Two cases of sporotrichoid leischmaniasis induced by antimonyate infiltration
Mohamed El Amraoui , Rachid Frikh, Naoufal Hjira, Mohammed Boui
, Rachid Frikh, Naoufal Hjira, Mohammed Boui
Department of Dermatology-Venereology, Mohammed V Military Training Hospital, Rabat, Morocco
Corresponding author: Dr. Mohamed El Amraoui
Submission: 16.12.2019; Acceptance: 18.02.2020
DOI: 10.7241/ourd.20203.25
Cite this article: El Amraoui M, Frikh R, Hjira N, Boui M. Two cases of sporotrichoid leischmaniasis induced by antimonyate infi ltration. Our Dermatol Online. 2020;11(3):321-322.
Citation tools:
Copyright information
© Our Dermatology Online 2020. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
Sir,
Sporotrichoid leishmaniasis is a sporadic form of cutaneous leishmaniasis characterized by staged subcutaneous nodules aligned on a lymphatic path. Its onset directly suggests underlying immunosuppression, but its installation after the initiation of local antimonial treatment remains enigmatic. We present two cases illustrating this phenomenon.
Case No. 1: A 30-year-old man, with a suspicion of an endemic area of leishmaniasis, consulted for an ulcerated nodule on the back of the left foot evolving for the past two months. A parasitological examination indicated cutaneous leishmaniasis. The patient received five antimony infiltrations. The evolution was marked by the appearance of three similar lesions staged along a hardened cord of the lower left limb (Fig. 1). A diagnosis of sporotrichoid leishmaniasis was accepted. The patient received systemic treatment with antimoniates with a favorable evolution.
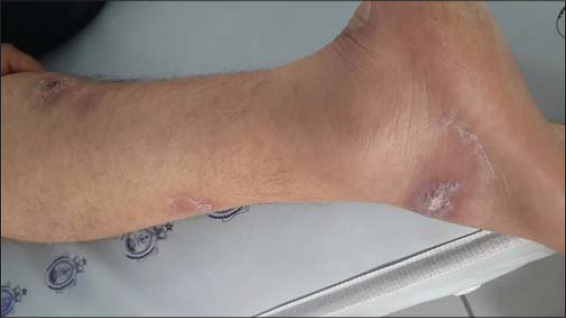 |
Figure 1: Sporotrichoid leishmaniasis of the left leg. |
Case No. 2: A 30-year-old man, with a suspicion of an endemic area of cutaneous leishmaniasis four months prior, consulted for two scaly erythematous lesions 4 cm in diameter, one on the right leg and one on the left wrist, evolving for the past two months. A diagnosis of cutaneous leishmaniasis was confirmed by parasitological examination and the patient received seven infiltrations of antimoniates. The evolution was marked by a partial improvement of the initial lesions and the appearance of seven firm subcutaneous nodules of 0.5 to 1 cm in diameter aligned along a lymphatic path of the left forearm (Fig. 2). Venous Doppler echo eliminated thrombophlebitis, and the histology of the nodule was nonspecific. A search for underlying immunosuppression was negative. The evolution was favorable after systemic treatment with antimoniates.
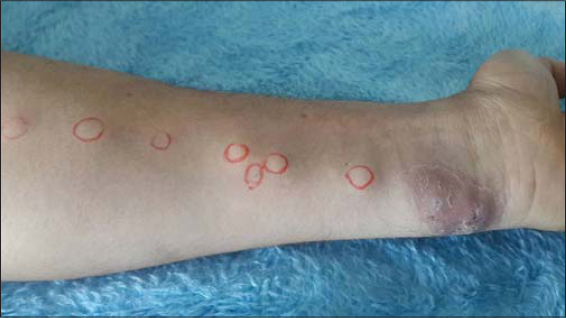 |
Figure 2: Sporotrichoid leishmaniasis of the left forearm. |
Cutaneous leishmaniasis is very common in this context, characterized by its large clinical polymorphism (large simulator). Sporotrichoid forms, on the other hand, are rare. The two main promoting factors of sporotrichoid leishmaniasis are the patient’s immune status and the species of leishmania.
Histology of nodules is often nonspecific and a search for Leishman’s bodies is rarely or very rarely positive. Treatment employs antimonates systemically, and resistant forms can be managed with Itraconazole or Amphotericin B. This form does not seem to be associated with a poor prognosis. However, the pathophysiological mechanisms of this dissemination after infiltration and negativation of biopsies remain enigmatic [1–3].
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients have given consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Hjira N, Frikh R, Marcil T, Lamsyah H, Oumakhir S, Baba N, et al. Clinical, epidemiological and evolutionary aspects in 157 cases of cutaneous leishmaniasis in Morocco. Pan Afr Med J. 2014;17:272.
2. Benzaquen M, Chambelland A , Fongue J, Melenotte C, Christen J-R, Ranque S, et al. Cutaneous sporotrichoid leishmaniasis treated with oral fluconazole. Dermatol Ther. 2019;32:e12976.
3. Carvalho LMV, Pimentel MIF, Conceição-Silva F, de Camargo Ferreira E Vasconcellos E, Valete-Rosalino CM, Lyra MR, et al. Sporotrichoid leishmaniasis:A cross-sectional clinical, epidemiological and laboratory study in Rio De Janeiro State, Brazil. Rev Inst Med Trop Sao Paulo. 2017;59:e33.
Notes
Source of Support: Nil,
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0001-7687-0158 http://orcid.org/0000-0001-7687-0158 |



Comments are closed.