Hookworm – Related cutaneous larva migrans: Case report
Siham Boularbah , Zakia Douhi, Sabrina Oujidi, Mariam Soughi, Sara Elloudi, Hanane Baybay, Fatima Zahra Mernissi
, Zakia Douhi, Sabrina Oujidi, Mariam Soughi, Sara Elloudi, Hanane Baybay, Fatima Zahra Mernissi
Department of Dermatology, CHU Hassan II, Fez, Morocco
Citation tools:
Copyright information
© Our Dermatology Online 2023. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
Hookworm-related cutaneous larva migrans is caused by the intradermal migration of soil-dwelling filariform larvae of dog and cat hookworms, most commonly Ancylostoma, usually develop itchy skin lesions, usually consisting of migrating superficial serpiginous traces, or sometimes stationary follicular eruptions. The plantar topography or on the regions of the body in contact with the sand of the beaches of the Antilles, West Africa and East Asia, the presence of fine and not very mobile serpiginous furrows and eczematization with vesiculobullous eruption, are characteristic. There are misleading profuse forms such as pseudo-folliculitis. We present a Moroccan patient who developed the disease after their return from and who responded well to treatment with albendazole.
Key words: Larva migrans; Albendazole; Serpiginous lesions
INTRODUCTION
Hookworm cutaneous larva migrans is a rare condition. It is due to accidental transcutaneous penetration in humans, most often young, of hookworm larvae of animal origin. Generally, at the level of the feet, the legs, the buttocks or the back [1] according to a sinuous path. We report a case of Moroccan holidaymakers who developed extensive illness after their return from Italy with multiple infestations on the hands.
CASE REPORT
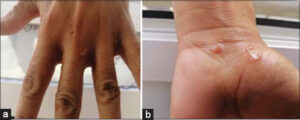
A 70 year old man, no pathological history, after 5 days of his return from Italy, he had noticed pruritic erythematous lesions on the wrist of the right hand (Fig. 1a) and the back of the left hand without notion of family or nocturnal pruritus or other associated systemic signs. History records prolonged dermal exposure to soils. Clinical examination revealed serpiginous sinuous lesions at the wrist of the left hand (Fig. 1b) and the back of the right hand. Dermoscopy did not show signs of scabies View the clinical context based on the serpiginous and itchy appearance of the eruption, absence of familial pruritus, absence of dermoscopic signs of scabies, the diagnosis of cutaneous larva migran was retained. The patient was treated with Albendazole at a dose of 200mg/d for three days with good improvement after 24 hours of treatment.
DISCUSSION
The cutaneous larva migrans syndrome or hookworm dermatitis corresponds to the active transcutaneous penetration in humans of hookworm larvae found in moist and warm soils soiled by the defections of animals, in particular dogs, cats, and other mammals 2]. Mainly caused by Ancylostoma braziliense, Ancylostoma caninum, Ancylostoma ceylonium, Uncinaria steoncephala, Bubostomum phlebotomus [1,2]. these organisms are most commonly found in tropical climates such as the southeastern United States, Latin America, the Caribbean, Southeast Asia. The point
of entry, usually the feet, legs, buttocks, or back, the parasites move up in a random pattern, causing a red-brown, raised, thread-like, curvy rash [2].
Tourists traveling to endemic areas who are affected have tended to be younger [3]. Our patient, meanwhile, is an elderly patient, and the point of penetration are hands without affecting the feet, probably because of their frequent extension with the contaminated soil in the heart of his bolot,
Clinically, the initial and pathognomonic sign is a linear or serpiginous erythematous or even papulovesicular lesion, slightly raised, which migrates upstream with an irregular movement and at a rate of 2-3mm/day [3]. This lesion most often appears in the first five days following the larval penetration of the skin.
Diagnosis is usually clinical based on history of recent travel to endemic areas in combination with a serpiginous and very itchy, raised rash. Laboratory tests are not necessary for diagnosis[2,3]. Eosinophilia is found in less than 40% of patients with CLM, but it is also not specific. Skin biopsy may reveal nematode larvae in a circular channel. In our patient the diagnosis was made solely on the basis of the pathognomonic clinical picture. Pharmacological management in local infection includes topical 10% thiabendazole solution 2-3 times daily for 5-10 days [4,5]. However, for multiple lesions or massive infestation, the treatment of choice being ivermectin, orally at a single dose of 200mg/kg [6], However, in countries that do not have ivermectin, such as Morocco, the prescription of repeated doses of albendazole constitutes a good therapeutic alternative. The recommended dose being 400mg/d for an average of three to seven days, with a good response in 92% to 100% of cases [4,5]. This was the case for our patient who showed an improvement in these symptoms within 48 hours following the administration of the first dose of albendazole (200mg/d).
In addition to pharmacological treatment, Prevention is just as simple and makes it possible to reduce the risk of infestation by cutaneous Larva migrans based on systematic washing of the hands after contact with the ground and before the meal and to avoid geophagy, eviction of dogs in public parks and avoid wearing socks in sandy areas, This was explained by the accumulation of sand at the level of the socks, which would contribute to prolonged contact with the parasite and therefore increase the chances of its penetration [4,5].
The case is reported because of the rarity of the disease and its occurrence in young men in the hands only.
CONCLUSION
Migran larva syndrome is a simple but rare and often poorly understood condition, clinical diagnosis is essential, but In our context, LMCAS can be subject to diagnostic wanderings.
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients gave their consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Peter B, Rosoľanka R, ŠimekováK, SzilágyiováM, MasnáJ. Imported skin parasitosis. Cas Lek Cesk. 2018;157:208-10.
2. Gill N, Somayaji R, Vaughan S. Exploring Tropical infections:a focus on cutaneous larva migrans. Adv Skin Wound Care. 2020;33:356-9.
3. Alexander KCL, Benjamin B, Kam LEH. Cutaneous larva migrans. Recent Pat Inflamm Allergy Drug Discov. 2017;11:2-11.
4. Jong-Yil C, Bong-Kwang J, Sung-Jong H. Albendazole and mebendazole as anti-parasitic and anti-cancer agents:an update. Korean J Parasitol. 2021;59:189-225.
5. Salissou L, Ousmane S, Doulla M, Brah S, Daou M, Ali D, et al. [Cutaneous Larva migrans:3 cases at the forehead]. Our Dermatol Online. 2017;8(Suppl. 1):36-9.
6. Vanhaecke C, Caumes E. Treatment of hookworm-related cutaneous larva migrans:albendazole or ivermectin?. Ann Dermatol Venereol. 2012;139:518-20.
Notes
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0002-3975-8316 http://orcid.org/0000-0002-3975-8316 http://orcid.org/0000-0002-5942-441X http://orcid.org/0000-0002-5942-441X http://orcid.org/0000-0003-3455-3810 http://orcid.org/0000-0003-3455-3810 |




Comments are closed.