Subungual osteochondroma
Imane Couissi , Zakia Douhi, Noura Kalmi, Meryem Soughi, Sara El Loudi, Hanane BayBay, Fatima Zahra Mernissi
, Zakia Douhi, Noura Kalmi, Meryem Soughi, Sara El Loudi, Hanane BayBay, Fatima Zahra Mernissi
Department of Dermatology, University Hospital Hassan II Fès, Morocco
How to cite this article: Couissi I, Douhi Z, Kalmi N, Soughi M, El Loudi S, BayBay H, Mernissi FZ. Subungual osteochondroma. Our Dermatol Online. 2023;14(e):e49.
Submission: 31.10.2022; Acceptance: 10.05.2023
DOI: 10.7241/ourd.2023e.49
Citation tools:
Copyright information
© Our Dermatology Online 2023. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
Osteochondroma is a common benign skeletal neoplasm, represents 20% to 50% of benign bone tumors, and is solitary 90% of the time [1]. The subungual form is rare and located specially on the toes. It is frequently observed more in adolescents and young adults, with a male-to-female ratio of 2:1.
Clinically, it is well defined, firm, and often painful exophytic tumor that develops progressively over months, and its growth may produce nail deformation and pain. It may detach the overlying nail to expose an exophytic tumor with an ulcerative surface that can be infected [2].
The tumor is loosely attached to bone rarely maybe soft-tissue tumors with bony attachment. They are prone to recur, but the malignant transformation is unlikely.
Radiologically, the appearance is classic of a blending of the soft-tissue tumor with the bony cortex with the cap of hyaline cartilage showing irregular calcification.
Histologically, the tumor consists of proliferating hyaline cartilage like that of a normal growing epiphysis [2].
Complete operative excision is the treatment of choice for subungual osteochondromas [2,3]. Complete removal with subsequent curettage of the base is preferred because incomplete excision has been reported to be responsible for almost 50% of recurrences [2].
We report a 62-year-old woman with a histologically confirmed subungual osteochondroma of the left third toe that has been evolving for 4 months, causing electric discharge pain.
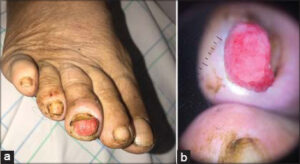
Clinical examination found an erythematous ulcerating nodule well limited under the nail on the left 3rd toe, overflowing at the free edge of the nail, measuring 1.5 cm causing distal onycholysis (Fig. 1a). Dermoscopy showed erythematous background with irregular linear vessels (Fig. 1b). The patient underwent total surgical removal of the tumor without recurrence.
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
REFERENCES
1. Pacifici M. The pathogenic roles of heparan sulfate deficiency in hereditary multiple exostoses. Matrix Biol. 2018;71-72:28-39.
2. Aiba H, Yamada S, Yamamoto N, Hayashi K, Miwa S, Tsuchiya H, et al. Spontaneous shrinkage of solitary osteochondromas. Skeletal Radiol. 2018;47:61-8.
3. Heyworth PB, Rashid M. Regression of a solitary osteochondroma of the distal humerus in toddler following trauma. Radiol Case Rep. 2019;14:187-9.
Notes
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0009-0005-2261-6919 http://orcid.org/0009-0005-2261-6919 http://orcid.org/0000-0002-5942-441X http://orcid.org/0000-0002-5942-441X http://orcid.org/0000-0003-3455-3810 http://orcid.org/0000-0003-3455-3810 |




Comments are closed.