Ulcerated Cutaneous Leishmaniasis
Patricia Chang1, Tyson Meaux2, Gylari Calderon1, Lorena Bay3
CLINICAL CASE
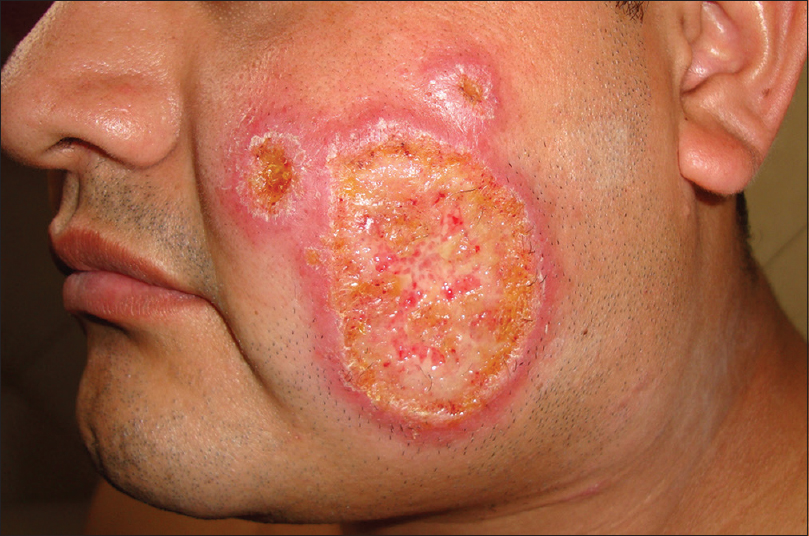
This is a case of a twenty-nine year old male patient who was referred to our dermatology service with an ulcerative lesion of the left cheek of approximately 4 cm, circular, with well-defined borders and a clean base of granulation tissue, as well as 2 ulcerated nodular lesions (Fig. 1). The rest of the physical exam was within normal limits.
Figure 1: Large Ulcer with clean base, well-defined erythematous borders and two nodular, ulcerated, satellite lesions
Family and personal history were noncontributory. The lesion on the left cheek first appeared two and a half months earlier, with a “clay-like appearance”, which he tended to scratch often. Gradually the lesion reached its current state, for which he sought treatment with an outside dermatologist. Presumptive diagnosis was deep fungal infection versus cutaneous leishmaniasis, and biopsy of the lesion showed a granulomatous process with negative Fite, PAS, and Gomori trichome stain. The patient was then referred to our dermatology service. Differential diagnosis included ulcerated cutaneous leishmaniasis, cutaneous lymphoma, and pyoderma gangrenosum. Upon further questioning, the patient claimed to have recently visited his homeland, Chisec Coban, which is an area in Guatemala that is endemic for leishmaniasis. We performed a microscopic examination of the lesion with Giemsa stain, obtained by skin scraping, was negative and another biopsy for histologic examination, along with fungal and bacterial culture. Histologic examination of the second biopsy again showed a granulomatous process highly suspicious for Leishmaniasis. More specifically, the lesion showed an epidermis with hyperkeratosis and parakeratosis with areas of plasma cells and neutrophils. Irregular acanthosis with thick rete ridges, some of them fused, with moderate spongiosis. From the papillary dermis to the deep reticular dermis, a dense diffuse inflammatory infiltrate consisting of histiocytes, lymphocytes, neutrophils, plasma cells and occasional eosinophils. Giemsa, periodic acid- Schiff (PAS) and Kinyoun were negative. The patient was sent to the Section of Parasitology of the National Laboratory of Health Leishmaniasis Unit confirmed the diagnosis of leishmaniasis with a scraping of the lesion examined with Giemsa stain, and the patient was started on intralesional and intramuscular glucantime 20, which led to complete healing of the lesion (Fig. 2).
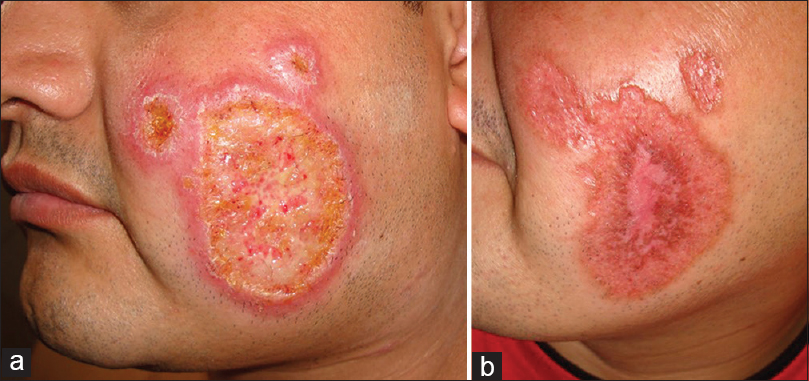
Figure 2: Pre and post treatment with Glucantime. a: Cutaneous Lesions before treatment. b: One month after treatment
DISCUSSION
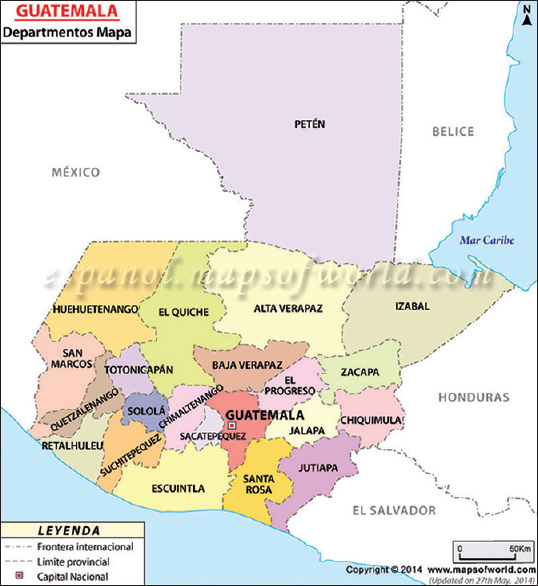
Cutaneous Leishmaniasis is a parasitic disease endemic to much of Latin America, and is caused by the species L. braziliensis, L. mexicana, L. panamensis/L. guyanensis, among others. The organism is transmitted by the bite of an infected female sandfly of the genera Phlebotomus or Lutzmyia, with lesions typically located on exposed areas of the body [1]. Manifestations may include single or multiple localized cutaneous ulcers, or diffuse cutaneous lesions with possible mucosal involvement, typically caused by L. Mexicana. Cutaneous lesions may consist of ulcers, reddish-brown, firm, infiltrative nodules, or verrucous plaques that may or may not ulcerate [2–5]. Along with a history of travel to an endemic area, the following are useful for the diagnosis of cutaneous leishmaniasis: microscopic analysis of skin scrapings revealing amastigotes, punch biopsy with tissue-impression smears, and needle aspiration of tissue fluid from the margin of a lesion with culture of the fluid to isolate the organism and identify the species [3]. Although lesions may heal spontaneously within 12-18 months, topical medications such as paromomycin sulfate 15% plus methylbenzethonium chloride 12%, ketoconazole cream under occlusion, cryotherapy, local heat, photodynamic therapy, laser ablation, and 100 ml intralesional sodium stibogluconate antimony are often used to avoid significant scarring of exposed areas, especially the face. Five milliliters of intralesional Antimony n-methyl glutamine (Glucantime) is often used in Central and South America due to local availability and efficacy [2,4]. Insecticides and pyrethroid-impregnated curtains are useful to prevent cutaneous leishmaniasis [3]. In Guatemala, the endemic areas for leishmaniasis are Peten, Huehuetenango, El Quiche, Alta Verapaz, and Izabal, and the most important area is Peten, with 80 percent of the cases (Fig. 3) [6].
Figure 3: Areas endemic for leishmaniasis in Guatemala
CONSENT
Written informed consent was obtained from the patient for publication of this case report and any accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of this journal.
REFERENCES
1. Magill AJ, Mandell GL, Bennett JE, Dolin R, Leishmania SpeciesPrinciples and Practice of Infectious Diseases 2010; 7th ed [Ebook]. chapter 276Churchill Livingston Elsevier;
2. James WD, Berger TG, Elston DM, Parasitic Infestations, Stings, and Bites in: Andrews’ Diseases of the Skin: Clinical Dermatology2006; Saunders Elsevier; 415-7.
3. Markele WH, Khaldoun MMO, Cutaneous leishmaniasis: recognition and treatmentAm Fam Physic 2004; 69: 1455-60.
4. Chang P, Acajabon MVV, Calderon G, Bay L, Leishmaniasis cutánea con facies leonineDermatol Rev Mex 2014; 58: 278-84.
5. Arenas R, Leishmaniasis in: DermatologiaMcGraw-Hill De Mexico 1987; 447.
6. Arana BA, Navin TR, Rizzo NR, Navin TR, Epidemiologia de la LeishmaniasisLa Leishmaniasis Cutanea en Guatemala 1994; 16.
Notes
Source of Support: Nil
Conflict of Interest: None declared.
Comments are closed.