Becker’s nevus syndrome: A new case series
Piotr Brzezinski 1,2, Anca Chiriac3, César Bimbi4, Lorenzo Martini5, Katarzyna Borowska6
1,2, Anca Chiriac3, César Bimbi4, Lorenzo Martini5, Katarzyna Borowska6
1Institute of Biology and Environmental Protection, Pomeranian Academy, ul. Arciszewskiego 22A, 76-200 Slupsk, Poland; 2Department of Dermatology, Provincial Specialist Hospital in Slupsk, Ustka, Poland; 3Department of Dermato-Physiology, Apollonia University Iasi, Strada Muzicii nr 2, Iasi-700399, Romania; 4Institute of Dermatology Centro Historico, Dermatology, Porto Alegre, Brazil; 5Department of Pharmaceutical Biotechnologies, University of Siena, Via A. Moro 2, 53100 Siena, Italy; 6Department of Histology and Embryology with Experimental Cytology Unit, Medical University of Lublin, Lublin, Poland
Corresponding author: Piotr Brzezinski, MD PhD
How to cite this article: Brzezinski P, Chiriac A, Bimbi C, Martini L, Borowska K. Becker’s nevus syndrome: A new case series. Our Dermatol Online. 2022;13(2):193-196.
Submission: 02.12.2021; Acceptance: 09.02.2022
DOI: 10.7241/ourd.20222.19
Citation tools:
Copyright information
© Our Dermatology Online 2022. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
Becker’s nevus syndrome (BNS) is a rare epidermal nevus syndrome characterized by Becker’s nevi and other, often unobtrusive, systemic symptoms and/or skin lesions, often ipsilateral. A Becker’s nevus (BN) is a hamartoma that is unilateral, hyperpigmented, and often hairy. Systemic symptoms typically involve breast gland hypoplasia and skeletal and muscular disorders. Herein, we describe three rare cases of Becker’s nevus syndrome. In the first case, the BN coexisted with ipsilateral breast gland hypoplasia; in the second case, the BN coexisted on both sides with breast gland hypoplasia and keratosis pilaris only in the left antecubital region and with scoliosis; in the third case, we found two Becker’s nevi in the left and right hip area associated with hypoplasia of the third canine tooth on the right side and with scoliosis. Our three cases were sporadic and all occurred in males. Coexisting symptoms of BN were found accidentally. We describe two new coexisting symptoms: atypical keratosis pilaris and hypoplasia of the canine teeth.
Key words: Becker’s nevus; Becker’s nevus syndrome; Ipsilateral Breast Hypoplasia; Hamartoma; Epidermal Nevus
INTRODUCTION
Becker’s nevus syndrome (BNS) is a rare epidermal nevus syndrome characterized by the presence of Becker’s nevi (BN) and other systemic and/or skin symptoms [1].
A Becker’s nevus (BN) is an epidermal cutaneous hamartoma characterized by hypertrichosis and hyperpigmentation. The nevus usually consists of a circumscribed, unilateral, irregularly shaped, hyperpigmented macule, commonly occurring around the anterior upper trunk, with or without hypertrichosis and/or acneiform lesions.
The association of a Becker’s nevus with developmental abnormalities such as breast gland hypoplasia, musculoskeletal defects, scoliosis, vertebral defects, pectus excavatum, hypoplasia of the sternocleidomastoid muscle, bilateral ureteral stenosis, soft tissue hypertrophy, fused carpal bones, pigmented epithelioid melanocytoma, café-au-lait spots has been described [2]. However, Danarti et al. described more unknown symptoms belonging to the clinical spectrum of BNS [3].
The etiopathogenesis of BNS is unclear, yet androgens may play a role in the clinical manifestations of BNS [4]. BNS involves the incomplete penetrance of autosomal dominant inheritance.
Herein, we present three cases of Becker’s nevus syndrome with the coexistence of ipsilateral breast gland hypoplasia, keratosis pilaris, and hypoplasia of the third canine tooth.
CASE REPORTS
Case 1
A sixteen-year-old male was initially referred to the doctor because of acne. Accidentally, a lesion on the right shoulder joint was found. It was brown, with a hairy surface, and was associated with hypoplasia of the ipsilateral breast. The lesion appeared spontaneously at 2–4 years of age, The patient had undergone no treatment. Detailed clinical and radiological examinations, including an X-ray of the spine, detected no other abnormalities. The Becker’s nevus was recognized on a clinical basis.
Case 2
A twelve-year-old male presented with a brown lesion on the anterior aspect of the chest (Fig. 1). The brown patch had a black, hairy surface and coexisted on both sides of the breast gland, more pronounced on the left side. Atypical keratosis pilaris located only in the left antecubital region was also found. All skin lesions appeared at 2–3 years of age. An X-ray of the spinal column confirmed the presence of scoliosis.
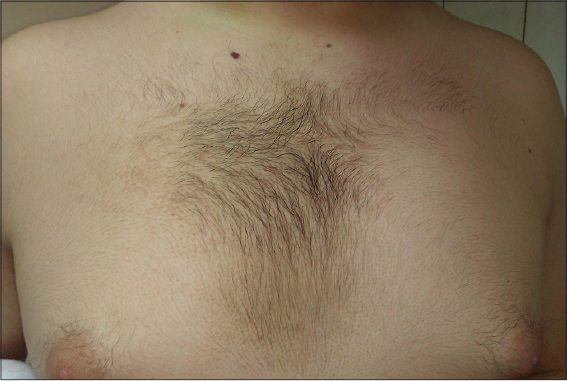 |
Figure 1: Hypertrichotic and hyperpigmented skin lesions on the anterior aspect of the chest and both sides of the breast gland hypoplastic with more severity on the left side (case 2). |
Case 3
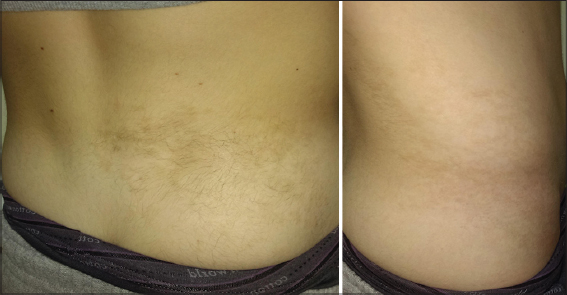
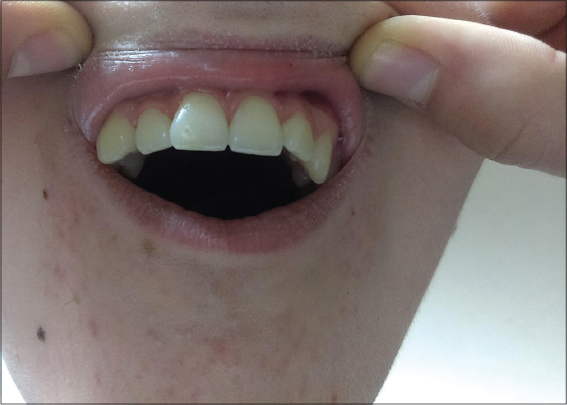
A fifteen-year-old male drew our attention due to the presence of two pigmented hairy areas present since early childhood, which had extended over time: one from the right lumbar area to the right side of the abdominal wall, another located along the left hip. Long, dark, asymmetric hair was spread throughout the light brown pigmented plaques. The pigmentation of the right hip area was less dark—only slightly brown—and with less asymmetric hair. (Figs. 2a and 2b). A histopathological examination of a biopsy taken from the brown patch revealed acanthosis, papillomatosis, increased melanin deposition in the basal layer, and hyperplasia of the erector pili muscle, confirming the suspicion of a Becker’s nevus. Complete blood count and routine liver and kidney tests were all within normal limits. An X-ray of the entire spine evidenced scoliosis while a dental examination revealed hypoplasia of the right canine tooth (Fig. 3).
Our patients were diagnosed with Becker’s nevus syndrome. Other skin areas and mucosal surfaces were unaffected. No family members or past histories had shown similar skin diseases. All patients reported that, in adolescence, the lesions spread with a concomitant increase in body hair in that region.
DISCUSSION
The Becker’s nevus (BN) was first described by Samuel Becker in 1949, yet it was in 1995 that the term BNS was first introduced by Happle, who found an association of BN with unilateral breast hypoplasia and muscle, skin, and/or skeletal abnormalities in 23 patients [5]. The exact etiology of the Becker’s nevus remains unknown. According to Torrelo et al., the genetic mechanism of BNS is a postzygotic, autosomal, lethal mutation that survives in a mosaic form [6]. Usually, BN lesions appear in childhood yet become evident after puberty. A hypothesis that the BN is an androgen-dependent nevus was suggested, as seen by a higher incidence in males, pubertal development, hypertrichosis, an association with intralesional acne, and an anomalous scrotum [1,7]. An increase in androgen receptors in the involved skin was also noted. Breast hypoplasia may be explained by the counterbalance effect of androgens that decrease the estrogenic action.
BNS affects males and females in equal proportion, yet some publications report a male-to-female ratio of 2 to 1 [2,7]. Others claim that it is more easily diagnosed in females due to the more visible breast hypoplasia [4].
The literature has described no more than seventy cases of BNS [4,5]. Following the observation of our cases, we believe that cases of BN/BNS may often be relatively subtle and pass undetected, and that, therefore, the syndrome could more common. The evolution of the BN is benign, the pigmentation rarely regresses, and the hair growth follows the onset of pigmentation.
A majority of publications have described BNS as a coexistence of BN and scoliosis or unilateral breast hypoplasia. We present, herein, a rare clinical presentation of BNS [3].
BNS may sometimes remain unnoticed since it usually proceeds with non-specific clinical findings [8]. All coexisting symptoms in our patients were found accidentally (scoliosis, atypical keratosis pilaris, and hypoplasia of the canine tooth).
Zawar et al. presented an interesting case of a BN coexisting with ipsilateral acanthosis nigricans (AN) [7]. The authors presented the case for the extreme rarity of a distinct morphological presentation of two different pigmentary disorders in the same patient.
Cuesta et al. reported the first case of a concurrent congenital acral BN and Kabuki-makeup syndrome [9]. The term Kabuki-makeup syndrome was coined after the peculiar facial features reminiscent of Japanese Kabuki theater masks.
We describe, herein, an exceedingly rare case of unilateral double Becker’s naevus. There have only been several documented cases with multiple and bilaterally symmetrical Becker’s nevi [6].
The treatment of BNS is difficult and may include surgical excision, Q-switched ruby laser (694 nm), Er: YAG laser, or pharmacotherapy with antiandrogen drugs, including spironolactone. At a dose of 50 mg/day, the improvement of breast hypoplasia has been reported. A satisfactory response with a significant reduction of hyperpigmentation was reported with topical flutamide. Nonsteroidal, antiandrogen, hypoplastic breast augmentation with autologous fat grafting appears promising and may be a safe treatment option with minimal side effects [10].
CONCLUSION
We report three rare cases, all males, in whom the coexisting symptoms of a BN were found accidentally. Described were new coexisting symptoms: atypical keratosis pilaris, hypoplasia of the canine tooth, and a rare unilateral asymmetrical double Becker’s nevus. Becker’s nevus syndrome involves extremely subtle clinical findings and, thus, many cases may remain undetected.
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients gave their consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Elharrouni AA, Douhi Z, Mrabat S, Baybay H, Elloudi S, Mernissi FZ. Atypical location of Becker’s nevus:About two cases. Clinical and dermoscopic features. Our Dermatol Online. 2020;11:e.1-3.
2. Sciallis GF, Sciallis AP. Becker nevus with an underlying desmoid tumor:A case report and review including Mayo Clinic’s experience. Arch Dermatol. 2010;146:1408-12.
3. Danarti R, König A, Salhi A, Bittar M, Happle R. Becker’s nevus syndrome revisited. J Am Acad Dermatol. 2004;51:965-9.
4. Cosendey FE, Martinez NS, Bernhard GA, Dias MF, Azulay DR. Becker nevus syndrome. An Bras Dermatol. 2010;85:379-84.
5. Milano A. Becker’s nevus with hypoplasia of the areola and nipple. Eur J Pediat Dermatol. 2016;26:188.
6. Mehta P, Kumar R, Jain SK, Rai NN. Unilateral asymmetrical double Becker’s naevus. Indian J Dermatol Venereol Leprol. 2014;80:470-1.
7. Zawar V, Goyal T, Kamra S. Becker’s nevus and ipsilateral acanthosis nigricans. Our Dermatol Online. 2014;5:388-90.
8. Torrelo A, Baselga E, Nagore E, Zambrano A, Happle R. Delineation of the various shapes and patterns of nevi. Eur J Dermatol. 2005;15:439-50.
9. Cuesta L, Betlloch I, Toledo F, Latorre N, Monteagudo AF. Kabuki syndrome:A new case associated with Becker nevus. Dermatol Online J. 2011;17:1.
10. Ho Quoc C, Fakiha M, Meruta A, Dlimi C, Piat JM, Delay E. Breast lipofilling:A new treatment of Becker nevus syndrome. Ann Chir Plast Esthet. 2015;60:336-9.5.
Notes
Source of Support: Nil,
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0001-6817-606X http://orcid.org/0000-0001-6817-606X http://orcid.org/0000-0002-0989-4931 http://orcid.org/0000-0002-0989-4931 http://orcid.org/000-0002-6396-7767 http://orcid.org/000-0002-6396-7767 http://orcid.org/0000-0003-0964-6169 http://orcid.org/0000-0003-0964-6169 |



Comments are closed.