Acral purpura and pityriasis rosea-like eruption following COVID-19 infection
Eleni Klimi 1, Dionysia Vasdeki2
1, Dionysia Vasdeki2
1Department of Dermatology Thriassio General Hospital Magula Athens Greece, 2Department of Plastic Surgery Thriassio General Hospital Magula Athens Greece
Corresponding author: Eleni Klimi, MD
Submission: 31.01.2022; Acceptance: 09.03.2022
DOI: 10.7241/ourd.20223.24
Cite this article: Klimi E, Vasdeki D. Acral purpura and pityriasis rosea-like eruption following COVID-19 infection. Our Dermatol Online. 2022;13(3):324-325
Citation tools:
Copyright information
© Our Dermatology Online 2022. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
Sir,
A 74-year-old female patient treated with angiotensin-converting enzyme inhibitor for arterial hypertension with metformin and atorvastatin for insulin-independent diabetes mellitus and hyperlipidemia, respectively, consulted the outpatient dermatological clinic for a rash that appeared fifteen days prior to consultation. The patient received the second dose of mRNA COVID-19 vaccine on July 29, 2021, and was due to receive the third dose on December 29, yet she fell ill on day 6 of the same month, probably being infected by one of her grandchildren. The eruption consisted of erythematous, purpuric macules on the anterior face of both tibia (Fig. 1a), of a solitary papule on the left hand (Fig. 1b), and of erythematous papules with a scale on the border on the left buttock (Fig. 1c). A collarette formed on the trailing edge of the advancing border of the hand lesion, a clinical sign pathognomonic of pityriasis rosea. Intense pruritus accompanied the eruption. No herald patch was observed, nor lesions on the trunk, being the typical location of lesions of pityriasis rosea, while lesions on the hands are absent in the typical cases of the disease. The oral and genital mucosae were intact. The cutaneous manifestations of COVID-19 include purpuric, chilblain, vesicular, urticarial, and pityriasis rosea-like lesions. Acral lesions are the most frequent location of the cutaneous manifestations associated with COVID-19 infection [1]. An acral distribution of lesions is a feature of mouth, hand, and foot disease due to infection with Coxsackie A16 virus [2], although no reactivation of this virus has been detected during the COVID-19 pandemic, while the reactivation of herpes 6 and herpes 7 virus associated with pityriasis rosea has occurred [3].
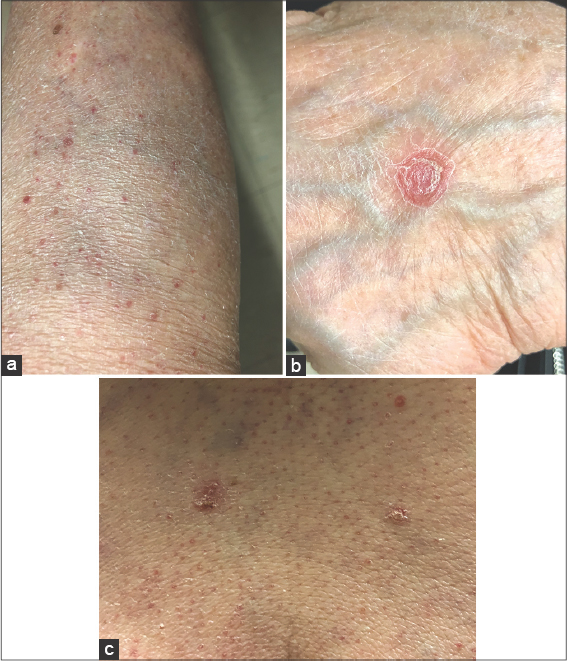 |
Figure 1: (a) Erythematous lesions on the right tibia. (b) Pityriasis rosea-like lesion on the left hand. (c) Erythematous papules on the left buttock with a peripheral scale. |
Erythema multiforme, a disorder associated with herpes infection, has likewise a typical acral distribution of the lesions and is described to be associated with COVID-19 infection during the pandemic [4,5]. The patient presented purpuric and pityriasis rosea-like lesions. Steroids, emollients and oral antihistamines were prescribed to relieve the itch. The lesions showed no significant improvement since their appearance two months earlier. This fact and the atypical morphology of the eruption led to the proposal of a biopsy, which the patient refused. A full blood count and urea, creatinine, and liver tests were within normal.
This case is being reported to increase awareness of the cutaneous manifestations of COVID-19 infection with mixed clinical signs, which, although benign in their course, may produce considerable discomfort.
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients gave their consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. de Masson A, Bouaziz JD, Sulimovic L, Cassius C, Jachiet M, Ionescu MA, et al;SNDV (French National Union of Dermatologists-Venereologists). Chilblains is a common cutaneous finding during the COVID-19 pandemic:A retrospective nationwide study from France. J Am Acad Dermatol. 2020;83:667-70.
2. Saguil A, Kane SF, Lauters R, Mercado MG. Hand-foot-and-mouth disease:Rapid evidence review. Am Fam Physician. 2019;100:408-14.
3. Drago F, Ciccarese G, Rebora A, Parodi A. Human herpesvirus-6, -7, and Epstein-Barr virus reactivation in pityriasis rosea during COVID-19. J Med Virol. 2021;93:1850-1.
4. Trayes KP, Love G, Studdiford JS. Erythema multiforme:Recognition and management. Am Fam Physician. 2019;100:82-8.
5. Gül Ü. COVID-19 and dermatology. Turk J Med Sci. 2020;50:1751-9.
Notes
Source of Support: Nil,
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0001-5113-5640 http://orcid.org/0000-0001-5113-5640 |



Comments are closed.