Pyoderma gangrenosum associated with ulcerative colitis. Case report and literature review
Mirela Vasileva 1, Vesna Brishkoska Boshkovski2
1, Vesna Brishkoska Boshkovski2
1Clinical Hospital Shtip, Shtip, Republic of Macedonia; 2General City Hospital 8th September, Skopje, Republic of Macedonia
Corresponding author: Dr. Mirela Vasileva
Submission: 01.05.2020; Acceptance: 18.07.2020
DOI: 10.7241/ourd.2020e.119
Cite this article: Vasileva M, Brishkoska Boshkovski V. Pyoderma gangrenosum associated with ulcerative colitis. Case report and literature review. Our Dermatol Online. 2020;11(e):e119.1-e119.3.
Citation tools:
Copyright information
© Our Dermatology Online 2020. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
Pyoderma gangrenosum (PG) is currently considered as a reactive inflammatory dermatosis and part of the spectrum of neutrophilic dermatosis.The etiology of PG is still unknown, and its pathophysiology is far from fully understood. Inflammatory bowel disease (IBD), PAPA (pyogenic arthritis, PG and acne) and PAPA-related syndromes often develop with PG. Diagnosis largely depends on careful observation of clinical features and disease progression. We present a case of a 30-year-old patient with an ulcer on the right lower leg who does not respond to standard therapy. The patient has no other accompanying symptoms. After a complete examination, the diagnosis of ulcerative colitis is made, as a very common pyoderma gangrenosum associate disease. A complete examination of cases of ulcers that not respond to the classic therapy is required. PG treatment and diagnosis is a real challenge and requires a wide range of tests.
Key words: Pyoderma gangrenosum; Ulcers; Ulcerative colitis
INTRODUCTION
PG is currently considered as a reactive inflammatory dermatosis and part of the spectrum of neutrophilic dermatosis.
The disease was first described by Brocq in 1916 as a “phagedenismegeometrique” and later named by Brunsting in 1930 who believed it was a streptococcal infection that caused gangrene [1].
The incidence of PG is estimated to be, 3 to 10 cases per million people per year [2]. PG affects individuals of any age, but is more common in young adults aged 25 to 54, and women are more commonly affected than men [3]. Rarely occur in children (less than 4% of cases), these cases are usually associated with other systemic diseases [2,4]. The clinical presentation of PG is variable, but is essentially characterized by multiple or single painful ulcerative skin lesions that progress rapidly and have a colorful, erythematous appearance. The lower extremities are most commonly affected [4].
ETIOPATHOGENESIS
The etiology of PG is still unknown, and its pathophysiology is far from fully understood. Inflammatory bowel disease (IBD), PAPA (pyogenic arthritis, PG and acne) and PAPA-related syndromes often develop with PG. In addition, other neutrophilic skin diseases, namely Sweet’s syndrome (SS) or Behçet’s disease, share clinical and pathological aspects with PG [5].
What is known so far in the etiopathogenesis of the disease are immune factors and neutrophil dysfunction. Immune factors include association with autoimmune diseases, the Pathergy phenomenon, a defective cell-mediated immune response, and the present deposits of immunoglobulins in dermal blood vessels [5].
Factors that cause immune, neutrophilic abnormalities are multiple and include genetic predisposition, parainflammatory, paraneoplastic, or paraimmunic phenomenon. In patients with a predisposition, the cause of PG may be a small trauma that, instead of a normal response that recognizes and removes the damaged tissue, will result in PG lesions. PG can also occur as a result of drug therapy such as granulocyte stimulating factor, inhibitor of epidermal receptor growth factor, and isotretinoin [5].
DIAGNOSIS
There are no characteristic changes during laboratory tests, elevated sedimentation rate, leucocytosis, and elevated C-Reactive protein (CRP) values are present. Sometimes anemia is present. Autoantibodies and circulating immune complexes are not usually detected. Biopsy and histopathological examination may show sterile neutrophilia and lymphocytic vasculitis, which may rule out other etiologies of skin ulcers.
Diagnosis largely depends on careful observation of clinical features and disease progression, for example ulcerative lesions are very painful and progress rapidly [3]. The presence of the Pathergy phenomenon, the association with some autoimmune diseases also helps in diagnosis [3].
TREATMENT
Treatment is a real challenge because there is no generally accepted gold standard for treating this disease. Therapeutic approaches are aimed at immune mediators and inflammatory cells [5].
The main goal of treatment is to limit tissue destruction and achieve closure of the ulcers with the best possible aesthetic result. Due to the present Pathergy phenomenon, it is necessary to avoid surgical debridement and skin grafting.
Drug therapy, intralesional corticosteroids, azathioprine or 6-mercaptopurine, topical Chromoglycate, Dapsone, and Cyclosporine are favored to improve the condition.
Corticosteroids are considered the first line of treatment, while other immunosuppressant and cytostatics are used as the second line therapeutics [2].
In the case of malignancy, immunosuppression should only be performed at minimal doses or not at all. PG can be linked to malignancy, which sometimes precedes diagnosis, so immunosuppressants as well as biological agents can be very risky to use. It is not excluded that a secondary infection of the ulceration is present, which requires the inclusion of an antibiotic in the therapy [2].
Patients with a mild form of the disease, especially those with superficial granulomatous form of PG, respond well to topical therapy. Topical corticosteroids, tacrolimus, sodium chromoglycate, nicotine, 5-aminosalicylic acid, and intralesional corticosteroids and cyclosporine give satisfactory results [5].
It is also necessary to manage the pain of patients with gradual reduction of analgesics at the first signs of clinical improvement.
CASE REPORT
A 30-year-old patient complains of changes in the right lower leg in the form of purulent ulcers that appeared a few months ago, followed by intense pain. The patient had no symptoms other than pain at the site of the ulceration. Local therapy with Hydrocolloid dressings and intravenous antibiotic was performed. The treatment had no effect, the ulceration continued to increase (Figs. 1a and 1b), after which we decided to take a biopsy. Histopathological analysis showed portions of papillary hyperplasia of epidermis with a zone of necrosis and blood flow with inflammatory cells of neutrophils, eosinophils, plasma cells, and rare lymphocytes.
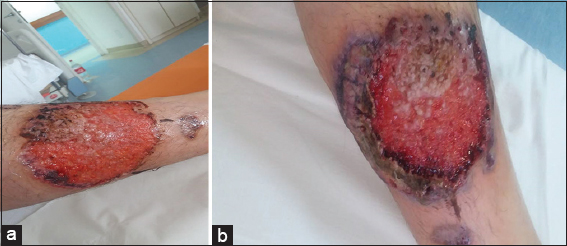 |
Figure 1: (ab) Ulcerative stage of rapidly progressive pyoderma gangrenosum ulcer, showing an elevated, purple, undermined with signs of necrosis edges, with hemorrhagic base. |
Laboratory tests show anemia, elevated (complement) C4 (0.407g/L), and high CRP (34.7mg/L) level.
The patient complaint that she occasionally felt abdominal pain, after which we decided to be thorough with the examinations. We first did an ultrasound examination of the abdomen that showed no abnormalities. MR enterography and colonoscopy were performed also without any pathological changes.
systemic antibiotics, gastroprotective, antioxidant therapy, and appropriate topical therapy were performed, but only after engaging an corticosteroid therapy, improvement of dermatological status followed. Improvement was evident only one week after the corticosteroid treatment. After a month of hospitalization, the patient was released for home treatment with frequent check-ups and dressings.
The patient comes to regular check-ups where a significant improvement in the condition is monitored (Fig. 2). After three months, she developed gastrointestinal problems, so after consultation with gastroenterologist and after a repeated colonoscopy, she was diagnosed with Ulcerative Colitis. With combination therapy by a gastroenterologist and dermatologist, the changes are intensely reversed.
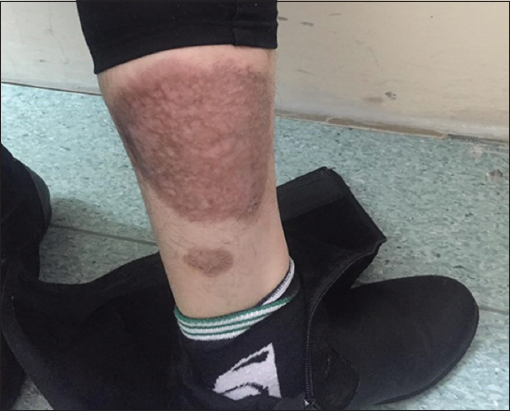 |
Figure 2: Hyperpigmented scar, 6 months after systemic therapy. |
DISCUSSION
There are several scientific papers that link this disease to autoimmune diseases, which has been confirmed in our case [3–5]. It is very important to differentiate between diagnoses. The presence of nonspecific systemic symptoms such as fever, arthralgia and the pathohistological finding in addition to neutrophilia is reason to think of pyoderma gangrenosum. The absence of symptoms of another disease is not a sure sign that there is no other accompanying autoimmune disease. We were able to make a timely diagnosis thanks to the clinical picture and the suspected pathohistological finding. Our persistence in diagnosing autoimmune disease in the background did not work, but 3 months later the diagnosis we suspected was made, and the tests, although initially negative, were not in vain.
CONCLUSION
A complete examination of cases of ulcers that not respond to the classic therapy is required. Local treatment of the wound is of particular importance in the treatment, but in this case it is not enough. The treatment of the disease in the background has proved to be an important factor in the rapid closure of ulcerations. In this disease we must not forget the psychological factor and the impact of the disease on the patient, in this case it is a young woman who has repeatedly emphasized the aesthetic problem. Early diagnosis leads to appropriate treatment and thus prevention of major psychological problems that the patient may face.
PG treatment and diagnosis is a real challenge and requires a wide range of tests.
Consent
The examination of the patient was conducted according to the Declaration of Helsinki principles.
The authors certify that they have obtained all appropriate patient consent forms. In the form the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
REFERENCES
1. Bhat RM, Nandakishore B, Sequeira FF, Sukumar D, Kamath GH, Martis J, et al. Pyoderma gangrenosum:An Indian perspective. Clin Exp Dermatol. 2011;36:242-7.
2. Bhat RM. Pyoderma gangrenosum:An update. Review Article. Department of Dermatology, Venereology and Leprosy, Fr Muller Medical College, Kankanady, Mangalore, India September 28, 2016.
3. Bennett Michelle L, Jackson JM, Jorizzo JL, Fleischer AB, White WL, Callen JP. Pyoderma gangrenosum a comparison of typical and atypical forms with an emphasis on time to remission. case review of 86 patients from 2 institutions. Medicine. 2000;79:37-46.
4. El Anzi O, Sqalli A, Maouni S, Znati K, Meziane M, Ismaili N, et al. Unusual presentation of pyoderma gangrenosum in an infant. Our Dermatol Online. 2019;10:308-9.
5. Gameiro A, Pereira N, Cardoso JC, Gonçalo M. Pyoderma gangrenosum:challenges and solutions. Clin Cosmet Investig Dermatol. 2015;8:285- 93.
Notes
Source of Support: Nil,
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0002-6807-5557 http://orcid.org/0000-0002-6807-5557 |



Comments are closed.