Tender erythematous papule on the face
Tasleem Arif1,2
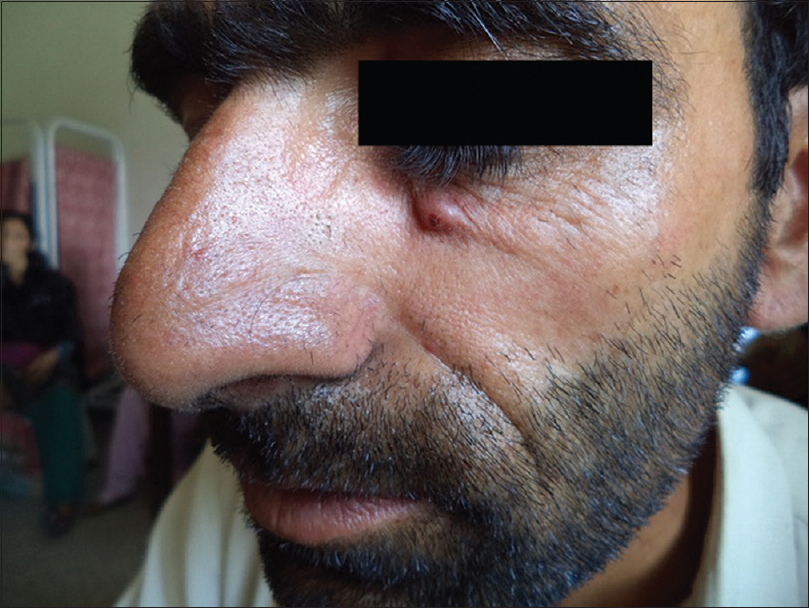
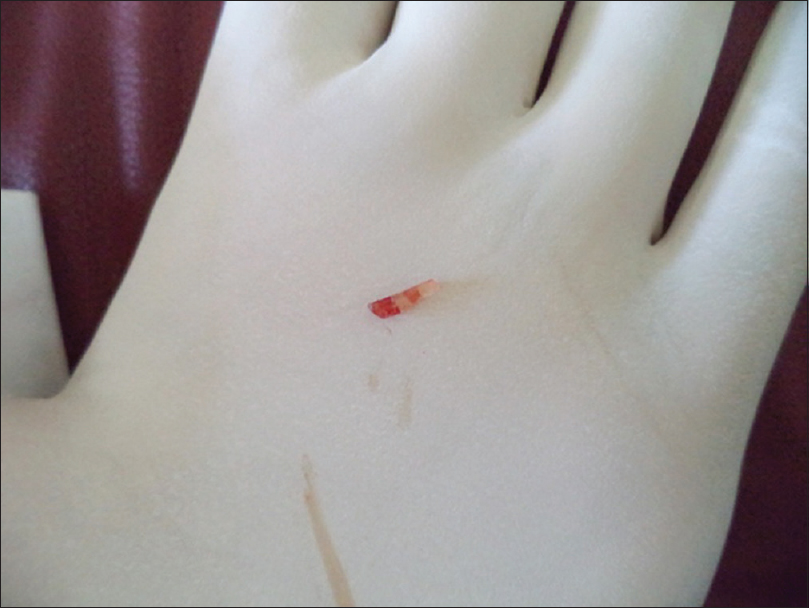
A 36 year old male visited our dermatological outpatient department (OPD) with a chief complaint of a raised reddish skin lesion on the left side of the face for the last one month. There is history of local discomfort associated with the lesion. The patient denied any history of trauma at the affected site. On physical examination, there was an erythematous papule around 1 cm in diameter present on the left side of the face 2-3 cm below the left lower eyelid (Fig. 1). It was firm in consistency and exquisitely tender. The summit of the papule was relatively harder and was the site of maximum tenderness. After manipulating the lesion in the minor operation theatre, a glass fragment of the size 9-10 mm × 2-3 mm was removed from the lesion (Figs 2A–B, and 3). A diagnosis of foreign body reaction to the glass was made. The affected skin at the lesional site was irrigated with normal saline. The patient was prescribed topical fluticasone plus mupirocin ointment and oral antibiotics in the form of Amoxycillin and clavulanic acid 625 mg thrice a day for one week. The lesion regressed completely in 2-3 weeks.
Figure 1: An erythematous papule on left side of the face
Figure 2: (A) Glass slit projecting out from the top of the erythematous papule (frontal view); (B) 2-3 mm of glass slit clearly visible coming out from the summit of the papule (lateral view)
Figure 3: Glass foreign body which has caused the foreign body reaction (9-10 mm × 2-3 mm)
Foreign body granuloma is a reaction pattern to either endogenous materials (hair shafts, keratin, cholesterol, etc.) or exogenous substances (suture material, glass, oil droplets, wooden material, metals, silica, etc.) which are immunologically inert. Soft tissue foreign bodies mostly occur secondary to some abrasive or penetrating trauma. These can lead to discomfort, delayed wound healing, deformity, localized and systemic infections [1–3]. A number of different types of foreign bodies elicit a granulomatous response which clinically present as erythematous brown or purple papules, plaques or nodules.
With the passage of time such lesions often become harder due to fibrosis. Retained foreign bodies can lead to bacterial infection while the vegetative foreign bodies have been reported to cause fungal infection [4].
CONSENT
The examination of the patient was conducted according to the Declaration of Helsinki principles. Written informed consent was obtained from the patient for publication of this article and any accompanying images.
REFERENCES
1. DeBoard RH, Rondeau DF, Kang CS, Sabbaj A, McManus JG, Principles of basic wound evaluation and management in the emergency departmentEmerg Med Clin North Am 2007; 25: 23-39.
2. Hollander JE, Singer AJ, Valentine SM, Shofer FS, Risk factors for infection in patients with traumatic lacerationsAcad Emerg Med 2001; 8: 716-20.
3. Stone DB, Koutouzis TK, Roberts JR, Hedges JR, Chanmugam AS, Foreign body removalClinical Procedures in Emergency Medicine 2004; 4th ed. Chap 37Philadelphia, Pa: Saunders; 694-715.
4. Kennedy CCT, Burd DAR, Creamer D, Burns T, Breathnach S, Cox N, Griffiths C, Mechanical and Thermal InjuryRook’s Textbook of Dermatology 2: 8th edition. U.K: Wiley-Blackwell; 28.39-28.51.
Notes
Source of Support: Nil
Conflict of Interest: None declared.

Comments are closed.