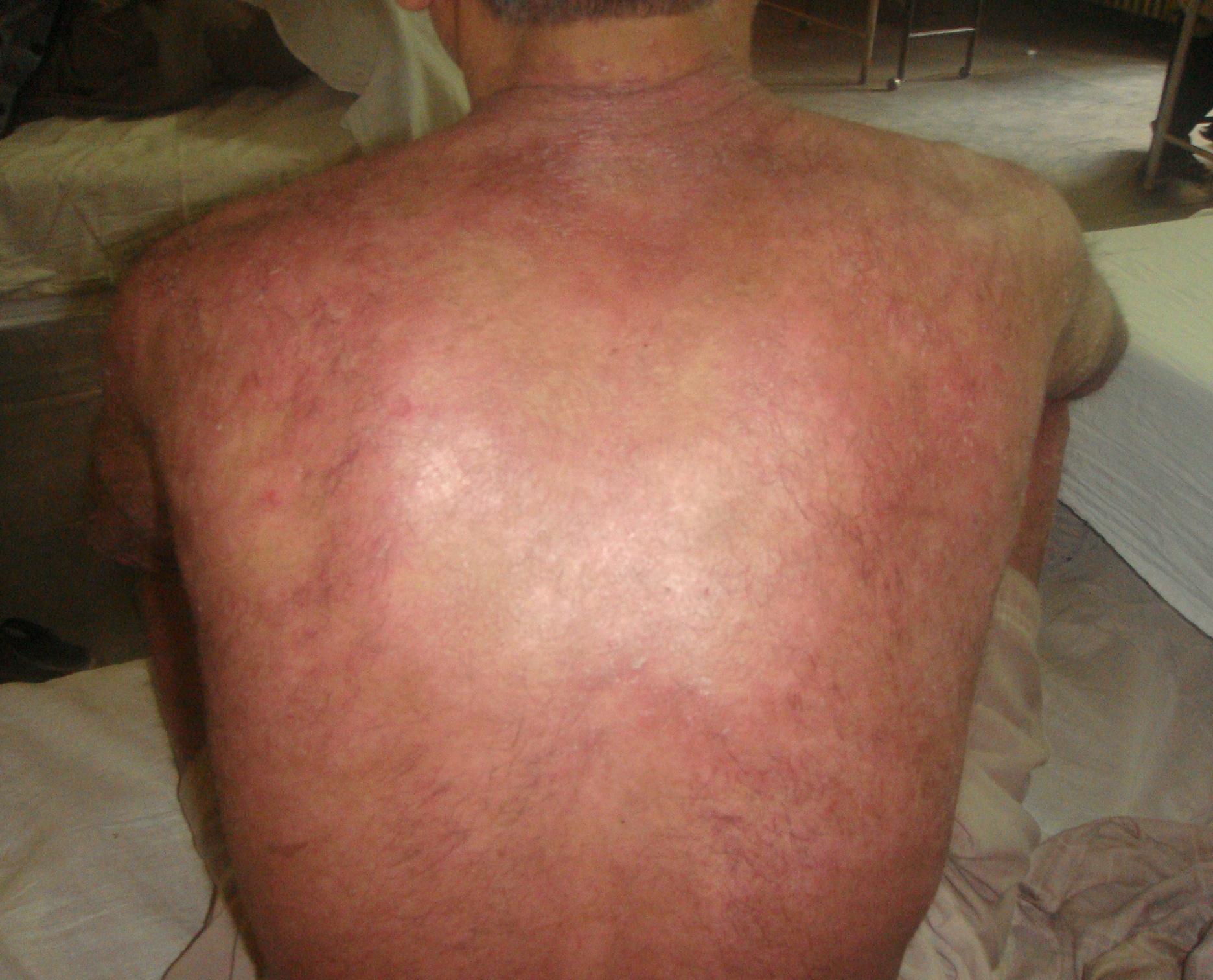 Figure 1. Psoriatic erythoderma
|
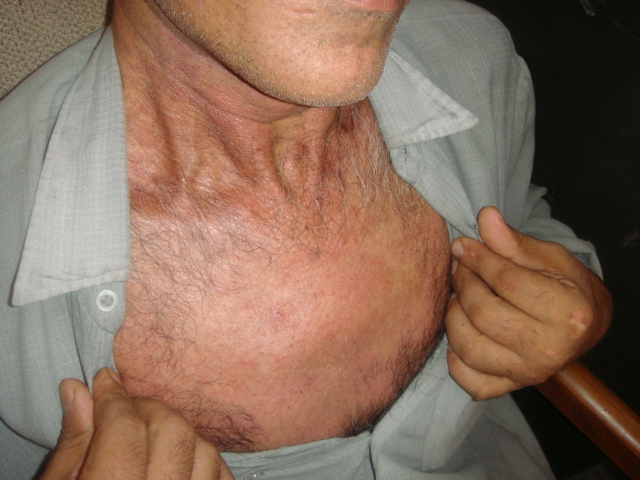 Figure2. involvement of manubriosternal joint
|
 Figure 3. Radiological involvement of the manubrialsternaljoint on MRI
|
Discussion
Psoriatic arthritis (PsA) is classified as seronegative spondyloarthropathy associated with HLAB27. The prevalence of psoriatic arthiritis in general population is reported to be 0.5 percent whereas in psoriatic population it affects about 5-30 percent patients. The diseases can start at any age but the usual age of onset is between 35 and 45 years about 10 years later than psoriasis [4]. However, in 15 percent cases it can precede the diagnosis of psoriasis. The Moll and Wright classification includes five clinical groups: asymmetrical oligoarthritis, symmetrical rheumatoid like pattern, predominantly distal interphalangial type, predominantly axialarthritis which includes spondylitis and sacroilitis and arthritis mutilans which is a destructive form of PsA. Psoriasis of the nails occur in about 75 percent PsA patients as compared to 30 percent with skin lesions alone [5]. Besides the affection of axial and peripheral joints, the involvement of temporomandibular joint is not uncommon in PsA [6]. The involvement of sternal joints as initial manifestation is unusual in PsA. The association of manubriosternal joint arthritis with palmoplantar pustulosis and psoriasis vulgaris has been reported [7]. Nancy et al reported a case of manubriosternal joint arthritis in a patient of generalized pustular psoriasis without involvement of any other axial or peripheral joint [6]. In our case, the patient had psoriasis for two decades but there was no evidence of any joint involvement. The monoarticular involvement of manubriosternal joint in association with psoriatic erythroderma has not been reported earlier and to the best of our knowledge this is the first report of this association. The various treatment options in PsA are NSAIDS, intraarticular corticosteroids, systemic retinoids, immunosupressants such as cyclosporine, azathioprine, and methotrexate, leflunamide. PUVA photochemotherapy and sulfasalazine are used successfully. Recently, TNF-alfa antagonists such as infliximab, etanercept and adalimumab are being increasingly used and are reserved for more severe cases. We treated our patient with weekly methotrexate only.
REFERENCES
1. Wright V, Moll JVH eds: Seronegative olyarthritis.Amsterdam: North Holland Publishing Company. 1976: 169-223.
2. Gladman DD: The natural history of psoriatic arthritis. Ballieres Clin Rheumatol 1994; 8: 379-394.
3. Hellivel PS, Hethen J, Sokoll K, Green M, Marchesoni A Lubreno E et al: Joint symmetry in early and late rheumatoid and psoriatic arthritis with a mathematical model. Arthiritis Rheumatol 2000; 43: 865-871.
4. Moll JMH: Psoriatic arthropathy. In: Mier D, Ven De Kerkoff PCM eds: Textbook of psoriasis. Edinburg Churchhill Livingstone. 1986; 55-83.
5. Wright V: Psoriasis arthritis. Br J Dermatol 1957;96:1-10.
6. Kononen M: Radiographic changes in the condyles of temporomandibular joint in psoriatic arthritis. Acta Radiol 1987; 28: 185-188.
7. Jurik AG, Graudal H, Carvalho A: Monoarticular involvement of manubriosternal joint involvement. Skeltal Radiol 1985; 14: 99-103.
8. Nancy J, Arthur A, Daniel J: Psoriatic arthritis affects manubriosternal joint. Arthritis Rheum 1986; 29: 1029-103
Comments are closed.