Bazex syndrome in a patient with pulmonary adenocarcinoma
Hazim Aburabie 1, Imane Alouani1, Saida Sefraoui1, Nada Zizi1,2, Siham Dikhaye1,2
1, Imane Alouani1, Saida Sefraoui1, Nada Zizi1,2, Siham Dikhaye1,2
1Department of Dermatology, Mohammed VI University Hospital of Oujda, Mohammed First University of Oujda, Morocco; 2Laboratory of Epidemiology, Clinical Research and Public Health, Faculty of Medicine and Pharmacy, Mohammed the First University of Oujda, Morocco
Corresponding author: Dr. Hazim Aburabie
Submission: 05.09.2019; Acceptance: 19.11.2019
DOI: 10.7241/ourd.20203.10
Cite this article: Aburabie H, Alouani I, Sefraoui S, Zizi N, Dikhaye S. Bazex syndrome in a patient with pulmonary adenocarcinoma. Our Dermatol Online. 2020;11(3):267-269.
Citation tools:
Copyright information
© Our Dermatology Online 2020. No commercial re-use. See rights and permissions. Published by Our Dermatology Online.
ABSTRACT
The paraneoplastic acrokeratosis or Bazex syndrome is a rare paraneoplastic dermatosis generally associated with malignancy, most often with squamous cell carcinoma of the upper aerodigestive tract, characterized by acral psoriasiform lesions. Amelioration of the eruption usually requires treatment of the underlying malignancy. We report the case of a Moroccan woman followed up for pulmonary adenocarcinoma who received treatment based on palliative chemotherapy; she later developed a cutaneous eruption. The clinical, biological and histological elements were in favor of paraneoplastic dermatosis (Bazex syndrome). Paraneoplastic acrokeratosis has been traditionally described as a paraneoplastic entity mainly associated with malignant tumor. Treatment of the underlying malignancy is the basis for managing paraneoplastic Bazex syndrome.
Key words: Bazex syndrome, Paraneoplastic syndrome, Squamous cell carcinomas
INTRODUCTION
Paraneoplastic acrokeratosis (Bazex syndrome), described by Bazex in 1965, is a rare paraneoplastic condition. It is strongly associated to various internal malignancies, including squamous cell carcinoma of the upper aerodigestive tract, but also in a number of other tumors. In this report, we describe a rare case of a 63-year-old Moroccan female who developed Bazex syndrome a year after being diagnosed with lung adenocarcinoma with cerebral metastasis.
CASE REPORT
A 63-year-old woman, was diagnosed with lung adenocarcinoma in May 2018. She first underwent radiation therapy (10 cycles received). The follow up imaging revealed cerebral metastasis of her lung adenocarcinoma. The patient then received palliative chemotherapy (carboplatin and paclitaxel). After her third cure of chemotherapy, she developed erythematous lesions on the hands and face.
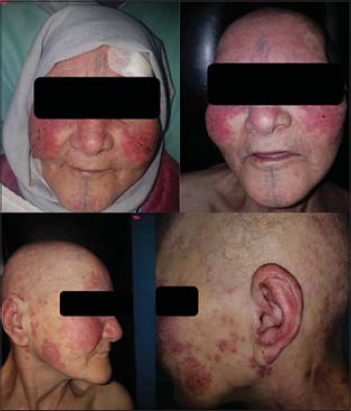
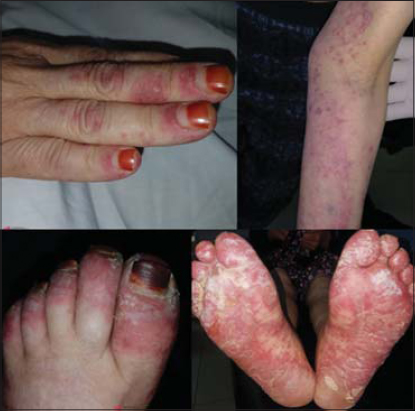
On physical examination, the patient presented a symmetric non-pruritic erythematous and keratotic erythematous plaque with fine borders covered by fine scales. The lesions were located on her face (cheeks and nose), helices of her ears and acral areas (fingers and toes). There was no megacapillary on periungual dermoscopy (Figs. 1 and 2).
The main differential diagnosis consisted of mixed connective tissue disease, systemic lupus erythematosus, dermatomyositis, hand-feet syndrome related to chemotherapy and Bazex syndrome.
Skin biopsy histology and direct immunofluorescent were not significative as well as for biological investigations for differential diagnosis. Hence, the diagnosis of acrokeratosis paraneoplastica (Bazex syndrome) was established. We prescribed topical corticosteroids with a slight regression of symptoms.
DISCUSSION
Bazex syndrome is a rare paraneoplastic skin condition, which is most prevalent with squamous cell carcinomas of the upper aerodigestive tract [1]. In a systematic review of the literature that identified 77 patients with Bazex syndrome, the underlying neoplasms were squamous cell carcinoma of the head and neck in 39 percent and squamous cell carcinoma of the lung in 11 percent, followed by gastrointestinal adenocarcinoma, genitourinary tumors, lymphomas and lung adenocarcinoma in 3.5 percent [2]. A review of the literature by Antonio Crucitti et al. showed that of 143 cases, only 5 had Bazex syndrome with pulmonary adenocarcinoma [3], a 6th case has been reported in the literature by Jing Zhao in 2016 [4].
In other studies reported by Rodrigues et al., this disease rarely affects female patients, with only 16 occurrences in the largest case series up to date. Cases accompanying lung adenocarcinoma in female patients as reported here by our patient are extremely rare, the first case of a female patient with pulmonary adenocarcinoma was reported in 1989 [5].
Typical clinical manifestations of Bazex syndrome include psoriasiform eruptions that favor the acral such as the fingers (61%), toes (39%) and nose (63%) with tenderness but no pruritus in most cases [4]. This condition normally progresses in 3 stages: cutaneous lesions on the ears, fingers, nails and palmoplantar keratosis. Remarkably, the underlying malignancy tends to display its symptoms during the stage of palmoplantar keratosis. The biological, histological and immunological findings of Bazex syndrome are unspecific, as in this patient. The underlying mechanism of this paraneoplastic syndrome in uncertain. A mixed reaction between specific types of tumours and cutaneous antigens may be responsible. The growth factors released by highly proliferative cancer cells and neoplasm associated with zinc deficiency might be implicated in the occurrence of this cutaneous paraneoplastic disorder [6].
In most patients, cutaneous manifestations of Bazex syndrome precede the diagnosis of malignancy by several months. However, the malignancy is diagnosed concurrently or before Bazex syndrome manifestations in approximately one-third of cases, as in our patient [7].
The lesions of Bazex syndrome are frequently resistant to targeted therapies but treatment of the neoplasm usually leads to resolution to the cutaneous findings. In our patient, we noticed a minor regression of cutaneous symptoms after chemotherapy. However, there are reports of patients in whom the cutaneous manifestations persist following successful therapy.
CONCLUSION
Our case demonstrates the rare occurrence of Bazex syndrome in a female patient diagnosed while being treated for lung adenocarcinoma with brain metastasis. Treatment of the underlying malignancy is the basis for managing paraneoplastic Bazex syndrome.
Consent
The examination of the patient was conducted according to the Declaration of Helsinki principles.
The authors certify that they have obtained all appropriate patient consent forms. In the form the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
REFERENCES
1. Rodrigues IA Jr, Gresta LT, Cruz RC, Carvalho GG, Moreira MH. Bazex syndrome. An Bras Dermatol. 2013;88(6 Suppl 1):209-11.
2. Räßler F, Goetze S, Elsner P, Acrokeratosis paraneoplastica (Bazex syndrome) –a systematic review on risk factors, diagnosis, prognosis and management. J Europ Acad Dermatol Venereol. 2017;31:1119-36.
3. Crucitti A, Feliciani C, Grossi U, La Greca A, Porziella V, Giustacchini P, et al. Paraneoplastic acrokeratosis (bazex syndrome) in lung cancer. J Clin Oncol. 2009;27:e266-8.
4. Zhao J, Zhang X, Chen Z, Wu J-H. Case Report:Bazex syndrome associated with pulmonary adenocarcinoma. Medicine (Baltimore). 2016;95:e2415.
5. Dabas G, De D, Handa S, Chatterjee D, Radotra BD. Acrokeratosis paraneoplastica (Bazex syndrome). QJM. 2018;111:63-4.
6. Boldt S, Wollina U. Bazex-syndrome with esophageal cancer. Our Dermatol Online. 2016;7:403-5.
7. Koh WL, Ang CC, Lim SP. Psoriasiform dermatitis in a case of newly diagnosed locally advanced pyriform sinus tumour:Bazex syndrome revisited. Singapore Med J. 2012;53:e12-4.
Notes
Source of Support: Nil,
Conflict of Interest: None declared.
Request permissions
If you wish to reuse any or all of this article please use the e-mail (brzezoo77@yahoo.com) to contact with publisher.
| Related Articles | Search Authors in |
|
|



Comments are closed.