Efficacy of topical 85% formic acid solution in the treatment of warts
Maria Gerodimou, Maria Gerochristou, George Emmanouil, Theodora Douvali, Maria Mazioti
Andreas Syggros Hospital of Cutaneous & Venereal Diseases, Athens, Greece
Corresponding author: Dr. Maria Mazioti
Submission: 17.05.2020; Acceptance: 06.08.2020
DOI: 10.7241/ourd.20204.7
Cite this article: Gerodimou M, Gerochristou M, Emmanouil G, Douvali T, Mazioti M. Effi cacy of topical 85% formic acid solution in the treatment of warts. Our Dermatol Online. 2020;11(4):363-366.
Citation tools:
Copyright information
© Our Dermatology Online 2020. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
Background: Warts represent a common skin disorder that may cause pain and cosmetic deformities. Although their spontaneous clearance can occur at any time, the high rate of transmission makes their treatment absolutely necessary.
Materials and Methods: 139 patients diagnosed with warts participated in our study, which involved dipping a cotton bud in an 85% formic acid solution and applying it to the warts for 3 seconds once weekly. A dermatologist examined the patients in a well-lighted room at baseline and after 4, 6, and 10 weeks of treatment.
Results: After completing the treatment, 79 out of the 139 patients (56.8%) showed complete remission of warts, 20 (28.8%) were partially cured, and 40 (14.4%) showed no change. Formic acid caused a first-degree chemical burn in 5 patients in the sixth week of treatment, resulting in a ten-day intermission until its next application. Only 15 patients (10.8%) complained about a burning sensation, which appeared after 6 applications in 8 patients and after 10 applications in the other 7 patients. Among the patients cured completely, 52 (65.8%) needed 10 weeks of treatment, 19 (24.05%) needed 6 weeks, and 8 (10.15%) achieved complete remission after 4 weeks.
Conclusions: Our study demonstrated that formic acid is a safe and economic therapeutic option for the treatment of warts that produces favorable results with few adverse effects.
Key words: Warts, Formic acid, Efficacy
INTRODUCTION
Warts are defined as benign tumors caused by the infection of keratinocytes with the human papillomavirus (HPV) and appearing as well-defined hyperkeratotic protrusions. Warts may take different morphological forms depending on the type of virus, their location, the immunological status of the patient, and the environmental factors. The types of warts observed include common, plantar, plane, filiform, and anogenital [1]. Various studies have discovered that a significant portion of school-age children and young adults are infected with HPV. Impairment of epithelial barrier function—mainly by trauma—and consequent inoculation of the virus, leads to the formation of warts, easily spread by autoinoculation and direct and indirect contact [2].
The high risk of contagion and the high rate of recurrence prompt patients to search for effective therapy as soon as possible. An overview of the available literature demonstrates that, although several treatments have been tested, none of them offers complete and safe disappearance of warts without side effects [2]. Formic acid is a topical agent that has been used with positive results. The following is a study that aimed to estimate the efficacy of topical 85% formic acid in the treatment of warts and to propose such treatment as a novel therapeutic option.
MATERIALS AND METHODS
The study involved 139 patients who referred to the outpatient clinic of Andreas Syggros University Hospital of Cutaneous and Venereal Diseases, Athens, Greece, and who were diagnosed with warts. Eligible patients were above 18 years old and had shown warts under no previous treatment for the last 6 months. The exclusion criteria included pregnancy, malignancy, diabetes mellitus, concomitant wounds and ulcers, and recent surgery. All participants gave written informed consent and received detailed instructions, according to which they had to dip a cotton bud in an 85% formic acid solution and apply it to their warts for 3 seconds once weekly. Patients were advised to put Vaseline around the warts before the application of formic acid in order to prevent irritation of the healthy skin. A dermatologist examined the patients in a well-lighted room at baseline and after 4, 6, and 10 weeks of treatment. A positive response to treatment was defined as the disappearance of warts, a partial response as a reduction in the total number of warts, and no response as no change in wart formations.
Statistical analysis was performed using the software SPSS Statistics, version 20.0, with the formula mean ± standard error of the mean (SEM). p values below 0.05 were considered statistically significant.
RESULTS
After completing the treatment, 79 out of the 139 patients (56.8%) showed complete remission of warts, 20 (28.8%) were partially cured, and 40 (14.4%) showed no change.
Among the patients cured completely, 52 (65.8%) needed 10 weeks of treatment, 19 (24.05%) needed 6 weeks, and 8 (10.15%) achieved complete remission after 4 weeks. As for the patients who showed a partial response, the number of warts remained stable during the first four weeks of therapy, whereas it was reduced between the sixth and tenth weeks.
Formic acid caused a first-degree chemical burn in 5 patients in the sixth week of treatment, resulting in a ten-day intermission until its next application. Only 15 patients (10.8%) complained about a burning sensation that appeared after 6 applications in 8 patients and after 10 applications in the other 7 patients.
The mean age was 34.42 ± 16.48 years. Females comprised 57.7% of the patients. The mean number of warts at baseline was 3.5 ± 6.1.
95 patients (68.3%) had palmar warts, 35 (25.2%) had plantar warts, 8 (5.8%) had palmoplantar warts, and one (0.7%) had a common wart on the scalp. Among the females, 80% had palmar warts, 18.8% had plantar warts, and 1.2% had palmoplantar warts. Among the males, palmar warts were noted in 52.7% of them, plantar warts in 33.9%, and palmoplantar warts in 11.9%. The only patient with a wart on the scalp was male.
A Pearson’s chi-squared test demonstrated that the sex-to-wart-location relationship was statistically significant (p = 0.002), but revealed no significant relationship between the complete disappearance of warts and their location (p = 0.822).
DISCUSSION
Warts represent a common skin disorder that may cause mild or even severe pain and cosmetic deformities. Although their spontaneous clearance can occur at any time, from a few months to years, the high rate of transmission makes their treatment absolutely necessary. The number, size, and location of warts and the age, compliance, and immunological status of the patient are the main factors that determine the choice of treatment [1].
First-line therapy involves the topical use of caustic acids to cause the destruction of the infected area of the epidermis. Salicylic acid in a concentration of 12–26%, possibly with the addition of lactic acid, is commonly used because of its keratolytic effect, which leads to the reduction of warts and the stimulation of the inflammatory response. Monochloroacetic and trichloroacetic acids and cantharidin are other highly irritant chemicals that can be used. The successful outcome of therapy with these chemicals requires their accurate application, that is, avoiding the healthy skin. Otherwise, chemical burns and pain are likely to occur [2].
Second-line treatments comprise cryotherapy, lasers, hyperthermia, photodynamic therapy, and surgical excision. Cryotherapy is commonly used and gives good results, but may easily cause frostbite injuries and pain [3]. Laser treatment is effective but its high cost, the risk of posttreatment scarring, the relatively long healing time, and the presence of infection particles in laser fumes are significant disadvantages [4]. Finally, several investigators have used topical or intralesional imiquimod, podophyllin, and podophyllotoxin, but their efficacy in the complete elimination of warts has not yet been proven [5].
Formic acid is a natural chemical found in ants, also produced industrially and used as a food additive. Formic acid applied to human tissue in high concentrations provokes denaturalization and coagulative necrosis, leading the virally infected cells to death. Clinically, formic acid application makes warts more whitish and causes the desquamation of their superficial layer [4].
The high success rate of wart treatment has been mentioned after topical puncture with 85% formic acid in a period of 1 to 3 months [6,7]. Tippanawar et al. have also reported that 82% of patients treated with 80% formic acid intralesionally achieved complete disappearance of warts after 10 applications [4]. Handjani et al. compared the efficacy of a topical 85% formic acid preparation with a combined topical solution of salicylic and lactic acid, and proved it to be an effective cure for warts after the use of formic acid, especially for warts located on the hands [8]. The results of our study are in accordance with the clinical trials set forth above. The efficiency of our therapy reached 56.8% in a period of 10 weeks, indicating that the topical application of 85% formic acid is an effective treatment for warts. Fig.1 shows the clinical result of formic acid application on a palmar wart after 10 weeks of treatment.
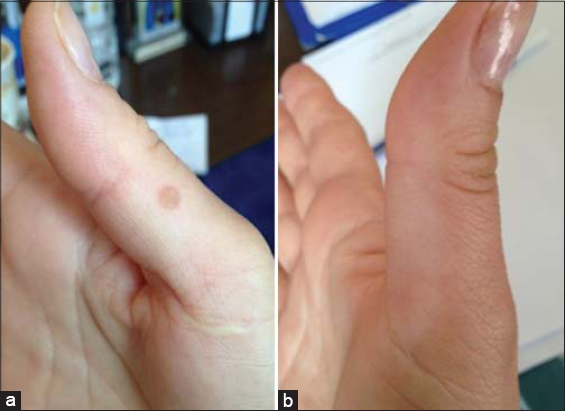 |
Figure 1: (a) A palmar wart at baseline. (b) The same palmar wart after 10 applications of topical 85% formic acid solution. |
Apart from its efficacy, the use of formic acid is an inexpensive option with no equipment requirements. In addition, the risk of posttreatment scarring and nail dystrophy is low, and patients can return to their occupations immediately; no local anesthesia is required, which makes it well tolerated by children [4,6–8]. As in all therapies, treatment with formic acid, a chemical acid, poses some adverse effects. A burning sensation, pain, and post-inflammatory hyperpigmentation may occur. Their incidence depends mainly on the concentration of formic acid and the duration and frequency of therapy. Balagué et al. were the first to mention a third-degree chemical burn in a patient after the application of a formic acid ointment continuously for six hours with an occlusive dressing. Although most of the adverse effects of formic acid are topical, blindness after eye contact is mentioned in the literature. Furthermore, continuous use of formic acid can lead to systemic absorption, causing acidosis, memory loss, confusion, and kidney and liver damage [7]. In our study, only 15 patients (10.8%) complained about a burning sensation, which occurred after 6 applications in 8 patients and after 10 applications in the other 7 patients. Furthermore, formic acid caused a first-degree chemical burn in 5 patients in the sixth week of treatment, resulting in a ten-day intermission until its next application.
CONCLUSIONS
Our study demonstrated that formic acid is a safe and economic therapeutic option for warts that gives good results with few adverse effects. Because it was not double-blind, the study showed some inevitable limitations. However, it highlights the necessity of conducting future large-scale studies in order to substantiate the effectiveness and benefits of these various treatments.
Statement of Human and Animal Rights
All the procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the 2008 revision of the Declaration of Helsinki of 1975.
Statement of Informed Consent
Informed consent for participation in this study was obtained from all patients.
REFERENCES
1. Lebwohl MG, Rosen T, Stockfleth E. The role of human papillomavirus in common skin conditions:current viewpoints and therapeutic options. Cutis. 2010;86:1-11.
2. Dall’oglio F, D’Amico V, Nasca MR, Micali G. Treatment of cutaneous warts:an evidence-based review. Am J Clin Dermatol. 2012;13:73-96.
3. Bruggink SC, Gussekloo J, Berger MY, Zaaijer K, Assendelft WJ, de Waal MW, et al. Cryotherapy with liquid nitrogen versus topical salicylic acid application for cutaneous warts in primary care:randomized controlled trial. CMAJ. 2010;182:1624-30.
4. Tippanawar SA, Kadam MN, Phatale SR, Kadam PM. Study of te efficacy of intralesional formic acid 80% in verruca vulgaris. Int J Adv Med. 2016;3:206-8.
5. Kwok CS, Gibbs S, Bennett C, Holland R, Abbott R. Topical treatments for cutaneous warts. Cochrane Database Syst Rev. 2012;9:CD001781.
6. Faghihi G, Vali A, Radan M, Eslamieh G, Tajammoli S. A double-blind, randomized trial of local formic acid puncture technique in the treatment of common warts. Skinmed. 2010;8:70-1.
7. BalaguéN, Vostrel P, Beaulieu JY, van Aaken J. Third degree formic acid chemical burn in the treatment of a hand wart:a case report and review of the literature. Springerplus. 2014;3:408.
8. Handjani F, Saki N, Zandi S, Sayyafan MS, Kardeh B, Emami Y, et al. Comparison of the efficacy of topical 85% formic acid versus a combination of topical salicylic acid and lactic acid in the treatment of warts:A randomized, triple-blind, controlled trial. Iran J Dermatol. 2016;19:1-5.
Notes
Source of Support: Nil.
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
|



Comments are closed.