A late onset of nevus of Ota in a 38-year-old female
Afaf Khouna 1, Hazim Aburabie1, Siham Dikhaye1,2, Nada Zizi1,2
1, Hazim Aburabie1, Siham Dikhaye1,2, Nada Zizi1,2
1Department of Dermatology, Mohammed VI University Hospital of Oujda, Medical School of Oujda, Mohammed First University of Oujda, Morocco, 2Department of Epidemiology, Clinical Research and Public Health Laboratory, Medical School of Oujda, Mohammed First University of Oujda, Morocco
Corresponding author: Dr. Afaf Khouna
Submission: 28.02.2020; Acceptance: 02.05.2020
DOI: 10.7241/ourd.2020S3.4
Cite this article: Khouna A, Aburabie H, Dikhaye S, Zizi N. A late onset of nevus of Ota in a 38-year-old female. Our Dermatol Online. 2020;11(Supp. 3):13-14.
Citation tools:
Copyright information
© Our Dermatology Online 2020. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
Nevus of Ota (NOO) is a blue-grey, usually unilateral macule of the face with a distribution following the first two branches of the trigeminal nerve. It is congenital in around 50% of cases. Onset after 25 years of age is rare and may be confused with other diagnoses, especially melanoma. We report the case of a 38-year-old Moroccan female with a late onset of NOO. Although late-onset NOO is rare, it should be kept in mind since there are good results with laser treatment, which can improve the aesthetic damage and, consequently, the quality of life of the patient.
Key words: Naevus of Ota; Congenital; Late onset; Laser
INTRODUCTION
Nevus of Ota (NOO), also known as oculodermal melanocytosis or nevus fuscoceruleus ophthalmomaxillaris, is a mottled, blue-grey macule usually located unilaterally. It is congenital in around 50% of cases, while, in other cases, it appears by the second decade of life [1]. Onset after 25 years of age is rare [2]. We report the case of a Moroccan female patient with a nevus of Ota, which appeared at the age of 38.
CASE REPORT
A 38-year-old Moroccan female presented herself with a solitary, relatively well-defined, blue-grey, mottled patch on the left cheek going to the nasolabial fold with brownish lentigo-like macules on the same cheek of a five-months duration (Fig. 1). Dermoscopy revealed a whitish-gray veil with brownish lentigo-like macules on top and some fine white dander (Fig. 2). The patient stated that the lesion had gradually darkened for the last months. She denied any previous skin lesions or use of topical skin preparations at this site. A skin biopsy revealed dendritic melanocytes with oar extensions filled with melanin pigment. These widely spaced elements within a moderately fibrous dermis are often arranged parallel to the skin surface. An ophthalmological examination revealed a scleral pigmentation on the left eye (Fig. 3) with a normal baseline ophthalmological evaluation. There was no pigmentation of the oral mucosa.
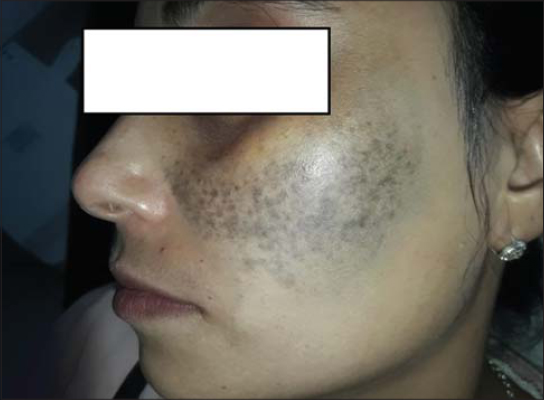 |
Figure 1: A nevus of Ota on the left cheek. |
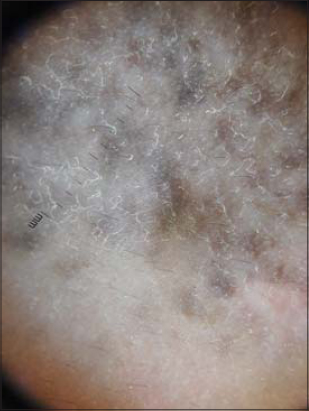 |
Figure 2: Dermoscopy of a nevus of Ota. |
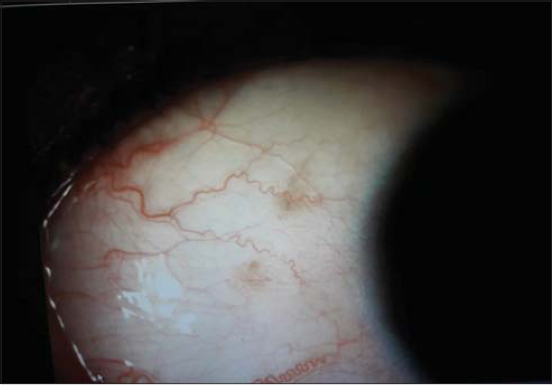 |
Figure 3: Scleral pigmentation of the left eye. |
DISCUSSION
Nevus of Ota (NOO) generally presents itself within the first year of life with a second peak around puberty [2]. It is a fairly common pigmentary disorder in Asians. Recent data from a Korean study of 87 cases revealed that the peak age of onset was during the first ten years (50.6%). In these studies, onset after the age of twenty-five years was not seen. In the English literature, only two cases of nevus of Ota had the onset at more than 30 years [1]. Ours is among the rare cases of a late appearance of a nevus of Ota (in a 38-year-old Moroccan female). Clinically, it manifests itself as speckled dark-brown to bluish unilateral macules involving the periorbital region, forehead, temple, cheek, or nose, corresponding to the distribution of the first two branches of the trigeminal nerve [1].
Q-switched ruby laser (QSRL) has been the type of laser most widely used for NOO. Q-switched alexandrite (QSA) and Nd:YAG lasers are as effective as Q-switched ruby laser. As QSRL has a higher absorption spectrum for melanin, it may lead to pigmentary abnormalities in Asian skin and, hence, Q-switched 1064 nm Nd:YAG laser is the preferred choice for pigmented skin. The same is not true for the Western skin type, for which QSRL is preferred [3]. Recently, however, better results were reported with picosecond lasers, both 755 nm alexandrite and 1064 nm Nd:YAG lasers are efficacious for the treatment of NOO [4].
CONCLUSION
A late and especially acute appearance of a nevus may be confused with a melanoma, hence the importance of increased awareness of the existence of late-onset nevi of Ota, which may help dermatologists in appropriate diagnosis and treatment.
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients gave their consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Chang SE, Kim KJ, Kim ES, Choi JH, Sung KJ, Moon KC, et al. Two cases of late onset Ota’s naevus. Clin Exp Dermatol. 2002;27:202-4.
2. Khurana A, Gupta A, Sardana K, Malhotra P. Late-onset naevus of Ota:a case series of six patients. Clin Exp Dermatol. 2019;44:703-5.
3. Rani S, Sardana K. Variables that predict response of nevus of ota to lasers. J Cosmet Dermatol. 2019;18:464-8.
4. Ohshiro T, Ohshiro T, Sasaki K, Kishi K. Picosecond pulse duration laser treatment for dermal melanocytosis in Asians:A retrospective review. Laser Ther. 2016;25:99-104.
Notes
Source of Support: Nil.
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
|



Comments are closed.