Prurigo pigmentosa and diabetes: A case report
Fatima Azzahra El Gaitibi , Sanae Sialiti, Asmae Abdelmoutalib, Soumaya Hamich, Mariame Meziane, Laila Benzekri, Nadia Ismaili, Karima Senouci
, Sanae Sialiti, Asmae Abdelmoutalib, Soumaya Hamich, Mariame Meziane, Laila Benzekri, Nadia Ismaili, Karima Senouci
Department of Dermatology, Mohammed V University in Rabat, Ibn Sina University Hospital, Rabat, Morocco
Corresponding author: Fatima Azzahra El Gaitibi, MD
Submission: 27.01.2021; Acceptance: 16.04.2021
DOI: 10.7241/ourd.20223.28
Cite this article: El Gaitibi FZ, Sialiti S, Abdelmoutalib A, Hamich S, Meziane M, Benzekri L, Ismaili N, Senouci K. Prurigo pigmentosa and diabetes: A case report. Our Dermatol Online. 2022;13(3):332-333.
Citation tools:
Copyright information
© Our Dermatology Online 2022. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
Sir,
Prurigo pigmentosa is a rare inflammatory disease first reported in 1971 by Nagashima et al. as a “peculiar pruriginous dermatosis with gross reticular pigmentation” in Japan [1], where the largest number of such cases have been described, with only several cases having been described elsewhere. Herein, we report a new case of prurigo pigmentosa.
A 32-year-old Moroccan female presented at our dermatology department with a several-week-old history of pruritic eruptions on the chest, abdomen, lumbosacral area, and neck. According to the patient, the onset was marked by itchy papules coalescing to plaques, secondarily becoming hyperpigmented reticulated macules. The patient was treated with antifungal drugs without improvement. Additionally, the patient had recently been diagnosed with type II diabetes and was treated by oral antidiabetics.
A physical examination revealed hyperpigmented macules arranged in a reticulate pattern, mainly on the chest, abdomen, lumbosacral area, and neck (Figs. 1 and 2). She had no acanthosis nigricans or other associated symptoms. The main diagnoses considered were pityriasis versicolor, confluent and reticulated papillomatosis of Gougerot–Carteaud, and prurigo pigmentosa. A histological examination revealed a discreetly atrophic epidermis surmounted by compact orthokeratotic hyperkeratosis and slight basal pigmentation. The dermis was the site of perivascular mononuclear infiltrates associated with a small number of melanophages. Periodic acid–Schiff staining was negative. This was consistent with the diagnosis of prurigo pigmentosa.
 |
Figure 1: Hyperpigmented macules arranged in a reticulate pattern on the chest and the abdomen. |
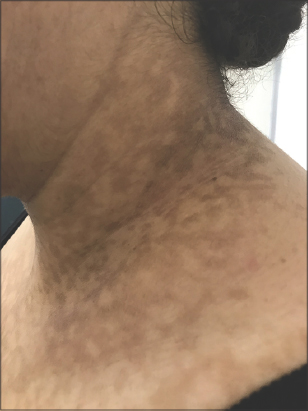 |
Figure 2: Hyperpigmented macules arranged in a reticulate pattern on the neck. |
After stabilizing the patient’s diabetes, the eruption disappeared spontaneously, leaving only faded pigmentation.
Prurigo pigmentosa occurs more often in females in the third decade of life [2]. It is characterized by erythematous itchy plaques or papules organized in a transient reticulate pattern, later with post-inflammatory hyperpigmentation that persists for several months. It commonly appears symmetrically on the chest, lumbosacral area, and neck.
Histologically, we noticed a superficial and perivascular mononuclear infiltrate with papillary dermal edema and spongiosis. In the advanced stage of the disease, lymphocytic dermal infiltrate is found along with upper dermal melanophages. Besides, the epidermis is the site of focal parakeratosis and sometimes necrotic keratinocytes [2].
The etiology is unknown. Several reported cases were associated with fasting, dieting, and diabetes. These suggest the probable contribution of ketosis to the pathogenesis [3]. Indeed, prurigo pigmentosa occurs more often in individuals with insulin-dependent diabetes, which progresses more easily to ketoacidosis than in those with non-insulin-dependent diabetes [4]. Glycemic control with the disappearance of ketonuria may therefore be sufficient to resolve prurigo pigmentosa. In some cases, however, treatment with cyclins or dapsone is necessary.
In the present case, the adaptation of an antidiabetic treatment and glycemic control resolved the rash.
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients gave their consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Nagashima M, Ohshiro A, Shimizu N. [A peculiar pruriginous dermatosis with gross reticular pigmentation]. Jap J Dermatol. 1971;81:78-91.
2. Almaani N, Al-Tarawneh AH, Msallam H. Prurigo Pigmentosa:A Clinicopathological report of three middle eastern patients. Case Rep Dermatol Med. 2018;2018:9406797.
3. Alshaya MA, Turkmani MG, Alissa AM. Prurigo pigmentosa following ketogenic diet and bariatric surgery:A growing association. JAAD Case Rep. 2019;5:504-7.
4. Ohnishi T, Kisa H, Ogata E, Watanabe S. Prurigo pigmentosa associated with diabetic ketoacidosis. Acta Derm Venereol. 2000;80:447-8.
Notes
Source of Support: Nil,
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0002-0313-6152 http://orcid.org/0000-0002-0313-6152 |



Comments are closed.