Localized skin-colored nodules and tumors on the trunk
Anissa Zaouak 1, Leila Bouhajja1, Wafa Koubaa2, Houda Hammami1, Samy Fenniche1
1, Leila Bouhajja1, Wafa Koubaa2, Houda Hammami1, Samy Fenniche1
1Department of Dermatology, Habib Thameur Hospital, Tunis, Tunisia; 2Department of Anatomopathology, Habib Thameur Hospital, Tunis, Tunisia
Corresponding author: Dr. Anissa Zaouak
Submission: 27.10.2019; Acceptance: 27.05.2020
DOI: 10.7241/ourd.20203.22
Cite this article: Zaouak A, Bouhajja L, Koubaa W, Hammami H, Fenniche S. Localized skin-colored nodules and tumors on the trunk. Our Dermatol Online. 2020;11(3):314-315.
Citation tools:
Copyright information
© Our Dermatology Online 2020. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
Sir,
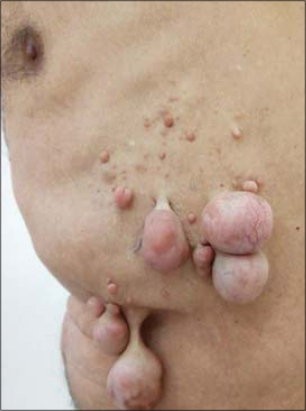
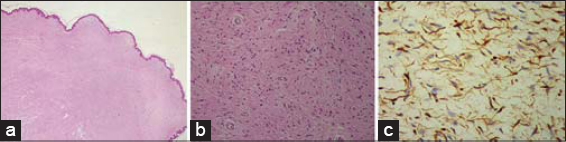
We report a 79-year-old man without a significant medical history referred to our department for multiple nodules and tumors on the left side of his trunk, which had appeared progressively for many years. Despite him having no family history of similar lesions, they had increased in size and number over the same area. A dermatological examination revealed multiple soft to firm skin-colored nontender nodules and pedunculated tumors varying in size from 1 to 7 cm in diameter localized on the left side of the trunk without crossing the midline (Fig. 1). Some of the cutaneous nodules showed a positive buttonhole sign. There were no similar lesions elsewhere. Café-au-lait macules, axillary and inguinal freckling, plexiform neurofibromas, and kyphoscoliosis were absent in the patient. There were no Lisch nodules on ophthalmological examination. A neurological examination was normal. Computerized tomography of the brain, chest, and abdomen was normal and tumor markers were negative. A skin biopsy of the skin-colored nodule was performed revealing well-circumscribed unencapsulated interlacing bundles of elongated cells with darkly stained nuclei (Figs. 2a and 2b). The tumor cells showed positive S100-protein immunoreactivity (Fig. 2c). Combining clinical and histopathological findings allowed us to confirm the diagnosis of late-onset segmental neurofibromatosis. The patient was scheduled for surgical removal of his cutaneous tumors for aesthetic reasons. Regular medical follow-up was also recommended.
Herein, we report a case of late-onset segmental neurofibromatosis (SNF) in an old patient. The cutaneous nodules had appeared spontaneously and progressively and had been slowly increasing in size. It is a rare variant of neurofibromatosis and its prevalence in the general population is estimated at 1 in 36,000–40,000 individuals [1].
Riccardi established the clinical features of segmental neurofibromatosis [2]. In fact, SNF is considered a noninherited form of neurofibromatosis and results from a postzygotic mutation in the NF1 gene leading to somatic mosaicism [3]. The neurofibromas are limited to one body region and the cutaneous features of neurofibromatosis type I are absent. Ophthalmological and neurological complications are rare in SNF [2]. The latter is usually unilateral, as in our case, but could also be bilateral [4] or even multiple [5]. Differential diagnosis includes soft fibromas, cutaneous schwannomas, cutaneous metastases, nevus lipomatosus cutaneous superficialis, cutaneous leiomyomas, trichoepitheliomas, xanthomas, and lymphomas. Histopathology is crucial for diagnosis, showing a well-circumscribed mass composed of spindle cells with elongated wavy nuclei in the dermis consistent with the diagnosis of neurofibroma [3]. In this case, there was no systemic involvement and no evidence of an internal malignancy. In fact, according to Dang et al. [6], segmental neurofibromatosis could be a paraneoplastic manifestation. Malignancies that could be associated with SNF include malignant peripheral nerve sheath tumors, malignant melanomas, breast cancer, gastric cancer, and colon cancer, which were absent in our patient [4,6]. SNF is an often-overlooked disorder since patients are usually asymptomatic and seek medical attention only for cosmetic reasons [7]. Hence, surgical removal of tumors is usually recommended, as performed in our patient. Finally, accurate diagnosis of this rare variant of neurofibromatosis is important since it gives different prognoses than neurofibromatosis type I. It is also important to reassure the patient and to provide proper genetic counseling [2].
Consent
The examination of the patient was conducted according to the principles of the Declaration of Helsinki.
The authors certify that they have obtained all appropriate patient consent forms, in which the patients have given consent for images and other clinical information to be included in the journal. The patients understand that their names and initials will not be published and due effort will be made to conceal their identity, but that anonymity cannot be guaranteed.
REFERENCES
1. Wagner G, Meyer V, Sachse MM. Segmental neurofibromatosis. Hautarzt. 2018;69:487-90.
2. Riccardi VM. Neurofibromatosis:clinical heterogeneity. Curr Probl Cancer. 1982;7:1-34.
3. Laurent KJ, Beachkofsky TM, Loyd A, Neiner JR. Segmental distribution of nodules on trunk. J Fam Pract. 2017;66:765-7.
4. Lopes MR, Vilar AN, Pockstaller MP, Daher JG, Azulay DR. Bilateral segmental neurofibromatosis. Int J Dermatol. 2014;53:1136-7.
5. Maouni S, Senouci K, Benzekri L. A rare case of multiple segmental neurofibromatosis. Eur J Dermatol. 2020;30:76-7.
6. Dang JD, Cohen PR. Segmental neurofibromatosis and malignancy. Skinmed. 2010;8:156-9.
7. Kim SR, Kibbi N, Imaeda S. Segmental neurofibromatosis 1 with gonosomal mosaicism. Int J Dermatol. 2019;58:e255-6.
Notes
Source of Support: Nil,
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0003-2062-2256 http://orcid.org/0000-0003-2062-2256 |



Comments are closed.