Bourneville-Pringle disease: The misleading acne!
Meryem Khalidi , Omar Boudi, Naoufal Hjira, Mohammed Boui
, Omar Boudi, Naoufal Hjira, Mohammed Boui
Dermatology-Venerology Department, Mohammed V Military Hospital of Instruction, Rabat, Morroco
Corresponding author: Meryem Khalidi, MD
How to cite this article: Khalidi M, Boudi O, Hjira N, Boui M. Bourneville-Pringle disease: The misleading acne ! Our Dermatol Online. 2021;12(e):e39.
Submission: 28.01.2021; Acceptance: 08.02.2021
DOI:10.7241/ourd.2021e.39
Citation tools:
Copyright information
© Our Dermatology Online 2021. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
Sir,
Tuberous Sclerosis, also known as Bourneville’s disease, is an autosomal dominant syndrome with variable clinical expression.. We report a case of a 12-year-old female with tuberous sclerosis, treated for 2 years as moderate inflammatory acne by general practitioner.
It’s a young female patient of 12 years old from a consanguineous family, having a history of suspected epileptic seizures in childhood stopped at 5 years old with normal psychomotor development.
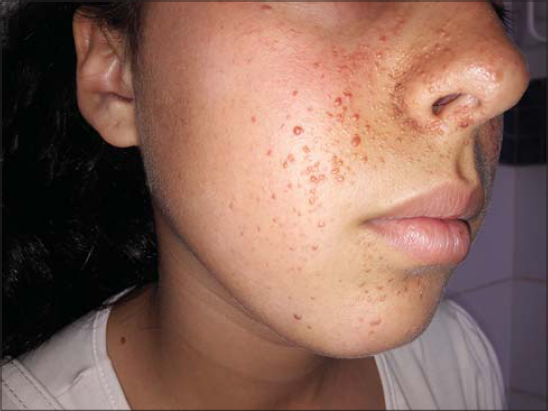
Physical examination revealed several small-scattered facial angiofibromas that were histologically determined by skin biopsy (Figs. 1 and 2). Hypomelanotic macules on her hands and back (Fig. 3), shagreen patches on her forehead and left inguinal area (Figs. 4 and 5). Periungual fibromas were seen in the fifth right toe (Fig. 6).
The MRI of brain showed multiple calcified sub ependymal nodules and cortical tubers. Neurological consult shows: normal status of conscience, without meningeal signs of irritation, cranial nerves without deficit, and no ataxia. Cardiological consult and ECG were normal. Multiple hamartomas or retinal achromic patches were noticed by ophthalmologic evaluation. Radiography of the chest was normal but truncal- abdominal CT had showed small size hepatic and renal angiomyolipoma. So with the above clinical findings, a diagnosis of Tuberous sclerosis was made, and the patient is under regular monitoring
Tuberous sclerosis is an autosomal dominant neurocutaneous syndrome with variable clinical expression.. It most often affects the skin and central nervous system [1]. Clinical presentations of tuberous sclerosis may range from clinically asymptomatic to a wide range of symptoms like seizures, chest pain, cough, flank pain, hematuria etc. Whenever a characteristic feature of tuberous sclerosis like facial angiofiromas, hypomelanotic macules, brain tubers, renal angiomyolipoma etc… is encountered, a thorough evaluation of other organ systems should be made. Besides ultrasound of the abdomen and CT and MRI of the brain, abdomen, as well as CT of the thorax, and other investigations include CT angiography, echocardiography etc…. must be done [2]. For confirmation of the findings and for genetic counseling, molecular tests may be used [3]. The Treatment of Tuberous sclerosis consists in addressing the symptoms caused by hamartomas and in prophylactic measures to prevent loss of function of the affected organ [4]. Since it is a systemic disease, a multidisciplinary approach is mandatory [5].
STB is a fairly common disease but it’s often underdiagnosed , with variable clinical expression dominated by neuropsychic and renal involvement. Therapeutic management must be multidisciplinary [6].
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients gave their consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Brzezinski P. Tuberous sclerosis (Bourneville’a-Pringle disease), skin lesions –case report. Dermatol Prakt. 2011;2:53-8.
2. Agrawal SN, Kulkarni YA, Deshmukh YR, Jane SD. Tuberous Sclerosis in Pregnancy. Our Dermatol Online. 2014;5:160-2.
3. Rasso A, Oukarf S, Sow A, Elloudi S, Baybay H, Farih MH, Mernissi FZ. Tuberous sclerosis complex and psoriasis:A possible common pathophysiology. Our Dermatol Online. 2020;11:406-8.
4. Khalid Al Aboud, Daifullah Al Aboud:Eponyms in the dermatolopathology literature linked to the neural tissues. Our Dermatol Online. 2013;4:395-8.
5. Bachaspatimayum R, Das P, Bhattacharjee N. Dyschromatosis universalis hereditaria:A rare case report from Northeast India. Our Dermatol Online. 2019;10:179-80.
6. Wataya-Kaneda M, Tanaka M, Hamasaki T, Katayama I. Trends in the prevalence of tuberous sclerosis complex manifestations:an epidemiological study of 166 Japanese patients. PLoS One. 2013;8:e63910.
Notes
Source of Support: Nil,
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
|








Comments are closed.