Coexsitence of facial and oral lichen planus pigmentosus
Rhizlane Chaoui , Selma El Kadiri, Zakia Douhi, Sara Elloudi, Hanane Baybay, Fatima Zahra Mernissi
, Selma El Kadiri, Zakia Douhi, Sara Elloudi, Hanane Baybay, Fatima Zahra Mernissi
Department of Dermatology,University Hospital Hassan II, Fez, Morocco
Corresponding author: Dr. Rhizlane Chaoui
Submission: 27.02.2020; Acceptance: 08.04.2020
DOI: 10.7241/ourd.2020e.33
Cite this article: Chaoui R, El Kadiri S, Douhi Z, Elloudi S, Baybay H, Mernissi FZ. Coexsitence of facial and oral lichen planus pigmentosus. Our Dermatol Online. 2020;11(e):e33.1-e33.2.
Citation tools:
Copyright information
© Our Dermatology Online 2020. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
Sir,
A 45-year-old, phototype IV female presented with darkening and mild itch on the face of one year’s duration. She was otherwise healthy, no history of exposure to drugs,toxic fumes,sun exposure or heavy metals could be elicited.7 months later, she developed sudden hyperpigmentation on the oral mucosa.
Dermatological examination revealed gray-brown pigmented macules with a smooth surface that had become confluent, forming pigmented patches with a reticular pattern on the cheeks,nose and labial area (Fig. 1).
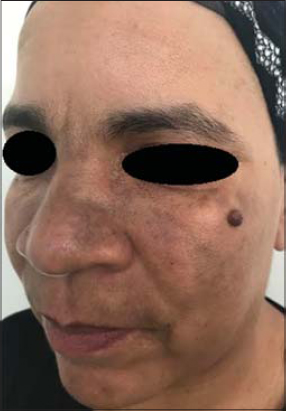 |
Figure 1: Multiple confluent gray-brown pigmented macules confluent on the cheeks,nose and labial area. |
Insepection of the oral cavity showed extensive pigmentation interspersed with whitish patchs that occupied almost the entire inner surface of the right cheek (Fig. 2). The rest of the physical examination was normal.
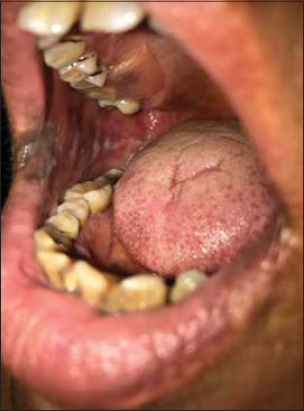 |
Figure 2: Extensive pigmentation interspersed with whitish patchs that occupied almost the entire inner surface of the right cheek. |
On dermoscopy, we observed exaggerated pseudoreticular pigmentary network with grey Peririfollicular globules and dots on the lesion of face (Fig. 3).
 |
Figure 3: Dermoscopy showed exaggerated pseudoreticular pigmentary network with gray perifollicular globules and dots on the face. |
These findings, in correlation with clinical examination, supported the diagnosis of facial and oral lichen planus pigmentosus.
Routine laboratory data including blood cell count and serology for hepatitis B and C were normal.
The patient was treated with topical tacrolimus 0.1% ointment twice daily, and measures of sunscreen for 4 months with partial improvement.
Lichen planus pigmentosus (LPPig), first described by Bhautani et al. [1] is a rare variant of classic lichen planus of unclear etiology that tends to occur in middle-aged individuals with skin types III to VI [2].
Clinically, lesions appear as small, dark brown, discrete, ill-defined, oval to round macules, which later become confluent to form large patches, located on sun-exposed areas of the face, neck, and flexural folds [2].
The mucous membrane,scalp, palms, soles, nail are rarely involved [3].
In rare instances pigmentation may be associated with the development of oral lichen planus,or follows its disappearance [4].
Dermoscopic features of LPPig includes exaggerated pseudoreticular network, gray-brown or gray-blue perifollicular globules and dots,vascular changes might be found in some cases [5].
The differential diagnosis of LPP should be established with a group of hyperpigmentation disorders, such as melasma, exogenous ochronosis, Riehl’s melanosis and erythema dyschromicum perstans (EDP) or ashy dermatosis. In our case the diagnosis of LPPig was facilate by the occurence of pigmentation in the oral mucosa.
There are no established treatments for LPP,but generally treatment consists of topical steroids, tacrolimus, depigmenting agents, photoprotection, and Q-switched Nd-YAG laser [6].
The case is being reported on account of the rarity of oral lichen planus pigmentosus.
Consent
The examination of the patient was conducted according to the Declaration of Helsinki principles.
The authors certify that they have obtained all appropriate patient consent forms. In the form the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
REFERENCES
1. Bhutani LK, Bedi TR, Pandhi RK, Nayak NC. Lichen planus pigmentosus. Dermatologica. 1974;149:43–50.
2. Takeoka S, Tada Y, Ohnishi T, Watanabe S. Case of lichen planus pigmentosus with unique distribution. J Dermatol. 2015;42:652–4.
3. Rieder E, Kaplan J, Kamino H, Sanchez M, Pomeranz MK. Lichen planus pigmentosus. Dermatol Online J. 2013;19:20713.
4. Lambertini M, Patrizi A, Ravaioli GM, Dika E. Oral pigmentation in physiologic conditions, post-inflammatory affections and systemic diseases. G Ital Dermatol Venereol. 2018;153:666-71.
5. Sonthalia S, Errichetti E, Kaliyadan F, Jha AK, Lallas A. Dermoscopy of lichen planus pigmentosus in Indian patients –Pitfalls to avoid. Indian J Dermatol Venereol Leprol. 2018;84:311-3.
6. Al-Mutairi N, El-Khalawany M. Clinicopathological characteristics of lichen planus pigmentosus and its response to tacrolimus ointment:an open label, non-randomized, prospective study. J Eur Acad Dermatol Venereol. 2010;24:535–40.
Notes
Source of Support: Nil.
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/000-0003-3455-3810 http://orcid.org/000-0003-3455-3810 |



Comments are closed.