Nevus comedonicus
Siham Belmourida , Mariame Meziane, Laila Benzekri, Nadia Ismaili, Karima Senouci
, Mariame Meziane, Laila Benzekri, Nadia Ismaili, Karima Senouci
Department of Dermatology-Venereology, Mohammed V University, IBN Sina Hospital, Rabat, Morocco
Corresponding author: Siham Belmourida, MD
Submission: 07.11.2020 Acceptance: 14.02.2021
DOI: 10.7241/ ourd.2021e.24
Cite this article: Belmourida S, Meziane M, Benzekri L, Ismaili N, Senouci K. Nevus comedonicus. Our Dermatol Online. 2021;12(e):e24.
Citation tools:
Copyright information
© Our Dermatology Online 2021. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
Nevus comedonicus is a rare disease and diagnosis is made chiefly on clinical grounds confirmed by histology [1].
We report the case of a young patient with Nevus comedonicus in the back.
A 22-year-old youngster, consulted for a cribriform closet evolving since childhood in the back, gradually increasing in size, not itching. Clinical examination noted the presence of an irregular patch measuring 7 cm long, slightly pigmented, made up of the juxtaposition of multiple dilated follicular ostia without papulo-pustules, abscesses or inflammatory signs opposite (Fig. 1). The remainder of the clinical examination did not reveal any abnormality. Skin biopsy showed an acanthosis epidermis invaginated at one point, forming a cystic mass hanging from the epidermis and filled with keratin, this lesion was connected in depth to atrophic hair follicles allowing the diagnosis of Nevus comedonicus. Paraclinical examinations did not show any abnormalities. The diagnosis of isolated Nevus comedonicus was retained and therapeutic abstention with regular clinical monitoring was proposed.
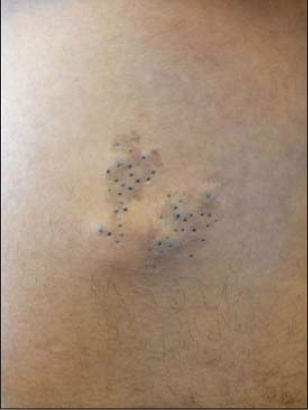 |
Figure 1: Nevus comedonicus: The juxtaposition of multiple dilated follicular ostia without papulo-pustules. |
Nevus comedonicus belongs to the group of epidermal hamartomas. It’s one of the rarest forms of cutaneous nevus. In contrast to atrophoderma vermiculatum, the interfollicular skin is typically normal in the nevus comedonicus syndrome [2]. Since the number of cases reported is relatively low in the literature and several such cases should be existing in communities, reporting of these would enhance the quantum of reported cases that would in turn naturally enable us to elucidate the full spectrum of the disease [3]. A therapeutic abstention may be indicated except in the event of complications or for aesthetic purposes. A local treatment can be proposed based on keratolytics, topical corticosteroids and oral retinoids, but the effectiveness of these various therapies is variable. Surgical treatment is sometimes indicated [4].
Nevus comedonicus is a clinical entity should be known by dermatologist.
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients gave their consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Tchernev G, Ananiev J, Semkova K, Dourmishev L, Schonlebe J, Wollina E. Nevus comedonicus:an updated review. Dermatol Ther (Heidelb) 2013;3:33–40.
2. Jeong HS, Lee HK, Lee SH, Kim HS, Yi SY. Multiple large cysts arising from nevus comedonicus. Arch Plast Surg 2012;39:63–6.
3. Awal G, Kaur T. Multidermatomal Nevus Comedonicus:How Dermoscopy aids diagnosis?. Our Dermatol Online. 2018;9:164-6.
4. Mehrolhasani N. Nevus comedonicus. Our Dermatol Online. 2014;5:300.
Notes
Source of Support: Nil,
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0002-2795-9161 http://orcid.org/0000-0002-2795-9161 |



Comments are closed.