Favre–Racouchot disease: A clinico-dermoscopic profile
Shagufta Rather , Sumaya Zeerak, Manzoor Bhat
, Sumaya Zeerak, Manzoor Bhat
Department of Dermatology, Government Medical College, Srinagar, University of Kashmir, Jammu and Kashmir, India
Corresponding author: Shagufta Rather, MD
How to cite this article: Rather S, Zeerak S, Bhat M. Favre–Racouchot disease: A clinico-dermoscopic profile. Our Dermatol Online. 2021;12(4):448-451.
Submission: 09.01.2021; Acceptance: 31.03.2021
DOI: 10.7241/ourd.20214.24
Citation tools:
Copyright information
© Our Dermatology Online 2021. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
Favre–Racouchot disease (FRD) is clinically characterized by the presence of open comedones, small papules, and cystic lesions with deep wrinkles and furrows on sun-exposed areas, especially the face. FRD is a purely cosmetic disorder, with most patients not requesting treatment. Dermoscopy may play a vital role in diagnosing early lesions of FRD, averting the need for an invasive procedure such as a skin biopsy, and helping to differentiate it from close mimics. The dermoscopic features of FRD have not been reported in the literature before. We report a clinicoepidemiological profile and dermoscopic findings in patients presenting with features suggestive of FRD.
Key words: Favre–Racouchot disease; dermoscopy; yellowish background; circular homogenous areas; keratin plugs
INTRODUCTION
Favre–Racouchot disease (FRD), originally described in 1932 by French dermatologist Maurice Favre and reviewed in detail by Favre and Racouchot in 1951, is also known as senile comedones, solar comedones, and nodular elastosis with cysts and comedones [1]. FRD is clinically characterized by the presence of large, open comedones, small papules, and cystic lesions with deep wrinkles and furrows on an underlying area of actinic damage. It usually develops in the periocular region and on the nose. However, the lateral neck, retroauricular areas, earlobes, and forearms may sometimes become involved [2,3]. Diagnosis is mainly clinical since most of the patients are often reluctant to undergo an invasive procedure such as skin biopsy and because of the benign and asymptomatic nature of the disease and, often, the lack of concern at an advanced age. Dermoscopy may improve the accuracy of diagnosis in an older age, helping to distinguish it from close mimics. Herein, we present a clinicoepidemiological profile and dermoscopic findings in a series of five patients with clinical features suggestive of FRD.
CASE SERIES
Five consecutive patients presenting to our outpatient department with features suggestive of FRD were enrolled and subjected to history taking and clinical examination. The criteria for diagnosing FRD included the presence of large, open, black comedones, symmetrically distributed in the temporal and periorbital areas, a diffuse yellowish hue of the skin, and the presence of deep wrinkles and furrows on a background of actinically damaged and atrophic skin. Only three of the five patients were subjected to a dermoscopic examination with a hand-held dermoscope (3Gen DermLite DL4, 10×). No case underwent histopathological confirmation.
As for the clinicodemographic profile of the patients (Table 1), the mean age on diagnosis was 66.4 years. All were chronic cigarette smokers with pack-years ranging from 25 to 30. The only female patient was a chronic hookah smoker. All were farmers by occupation with a history of significant daily sun exposure and had never followed any specific sun protection measures or applied sunscreen.
 |
Table 1: Patient characteristics of FRD |
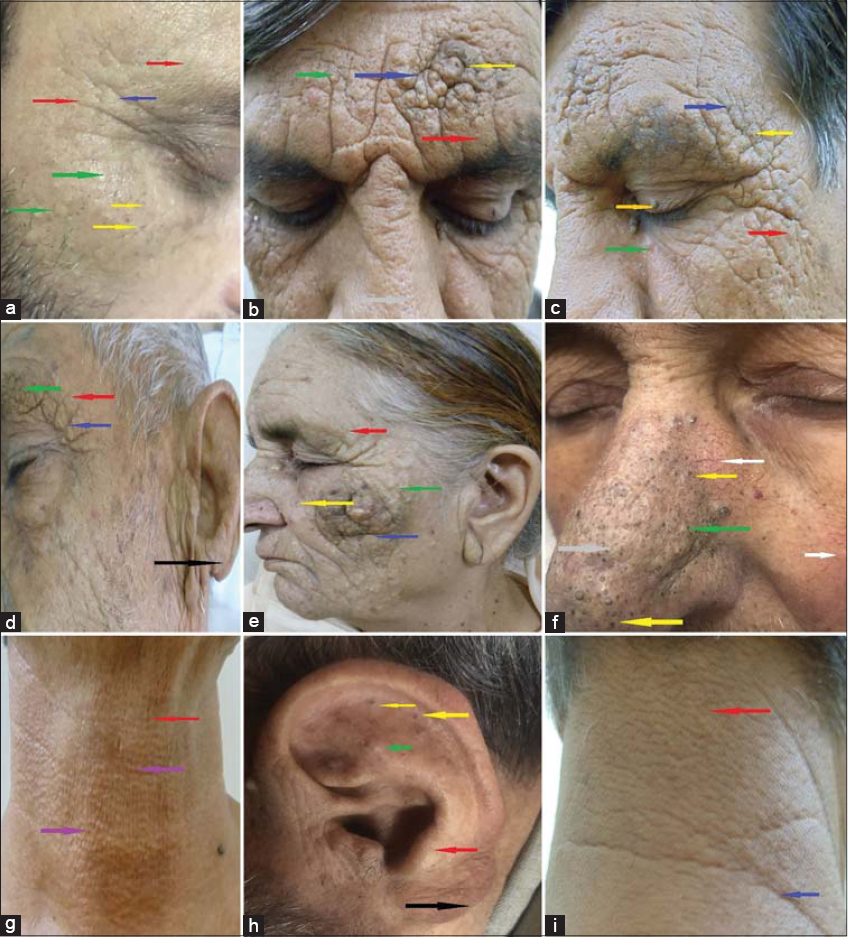
On clinical examination, all cases exhibited a classical triad of multiple, large, open—with few closed—comedones and numerous 0.5–6 mm yellow-to-brown papules and nodules clustered around the temporal and periocular region in a symmetrical fashion, deep wrinkles and furrows involving predominantly the forehead and the zygomatic and malar areas, and a background of actinically damaged and atrophic skin with a diffuse yellowish hue. The surrounding skin had a thickened, soft, and waxy appearance. Similar lesions were observed on the dorsum of the patulous nose in three patients. Accompanying cutis rhomboidalis nuchae was seen in two patients. One patient bore an actinic comedonal plaque, considered a variant of FRS, presenting as a skin-colored, lobular plaque with comedones and yellow cysts localized in the right malar region. Other areas involved were the lateral sides of the neck (two cases), the retroauricular areas (two cases), and the earlobes (three cases). Cases with severe disease had a peculiar facial appearance with coarsening of facial features. Lateral madarosis of both eyebrows was present in three cases (Figs. 1a – 1i).
DERMOSCOPIC FINDINGS
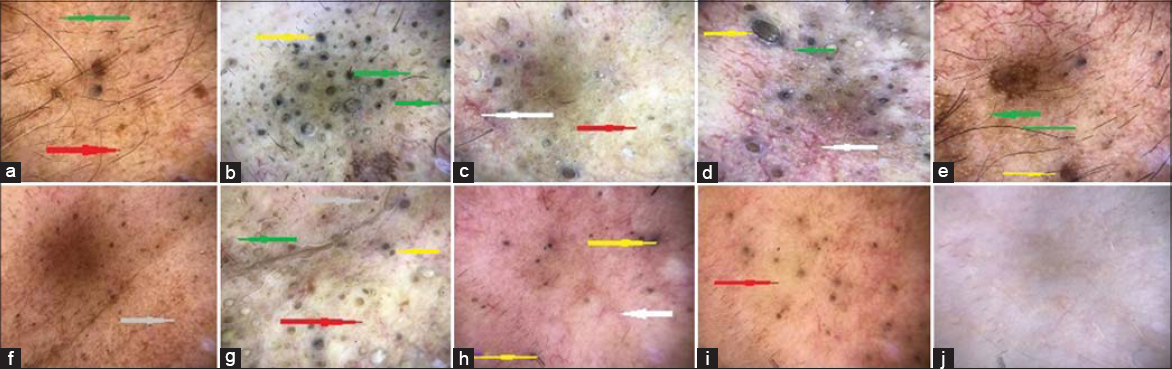
The following dermoscopic findings were noted (Figs. 2a – 2j):
- Numerous circular homogenous areas in shades of light-to-dark brown, sometimes black, depending on the openness of comedones, with remarkable keratin plugs, situated superficially (all cases);
- Multiple, large, black, barrel-shaped rings surrounding hair follicles against a creamy white to yellowish background (open comedones);
- Multiple, small, well-defined, structureless, yellowish-brown homogenous circular areas surrounding keratin plugs (closed comedones);
- Intervening, apparently normal skin showing an atypically yellowish hue, corresponding to solar elastosis of the skin, linear arborizing vessels, numerous small comedones, and pigmentary changes, together representing chronic actinic damage of the skin, seen mainly on the forehead, cheeks, and nose, and in the periorbital areas;
- Linear arborizing vessels corresponding to telangiectasias (three cases);
- Enlarged facial skin pores and embedded blackheads correlating with well-defined dilated pilosebaceous openings visible on dermoscopy (five cases).
DISCUSSION
Six percent of the population in the 54-to-76-year-old age group are said to be affected by FRD. [2,3]. The mean age of 66.4 years, the age of onset, the male predominance, and the typical clinical presentation observed bore resemblance to other studies. The exact pathogenesis of FRS remains unexplained. A number of risk factors, such as chronic UV exposure, cigarette smoking, and therapeutic radiation, have been suggested to play a role [4]. All our patients proved to be heavy smokers of 25–30 pack-years with significant UV exposure. This was mainly linked with occupational exposure as nearly all were farmers by occupation and had other sorts of outdoor jobs as laborers. Clinical evidence of actinic epidermal damage or solar elastosis was present in all cases.
Although a biopsy-proven diagnosis for a majority of cases of FRD has been described in the literature [3,4], histopathology was not performed in our study as most of the patients came to us with other cutaneous complaints and it was a coincidental diagnosis, with the patients showing no concern for it.
The associated cutaneous disorders in our patients were basal cell carcinoma in one, eyelid papilloma in one, and actinic keratosis in two. Cutaneous myxoma, actinic keratosis, basal and squamous cell carcinoma, trichostasis spinulosa, keratoacanthoma, and eyelid papilloma have been reported in patients with FRD [5].
The dermoscopic features of FRD have not been reported in the literature before. Only one report, describing the dermoscopic finding of an inflammatory lobular plaque on the cheek in a case of FRD, has been published [6].
FRD needs to be differentiated from acne comedones, milia, colloid milium, syringomas, trichoepitheliomas, and sebaceous hyperplasia. Comedones are very similar to those of acne vulgaris but without perilesional inflammation or associated inflammatory lesions. A central white structure and a surrounding brown ring are the typical findings in milia; a whitish structure surrounded by an erythematous halo is seen in trichoepithelioma; glittering yellowish white globules are a feature of syringoma; and multiple dull, yellowish-white globules with surrounding vessels are seen in sebaceous hyperplasia. Sebaceous nevi show bright, yellow dots not associated with hair follicles [7,8].
No standard treatment protocols have been devised so far. Preventive measures include the avoidance of sun exposure, the use of broad-spectrum sunscreen, and the discontinuation of smoking. Topical retinoids, alone or as part of combined strategies, have been described as the mainstay of treatment. The use of superpulsed CO2 laser followed by the extraction of cystic and comedonal material, dermabrasion, curettage, and chemical peels have been used with mixed cosmetic results [4].
CONCLUSION
FRD is a purely cosmetic disorder, with most patients not asking for treatment. Dermoscopy may play a vital role in:
- An accurate diagnosis if dealing with early lesions specifically;
- Determining whether a biopsy is needed or not in light of clinical observations;
- Averting the need for an invasive procedure such as a skin biopsy and helping to differentiate it from close mimics.
To the best of our knowledge, no Indian literature exists on the dermoscopic appearance of FRD and ours is the first from this part of the globe.
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients gave their consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Favre M, Racouchot J. [Nodular cutaneous elasteidosis with cysts and comedones]. Ann Dermatol Syphiligr (Paris) 1951;78:681-702.
2. Raveendra L. A clinical study of geriatric dermatoses. Our Dermatol Online. 2014;5:235-9.
3. Mahajan VK, Chauhan PS, Mehta KS, Sharma V. Favre-Racouchot syndrome. Our Dermatol Online. 2013;4:328-9.
4. Paganelli A, Mandel VD, Kaleci S, Pellacani G, Rossi E. Favre-Racouchot disease:Systematic review and possible therapeutic strategies. J Eur Acad Dermatol Venereol. 2019;33:32-41.
5. Zhang R, Zhu W. Favre-Racouchot syndrome associated with eyelid papilloma:A case report. J Biomed Res. 2012;26:474-7.
6. Chessa MA, Filippi F, Ferrara F, Patrizi A, Baraldi C. A case of unilateral inflamed plaques with comedones of the face. Dermatol Pract Concept. 2018;8:292-4.
7. Alfaro-Castellón P, Mejía-Rodríguez SA, Valencia-Herrera A, Ramírez S, Mena-Cedillos C. Dermoscopy distinction of eruptive vellus hair cysts with molluscum contagiosum and acne lesions. Pediatr Dermatol. 2012;29:772-3.
8. Nayak SS, Mehta HH, Gajjar PC, Nimbark VN. Dermoscopy of general dermatological conditions in Indian population:A descriptive study. Clin Dermatol Rev 2017;1:41–51.
Notes
Source of Support: Nil,
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0002-0980-6014 http://orcid.org/0000-0002-0980-6014 |



Comments are closed.