Pathomimia among children provoked by deodorant spray: 2 new cases
Ibtissam Benslimane Kamal 1, Fatima-Ezzahra El Fetoiki1, Fouzia Hali1, Ghizlane Benjelloun2, Soumiya Chiheb1
1, Fatima-Ezzahra El Fetoiki1, Fouzia Hali1, Ghizlane Benjelloun2, Soumiya Chiheb1
1Department of Dermatology-Venereology, UHC Ibn Rochd, Casablanca, Morocco, 2Department of Child Psychiatry, UHC Abderrahim EL Harouchi, Casablanca, Morocco
Corresponding author: Dr. Ibtissam Benslimane Kamal
How to cite this article: Benslimane Kamal I, El Fetoiki F-E, Hali F, Benjelloun G, Chiheb S. Pathomimia among children provoked by deodorant spray: 2 new cases. Our Dermatol Online. 2021;12(3):273-276.
Submission: 14.07.2020; Acceptance: 11.10.2020
DOI: 10.7241/ourd.20213.9
Citation tools:
Copyright information
© Our Dermatology Online 2021. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
Pathomimia is defined as a fictitious disease caused consciously by the patient themself and for which they deny responsibility. We report two new cases of children with atypical clinical pathomimia. Two girls of 11 and 14 years of age with no particular medical history, but with family conflicts, presented a similar clinical appearance: painful erythemato-bullous lesions on the left upper limb and the abdomen. Lesions appeared one after another leaving rounded hypochromic scars. All lesions were in accessible areas. The results of the questionnaires answered by the mothers show that the two girls had been using spray deodorant frequently. The diagnosis of pathomimia by cold burn due to misuse of deodorant spray was suspected. A dermatological and child psychiatry support was set up. There have been few cases of pathomimia by cold burn caused by misuse of deodorant spray. It, therefore, seems necessary to report these cases.
Key words: Pathomimia; Pathomimia among children; Cold burn; Misuse of deodorant spray
INTRODUCTION
Factitious disorders are reported in approximately 1% of patients seen in psychiatry [1]. Pathomimia is a type of fictitious disorder caused consciously by the patient themself and for which they deny all responsibility [2]. Pathomimia is rare among children. We report two new cases of children with atypical clinical pathomimia caused by deodorant spray.
CASE REPORT
Case 1: A 11-year-old female with no history of illness, including psychiatric diseases, consulted for erythematous bullous lesions of the flexion face of the left upper limb, which appeared one after another from the distal area of the forearm to the shoulder over a period of 4 days. A dermatological examination found lesions in a layered arrangement along the limb resulting in crusty lesions, then rounded and linear hypochromic scars (Fig. 1).
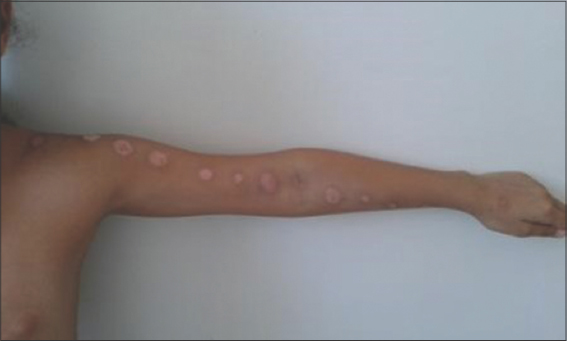 |
Figure 1: Rounded and linear hypochromic lesions arranged on the left upper limb. |
Case 2: A 14-year-old girl, with no particular pathological history, consulted for a sudden appearance, in an interval of 15 days, of multiple lesions of different age, erythematous and erythematous bullous painful center on the left upper limb and abdomen and some lesions on the leg. The lesions quickly gave way to crusty lesions, then rounded hypochromic scars. All these lesions were located in accessible areas and at the contralateral level of the dominant hand (Figs. 2 and 3). The patient had benefited, before consulting us, from a skin biopsy objectifying epidermal necrolysis evoking a bullous fixed pigmented erythema but there was no medication taken reported by the patient herself or her family.
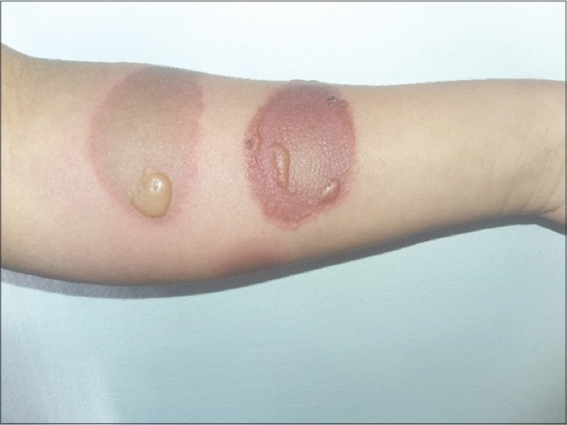 |
Figure 2: Erythematous bullous lesions on the left upper limb. |
 |
Figure 3: Lesions on the abdomen quickly giving way to crusty lesions, then rounded hypochromic scars. |
For the two patients, we noted the presence of recent school-associated difficulties with significant family conflicts. An interview with the two mothers revealed that the two girls had frequently been using deodorant sprays. Faced with this important detail, which adds to emotional vulnerability and to the family conflicts reported by the family, the typical aspect of burn injury and the arrangement of the lesions only in accessible areas made us suspect the diagnosis of pathomimia by cold burn due to misuse of deodorant spray. Dermatological and child psychiatric care was implemented for the two patients. Dermatological care involving occlusive dressings based on petrolatum and healing creams was prescribed (Fig. 4). This had led to the appearance of new lesions on the right forearm in the second case. The dressings were maintained even after the lesions had healed in order to avoid any manipulation or recurrence. On the psychological level, collaboration with child psychiatrists was established. The 14-year-old patient had to be hospitalized in a child psychiatry unit for 5 days, revealing deep psychological damage. During this period, the patient presented no new lesions. The two patients were lost to follow-up; case 1 after two consultations and case 2 after leaving the child psychiatry service.
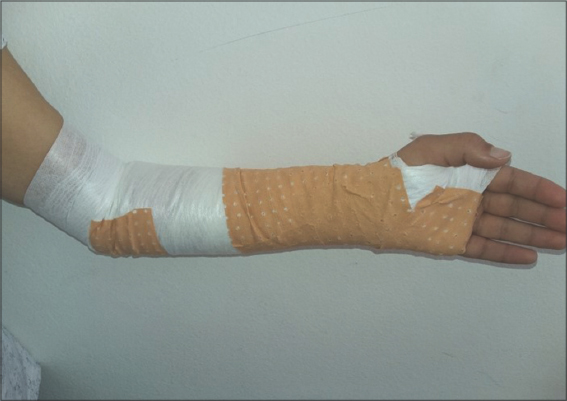 |
Figure 4: Dressing treating and covering of the lesions. |
DISCUSSION
This paper reports two cases for their didactic value, the diagnosis of which was mistaken leading to abusive assessments. Cutaneous pathomimies involve the creation of skin self-lesions: the pathomime intervenes on the body. These lesions, secondary to external actions, are maintained and repeated, while the patient denies any participation in their creation and maintenance. Once the lesions are installed, the patient asks to be cured. The dominant motivation for taking action is repeatedly wanting to be recognized as sick [2]. The clinical picture is often stereotyped with bizarre linear or geometric lesions on accessible areas—the face, neck, hands, forearms—and a fuzzy clinical history [3]. Defontaine-Catteau specifies three attitudes: beautiful indifference, demonstration, and the maintenance and aggravation of lesions [4]. On the psychopathological level, we find elements in favor of relatively poor mentalization, search for love or rejection of the regressive type, indifference to the symptom, emotional dependence, impulsivity, mystification, aggressive sadomasochistic impulses, fragile narcissism, and mechanisms of denial defenses [2]. In the literature, there are few cases of infantile pathomimia, in these children as in ours; we often observe academic difficulties and a family life in crisis [3]. Cutaneous pathomimia in children represents around 1 in 23,000 consultations and nearly 1 in 785 consultations in pediatric dermatology, according to a Mexican study. Childhood pathomimia mainly affects prepubescent girls with an average age of 12 years (2–18 years). The history with the family and the child is often fuzzy, and there are no symptoms or associated prodrome. Diagnosis is often late, delayed by the absence of consultation or by an incorrect diagnosis. In addition, almost half of the patients do not attend a second consultation [5]. The clinical spectrum extends from surface erosion most frequently, to hyper- or hypopigmented lesions, excoriations, ulcerated lesions created by physical or chemical agents; infectious skin lesions such as abscesses or cellulitis by injection of contaminated material, nail granulomas, lymphedema by chronic restriction of a limb, contusion, necrotic, purpuric eczematiform lesions, to a more advanced stage of scabs and scars [5–6]. A cohort published in 2018 was able to report only 56 cases of pathomimia by use of spray, including children and adults. The team demonstrated that the median age of this type of patient was 13 years, that 70.5% were females, and that the median time before consulting was 6 days. Two subgroups were identified: a group that inflicted injuries on themselves in a group known as the courage test and a group that inflicted injuries on their own indicating psychological distress [7]. It should be noted that the use of a spray from a distance of 5 cm for a period of 30 seconds lowers the temperature by 15°C, which causes cold burns responsible for lesions similar to those in our two patients [8]. Anxiety and depression are the most frequently noted conditions, followed by personality disorders in patients with pathomimia [9]. Treatment of such children is special. Forced disappearance of lesions is possible by occlusive dressing, with the possible consequence of the appearance of similar lesions elsewhere on the body [10], an attitude that we adopted in our patients and that led to the appearance of new lesions on the right forearm in the second case. The main difficulty lies in psychological care. It is not advisable to confront the child directly. The best attitude remains to hide from the child that one has understood [6]. Indeed, the immediate proposal for a psychiatric consultation can be perceived as a rejection on the part of the doctor with a risk of worsening the lesions especially when the child is confronted [5] or can scare the patient away. Nevertheless, the need for a psychiatric consultation is obvious [6].
CONCLUSION
Skin pathomimia among children is a rare diagnosis and one of elimination. The diagnosis should be suspected if skin lesions are not consistent with any dermatosis and if the lesions are located in areas accessible to the dominant hand. It is a psychopathological manifestation that is difficult to manage and requires cooperation between a dermatologist and a child psychiatrist.
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients gave their consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Lempérière T. Conversion disorders, factitious disorders, malingering:Clinical approach. Annal Médico-Psychol. 2010;168:286-90.
2. Samai-Haddadi D. La pathomimie cutanée, une perversion malmentalisée?Psychol Clin Projective. 2008;1:189-219.
3. Gil-Bistes D, Kluger N, Guillot B, Bessis D. Dermatitis artefacta in a young girl. Arch Pediatr. 2010;17:1543-5.
4. Defontaine-Catteau MC. Troubles factices et douleurs. Questions posées àMarie-Claude Defontaine-Catteau. Douleurs. 2009;10:100-3.
5. Saez-de-Ocariz M, Orozco-Covarrubias L, Mora-Magaña I, Duran-McKinster C, Tamayo-Sanchez L, Gutierrez-Castrellon P, et al. Dermatitis artefacta in pediatric patients:experience at the national institute of pediatrics. Pediatr Dermatol. 2004;21:205-11.
6. Abilkassem R, Dini N, Ourai H, Kmari M, Agadr A. Factitious disorders in the child:of a case. Pan Afr Med J. 2013;14:23.
7. Maguire R, Patel B, McBride A. Intentional self-inflicted and peer-inflicted aerosol skin injuries called 'frosties’:Cohort series and systematic literature review. Aust J Gen Pract. 2018;47:477-82.
8. Camp DF, Ateaque A, Dickson WA. Cryogenic burns from aerosol sprays:a report of two cases and review of the literature. Br J Plast Surg. 2003;56:815-7.
9. Finore ED, Andreoli E, Alfani S, Palermi G, Pedicelli C, Paradisi M. Dermatitis artefacta in a child. Pediatr Dermatol. 2007;24:51-6.
10. Barfety-Servignat V. From secrecy to sacrifice of the body, history to be shown?Douleurs. 2016;17:296-305.
Notes
Source of Support: Nil,
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
|



Comments are closed.