Kawasaki-like disease in children with COVID-19
Hasna Kerrouch , Meryem Khalidi, Rachid Frikh, Naoufal Hjira, Mohammed Boui
, Meryem Khalidi, Rachid Frikh, Naoufal Hjira, Mohammed Boui
Dermatology Venerology Department, Military Hospital Instruction Mohammed, University Mohammed V, Rabat, Morocco
Corresponding author: Hasna Kerrouch, MD
How to cite this article: Kerrouch H, Khalidi M, Frikh R, Hjira N, Boui M. Kawasaki-like disease in children with COVID-19. Our Dermatol Online. 2022;13(2):225-226.
Submission: 02.11.2021; Acceptance: 03.02.2022
DOI: 10.7241/ourd.20222.30
Citation tools:
Copyright information
© Our Dermatology Online 2022. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
Sir,
In late 2019, a new type of viral infection emerged in Wuhan, China, known as severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), which causes coronavirus disease 2019 (COVID-19) and which has become the most challenging pandemic of this century.
COVID-19 has affected individuals of all ages worldwide. Epidemiological data from numerous countries show that children are a small minority of those who test positive.
Most children with COVID-19 show mild symptoms or are asymptomatic, yet new concerns have emerged, with reports on hyperinflammatory states or Kawasaki-like disease [1,2].
Kawasaki disease (KD) is a systemic vasculitis of unknown etiology that occurs mainly in children and rarely in adults [3].
Herein, we report a child with Kawasaki-like disease associated with COVID-19.
A fifteen-year-old boy presented to our department with a four-day history of high fever, vomiting, diarrhea, abdomen pain, and erythematous rash. His previous medical history was unremarkable. A physical examination revealed diffuse, erythematous, maculopapular rash, bilateral conjunctivitis, erosive hyperemia of the oral mucosa, scrotal erythema, and a deepithelialized tongue (Figs. 1 and 2).
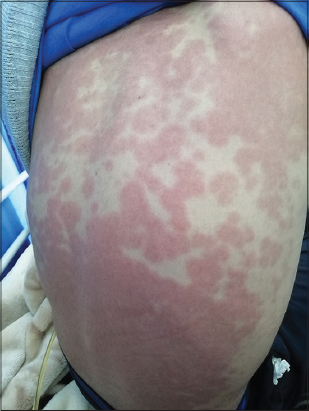 |
Figure 1: Diffuse, erythematous, maculopapular rash. |
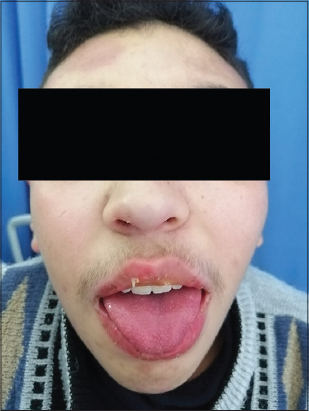 |
Figure 2: Erosive hyperemia of the oral mucosa. |
Laboratory tests showed liver transaminases, lymphopenia, thrombocytopenia, hypoalbuminemia, and significantly increased ferritin and other inflammatory markers. A chest X-ray and ECG were normal. A nasopharyngeal swab for SARS-CoV-2 was negative. Broad-spectrum empiric antibiotics were administered.
In the meanwhile, the patient developed cardiac involvement: hypotension, tachycardia, tachypnea with oxygen desaturation, abnormal troponin T, high levels of D-dimer, and reduced systolic function on echocardiography. Treatment was switched to IG IV 2 g/kg and intravenous corticosteroid 2 mg/kg. Improvements in clinical condition, laboratory, and imaging results was noticed.
We measured anti-S-specific IgG antibodies to SARS-CoV-2 and found that the patient had high positive titers of IgG antibodies against SARS-CoV-2.
Kawasaki disease (KD) is a rare, acute pediatric vasculitis, with coronary artery aneurysms as its main complication.
Infectious triggers have been suggested in the etiology of KD due to an epidemic pattern and marked seasonality [4].
The diagnosis requires at least five days of fever and the occurrence of at least four of the five following principle clinical features [5]:
- Extremity changes with erythema and edema of the palms and soles during the acute phase. Skin peeling may be present in the convalescent phase.
- Diffuse polymorphic rash, including diffuse, maculopapular erythroderma or erythema multiforme-like.
- Bilateral nonexudative bulbar conjunctivitis, typically sparing the limbus.
- Oral mucosal changes with cracked lips, oral and pharyngeal erythema, and the “strawberry tongue” (erythema of the tongue with prominent fungiform papillae).
- Cervical lymphadenopathy, typically unilateral, at least 1.5 cm in diameter.
Recently, several cases of Kawasaki-like disease have been reported in various locations that coincide with the SARS-CoV-2 pandemic, producing concerns about the association of COVID-19 with KD.
COVID-19, caused by SARS-CoV-2, is a viral disease characterized by the inflammation and infection of endothelial cells.
The presence of viral elements and inflammatory cells within endothelial cells and the evidence of endothelial cell death suggests that SARS-CoV-2 infection facilitates endotheliitis through direct viral involvement and an inflammatory response [6].
We present our patient with KD-like disease associated with SARS-CoV-2 infection. To date, there has been no clear answer to the inquiries concerning Kawasaki-like disease in children with COVID-19. Therefore, we await further studies to explain its clinical course and pathophysiology.
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients gave their consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Choi S-H, Kim HW, Kang J-M, Kim DH, Cho EY. Epidemiology and clinical features of coronavirus disease 2019 in children. Clin Exp Pediatr. 2020;63:125.
2. Dong Y, Mo X, Hu Y, Qi X, Jiang F, Jiang Z, et al. Epidemiological characteristics of 2143 pediatric patients with 2019 coronavirus disease in China. J Emerg Med. 2020;58:712-3.
3. Burns JC, Glode MP. Kawasaki syndrome. Lancet. 2004;364:533-44.
4. KombatéK, Teclessou JN, Douti NK, Saka B, Akakpo AS, Mouhari-TouréA, et al. [Kawasaki disease:First observation in a togolese child 3 years old]. Our Dermatol Online. 2016;7:459-64.
5. McCrindle BW, Rowley AH, Newburger JW, Burns JC, Bolger AF, Gewitz M, et al. Diagnosis, treatment, and long-term management of Kawasaki disease:A scientific statement for health professionals from the American Heart Association. Circulation. 2017;135:e927-99.
6. Varga Z, Flammer AJ, Steiger P, Haberecker M, Andermatt R, Zinkernagel AS, et al. Endothelial cell infection and endotheliitis in COVID-19. Lancet. 2020;95:1417-8.
Notes
Source of Support: Nil,
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0002-2127-3863 http://orcid.org/0000-0002-2127-3863 |



Comments are closed.