Superficial epidermolytic ichthyosis: A rare disorder with the unusual absence of blistering
1Department of Dermatology, Venereology and Leprosy, Dr Rajendra Prasad Government Medical College Tanda at Kangra HP, India, 2Department of Dermatology, Venereology and Leprosy Indira Gandhi Medical College Shimla HP, India
Corresponding author: Prajul Mehta, MD
How to cite this article: Rana A, Mehta P. Superficial epidermolytic ichthyosis: A rare disorder with the unusual absence of blistering. Our Dermatol Online. 2022;13(1):89-91.
Submission: 02.02.2021; Acceptance: 06.05.2021
DOI:10.7241/ourd.20221.22
Citation tools:
Copyright information
© Our Dermatology Online 2022. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
Superficial epidermolytic ichthyosis (SEI), formerly known as ichthyosis bullosa of Siemens (IBS), is an extremely rare keratinization disorder with superficial peeling, with an estimated prevalence of 1:500,000, caused by a variety of mutations in the keratin 2E gene. The clinical features include hyperkeratosis and blistering, but these are milder than in epidermolytic hyperkeratosis. The treatment is symptomatic and involves keratolytics and emollients. Herein, we report a case of SEI with the unusual absence of spontaneous blistering.
Key words: Superficial epidermolytic ichthyosis; Keratin; Blistering
INTRODUCTION
Epidermolytic hyperkeratosis was originally described histologically by Nikolski in 1987 [1]. Although it is an autosomal dominant disorder, 50% of cases may be sporadic due to spontaneous mutations [2]. Ichthyosis bullosa of Siemens (IBS) is a milder variant of this condition, which is now designated as superficial epidermolytic ichthyosis (SEI). It is distinguished clinically from epidermolytic hyperkeratosis by the absence of erythroderma, the localization of dark grey hyperkeratosis in the flexures, and areas of peeling skin, known as the “Mauserung phenomenon” [3]. While it bears a number of similarities to bullous congenital ichthyosiform erythroderma, the clinical features are much milder and it is caused by a mutation in the gene encoding keratin 2E [4]. Herein, we report an extremely rare case of IBS without any history of spontaneous blistering.
CASE REPORT
A full-term five-month-old boy, born of a non-consanguineous marriage, presented with generalized thickening of the skin persistent since the age of four months. This was followed by peeling skin without any underlying erythema, and subsequent clearance. The patient was born with normal, non-erythematous, and non-scaly skin with no history of a restrictive membrane at birth. There was no history suggestive of erythroderma or palmoplantar hyperhidrosis and no preceding history of blistering. Additionally, there were no familiar similar cases. An examination revealed scaling on the trunk and extremities, with the scales accentuated in the flexural creases. The flexures showed visible hyperkeratosis with a typical rippled pattern and there was peeling of normal skin on the trunk without any erythema (“Mauserung” phenomenon) (Figs. 1 and 2).
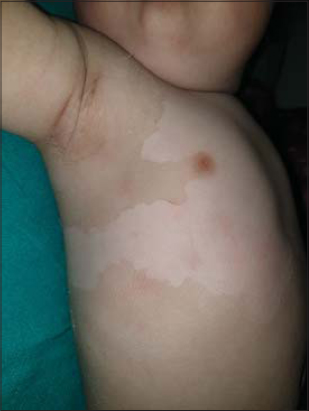 |
Figure 1: Peeling skin and hyperkeratosis accentuated in the flexural areas. |
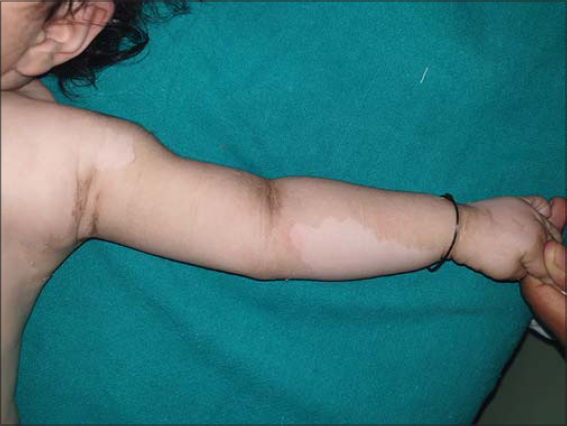 |
Figure 2: Peeling of the hyperkeratotic skin with underlying normal skin without any erythema (“Mauserung” phenomenon). |
A biopsy could not be performed as the parents did not give consent to do so. Owing to the patient’s low socioeconomic status and the lack of facilities at our institute, genetic studies could not be performed.
On the basis of the clinical picture, a provisional diagnosis of ichthyosis bullosa of Siemens was made. The patient was prescribed white soft paraffin and light liquid paraffin to be applied on the body liberally at least twice daily.
DISCUSSION
Superficial epidermolytic ichthyosis (SEI) is a rare condition (1 in 500,000), less common than epidermolytic hyperkeratosis (1 in 250,000) [5]. The mode of inheritance in most of the reported cases is autosomal-dominant, although sporadic cases have been reported [3,6].
SEI is milder than epidermolytic hyperkeratosis, often with no abnormalities at birth. Blistering in response to trauma develops in infancy. Hyperkeratosis with dark brown skin, but little true scales, develops mainly in the flexural areas of the extremities. Superficial peeling of the skin (“Mauserung” phenomenon) is typical [7]. Histopathologically, epidermolysis is confined to the granular and upper spinous layer of the epidermis in SEI, in contrast to congenital bulbous ichthyosiform erythroderma, in which it involves the deeper suprabasal layer as well [8].
Koley et al. presented a case with no history or clinical evidence of blistering at the time of presentation, as in our case; the occurrence of a similar disease in the generation prior to the generation affected was not observed [5]. It may be presumed that, in this case, the disease appeared as a result of a sporadic mutation. Rajiv et al. described a fourteen-year-old boy whose blistering improved with age but the problem of peeling skin worsened [9].
Although the diagnosis may be confirmed only by molecular genetic testing, a clinical examination helps to differentiate bullous ichthyosiform erythroderma from SEI [10]. The typical pathological findings are compact hyperkeratosis, pronounced vacuolar degeneration in the upper stratum spinosum and stratum granulosum, filament clumping, and a thickened granular layer with irregularly shaped keratohyaline and acantholysis [1]. Unfortunately, there is no permanent solution for this condition. A topical emollient is the last resort, with 0.05% tazarotene gel showing a satisfactory result in a recent report [9].
CONCLUSION
Superficial epidermolytic ichthyosis is a rare disorder, and the absence of blistering is extremely rare, as reported in the present case.
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients gave their consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Lacz NL, Schwartz RA, Kihiczak G. Epidermolytic hyperkeratosis:A keratin 1 or 10 mutational event. Int J Dermatol. 2005;44:1-6.
2. Shimomura Y, Sato N, Tomiyama K, Takahashi A, Ito M. A sporadic case of epidermolytic hyperkeratosis caused by a novel point mutation in the keratin 1 gene. Clin Exp Dermatol. 2006;31:286-7.
3. Das A, Das A, Bhattacharya S, Ghosh A, Shome K. Superficial epidermolytic ichthyosis. Indian J Dermatol Venereol Leprol 2015;81:656.
4. Cervantes T, Pham C, Browning JC. Superficial epidermolytic ichthyosis:A report of two families. Pediatr Dermatol. 2013;30:469-72.
5. Koley S, Salodkar A, Gupta S, Bhanke A, Ujawane A, Shazia B. Ichthyosis bullosa of Siemens sans history of blistering:An interesting case report. J Pakistan Assoc Dermatol 2009;19:171-4.
6. Akiyama M, Tsuji-Abe Y, Yanagihara M, Nakajima K, Kodama H, Yaosaka M, et al. Ichthyosis bullosa of Siemens:its correct diagnosis facilitated by molecular genetic testing. Br J Dermatol. 2005;152:1353-6.
7. Whittock NV, Ashton GH, Griffiths WA, Eady RA, McGrath JA. New mutations in keratin 1 that cause bullous congenital ichthyosiform erythroderma and keratin 2e that cause ichthyosis bullosa of Siemens. Br J Dermatol. 2001;145:330-5.
8. Sarkar P, Saha A, Malakar S. Ichthyosis bullosa of Siemens sans blistering with extracutaneous features:A subtype or association?Indian J Paediatr Dermatol. 2015;16:188-90.
9. Rajiv S, Rakhesh SV. Ichthyosis bullosa of Siemens:Response to topical tazarotene. Indian J Dermatol Venereol Leprol. 2006;72:43-6.
10. Ang-Tiu CU, Nicolas ME. Ichthyosis bullosa of Siemens. J Dermatol Case Rep. 2012;6:78-81.
Notes
Source of Support: Nil,
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
|




Comments are closed.