Profuse sebaceous hyperplasia of the face induced by ciclosporin in a young man
Siham Boularbah , Zakia Douhi, Sabrina Oujidi, Mariam Soughi, Sara Elloudi, Hanane Baybay, Fatima Zahra Mernissi
, Zakia Douhi, Sabrina Oujidi, Mariam Soughi, Sara Elloudi, Hanane Baybay, Fatima Zahra Mernissi
Department of Dermatology, CHU Hassan II, Fez, Morocco
Citation tools:
Copyright information
© Our Dermatology Online 2023. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
Sebaceous hyperplasia is a benign skin condition, presenting as disseminated umbilical yellowish-pink papules, usually on the face. Histologically, each lesion consists of a large multilobed sebaceous gland whose acini confluence in a central collector that corresponds to the clinical umbilication The condition may occur sporadically as a result of chronological aging and photoaging, in a familial form or as a manifestation of Muir-Torre syndrome. Also, more and more cases of eruptive multiple sebaceous hyperplasia secondary to cyclosporine have been described of which we describe an exceptional case.
Key words: Ciclosporin; Sebaceous hyperplasia; Acitretin
INTRODUCTION
Cyclosporine became a reference treatment for transplant patients from the beginning of the 1980s. In the blood, cyclosporine is 90% bound with proteins and is found in plasma in a proportion of 33-47%. Its main side effects are kidney failure and high blood pressure. Many skin complications have also been described. Some, such as the occurrence of carcinomas, are a non-specific consequence of immunosuppression. They are observed with other immunosuppressive drugs such as azathioprine [1]. Other complications, such as damage to the pilosebaceous follicle, seem on the contrary to be specific to ciclosporin. The most frequently reported damage to the pilosebaceous follicle are hypertrichosis, keratosis pilaris, acne and folliculitis [2]. Cyclosporine can more rarely cause profuse sebaceous hyperplasia.
CASE REPORT
A 33-year-old man, with a personal or family history of skin, monitored for a rheumatological problem, was put on ciclosporin. Consulted for a non-pruritic papular eruption that had been developing for 6 weeks.
Dermatological examination found yellow or flesh-colored papules, two to five millimeters in diameter, umbilical, sometimes centered by a comedo (Fig. 1a). There were no inflammatory lesions, in particular no pustules. The papules converged on almost the entire surface of the cheeks, forehead, e. Three diagnostic hypotheses were suggested: molluscum contagiosum, multiple adnexal tumors of the face and profuse sebaceous hyperplasia.
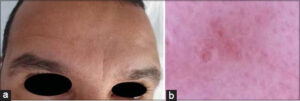 |
Figure 1: (a) Clinical image of Papular eruption of the face occurring during treatment with ciclosporin. (b) Dermoscopic image: Central yellowish aspect and vascularization in crown. |
Dermoscopic examination showed an aggregation of yellowish-white clumps with linear vessels in a crown (Fig. 1b). Dermoscopic examination confirmed the diagnosis of sebaceous hyperplasia.
The patient was treated with isotretinoin at a dose of 20 mg per day. This dose was then reduced to 10 mg per day due to an increase in cholesterolaemia to 2.6 g/l. but the patient was lost sight of.
DISCUSSION
Sebaceous hyperplasia (SH) is a benign proliferation of the sebaceous glands, which in most cases is idiopathic and affects middle-aged men. SH results from intrinsic aging and extrinsic aging. In addition, this condition can occur in the context of genetic diseases such as Muir-Torre syndrome or familial HS. Some data reported in the literature suggest that ciclosporin could also be a causal factor. The mechanism of action of ciclosporin linked to the accumulation of the highly lipophilic molecule in the sebaceous gland [1]. Ciclosporin is a 5-alpha reductase inducer. It stimulates sebaceous secretion, which probably contributes to damage to the pilosebaceous follicle [2].
The classic manifestations of GHS are flesh-colored or whitish-yellow papules, normally umbilical, ranging in size from 2 to 9 mm [3]. Diagnosis is usually based on clinical features. Dermoscopy is a non-invasive diagnostic tool that allows the visualization of many yellowish-white lobulated structures on a pale yellow or yellowish-red background, corresponding to the sebaceous lobules and the umbilication at the center of the lesion, corresponds to a dilated follicular infundibulum, and the crown or the linear-irregular vessels, correspond to the dilated vessels [3].
Treatment modalities include photodynamic therapy with aminolevulinate methyl, topical dichloroacetic acid, cryotherapy, electrodesiccation, Pulsed dye laser or carbon dioxide laser and also Isotretinoin by inhibition of sebaceous secretion [4].
CONCLUSION
HS is a skin lesion that should be added to the possible rare but specific pilosebaceous changes occurring during cyclosporin treatment. Our case is exceptional because of the extension and rapid development of the lesions. Moreover, these lesions are essentially described in renal transplant recipients. To our knowledge, this is only the first case of disseminated HS observed after treatment for a rheumatological problem and not after bone marrow transplantation.
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients gave their consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Brzezinski P, Chiriac A. Sebaceous hyperplasia in neonates and adults. Our Dermatol Online. 2015;6:107-8.
2. Emiliano G, Silvia PG, Vano-Galván S, Jaén-Olasolo P. [Multiple sebaceous hyperplasia secondary to ciclosporin in a heart transplant patient]. Imag Seman. 2013;261:98-107.
3. Zaouak A, Hammami H, Fenniche S. Dermoscopy as an adjuvant tool for the diagnosis of sebaceous hyperplasia. Our Dermatol Online. 2020;11:e113.1-e113.2.
4. McDonald SK, Goh MS, Chong AH. Successful treatment of cyclosporine-induced sebaceous hyperplasia with oral isotretinoin in two renal transplant recipient. Australas J Dermatol. 2011;52:227 .
Notes
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0002-3975-8316 http://orcid.org/0000-0002-3975-8316 http://orcid.org/0000-0002-5942-441X http://orcid.org/0000-0002-5942-441X http://orcid.org/0000-0003-3455-3810 http://orcid.org/0000-0003-3455-3810 |




Comments are closed.