Scrotal Kaposi’s sarcoma in an immunocompetent patient: A case report and review of the literature
Department of Dermatology; Taif University, Taif, Saudi Arabia
Corresponding author: Daifullah Al Aboud, MD
How to cite this article: Al Aboud D. Scrotal Kaposi’s sarcoma in an immunocompetent patient: A case report and review of the literature. Our Dermatol Online. 2022;13(e):e59.
Submission: 18.06.2022; Acceptance: 05.08.2022
DOI: 10.7241/ourd.2022e.59
Citation tools:
Copyright information
© Our Dermatology Online 2022. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
Kaposi’s sarcoma (KS) is a malignancy that generally affects the skin. It may be systemic with internal organ involvement, originating from the vascular endothelium. It is an acquired immunodeficiency syndrome (AIDS)-defining illness. Human herpes virus-8 (HHV-8) infection is involved in its pathogenesis. KS lesions have a general distribution, often involving the skin of the feet and legs and, to a lesser extent, the hands, arms, and trunk. Isolated scrotal involvement in an immunocompetent patient is a highly rare presentation. Herein, we present an immunocompetent Saudi patient with scrotal KS. A review of the related literature is also presented.
Key words: Angiokeratoma; Human Herpes Virus Type-8 (HHV-8); Kaposi’s Sarcoma; Scrotum
INTRODUCTION
Kaposi’s sarcoma (KS) is not an uncommon vascular tumor [1–11]. It was first described by Moritz Kaposi in 1872. It is caused by human herpes virus-8 (HHV-8) infection. Its cutaneous involvement is usually characterized by diffuse, vascular-looking macules, plaques, and nodules. It is mainly encountered in patients with HIV.
KS affects the skin in a diffuse pattern [1–11]. Isolated scrotal involvement in an immunocompetent patient is a rare presentation. Only a small number of reports on this presentation have been published. Herein, we present an additional case of this rare condition.
CASE REPORT
A 56-year-old Saudi male patient, not known to have a chronic medical problem before, presented with progressive, almost asymptomatic nodules on the scrotum present for more than one year. The patient reported occasional bleeding on shaving the scrotum. He was married and did not have sexual activities outside the marriage. He had no history of blood transfusion or a known risk factor of HIV infection.
A physical examination revealed multiple, skin-colored, red-to-violaceous nodules of various sizes on the scrotum (Fig. 1). There as no noticeable cutaneous lymphedema, no penile involvement, and no skin lesions elsewhere. The inguinal lymph nodes were not enlarged. Basic hematological and biochemical blood tests were all within normal ranges, and the patient was negative for HIV. A punch skin biopsy revealed the classical microscopic features of Kaposi’s sarcoma, which was also confirmed by CD34 and HH-8 immunohistochemical stains.
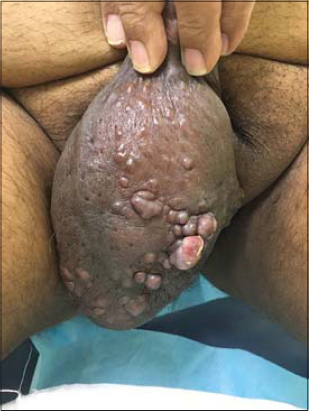 |
Figure 1: Multiple nodules of Kaposi’s sarcoma on the scrotum. |
The patient was referred to the urological and oncological department for further management.
DISCUSSION
Kaposi’s sarcoma (KS) is a vascular tumor [1–15]. The subtypes of KS include classic KS, African-type (endemic) KS, transplantation-associated KS, and HIV/AIDS-related KS [4].
The classical form is often seen in older male patients of Mediterranean or Ashkenazi descent, more commonly affecting the lower extremities and feet. It may rarely show visceral involvement [4,5].
Our case might have been a form of localized classic KS. Yet, it is difficult to be certain of the exact pathogenesis of localized KS. However, different precipitating factors and associations have been linked to localized KS. These include surgical wounds [13], trauma [14], and radiation [15].
The internal organ involvement may be asymptomatic. Asymptomatic stomach involvement has been estimated at 82% in classic KS. Therefore, studies have recommended screening patients with KS by endoscopy [4,5]. The value of this screening has not yet been studied in patients with localized KS, as in our case.
KS may be localized on the penis alone [11,12] and, much rarely, on the scrotum alone [4–10]. The first report of isolated scrotal KS was published in 1976 [7]. This was followed by several other reports. The case reported by Ozmen et al. [5] had a history of chemotherapy for lung cancer, which the authors suggested to be a possible precipitation factor in their case.
Our case highlight the importance of examining the scrotum as a potential site for involvment in cases with KS. It also highlights the importance of a skin biopsy in establishing the diagnosis of scrotal dermatoses. The morphological shape of the lesions in our case may have been mistaken for lymphangioma circumscriptum or angiokeratoma of Fordyce.
The treatment options for KS include, in general, total excision, chemotherapy, cryotherapy, laser ablation, electrocautery, radiotherapy, intralesional or systemic injection of cytotoxic agents, and alpha and beta interferon as an adjuvant therapy, photodynamic therapy, and photodynamic treatment with imiquimod or nitrogen mustard [4,5].
Despite the use of various methods for classical KS, there is no standard treatment procedure administered to cases with genital KS. Treatments for genital KS include local excision, circumcision, and radiotherapy, chemotherapy, and IFN-alpha treatment.
A good response with 5% topical imiquimod as a treatment for localized genital Kaposi’s sarcoma in an HIV-negative male was reported [11]. Vyas et al. performed total scrotectomy and bilateral orchiectomy in their report with scrotal KS [7].
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients gave their consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Mai S, Mansouri S, Outznit M, Znati K, Senouci K, Meziane M. Anaplastic transformation in a classic Kaposi’s sarcoma. Our Dermatol Online. 2020;11:329-30.
2. Agrawal SN, Rawal AA, Jane SD. Classic Kaposi’s sarcoma:A rare case with unusual presentation. Our Dermatol Online. 2014;5:68-70.
3. Chaouche M, Barbach Y, Dah Cherif A, Gallouj S, Mernissi FZ. Nodular bleeding lesion on the sole revealing a case of Kaposi’s sarcoma. Our Dermatol Online. 2019;10:e15.1-e15.2.
4. Yenice MG, Varnal?E, Şeker KG, Kavak A, Tu?cu V. Scrotal Kaposi’s sarcoma in HIV-negative patient:A case report and review of the literature. Turk J Urol. 2018;44:182-4.
5. Ozmen H, Baba D, Kacagan C, Kayikci A, Cam K. Case report:HIV-negative isolated scrotal Kaposi’s sarcoma. Int J Surg Case Rep. 2014;5:1086-7.
6. Turan H, Uslu E, Erdem H, Başar F. Kaposi sarcoma of scrotum:A case report. Abant Med J. 2013;2:254-5.
7. Vyas S, Manabe T, Herman JR, Newman HR. Kaposi’s sarcoma of scrotum. Urology. 1976;8:55-82.
8. Tela UM, Ibrahim AG, Abubakar AS, WaruGoni B, Musa AB, Waziri A. Localised primary Kaposi’s sarcoma of the scrotum:A rare presentation. IOSR-JDMS. 2014;13:83-5.
9. Serrano C, Sánchez G, del Mar Serrano M, Linares J, Dulanto C, Naranjo R. [Nodules and violaceous plaques on the scrotum and thigh]. Actas Dermosifiliogr. 2005;96:127-9.
10. Johnson DE, Chica J, Rodriquez LH, Luna M. Kaposi’s sarcoma presenting as scrotal ulcerations. Urology. 1977;9:686-8.
11. Fairley JL, Denham I, Yoganathan S, Read TRH. Topical imiquimod 5% as a treatment for localized genital Kaposi’s sarcoma in an HIV-negative man:A case report. Int J STD AIDS. 2012;23:907-8.
12. Soufiane M, Fadl TM, Nawfel M, Ouafae M, Kawtar Z, Afaf L, et al. Kaposi’s sarcoma:HIV-negative man with isolated penile localization. Indian J Pathol Microbiol. 2010;53:535-6.
13. Webster-Cyriaque J. Development of Kaposi’s sarcoma in a surgical wound. N Eng J Med. 2002;346:1207-10.
14. Rotoli M, Zamparelli F, Nardi M, Cerimele D. Post-traumatic localization of HIV-related Kaposi’s sarcoma:A case report. Tumori. 1989;75:12-3.
15. Cota C, Lora V, Facchetti F, Cerroni L. Localized post-radiation Kaposi sarcoma in a renal transplant immunosuppressed patient. Am J Dermatopathol. 2014;36:270-3.
Notes
Source of Support: Nil,
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
|




Comments are closed.