Rickettsiosis in a child
Rhizlane Chaoui , Hanane Baybay, Selma El Kadiri, Sara Oukarfi, Zakia Douhi, Sara Elloudi, Fatima Zahra Mernissi
, Hanane Baybay, Selma El Kadiri, Sara Oukarfi, Zakia Douhi, Sara Elloudi, Fatima Zahra Mernissi
Department of Dermatology,University Hospital Hassan II, Fez, Morocco
Corresponding author: Dr. Rhizlane Chaoui
Submission: 29.02.2020; Acceptance: 08.04.2020
DOI: 10.7241/ourd.2020e.34
Cite this article: Chaoui R, Baybay H, El Kadiri S, Oukarfi S, Douhi Z, Elloudi S, Mernissi FZ. Rickettsiosis in a child. Our Dermatol Online. 2020;11(e):e34.1-e34.2.
Citation tools:
Copyright information
© Our Dermatology Online 2020. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
Sir,
A 10 year old girl, was admitted to emergency department because of fever, headache, anorexia, myalgias that was present 4 days following a bite insect with itchy, hot and painfull erythematous swelling on the right knee. She was treated initially with analgesics and antibiotics (amoxicillin) without response.
After one day, a skin rash was appear involving the entire body. She was otherwise healthy.
On her admission, she was conscious and had a fever of 39°C.
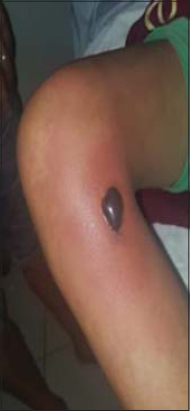
Dermatological examination revealed a hot, painful and poorly demarcated erythema of the right leg with an haemorrhagic bullae on the inner side of the right knee (Fig. 1). Maculopapular rash was noted on trunk, forearms, lower limbs, buttocks and palms (Fig. 2).
No palpable lymphadenopathy was noted and the abdomen was soft with no organomegaly.
In front of this clinical presentation,diagnosis of rickettsiosis was suspected. Laboratory tests were unremarkable and rickettsia serology was negative.
The patient was prescribed doxycycline 200 mg per day with a good improvement after 7 days of treatment (Fig. 3).
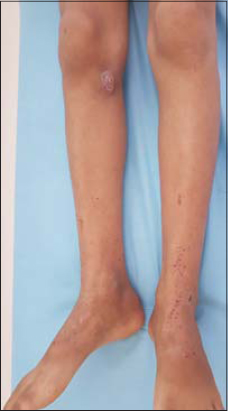 |
Figure 3: Complete healing and clearance of lesions after 7 days of treatment. |
Rickettsial diseases are a group of various and specific communicable diseases caused by obligate intracellular gram negative bacilli and transmitted to man by arthropod vectors (tick, mite, flea and louse) [1].
Severity of manifestations varies from a mild, self-limiting illness to a life threatening disaster.
Initially patients present with nonspecific symptoms such as headache, fever, anorexia, arthromyalgia. Gastro-intestinal symptoms can be seen early in this disease. Skin rash is usually not present until after 2–4 days of illness. Cutaneous signs include Maculopapular rash that spreads rapidly to involve the entire body, purpuric rash, painless eschar at the site of inoculation [2].
Rickettsial illness can involved lung, heart, kidney, central nervous system and gastrointestinal system.
The diagnosis of a rickettsial disease has most often been confirmed by serological testing [3].
Treatment of choice for all age groups include Doxycycline and it must to be started early because a delay in initiating treatment may prove fatal [4].
Our observation illustrated a case of rickettsiosis whose diagnosis is made despite a negative serology while relying on other arguments of strong presumption.
Consent
The examination of the patient was conducted according to the Declaration of Helsinki principles.
The authors certify that they have obtained all appropriate patient consent forms. In the form the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
REFERENCES
1. Kulkarni A. Childhood rickettsiosis. Indian J Pediatr. 2000;78:81–7.
2. Mouffok N, Parola P, Lepidi H, Raoult D. Mediterranean spotted fever in Algeria —new trends. Int J Infect Dis. 2009;13:227–35.
3. Blacksell SD, Sharma NP, Phumratanaprapin W, Jenjaroen K, Peacock SJ, White NJ, et al. Serological and blood culture investigations of Nepalese fever patients. Trans R Soc Trop Med Hyg. 2007;101:686–90.
4. Baker CJ. Red book atlas of paediatric infective disease. AAP. 2007;217–23.
Notes
Source of Support: Nil.
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/000-0003-3455-3810 http://orcid.org/000-0003-3455-3810 |




Comments are closed.