Complications of gel manicures
Katherine Woolridge 1, Deirdre Hooper2
1, Deirdre Hooper2
1School of Medicine, Louisiana State University Health Sciences Center, New Orleans, Louisiana, USA, 2Cofounder, Audubon Dermatology, Assistant Clinical Professor, LSU and Tulane Departments of Dermatology; School of Medicine, Louisiana State University Health Sciences Center Medical School, Dermatology Residency, New Orleans, Louisiana, USA
Corresponding author: Katherine Woolridge, BS
How to cite this article: Woolridge K, Hooper D. Complications of gel manicures. Our Dermatol Online. 2021;12(e):e75.
Submission: 02.06.2021; Acceptance: 16.08.2021
DOI: 10.7241/ourd.2021e.75
Citation tools:
Copyright information
© Our Dermatology Online 2021. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
Green nail syndrome is a nail disorder mostly seen in the elderly and those frequently exposed to water. Gel nail polish has become a very popular alternative to regular nail polish received during manicures. This popularity has allowed potential adverse effects to surface. We present a unique case of green nail syndrome in a healthy 50 year old healthy female after the removal of gel nail polish after a few weeks. The case raises awareness to potential complications and further consequences of gel manicures.
Key words: Gel Manicure; Green Nail Syndrome; Chloronychia; Nails
Introduction
Gel manicures have become widely popular in recent years. Unfortunately, with the growing popularity comes the unveiling of unwanted complications. Green nail syndrome, or chloronychia, results in greenish nail discoloration from a Pseudomonas infection [1]. Herein, we report a case of green nail syndrome in a healthy patient after removal of gel nail polish. While no bacterial culture was performed on this patient, the difficulty of noninvasively culturing a nail plate must be taken into consideration. Additionally, Geizhals et al found that dermoscopic and clinical evaluation along with green discoloration of multiple nails is sufficient for a Pseudomonas infection diagnosis [2].
CASE REPORT
A 50 year old healthy African American female presented with discoloration of her fingernails. The patient had noticed areas of green discoloration on multiple bilateral nails after removal of light brown gel nail polish several months prior. She had denied improvement or worsening of her fingernails since that time. Physical examination revealed onycholysis and green discoloration of her distal fingernails on the left third and fourth and right third and fifth phalanges (Figs. 1a – 1c). Dermatoscope evaluation allowed for magnified visualization of the brownish green discoloration as well as the light green fading border. The onychodystrophy was first investigated with a potassium hydroxide preparation test. Subsequent analyzation of the nail scrapings resulted negative for hyphae. Bacterial cultures were not sent, as noninvasive collection was impossible. The diagnosis of green nail syndrome by a Pseudomonas infection was made on the basis of Geizhals et al’s study results: findings of multiple green discolored nails, onycholysis, and faded borders seen via dermatoscope [2]. The patient’s green nails cleared after multiple soaks with equal parts vinegar and water.
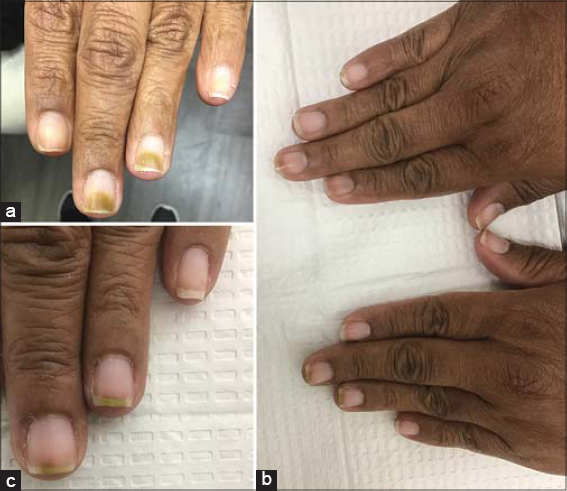 |
Figure 1: (a-c) Greenish discoloration of patient’s fingernails at two subsequent office visits. |
DISCUSSION
Green nail syndrome is usually seen in patients with constant or recurrent exposure to water. This is not surprising as the most common culprit, Pseudomonas aeruginosa, favors colonization of moist areas of the body when infected [1,3]. Additionally, previous nail trauma is a risk factor for the development of green nail syndrome. Subsequent onycholysis, or separation of the nail plate from the bed, allows for the entrance and growth of Pseudomonas under the nail, especially when hands are exposed to moist environments frequently [1]. Pseudomonas aeruginosa produces the green pigment pyocyanin that turns the nail bed a greenish hue [3]. Hence, the appropriate naming of this nail disorder.
While manicures with gel polish are marketed as longer lasting than regular nail polish, this benefit may jeopardize the health of the nail. The polish is tough on the nail as ultraviolet light is used to harden the gel to the nail to make a strong, long-lasting manicure. This can result in nails being left brittle and prone to onycholysis. Along with the potential trapping of moisture under the gel nail polish, the manicure can leave the nails prone to colonization of bacteria, particularly Pseudomonas. When the gel polish is removed, the forceful buffing, filing and soaking in acetone that is required is particularly damaging to the nail plate [4]. Without the protection of a healthy natural nail, the addition of new gel polish to these thin buffed nails allows for the opportunity of bacteria to get trapped and harbor within the nail bed. This colonization allows for the production of pyocyanin by the organism and the development of green nail syndrome.
Green nail syndrome as a result of nail art is very scarce in the literature. Hur et al reported a female who presented with light green/yellow discoloration of a single fingernail after removal of gel nail polish. The patient was diagnosed with green nail syndrome and a microbiology culture grew Pseudomonas oryzihabitans. This finding was surprising as the usual bug of green nail syndrome is P. aeruginosa [5].
In order to prevent unnecessary bacterial exposure to patients, in particular the immunosuppressed, physicians and all health care workers should recognize the potential susceptibility to nail infection and green nail syndrome when applying gel nail polish to their own fingernails [5]. Interestingly, Hewlett et al found that the number of bacterial organisms increased with time on nails painted with either regular nail polish or gel nail polish. Although gel polish was not found to increase the bacterial load more than regular polish, they reported that gel polish may hinder the effectiveness of alcohol hand sanitizer on decreasing bacteria [6]. The thickness and longer lasting qualities of the gel nail polish may allow for these detrimental findings. While green nail syndrome has a favorable outcome in the immunocompetent, Pseudomonas infections in the immunosuppressed are linked with a worse prognosis [7,8]. By raising awareness of complications of gel manicures, we hope to prevent unnecessary nail disorders in patients and allow for quick diagnosis and treatment by providers.
CONCLUSION
While complications of manicures may seem rare, the relatively new popularity of gel nail polish still allows time for problems to surface. The importance of prompt diagnosis and treatment of green nail syndrome prevents possible worsening or exposure to immunosuppressed contacts. Additionally, the sole knowledge of the potential complications may spark individuals to think twice before receiving such services.
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients gave their consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Chiriac A, Brzezinski P, Foia L, Marincu I. Chloronychia:Green nail syndrome caused by Pseudomonas aeruginosa in elderly persons. Clin Interv Aging. 2014;10:265-7.
2. Geizhals S, Lipner SR. retrospective case series on risk factors, diagnosis and treatment of pseudomonas aeruginosa nail infections. Am J Clin Dermatol. 2020;21:297-302.
3. Disorders of the nail apparatus |Fitzpatrick’s Color Atlas and Synopsis of Clinical Dermatology, 8e |AccessMedicine |McGraw-Hill Medical. Accessed November 22, 2020. https://accessmedicine-mhmedicalcom.ezproxy.lsuhsc.edu/content.aspx?bookid=2043&sectionid=154896484#1140788084
4. Nassim J, Liu K. A look at the effects of nail polish on nail health and safety. Published online 2019. https://www.health.harvard.edu/blog/a-look-at-the-effects-of-nail-polish-onnail-health-and-safety-2019112118231
5. Hur K, Cho S. Chloronychia caused by Pseudomonas oryzihabitans infection. JAAD Case Rep. 2020;6:918-20.
6. Hewlett AL, Hohenberger H, Murphy CN, Helget L, Hausmann H, Lyden E, et al. Evaluation of the bacterial burden of gel nails, standard nail polish, and natural nails on the hands of health care workers. Am J Infect Control. 2018;46:1356-9.
7. Wu DC, Chan WW, Metelitsa AI, Fiorillo L, Lin AN. Pseudomonas skin infection. Am J Clin Dermatol. 2011;12:157-69.
8. Dermatology:2-Volume Set – 3rd Edition. Accessed December 3, 2020. https://www.elsevier.com/books/dermatology-2-volume-set/bolognia/978-0-7234-3571-6
Notes
Source of Support: Nil,
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
|



Comments are closed.