Deep skin and soft tissue infection of the neck – first sign of unrecognized diabetes mellitus
Uwe Wollina , Violetta Bujok, Caroline Fürll, Gesina Hansel
, Violetta Bujok, Caroline Fürll, Gesina Hansel
Department of Dermatology and Allergology, Städtisches Klinikum Dresden, Academic Teaching Hospital, 01067 Dresden, Germany
Corresponding author: Dr. Prof. Uwe Wollina
Submission: 16.11.2019; Acceptance: 22.01.2020
DOI: 10.7241/ourd.20203.21
Cite this article: Wollina U, Bujok V, Fürll C, Hansel G. Deep skin and soft tissue infection of the neck – fi rst sign of unrecognized diabetes mellitus. Our Dermatol Online. 2020;11(3):312-313.
Citation tools:
Copyright information
© Our Dermatology Online 2020. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
Sir,
Skin and soft tissue infections (SSTIs) are common infectious disorders, while complicated SSTI (cSSTIs) representing the more severe subtype developing deep-seated infection, a requirement for surgical intervention, the presence of systemic signs of infection, and the presence of complicating comorbidities [1]. These disorders require initiation of appropriate empiric broad-spectrum antimicrobial therapy, early aggressive surgical intervention for drainage of abscesses and debridement, and identification of responsible bacteria and appropriate de-escalation of antimicrobial therapy [2]. Carbuncles and cSSTIs may be a symptom of unrecognized diabetes mellitus [3].
A 38 year-old male patient presented with a carbuncle on his neck worsening during 7 days of ambulatory oral antibiosis with ampicillin/sulbactam. His medical history was unremarkable despite a type-I-allergy against and dog and cat epithelia. After a couple of days, he developed fever and malaise. Therefore, he was admitted to the Department of Dermatology and Allergology.
On examination we observed a tense and very painful erythematous swelling on his neck about 10 cm in diameter with central pustulations and putride discharge (Fig. 1). Neck lymph nodes were swollen and painful. Or working diagnosis was cSSTI following a neck carbuncle.
 |
Figure 1: Carbuncle of the neck with putride discharge. The erythema and swelling in the surrounding tissue indicate deep skin and soft tissue infection more extensive than the initial carbuncle. |
Laboratory investigations: Leukocytosis of 20.75 Gpt/l (normal range 3.8 – 11.00), thrombocytosis of 414.0 Gpt/l, neutrophila of 18.4 Gpt/l (1.8 – 7.6), C-reactive protein 277 mg/l (<5), HbA1C (IFFC) 92 mmol/ml (20-42), glucose up to 16.9 mmol/l (4.1 – 5.9).
Urine: glucosuria > 1000 mg/dl (<50), proteinuria 50 mg/dl (<10), ketone >150 mg/dl (<5).
Microbiology: Staphylococcus aureus, sensible to ampicillin/sulbactam.
Histology: Extensive perifollicular putrid and absceding inflammation with perforations to the skin surface.
Imaging techniques: Computerized tomography of neck and chest with extensive inflammatory infiltration of subcutaneous adipose tissue of the neck, multiple inflammatory-reactive lymph nodes (Figs. 2a and 2b). Abdominal sonography remained unremarkable.
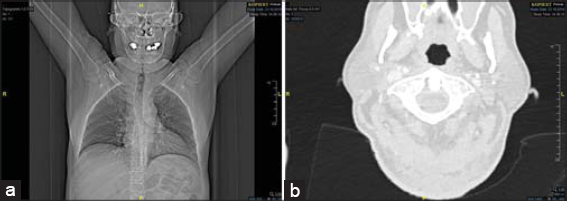 |
Figure 2: (a) CT-Imaging excludes mediastinal or pulmonary spread of the skin and soft tissue infection. (b) Deep infection of the neck. |
Ophthalmologic investigation: Non-proliferative diabetic retinopathy.
Treatment: We started with a dose escalation of 3 g ampicillin/sulbactam i.v. and metronidazole 500 mg i.v. every 8 hours and added oral metamizole 3 x 1 g/d. Aggressive surgical drainage of the abscess was performed. The wounds were irrigated repetitively using Ringer’s solution, and framycetin sulfate powder was applied. Systemic antibiosis was adapted to microbiological findings, dose was escalated.
Within 7 days, the fever ceased, leukocytosis, neutrophilia, thrombocytosis, and C-reactive protein normalized.
Drug therapy of diabetes mellitus was initialized with the diabetologist using a combination of short and long acting insulins: Actrapid HM® (Novo Nordisk) and Toujeo® (Insulin Glargin 300 I.E/ml; Sanofi). After release from the hospital the patient was referred to a diabetologist for further treatment and monitoring.
cSSTI are an extreme of the common SSTIs. They often are associated to significant comorbidities, sometimes unrecognized as in the present case. Analysis of comorbidities in patients with deep neck infections demonstrated diabetes mellitus in 19.0% to 20.5% [4,5]. In a meta-analysis of deep neck infections, diabetes mellitus was associated with multispacer spread of infection (Relative risk [RR] 1.96) and complications (RR 2.42) [6].
The most common bacteria responsible for carbuncles and cSSTI of the neck include anerobic Peptostreptococcus, Streptococcus aureus, Streptococcus viridans, Streptococcus pyogenes, but in diabetics Klebsiella pneumoniae acquires also importance [5,6].
Other skin diseases that warrant the exclusion of unrecognized diabetes mellitus are necrobiosis lipoidica [7], eruptive xanthomas [8], acne keloidalis nuchae [9], and secondary phimosis [10].
In conclusion, carbuncles and cSSTis can be a symptom of unrecognized and uncontrolled diabetes. Early recognition and a combined approach with aggressive surgery and specific antibiosis is essential to prevent complications such as mediastinitis, pneumonia or sepsis (in case of neck localization). Diabetes and other comorbidities need an adequate treatment in a multidisciplinary approach.
Consent
The examination of the patient was conducted according to the Declaration of Helsinki principles.
The authors certify that they have obtained all appropriate patient consent forms. In the form the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
REFERENCES
1. Sunderkötter C, Becker K, Eckmann C, Graninger W, Kujath P, Schöfer H. Calculated initial parenteral treatment of bacterial infections:Skin and soft tissue infections. GMS Infect Dis. 2020;8:Doc11. doi:10.3205/id000055
2. Rath E, Skrede S, Oppegaard O, Bruun T. Non-purulent skin and soft tissue infections:predictive power of a severity score and the appropriateness of treatment in a prospective cohort. Infect Dis (Lond). 2020;52:361-71.
3. Venkatesan R, Baskaran R, Asirvatham AR, Mahadevan S. 'Carbuncle in diabetes’:a problem even today!BMJ Case Rep. 2017;2017. pii:bcr-2017-220628.
4. Kauffmann P, Cordesmeyer R, Tröltzsch M, Sömmer C, Laskawi R. Deep neck infections:A single-center analysis of 63 cases. Med Oral Patol Oral Cir Bucal. 2017;22:e536-41.
5. Kakoschke TK, Ehrenfeld M, Mast G. [Severe bacterial soft tissue infections in the head and neck region :Overview of the causes, pathogenesis, diagnostics, treatment and possible sequelae]. Chirurg. 2020;91:283-92.
6. Hidaka H, Yamaguchi T, Hasegawa J, Yano H, Kakuta R, Ozawa D, et al. Clinical and bacteriological influence of diabetes mellitus on deep neck infection:Systematic review and meta-analysis. Head Neck. 2015;37:1536-46.
7. Erfurt-Berge C, Dissemond J, Schwede K, Seitz AT, Al Ghazal P, Wollina U, et al. Updated results of 100 patients on clinical features and therapeutic options in necrobiosis lipoidica in a retrospective multicentre study. Eur J Dermatol. 2015;25:595-601.
8. Wollina U, Koch A, Hansel G, Schönlebe J. Eruptive xanthomas – two case reports with distinct features. Open Access Maced J Med Sci. 2018;6:2152-4.
9. Bimbi C, Brzeziński P. Combined treatment of keloids and scars with Nd:YAG 1064 nm laser and cryotherapy:Report of clinical casswses. Our Dermatol Online. 2020;11:149-53.
10. Bonifaz A, Tirado-Sánchez A, Jaramillo-Manzur C, Araiza J, Fierro-Arias L. Candida balanitis. Clinical and mycological study about the effi cacy of a single-day oral treatment with itraconazole (400 mg). Our Dermatol Online. 2020;11:1-5.
Notes
Source of Support: Nil,
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
 http://orcid.org/0000-0001-5933-2913 http://orcid.org/0000-0001-5933-2913 |



Comments are closed.